Statins (also known as 3-hydroxy-3-methyl-glutaryl coenzyme A [HMG-CoA] reductase inhibitors) are generally recognized as the treatment of choice in patients with hypercholesterolemia because they are easy to use, effective, and well tolerated. However, there are currently five statins on the market: synthetic statins (atorvastatin and fluvastatin), and three natural statins—(lovastatin, pravastatin, and simvastatin). Cerivastatin was recently withdrawn from the market. Chong and colleagues reviewed the various statins to determine if there are clinical advantages to choosing one over the others. The statins have different abilities to lower low-density lipoprotein (LDL) cholesterol levels, differing pharmacokinetics, differing interactions with drugs and foods, and variable costs.
Statins lower cholesterol levels through inhibition of HMG-CoA reductase. The synthetic and natural statins have essentially equivalent efficacy at improving the lipid profile. However, in patients who do not achieve their LDL goals, atorvastatin and simvastatin may be the best choices for initial therapy.
Statins also have antiproliferative effects on smooth muscle cells and antioxidant and anti-inflammatory effects, all of which may help to reduce coronary events. Current research does not clearly suggest that one statin is better than another at causing these effects.
Bioavailability varies widely among the statins: simvastatin is less than 5 percent bioavailable, while fluvastatin is approximately 24 percent bioavailable. The agents are also absorbed at rates ranging from about 30 percent with lovastatin to 98 percent with fluvastatin. First-pass metabolism occurs in all statins except pravastatin. Pravastatin is also the least protein-bound of the statins (about 50 percent), compared with the others, which are more than 90 percent protein-bound.
FIGURE. Statin Selection or Substitution
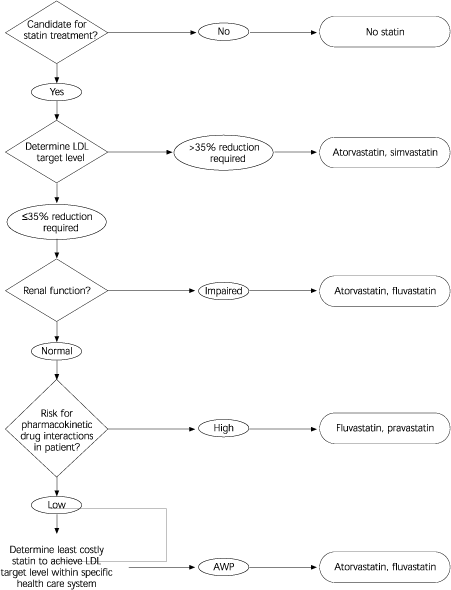
Simplified flow chart of major considerations for statin selection or substitution. The cost-effective statin choices in the last stage are based on an analysis using AWP and may depend on the specific heath care setting. (LDL = low-density lipoprotein cholesterol; AWP = average wholesale price.)
Adapted with permission from Chong PH, Seeger JD, Franklin C. Clinically relevant differences between the statins: implications for therapeutic selection. Am J Med 2001;111:396.
Pravastatin and fluvastatin are hydrophilic, which may cause less insomnia than the other statins (which are lipophilic). This may not be a clinically important distinction, so selection on this criterion alone is probably not warranted. However, if a patient develops insomnia, switching to a different agent is an option. Renal elimination occurs in greater proportions with pravastatin, and a dose reduction may be reasonable in patients with moderate or greater renal dysfunction. If creatinine clearance is less than 60 mL per minute (1.00 mL per second), the medication should be started at one half the usual starting dosage and titrated according to response. Atorvastatin and fluvastatin do not require dosage adjustments in patients with renal impairment.
All statins are associated with drug interactions, mainly because of their effects on the cytochrome P450 enzymatic pathway. However, pravastatin does not undergo metabolism by this pathway. Fluvastatin is metabolized by the CYP2C9 isoenzyme, while the other statins are metabolized by the CYP3A4 isoenzyme. Because a number of other medication interactions may occur, it is prudent to check these interactions before prescribing one of these medications.
Food interactions may also occur; grapefruit juice increases levels of atorvastatin, lovastatin, and simvastatin. Food increases the bioavailability of lovastatin, so this medication should be taken with food. Conversely, the bioavailability of pravastatin, atorvastatin, and fluvastatin is decreased by food, but this effect is not thought to change the lipid-lowering effects. Therefore, these three statins can be taken at any time.
In the accompanying figure, the authors offer an approach to determining which statin is appropriate for each patient.

