
Am Fam Physician. 2001;64(10):1681-1682
to the editor: Rectus sheath hematoma is an uncommon cause of acute abdominal pain. It may occur as a result of direct trauma, spontaneously, or as a result of twisting or abrupt changes in position.1 Other precipitating factors include anticoagulation, recent surgery, medication injection, or increased intra-abdominal pressure from coughing or pregnancy.1 Rectus sheath hematoma has been previously described in a patient receiving enoxaparin at 30 mg subcutaneously every 12 hours.1 We report the case of a patient who developed rectus sheath hematoma during treatment with enoxaparin, 70 mg subcutaneously every 12 hours, and in whom bleeding was controlled through coil embolization of the inferior epigastric artery.
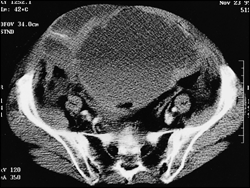
A 75-year-old woman was admitted to the hospital for pneumonia and new-onset atrial fibrillation. In addition to antibiotics, the patient was placed on enoxaparin, 70 mg subcutaneously every 12 hours. On the second day after admission, the patient complained of a sudden onset of right lower quadrant abdominal pain followed by evidence of hy-povolemic shock. Laboratory studies revealed a 3 g per dL drop in the hemoglobin concentration. Physical examination revealed a palpable, firm, tender, nonmobile 5 × 6 cm right lower quadrant abdominal mass. Abdominal ultrasound confirmed an 18 × 9 3 16 cm rectus sheath cystic mass. There was a small previous injection site near the center of the hematoma. A computed tomographic scan of the abdomen performed three hours later showed a 21 × 14 × 8 cm hematoma expanding in the lower half of the right rectus sheath (see the accompanying figure).
The patient was resuscitated with intravenous fluids, fresh frozen plasma, packed red blood cells, crystalloids, and protamine sulfate. Aortoiliac and pelvic arteriography with superselective catheterization showed bleed ing emanating from two small collaterals from the right inferior epigastric artery. Bleeding was stopped through embolization with two tornado coils in the right inferior epigastric artery. The patient made a gradual and full clinical recovery.
Low-molecular-weight heparin (LMWH) offers several advantages when compared with unfractionated heparin (UH), including improved bioavailability, ease of administration, lack of required monitoring, and a decreased incidence of heparin-induced thrombocytopenia. In most clinical circumstances, the risk of bleeding appears to be comparable with that of UH.2
Results of a small prospective study in patients with atrial fibrillation showed that LMWH was an effective alternative for providing anticoagulation.4 Protamine sulfate was administered because of the persistent bleeding despite the fact that it incompletely reverses antifactor Xa activity produced by LMWH. LMWH has some disadvantages as opposed to unfractionated heparin. First, it is difficult to obtain a prompt and accurate assessment of the degree of anticoagulation that has been induced with LMWH. Second, the anticoagulant effect of LMWH is more difficult to reverse promptly because of its administration into the subcutaneous tissue and a longer biologic half-life.
We believe that the patient's coughing, anticoagulation, and possible needle puncture of the inferior epigastric artery contributed to the hematoma. Awareness of this rare clinical entity is important in the differential diagnosis of acute abdominal pain. The majority of patients with rectus sheath hematoma are treated conservatively. Catheter embolization offers a suitable alternative to surgical management in cases in which the hematoma continues to expand.