Endoscopy is increasingly used to diagnose and treat a growing number of gastrointestinal conditions. Up to 1.9 percent of the more than 500,000 colonoscopies performed in the United States each year result in significant complications. Although the overall rate of complications is believed to be low, the occurrence of complications is highly dependent on the experience and skill of the endoscopist. Kavic and Basson reviewed the literature to summarize the potential complications of endoscopy.
Adverse effects may be caused by sedation. At least 7 percent of patients undergoing gastroscopy develop oxygen saturation levels lower than 80 percent. However, some patients experience significant discomfort when sigmoidoscopy is performed without sedation. Topical anesthetic agents reduce discomfort but can interfere with motor function. No guidelines have been established on the use of sedation, oxygen or intravenous access lines during endoscopy procedures.
The requirement to fast before endoscopy may cause problems in diabetic patients and others. In addition, fewer than 20 percent of patients are able to take the 4L of fluid required by conventional bowel preparations, and these regimens may result in hypovolemia or electolyte imbalances. Small-volume preparations are available but may not result in adequate bowel clearing, and the heavy salt and phosphate content may compromise some patients, especially those with renal or cardiac problems. Preparations requiring enemas may result in mechanical damage to bowel mucosa.
Perforation is the most common and serious complication of colonoscopy. Approximately 66 percent of perforations are retrosigmoid and 13 percent are cecal. The ascending, descending and transverse colon each account for about 7 percent of perforations. Perforation, which can result from direct mechanical trauma or pneumatic distention of the bowel, may not cause overt peritoneal signs and symptoms. Detection requires upright radiographs of the abdomen and computed tomographic scan, if necessary. Although surgery is often required to repair perforations, in selected patients the condition can resolve with conservative treatment provided the perforation is small and peritonitis does not develop (see accompanying figure).
FIGURE. Management of Colonoscopic Perforation
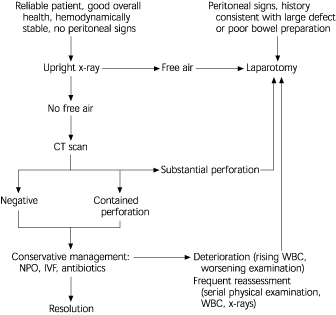
A suggested algorithm for treatment of colonoscopic perforation. (CT = computed tomographic; NPO = nothing by mouth; IVF = intravenous fluids; WBC = white blood count)
Reprinted with permission from Kavic SM, Basson MD. Complications of endoscopy. Am J Surg 2001;181:324.
Hemorrhage is most common when colonoscopy is used to biopsy or remove colonic lesions. Hemorrhage can occur up to two weeks postprocedure. Patients should be closely monitored with frequent checks of hematocrit levels. In approximately 65 percent of cases, the condition resolves with supportive therapy. Tagged red-blood scan or repeat colonoscopy may be required to identify the source of continued bleeding.
Less common but serious complications of colonoscopy include splenic trauma, vasovagal reactions and endocarditis. Sepsis and other infections following colonoscopy are rare.

