
Am Fam Physician. 2002;65(12):2501-2505
Basal cell nevus syndrome is an autosomal dominant condition with complete penetrance and variable expressivity. It is characterized by five major components, including multiple nevoid basal cell carcinomas, jaw cysts, congenital skeletal abnormalities, ectopic calcifications, and plantar or palmar pits. Other features include a host of benign tumors, ocular defects, and cleft lip and palate. Guidelines for diagnosis include a family history, careful oral and skin examinations, chest and skull radiographs, panoramic radiographs of the jaw, magnetic resonance imaging of the brain, and pelvic ultrasonography in women.
Basal cell nevus syndrome, also known as Gorlin's syndrome, was first reported by Jarisch and White in 1894. The spectrum of disease associated with this syndrome was described in detail by Gorlin in 1960.1 The prevalence is estimated to be 1 per 60,000 persons.2 This syndrome is characterized by five major components as well as other features that may be present (Table 1).3,4 Basal cell nevus syndrome is an autosomal dominant condition with complete penetrance and variable expressivity.5,6 The gene responsible has been localized to chromosome 9q22.1–q31.7,8
| Clinical features | Percentage of patients affectd | |
|---|---|---|
| Multiple nevoid basal cell carcinomata3 | 50 | |
| Odontogenic keratocysts (jaw cysts are the earliest presenting sign) | 65 to 70 | |
| Congenital skeletal abnormalities | 65 to 70 | |
| Bifid ribs | ||
| Synostosis | ||
| Frontal and parietal bossing | ||
| Hypertelorism | ||
| Sprengel's deformity (high scapulae) | ||
| Ectopic calcification of the falx cerebri | 65 to 70 | |
| Plantar and/or palmar pits4 | 60 | |
| Other features | Varies | |
| Neoplasms and hamartomas | ||
| Medulloblastomas | ||
| Myocardial fibromas | ||
| Meningiomas | ||
| Ovarian fibromas | ||
| Rhabdomyomas | ||
| Lymphomesenteric cysts | ||
| Ocular defects | ||
| Colobomas | ||
| Cataracts | ||
| Glaucoma | ||
| Cleft lip and palate | ||
The patient described in the following illustrative case was not diagnosed for several years, despite an array of physical signs and symptoms. Increased awareness on the part of the family physician could have led to earlier referral for specialized diagnosis and treatment. Early diagnosis and treatment may reduce the severity of the long-term sequelae of basal cell nevus syndrome, including malignancy and oromaxillofacial deformation and destruction.
Illustrative Case
A 15-year-old female with complaints of increasing facial swelling of the mandibular and maxillary regions presented to a plastic surgery clinic after referral from her primary care physician. The swelling had persisted for several years despite conservative treatment with anti-inflammatory agents. The patient's past medical history was significant for multiple cutaneous cystic lesions on the face, chest, and back that necessitated several surgical excisions during the past several years; severe amblyopia; asthma; and recurrent urinary tract infections. The patient was adopted, and her family history is unknown.
On physical examination, multiple facial cutaneous nevi were evident, with marked bifrontal bossing. Multiple areas of swelling were noticeable in the mandibular and maxillary regions (Figures 1 and 2). An expansile lesion of the right mandibular cortex was visualized and palpated, as well as a right maxillary expansile lesion. The upper left and right lateral incisors were missing. Palpation of the areas of swelling did not produce pain, nor was any erythema present.
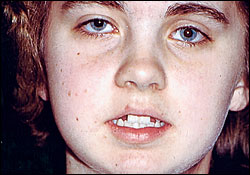
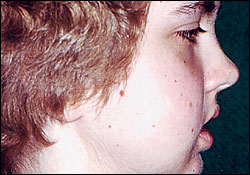
Diagnostic tests included skull and chest radiographs, panoramic films, and computed tomographic scans (Table 2).
| Radiologic diagnosis | Examples |
|---|---|
| Skull radiograph | Calcified falx cerebri (see Figure 3) |
| Panoramic films* | Right mandibular ramus odontogenic cyst measuring 6 × 2.5 cm displacing the embedded lower left third molar |
| Right mandibular body odontogenic cyst measuring 2.5 × 1.5 cm diverting the roots of the lower left second tricuspid and the lower left first molar | |
| Odontogenic cyst around the crown of the impacted upper right third molar | |
| Right maxillary cystic lesion with a 3-cm diameter associated with the imbedded left upper third molar (see Figure 4) | |
| Computed tomography | Confirmed the panoramic radiographic findings scan |
| Chest radiograph | Showed rib asymmetry, especially of the second and third ribs |
| No bifid ribs were found |
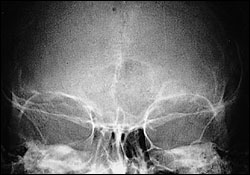
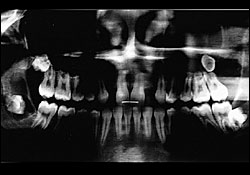
Under general anesthesia, the patient underwent excision of all odontogenic cysts with extraction of all four third molars (Figures 5 and 6). The right infraorbital, lingual, and mental nerves were visualized during the surgery. The excised jaw cysts were diagnosed as odontogenic keratocysts by histopathologic examination.
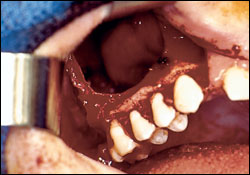
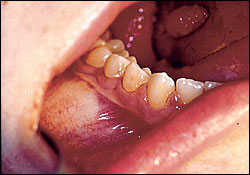
The patient's postoperative course was unremarkable, and she recovered well. She is being monitored closely for nevi and jaw cyst recurrence with biannual follow-up examinations and annual panoramic films. No recurrence has been detected in the 10 months following her surgery.
Clinical Presentation
The presence of multiple odontogenic cysts, a calcified falx cerebri, and multiple cutaneous nevi establishes a diagnosis of basal cell nevus syndrome. The presenting sign of increasing facial swelling results from expansion of the cystic lesions on the jaw. Odontogenic keratocysts are cystic lesions lined with keratinized epithelium. Most authors identify the dental lamina as the origin of the cysts.
Cysts most frequently occur in the molarramus region of the mandible, but they may also occur in the maxilla.9 Cyst development may occur in patients as young as four years.10 These cysts have a proclivity for local invasion, including involvement of the teeth, and they have a tendency to recur. A recurrence rate of 60 percent in patients with basal cell nevus syndrome has been documented.11 Recurrence is the consequence of incomplete removal, remnants of dental lamina within the jaw, or the presence of satellite cysts. Therefore, treatment consists of wide surgical excision and curettage with extraction of associated teeth. Bone grafting and alveolar nerve grafting may be required in some instances.
Histopathologic examination of excised tissue is required because several cases of malignant transformation to squamous cell carcinoma have been reported in the literature.12 Close follow-up of these patients is necessary to monitor for recurrence of odontogenic keratocysts and the development of basal cell carcinoma of the skin. Biannual physical examinations and annual panoramic films are recommended.
Role of the Family Physician
The family physician's role in treating patients with basal cell nevus syndrome is threefold. First, the physician should recognize the syndrome by the history and physical examination and be alerted to the other findings that may coexist. The history should include relevant medical and dental information, including removal of jaw cysts, abscesses, or skin lesions. Any relevant family history, including brain tumors or female-organ tumors, should be ascertained.
The physical examination should include an oral inspection for mandibular and maxillary swelling, head circumference and head shape inspection, skin examination for basal cell nevi, and pits on the palms and soles. The necessary radiographic studies, such as chest and skull radiographs and panoramic films, should be obtained early in the treatment process to confirm the syndrome and establish a clear treatment plan. A magnetic resonance image of the brain would be important to detect meningiomas or medulloblastomas at an early age. Medulloblastomas can be detected between two and three years of age and may be treated with radiotherapy. Ovarian ultrasonography for detection of ovarian cysts or fibromas is also indicated.
The second task is to alert family members to be tested for the syndrome, because it is an autosomal dominant disorder that has been identified in families.6–8 Finally, the patient should be referred to the appropriate subspecialists, including a neurosurgeon, plastic surgeon, or obstetrician, depending on the specific manifestations that need to be addressed.