
Am Fam Physician. 2002;65(9):1877-1878
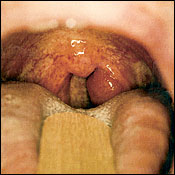
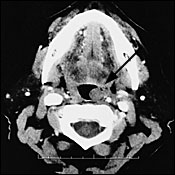
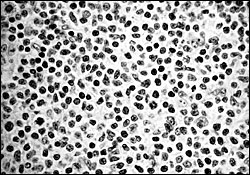
A 75-year-old woman presented for a physical examination. Her history was significant for intermittent dysphagia. She denied any history of cigarette smoking or alcohol use. Physical examination showed a well-defined 2 cm × 3 cm submucosal mass in the left peritonsillar region (Figure 1). The mucosa overlying the lesion was normal in appearance. Palpation revealed the mass to be firm, well circumscribed, and somewhat mobile. There were no other intraoral abnormalities identified on the remainder of the physical examination. The patient underwent a computed tomographic scan of the head and neck (Figure 2, arrow) followed by an excisional biopsy of the mass. Figure 3 shows a pathology specimen micrograph.
Question
Discussion
The answer is C: non-Hodgkin's lymphoma (NHL). The head and neck is not a common site for initial presentation of NHL, but when seen, it can arise in lymphoid tissue (e.g., tonsils, adenoids) or various extralymphoid sites including the nasal cavity, paranasal sinuses, thyroid, and orbit. Extranodal NHL typically occurs in patients 50 to 60 years of age,1–3 and more than one half of these involve the tonsils or adenoidal tissue.3 Symptoms, when they occur, are typically because of compression or displacement of surrounding structures. If the mass is large enough, it can even cause partial obstruction of the oropharynx. The majority of head and neck NHLs are of the intermediate grade, with the diffuse large cell type B-cell lymphomas being the most common histologic subtype.
Treatment of localized low-grade lymphomas includes radiation therapy. Patients with more extensive disease can be offered single-agent or combination chemotherapy. Alternatively, depending on the patient's age and comorbid diseases, treatment can be postponed in patients with low-grade lymphoma until symptomatic disease progresses or warrants intervention,4 because these types of tumors are not curable.
Peritonsillar abscess (quinsy) is a suppurative complication of pharyngitis or tonsillitis. It most commonly affects young adults and typically presents with high fever and neck pain. The infection may spread to involve the parapharyngeal or retropharyngeal spaces with complications including mediastinitis and septic thrombophlebitis.5 Evaluation of the oropharynx typically reveals a fluctuant, erythematous, and edematous mass causing deviation of the uvula to the opposite side. Cultures are polymicrobial with aerobic Streptococci (group A) and anaerobic Bacteroides species predominating.
Squamous cell carcinoma (SCC) of the oropharynx, like NHL, can present as an exophytic mass. The distinction is particularly important because lymphomas are more responsive to treatment.1 Definitive diagnosis can only be made through biopsy and histopathologic examination. Risk factors for SCC of the head and neck include smoking and alcohol consumption, immune deficiency, and SCC of other sites, including lung, larynx, and esophagus.
Herpangina is a vesicular disease of the oropharynx usually caused by Coxsackie A viruses. The disease occurs most commonly in children during summer and fall. Clinical manifestations include small-ulcerated vesicles in the soft palate and posterior pharynx. Treatment involves supportive care, and regression usually occurs over a period of several weeks.
Hypertrophic tonsils are usually seen in young children with chronic allergies. Typically, patients will have bilateral hypertrophic tonsils and a history of chronic allergy symptoms.