A committee for the American College of Cardiology/American Heart Association (ACC/AHA) Task Force on Practice Guidelines recently updated the 1996 guidelines on perioperative cardiovascular evaluation for noncardiac surgery. The executive summary of the revised guidelines was published in the March 12,2002 issue of Circulation.
Beyond providing medical clearance for surgery, the preoperative cardiac evaluation has these purposes:
- To evaluate the patient’s current medical status.
- To make recommendations on the risk, evaluation, and management of cardiac problems during the perioperative period.
- To provide a clinical risk profile for use in making treatment decisions that may affect short- and long-term cardiac outcomes.
The goals of the perioperative evaluation are to assess cardiac risk, determine the most appropriate tests and treatments for optimal patient care, and contain costs by avoiding unnecessary testing.
The predominant theme of the ACC/AHA updated guidelines is that preoperative intervention is rarely required for the sole purpose of lowering surgical risk. The classifications of evidence used in summarizing the indications for specific treatments are provided in Table 1.1
TABLE 1 Classifications of Evidence for Specific Treatments
| Class I | Conditions for which there is evidence and/or general agreement that a given procedure or therapy is useful and effective |
| Class II | Conditions for which there is conflicting evidence and/or a divergence of opinion about the usefulness or efficacy of performing the procedure or therapy |
| Class IIa | Weight of evidence or opinion is in favor of usefulness or efficacy |
| Class Ilb | Usefulness or efficacy is less well established by evidence or opinion |
| Class III | Conditions for which there is evidence and/or general agreement that a procedure or therapy is not useful or effective and in some cases may be harmful |
Adapted with permission from Eagle KA, Berger PB, Calkins H, Chaitman BR, Ewy GA, Fleischmann KE, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary. Circulation 2002;105:1258.
Preoperative Evaluation
The history, physical examination, and electrocardiogram (ECG) are directed at identifying preexisting cardiac disease and other conditions that may increase perioperative risk. Disease severity and stability, as well as previous treatments, also need to be determined.
Functional capacity, which can be expressed in metabolic equivalent (MET) levels, can be an important factor. A patient who cannot meet a 4-MET demand with most normal daily activities has increased perioperative cardiac and long-term risks. Energy requirements for various activities can be estimated using a questionnaire (Table 2).1–3
TABLE 2 Estimated Energy Requirements for Various Activities*
| Energy expenditure† | Questions | |
|---|---|---|
| 1 MET | Can you— | |
| Take care of yourself? | ||
| Eat, dress, or use the toilet? | ||
| Walk indoors around the house? | ||
| Walk a block or two on level ground at 2 to 3 miles per hour (3.2 to 4.8 kilometers per hour)? | ||
| 4 METs | Can you— | |
| Climb a flight of stairs or walk up a hill? | ||
| Walk on level ground at 4 miles per hour (6.4 kilometers per hour)? | ||
| Run a short distance? | ||
| Do heavy work around the house, such as scrubbing floors and lifting or moving heavy furniture? | ||
| Take part in moderate-energy recreational activities such as golf, bowling, dancing, doubles tennis, or throwing a baseball or football? | ||
| More than 10 METs | Can you— | |
| Take part in high-energy sports such as swimming, singles tennis, football, basketball, or skiing? | ||
MET= metabolic equivalent.
*— This questionnaire was adapted from the Duke Activity Status Index2 and the American Heart Association exercise standards.3
†— Energy expenditures for the first grouping (e.g., eating, walking indoors) range from 1 to 4 METs; energy expenditures for the second grouping (e.g., climbing stairs, moderate recreational activities) range from 4 to 10 METs.1
Adapted with permission from Eagle KA, Berger PB, Calkins H, Chaitman BR, Ewy GA, Fleischmann KE, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary. Circulation 2002;105:1261.
Other factors that can help determine cardiac risk include the patient’s age and comorbid conditions. Significant comorbid conditions include chronic pulmonary disease, diabetes mellitus, renal dysfunction, and peripheral vascular disease. Cardiac risk is also higher with certain surgeries, such as vascular procedures and complicated, prolonged abdominal, thoracic, and head and neck procedures.
Conditions that have been associated with an increased risk of perioperative morbidity include coronary artery disease, heart failure, a history of cerebrovascular disease, an elevated creatinine level (greater than or equal to 2 mg per dL [ 180 μmol per L]), diabetes requiring insulin treatment, and high-risk surgery. Based on consensus, the ACC/AHA committee divided markers (predictors) of clinical risk into three categories (Table 3).1,4
TABLE 3 Clinical Predictors of Increased Perioperative Cardiovascular Risk*
| Major predictors | Intermediate predictors | Minor predictors | |
| Unstable coronary syndromes | Mild angina pectoris (Canadian class I or II4) | Advanced age | |
| Acute or recent myocardial infarction† with evidence of important ischemic risk by clinical symptoms or noninvasive study | Previous myocardial infarction by history or pathologic Q waves | Abnormal electrocardiogram (left ventricular hypertrophy, left bundle branch block, ST-T abnormalities) | |
| Unstable or severe angina‡ (Canadian class III or IV4) | Compensated or previous heart failure | Rhythm other than sinus rhythm (e.g., atrial fibrillation) | |
| Decompensated heart failure | Diabetes mellitus (particularly type 1 diabetes) | Low functional capacity (e.g., inability to climb one flight of stairs carrying a bag of groceries) | |
| Significant arrhythmias | Renal insufficiency | History of stroke | |
| High-grade atrioventricular block | Uncontrolled systemic hypertension | ||
| Symptomatic ventricular arrhythmias in the presence of underlying heart disease | |||
| Supraventricular arrhythmias with uncontrolled ventricular rate | |||
| Severe valvular disease | |||
*— Increased risk of myocardial infarction, heart failure, or death.
†— Based on the American College of Cardiology National Data Library, myocardial infarction occurring within the previous seven days is considered acute; myocardial infarction occurring within more than seven days and up to 30 days is considered recent.
‡— May include stable angina in patients who are unusually sedentary.
Adapted with permission from Eagle KA, Berger PB, Calkins H, Chaitman BR, Ewy GA, Fleischmann KE, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary. Circulation 2002;105:1261.
STEPWISE APPROACH TO PERIOPERATIVE CARDIAC ASSESSMENT
A proposed stepwise approach for determining which patients are most likely to benefit from preoperative coronary assessment and treatment is provided in Figure 1.1 This approach depends on assessment of clinical predictors, previous coronary evaluation and treatment, functional capacity, and surgery-specific risk. Steps corresponding to the algorithm are described in Table 4.1,5
FIGURE 1. Preoperative Cardiac Assessment
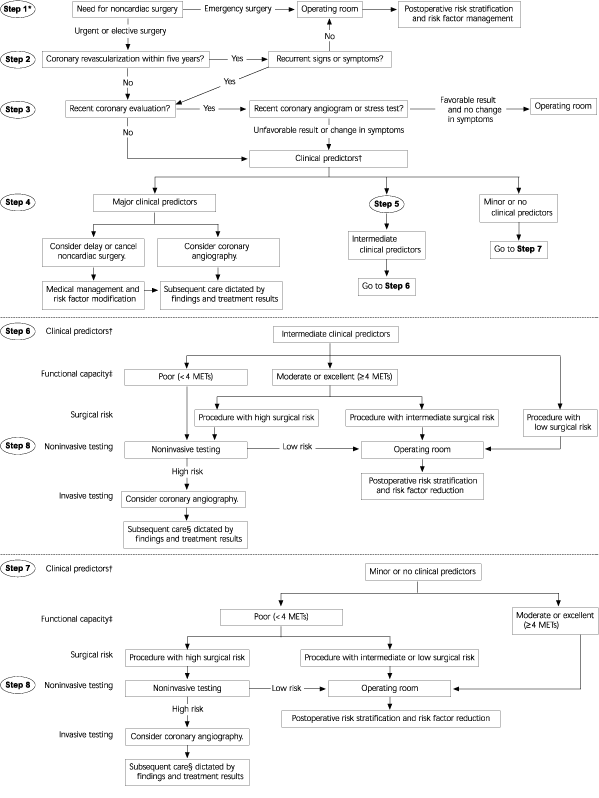
Stepwise approach to cardiac assessment before noncardiac surgery.
Adapted with permission from Eagle KA, Berger PB, Calkins H, Chaitman BR, Ewy GA, Fleischmann KE, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary. Circulation 2002;105:1260.
TABLE 4 Steps in Assessing Preoperative Cardiac Risk in Noncardiac Surgery*
| Step 1 | What is the urgency of noncardiac surgery? Certain emergencies do not allow time for a preoperative cardiac evaluation. Postoperative risk stratification may be appropriate for some patients who have not had this assessment before. |
| Step 2 | Has the patient undergone coronary revascularization in the past five years? If so, and if clinical status has remained stable without recurrent symptoms and/or signs of ischemia, further cardiac testing is generally not necessary.5 |
| Step 3 | Has the patient had a coronary evaluation in the past two years? If coronary risk was adequately assessed and the findings were favorable, it is usually not necessary to repeat testing unless the patient has experienced a change or has had new symptoms of coronary ischemia since the previous evaluation. |
| Step 4 | Does the patient have an unstable coronary syndrome or a major clinical predictor of risk? When elective noncardiac surgery is being considered, the presence of unstable coronary disease, decompensated heart failure, symptomatic arrhythmias, and/or severe valvular disease usually leads to cancellation or delay of surgery until the problem has been identified and treated. |
| Step 5 | Does the patient have intermediate clinical predictors of risk? The presence or absence of previous myocardial infarction by history or electrocardiogram, angina pectoris, compensated or previous heart failure, preoperative creatinine level greater than or equal to 2 mg per dL [180 μmol per L]), and/or diabetes mellitus helps to further stratify clinical risk for perioperative coronary events. Consideration of functional capacity and level of surgery-specific risk allows a rational approach to identifying patients who are most likely to benefit from further noninvasive testing. |
| Step 6 | Patients without major predictors but with intermediate predictors of clinical risk and moderate or excellent functional capacity can generally undergo intermediate-risk surgery with little likelihood of perioperative myocardial infarction or death. Conversely, further noninvasive testing is often considered in patients with poor functional capacity or moderate functional capacity but higher risk surgery, especially patients with two or more intermediate predictors of cardiac risk. |
| Step 7 | Noncardiac surgery is generally safe in patients with neither major nor intermediate predictors of cardiac risk and moderate or excellent functional capacity (4 METs or greater). Additional testing may be considered on an individual basis in patients without clinical markers but with poor functional capacity who are to undergo higher risk surgery, particularly patients with several minor clinical predictors of risk who are scheduled to undergo vascular surgery. |
| Step 8 | The results of noninvasive testing can be used to determine the need for additional preoperative testing and treatment. In some patients with documented coronary artery disease, the risk of coronary intervention or corrective cardiac surgery may approach or even exceed the risk of the proposed noncardiac surgery. This approach may be appropriate, however, if it significantly improves the patient’s long-term prognosis.† |
*— See Figure 1.
†— For some patients, careful consideration of clinical, surgery-specific, and functional capacity results in the decision to perform coronary angiography.
Adapted with permission from Eagle KA, Berger PB, Calkins H, Chaitman BR, Ewy GA, Fleischmann KE, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary. Circulation 2002;105:1257–67.
Specific Preoperative Cardiovascular Conditions
HYPERTENSION
Stage 3 hypertension (180/110 mm Hg or higher) should be controlled preoperatively. Effective control often can be achieved with outpatient treatment for several days to weeks before surgery. For more urgent surgery, blood pressure can be lowered with rapid-acting agents. Antihypertensive therapy is continued through the perioperative period.
VALVULAR HEART DISEASE
To lower the risk of perioperative heart failure or shock, symptomatic stenotic lesions often require percutaneous valvotomy or valve replacement before noncardiac surgery. Patients with symptomatic regurgitant valvular disease may be stabilized with intensive medical therapy and monitoring before surgery, with definitive treatment given later.
When delaying noncardiac surgery may have serious consequences, medical therapy and monitoring are appropriate. Exceptions may include severe valvular regurgitation with a reduction in left ventricular function. In these patients, limited hemodynamic reserve increases the likelihood of destabilization during perioperative stresses.
MYOCARDIAL DISEASE
Patients with dilated and hypertrophic cardiomyopathy are at increased risk for perioperative heart failure. In these patients, preoperative management is directed at maximizing hemodynamic status. An estimate of hemodynamic reserve can be helpful in anticipating potential complications. Intensive medical therapy and monitoring are provided after surgery.
ARRHYTHMIAS
Patients with arrhythmias or cardiac conduction disturbance should be evaluated for underlying cardiopulmonary disease, metabolic abnormality, or drug toxicity. Treatment for the underlying cause of a symptomatic or hemodynamically significant rhythm disturbance should be initiated; the arrhythmia should also be treated.
Aggressive perioperative monitoring or treatment of frequent premature ventricular beats and asymptomatic nonsustained ventricular tachycardia generally is not necessary. These rhythm disturbances have not been associated with an increased risk of nonfatal myocardial infarction or cardiac death.
PACEMAKERS AND IMPLANTABLE CARDIOVERTER-DEFIBRILLATORS
The evaluation of an implantable pacemaker or automatic implantable cardioverter-defibrillator (ICD) depends on the urgency of surgery, the pacemaker leads (bipolar or unipolar), the electrocautery (bipolar or unipolar), the distance between the pacemaker and electrocautery, and pacemaker dependency.
Immediately before surgery, an ICD should be programmed off. The device should be programmed on again after surgery.
Supplemental Preoperative Evaluation
Specific recommendations depend on the individual patient and circumstance. The exercise ECG is the test of choice in most ambulatory patients. The ACC/AHA classifications of evidence used to summarize the indication for a particular therapy or treatment (Table 11) are used in the following discussions.
RESTING LEFT VENTRICULAR FUNCTION
Perioperative ischemic events are not consistently predicted by the resting left ventricular function. Recommendations for preoperative noninvasive evaluation of left ventricular function are as follows:
- Class I: current or poorly controlled heart failure (repeat preoperative testing may not be necessary if previous evaluation documented severe left ventricular dysfunction).
- Class IIa: previous heart failure; dyspnea of unknown origin.
- Class III: as a routine test of left ventricular function in patients without previous heart failure.
12-LEAD RESTING ECG
Some ECG abnormalities are clinical predictors of increased perioperative and long-term cardiovascular risk in patients at clinically intermediate or high risk who are undergoing intermediate- or high-risk surgical procedures. Recommendations for the performance of the preoperative 12-lead resting ECG are as follows:
- Class I: recent episode of chest pain (or ischemic equivalent) in patients at clinically intermediate or high risk who are scheduled to undergo an intermediate- or high-risk procedure.
- Class IIa: asymptomatic patients with diabetes mellitus.
- Class IIb: Previous coronary revascularization.
Asymptomatic male patients older than 45 years and female patients older than 55 years who have two or more risk factors for atherosclerosis.
Previous hospitalization for cardiac causes.
- Class III: as a routine test in asymptomatic patients undergoing low-risk operative procedures.
EXERCISE OR PHARMACOLOGIC STRESS TESTING
Through changes in the ECG and hemodynamic response, exercise stress testing can provide an estimate of functional capacity and detect myocardial ischemia. Recommendations for exercise or pharmacologic stress testing are as follows:
- Class I: Diagnosis in adult patients with an intermediate pretest probability of having coronary artery disease.
Assessment of prognosis in patients who are under going initial evaluation for suspected or proven coronary artery disease; evaluation of patients who have a significant change in clinical status.
Demonstration of myocardial ischemia before coronary revascularization is performed.
Assessment of the adequacy of medical treatment; if recent evaluation is not available, evaluation of prognosis after an acute coronary syndrome.
- Class IIa: evaluation of exercise capacity when subjective assessment is not reliable.
- Class IIb: Diagnosis in patients with a high or low pretest probability of coronary artery disease (e.g., resting ST-depression of less than 1 mm, digitalis therapy, ECG criteria for left ventricular hypertrophy).
Detection of restenosis within initial months after percutaneous coronary intervention in high-risk asymptomatic patients.
- Class III: For exercise stress testing, diagnosis in patients who have resting ECG abnormalities that preclude adequate assessment (e.g., electronically paced ventricular rhythm, pre-excitation syndrome, resting ST-depression greater than or equal to 1 mm, left bundle-branch block).
Severe comorbid conditions that are likely to limit life expectancy or candidacy for revascularization.
Routine screening of asymptomatic adult patients.
In young patients, investigation of isolated ectopic beats.
CORONARY ANGIOGRAPHY
Recommendation for coronary angiography before or after noncardiac surgery are as follows:
- Class I: known or suspected coronary artery disease.
Evidence indicating a high risk for adverse outcome based on the results of noninvasive tests.
Angina that does not respond to adequate medical therapy.
Unstable angina, particularly when intermediate-or high-risk noncardiac surgery is scheduled.
Equivocal results on noninvasive tests in patients at high clinical risk who are to undergo high-risk surgery.
- Class IIa: Multiple markers of intermediate clinical risk when vascular surgery is scheduled (noninvasive testing should be considered first).
Moderate to large ischemia on noninvasive testing, but no high-risk features and no reduced left ventricular ejection fraction.
Nondiagnostic results on noninvasive tests in patients at clinically intermediate risk who are scheduled for high-risk noncardiac surgery.
Urgent noncardiac surgery in patients who are recovering from acute myocardial infarction.
- Class IIb: Perioperative myocardial infarction.
Medically stabilized class III or IV angina when low-risk or minor surgery is scheduled.
- Class III: Low-risk noncardiac surgery in patients who have known coronary artery disease but no high-risk results on noninvasive tests.
No symptoms and excellent exercise capacity (7 METs or more) after coronary revascularization.
Mild stable angina, but good left ventricular function and no high-risk results on noninvasive tests.
Patients who are not candidates for coronary revascularization because of comorbid conditions, severe left ventricular dysfunction (e.g., left ventricular ejection fraction below 0.20), or refusal to undergo the procedure.
As part of the evaluation for liver, lung, or renal transplantation in patients younger than 40 years, unless high risk for an adverse outcome is demon strated on noninvasive testing.
Preoperative Coronary Revascularization and Perioperative Medical Therapy
The indications for coronary artery bypass grafting are the same as those reviewed in the ACC/AHA guideline on the procedure.6
The recommendations for perioperative medical therapy are as follows:
- Class I: Beta-blocker therapy recently required to control symptoms of angina; symptomatic arrhythmias or hypertension.
Beta blockers for patients at high cardiac risk because of ischemia found on preoperative testing who are scheduled for vascular surgery.
- Class IIa: beta blockers if the preoperative evaluation identifies untreated hypertension, coronary disease, or major clinical risk factors for coronary disease.
- Class IIb: alpha2 agonist for perioperative control of hypertension, known coronary artery disease, or major risk factors for coronary artery disease.
- Class III: Contraindication to beta-blocker therapy.
Contraindication to alpha2-agonist therapy.
Postoperative and Long-Term Management
Despite optimal management, perioperative myocardial infarction occurs in some patients. After benefits and risks have been weighed, angioplasty should be considered when symptomatic perioperative ST-segment elevation myocardial infarction occurs because of sudden thrombotic occlusion. Aspirin therapy should be started as soon as possible. Treatment with a beta blocker and angiotensin-converting enzyme inhibitor may also be helpful. Because of the risk of future cardiac events, careful evaluation for residual ischemia and left ventricular dysfunction is necessary when acute myocardial infarction occurs in the perioperative period.
Secondary risk reduction is appropriate when cardiovascular abnormalities are detected during evaluations performed before elective surgery. Most patients with known or newly detected coronary artery disease do not have cardiac events during elective noncardiac surgery. After risk has been determined, patients generally benefit from pharmacologic therapy to lower low-density lipoprotein cholesterol levels, increase high-density lipoprotein cholesterol levels, or both.
The full report of the updated guidelines is available on the ACC and AHA Web sites:www.acc.org/clinical/guidelines/perio/update/pdf/perio_update.pdf andwww.americanheart.Org/downloadable/heart/1013454973885perio_update.pdf.

