Rheumatoid arthritis, juvenile rheumatoid arthritis, Sjögren's syndrome, the seronegative spondyloarthropathies, systemic lupus erythematosus, multiple sclerosis, giant cell arteritis, and Graves' disease are autoimmune disorders commonly encountered by family physicians. These autoimmune disorders can have devastating systemic and ocular effects. Ocular symptoms may include dry or red eyes, foreign-body sensation, pruritus, photophobia, pain, visual changes, and even complete loss of vision. Because a number of these diseases may initially present with ocular symptoms, physicians should maintain a high index of suspicion to make a timely diagnosis. A thorough ophthalmic examination, including visual acuity, pupillary reaction, ocular motility, confrontation field testing, external inspection, and direct ophthalmoscopy with fluorescein staining, should be completed. In the patient with the complaint of a “dry eye” or a “red eye,” simple tools such as the Schirmer's test or the blanching effect of phenylephrine can be useful in diagnosis. In general, managing the systemic effects with nonsteroidal anti-inflammatory drugs, corticosteroids, and immunosuppressive agents controls the ocular symptoms. When visual function is threatened, surgical therapy may be necessary. Early and accurate diagnosis with prompt treatment or referral to an ophthalmologist may prevent systemic and ocular disabilities.
Patients with autoimmune diseases are frequently encountered by family physicians. It is important to understand not only the systemic effects of these diseases but also their ocular manifestations (Table 1). Most ocular complications involve the cornea but may also include the conjunctiva, uvea, sclera, retina, and surrounding structures (Figure 1). The majority of these diseases will ultimately need to be referred to an ophthalmologist.
TABLE 1 Ocular Manifestations of Autoimmune Disease
| Disease | Ocular manifestations |
|---|---|
| Rheumatoid arthritis | Keratoconjunctivitis sicca, scleritis, episcleritis, keratitis, ulcerative keratitis, choroiditis, retinal vasculitis, episcleral nodules, retinal detachments, macular edema |
| Juvenile rheumatoid arthritis | Uveitis |
| Sjögren's syndrome | Keratoconjunctivitis sicca |
| Ankylosing spondylitis | Uveitis |
| Reiter's syndrome | Conjunctivitis, uveitis, keratitis |
| Enteropathic arthritis | Uveitis, episcleritis, peripheral ulcerative keratitis |
| Psoriatic arthritis | Uveitis, conjunctivitis, keratitis |
| Systemic lupus erythematosus | Keratoconjunctivitis sicca, conjunctivitis, uveitis, episcleritis, scleritis, keratitis, retinal hemorrhages, retinal vasculitis, proliferative retinopathy, optic neuritis, ischemic optic neuropathy, hemianopia, amaurosis, internuclear ophthalmoplegia, pupillary abnormalities, oculomotor abnormalities, visual hallucinations |
| Multiple sclerosis | Afferent: optic neuritis, retrobulbar neuritis, visual field defects |
| Efferent: internuclear ophthalmoplegia, dysmetria, nystagmus, cranial nerve palsies | |
| Giant cell arteritis | Amaurosis fugax, diplopia, vision loss |
| Graves' disease | Proptosis/exophthalmos, lid lag and retraction, keratitis, decreased visual acuity, reduced visual fields, relative afferent pupillary defect, loss of color vision |
| Myasthenia gravis | Diplopia, eyelid ptosis |
| Sarcoidosis | Uveitis, conjunctival nodules, cranial nerve palsies, enlarged lacrimal glands, optic neuropathy |
| Wegener's granulomatosis | Proptosis/exophthalmos, orbital cellulitis, uveitis, corneal ulcers, optic neuropathy |
| Behçet's syndrome | Uveitis, hypopyon |
| Antiphospholipid syndrome | Vaso-occlusive retinopathy, ischemic optic neuropathy |
| Polyarteritis nodosa | Episcleritis, scleritis, optic neuropathy |
| Takayasu's arteritis | Vaso-occlusive retinopathy, ischemic optic neuropathy, cataracts |
| Dermatomyositis | Eyelid/conjunctival edema, retinopathy, uveitis |
FIGURE 1.
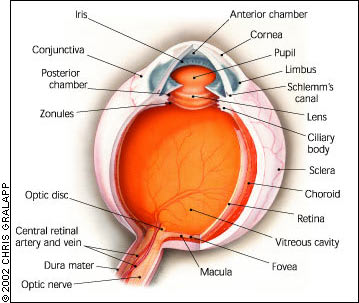
Cross section of the eye.
Rheumatoid Arthritis
Approximately 25 percent of patients with rheumatoid arthritis (RA) will have ocular manifestations. These may include keratoconjunctivitis sicca, scleritis, episcleritis, keratitis, peripheral corneal ulceration, and less common entities such as choroiditis, retinal vasculitis, episcleral nodules, retinal detachments, and macular edema.1,2
Keratoconjunctivitis sicca, or dry eye syndrome, is the most common ocular manifestation of RA and has a reported prevalence of 15 to 25 percent.1,2 Symptoms are historically more prominent during the latter part of the day because of the evaporation of the tear film (Table 2). A simple and easy-to-perform test assessing the function of the lacrimal glands is the Schirmer's test (Figure 2). It is performed by first drying the tear film, then inserting a Schirmer strip into the lower conjunctival cul-de-sac toward the temporal aspect of the lower lid. No anesthetic should be used. After five minutes, if the strip measures less than 10 mm of wetting, the lacrimal glands are not functioning correctly. If a slit lamp is available, corneal examination may reveal punctate erosive keratopathy or filaments.3,4
FIGURE 2.
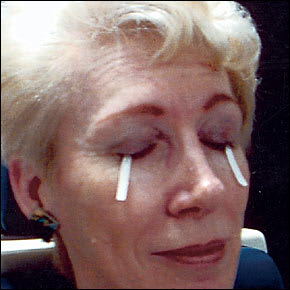
The Schirmer's test is used to assess the function of the lacrimal glands.
The primary goal in managing dry eye is to replenish or preserve the tear film. Patients should be educated about simple measures such as using sunglasses and room humidifiers, and avoiding dry environments before turning to tear substitutes. Natural or artificial tear substitutes can help alleviate more severe symptoms, but most contain preservatives that can be toxic to the cornea.5 In severe cases, occlusion of the lacrimal drainage puncta or tarsorrhaphy will be necessary.
Scleritis (Figure 3) or episcleritis (Figure 4) in patients with RA occurs at a prevalence rate of 4 to 10 percent.1 RA is the most common cause of scleritis, accounting for approximately 18 to 33 percent of cases.1,2,6 Scleritis and episcleritis are distinguished on the basis of anatomy and appearance1,2,7 (Table 2). Symptoms may be similar, but the pain in scleritis is more evident and severe. Tenderness to palpation of the globe can help differentiate the two. After asking the patient to look down with eyelids closed, the physician gently presses the globe. Patients with scleritis have tenderness on palpation, while those with episcleritis do not.
TABLE 2 Ocular Signs and Symptoms in Autoimmune Disease
| Condition | Symptoms | Signs | Treatment |
|---|---|---|---|
| Keratitis | Pain with photophobia, foreign body sensation, tearing, red eye, decreased vision | Inflammatory cell infiltrate, corneal opacification, corneal vascularization, corneal ulceration | NSAIDs, topical/oral/IV steroids, immunosuppressives, surgery |
| Keratoconjunctivitis sicca | Dry eye, burning, pain, blurred vision, pruritus, foreign-body sensation, mucous threads and crusting about the eyelids | Diminished corneal tear meniscus, abnormal Schirmer's test | Sunglasses, room humidifiers, tear substitutes, surgery |
| Scleritis | Gradual onset; deep, boring pain may radiate into cheek, eyebrows, and temples blurred vision; photophobia | Decreased visual acuity; bluish appearance with engorged blood vessels; may have immovable, tender nodules over the sclera, general tenderness on palpation; engorged blood vessels do not blanch with phenylephrine (Neo-Synephrine); avascular areas over the sclera | NSAIDs, topical/oral/IV steroids, immunosuppressives, surgery |
| Episcleritis | Sudden onset; mild ache may radiate into cheek, eyebrows, and temples; no blurred vision; photophobia | No change in visual acuity; bright red appearance with engorged blood vessels; may have movable, nontender nodules over the episclera; no tenderness on palpation; engorged blood vessels blanch with phenylephrine | NSAIDs, topical/oral steroids |
| Uveitis | Red eye, pain, photophobia, blurred vision | Decreased visual acuity, inflammatory infiltrate in the anterior chamber, synechiae, pupillary miosis | Cycloplegics, topical steroids, immunosuppressives |
| Optic neuritis | Visual loss, pain with eye movement, photophobia | Decreased visual acuity, loss of color vision, central scotoma, afferent pupillary defect, swollen optic nerve | IV steroids with positive MRI findings |
| Exophthalmos | Irritable and gritty eyes, double or blurred vision, photophobia, increased tearing, orbital pressure | Protruding globe, widened palpebral fissures, conjunctival injection and chemosis, lid lag and retraction, exposure keratitis | Lubricating eye drops, sleeping with head elevated, sunglasses, eyelid taping at night, steroids, radiotherapy, surgery |
NSAIDs = nonsteroidal anti-inflammatory drugs; IV = intravenous; MRI = magnetic resonance imaging.
FIGURE 3.
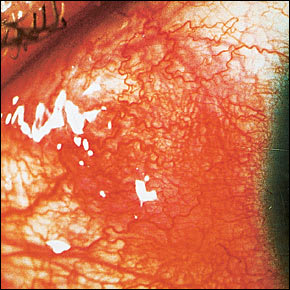
Scleritis. Engorged scleral vessels do not blanch with application of topical phenylephrine 2.5 percent.
FIGURE 4.
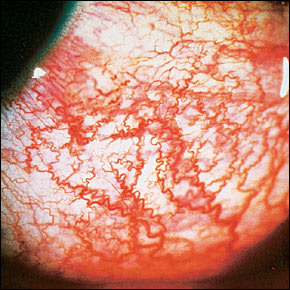
Episcleritis. Engorged episcleral vessels give the eye a bright red appearance. Blanching of the vessels occurs with application of topical phenylephrine 2.5 percent.
Topical phenylephrine 2.5 percent (Neo-Synephrine) can help the physician distinguish dilated vessels caused by scleritis from those caused by episcleritis. The instillation of one to two drops in the affected eye will cause the engorged vessels caused by episcleritis to blanch while those caused by scleritis remain dilated. Patients should be warned that phenylephrine will cause blurred vision and dilation of the pupil for approximately three hours. This test should not be done in patients with a history of glaucoma.
Among the variations of scleritis, necrotizing scleritis with inflammation is the most destructive. In addition to the ocular findings in non-necrotizing scleritis, avascular areas of the sclera or necrosis may be seen, surrounded by scleral edema (Figure 5). Complications include scleral thinning, staphyloma, or perforation.1,7 Necrotizing scleritis without inflammation is a sign of long-standing RA and can lead to scleromalacia perforans (Figure 6).
FIGURE 5.
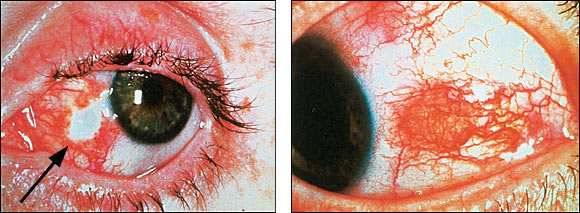
Necrotizing scleritis (left) and scleritis (right). Note the avascular areas of sclera surrounded by edema (arrow).
FIGURE 6.
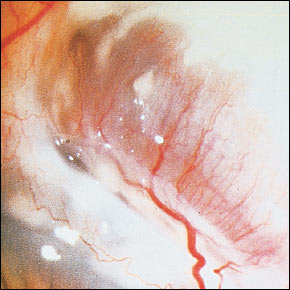
Scleromalacia perforans. Note the thinning of the sclera, which leaves the choroid bare and covered by a thin layer of conjunctiva.
Between the two forms of episcleritis, simple episcleritis is more common in patients with RA. The presence of subconjunctival nodules that are mobile over the sclera differentiates nodular episcleritis from simple episcleritis.1,7 Both forms of episcleritis can be confused with severe conjunctivitis because of the bright-red appearance of the eye and should be differentiated with the help of a thorough history and physical examination.
The importance of correctly diagnosing and distinguishing between scleritis and episcleritis is based on the potential ocular and systemic complications associated with scleritis. Studies have shown that patients with RA-associated scleritis have more widespread systemic disease and a higher mortality rate than those without scleritis.6–8 The initial treatment of scleritis and episcleritis should be focused on relieving discomfort and stopping progression of the disease. Initial therapy includes oral indomethacin (Indocin) or other nonsteroidal anti-inflammatory drugs (NSAIDs). Patients who do not respond to these medications should be referred to an ophthalmologist for possible treatment with topical steroids or systemic immunosuppressive medications.
Corneal disease in patients with RA can be an isolated complication, but it is most commonly associated with keratoconjunctivitis sicca or a form of anterior scleritis. The spectrum of disease may include keratitis, sclerosing keratitis, and peripheral or paracentral ulcerative keratitis1,2,6,7 (Table 2). The drying effects of keratoconjunctivitis sicca lead to devitalized epithelial cells and punctate epithelial erosions. Keratitis associated with scleritis may be acute or sclerosing. Acute keratitis has been identified in 30 to 70 percent of patients with scleritis or episcleritis-associated RA.1,6 It is marked by an inflammatory cell infiltrate that may result in corneal scarring, ulceration, or melting.1,6
Sclerosing keratitis is a chronic process marked by an area of opacified and vascularized cornea that progresses toward the visual axis. This area of opacification may be more evident with fluorescein staining. Peripheral and paracentral ulcerative keratitis can occur in association with, or in the absence of, scleritis and are marked by corneal thinning in the juxtalimbal cornea (peripheral) or the central (paracentral) cornea1,2 (Figure 7). Without treatment, perforation (Figure 8) and visual loss may occur. Care must be taken when prescribing steroids to prevent further thinning of the cornea. It is important that the patient receive a thorough ocular examination with frequent slit lamp follow-up evaluations. Typically, topical steroids, immunosuppressive therapy, surgical intervention, or a combination of the above will be required to preserve vision. Surgical options include ulcer debridement, conjunctival resection, corneal graft, application of tissue adhesives, sclerectomy, and scleral patch grafting.1,2,8
FIGURE 7.
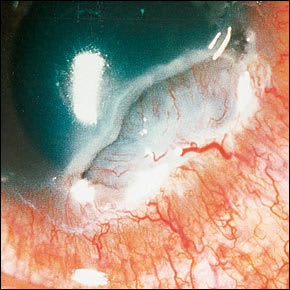
Peripheral corneal ulceration. Note the crescent-shaped destructive inflammation of the juxtalimbal cornea.
FIGURE 8.
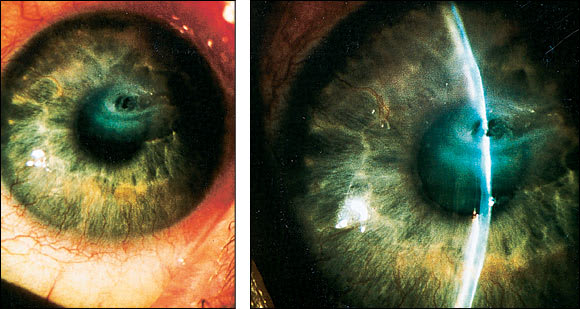
Corneal perforation. Severe tear deficiency leads to breakdown of the corneal epithelial layer.
Other, less common ocular manifestations of RA include choroiditis, retinal vasculitis, episcleral nodules, exudative or serous retinal detachments, and macular edema.1,2,6 A high index of suspicion can preserve vision and prevent further ocular complications.
Juvenile Rheumatoid Arthritis
Juvenile rheumatoid arthritis accounts for approximately 80 percent of cases of uveitis in children.1,2,9 Delay in diagnosis can lead to cataracts, glaucoma, and blindness. Although uveitis can be found in all forms of juvenile RA, it is most commonly found in the pauciarticular subtype. Most patients will be symptom-free or have blurred vision (Table 2). On examination, the patient may have decreased visual acuity, band keratopathy, synechiae (Figure 9), cataracts, or elevated ocular pressure. Diagnosis or suspicion of juvenile RA should prompt a referral to a pediatric ophthalmologist. Recommendations for ocular screening examinations are based on the risk of developing uveitis (Table 3).10 Therapy involves close monitoring by an ophthalmologist, with the use of cycloplegic agents, steroids, NSAIDs, or immunosuppressive agents.1,2
FIGURE 9.
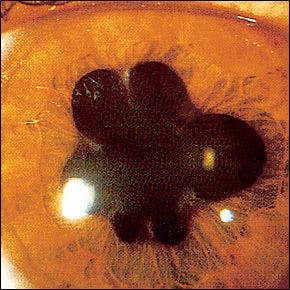
Posterior synechiae caused by adhesion of the iris to the lens, resulting in an irregularly shaped pupil.
TABLE 3 JRA Risk Categories for Developing Uveitis and Recommended Ocular Examinations
| Risk | Recommendations |
|---|---|
| High: should have ocular examination every three months | Pauci- or polyarticular arthritis; positive for antinuclear antibodies |
| Onset of arthritis ≤7 years | |
| Duration of arthritis ≤4 years | |
| Moderate: should have ocular examination every six months | Pauci- or polyarticular arthritis; positive for antinuclear antibodies |
| Onset of arthritis ≤7 years | |
| Duration of arthritis >4 years | |
| Low: should have ocular examination every 12 months | Pauci-, polyarticular, or systemic arthritis; negative for antinuclear antibodies |
| Onset of arthritis >7 years | |
| Duration of arthritis >4 years |
JRA = juvenile rheumatoid arthritis.
Adapted with permission from American Academy of Pediatrics, Subcommittees of Rheumatology and Ophthalmology. Guidelines for ophthalmic examinations in children with juvenile rheumatoid arthritis. Pediatrics 1993;92:295-6.
Sjögren's Syndrome
The primary ocular manifestation of Sjögren's syndrome is keratoconjunctivitis sicca. The signs and symptoms are similar to those of keratoconjunctivitis sicca associated with RA. In addition to the treatment noted above, 5 mg of oral pilocarpine (Salagen) four times daily may improve the symptoms of dry eyes and dry mouth.11,12 [Reference 11, Evidence level A, randomized controlled trial ] Patients should be cautioned that the side effects of diaphoresis and poor night vision may occur.
Spondyloarthropathies
Among the seronegative spondyloarthropathies, uveitis in ankylosing spondylitis is the most common ocular manifestation. It occurs in approximately 25 percent of patients with ankylosing spondylitis, in up to 37 percent of patients with Reiter's syndrome, in approximately 20 percent of patients with psoriatic arthritis, and in up to 9 percent of patients with enteropathic arthritis (arthritis associated with Crohn's disease or ulcerative colitis).2,13–15 Ocular symptoms can be unilateral or bilateral, and pain is caused by ciliary spasm in response to anterior chamber inflammation. As noted earlier, patients suspected of having uveitis should be referred to an ophthalmologist. Complications include glaucoma, cataracts, or blindness.
Systemic Lupus Erythematosus
Ocular disease occurs in 20 percent of patients with systemic lupus erythematosus (SLE). In some cases, ocular disease may indicate reactivation of SLE that was thought to be in remission.16 External ocular manifestations include keratoconjunctivitis sicca, conjunctivitis, uveitis, episcleritis, scleritis, keratitis, and a discoid lupus rash over the eyelids that is often confused with blepharitis.16,17 Neuroophthalmic involvement in SLE is primarily caused by microinfarction, hemorrhage, or vasculitis in various locations of the eye and along the visual pathway. Typical complications include optic neuritis, ischemic optic neuropathy, hemianopia, amaurosis, internuclear ophthalmoplegia, pupillary abnormalities, oculomotor abnormalities, pseudotumor cerebri, and visual hallucinations.16
Retinal disease primarily occurs in patients with active SLE and may include cotton-wool spots (Figure 10), retinal hemorrhages, retinal vasculitis, or proliferative retinopathy. Treatment of ocular disease is based on specific pathology and underlying disease.16 Keratoconjunctivitis sicca is thought to be the most common manifestation and can be treated as noted above.
FIGURE 10.
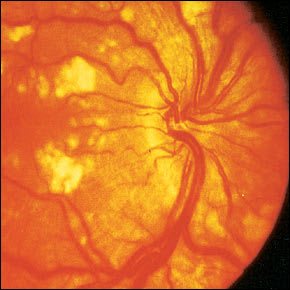
Cotton-wool spots in a patient with systemic lupus erythematosus.
Retinal disease has a high morbidity and should be treated aggressively by an ophthalmologist.16,17 Ophthalmic screening programs in SLE are controversial. Most physicians agree that patients on antimalarial or steroid regimens should receive a full dilated-eye examination on initiation of therapy then with routine examinations in low-risk patients and yearly for high-risk patients. High risk is defined by medication dosage (>6.5 mg per kg hydroxychloroquine or >3 mg per kg chloroquine), duration of use (more than five years), high body fat level, presence of renal or liver disease, presence of concomitant retinal disease, and age greater than 60 years.16,18
Multiple Sclerosis
The ocular manifestations of multiple sclerosis (MS) can be divided into afferent and efferent disorders19 (Table 1). Optic neuritis is diagnosed in 75 percent of patients with MS and is the presenting symptom in 14 to 25 per cent of cases19,20 (Table 2). Visual field defects in patients with MS are a result of demyelination along the visual pathway. Bilateral internuclear ophthalmoplegia is almost always caused by a demyelinating disorder.19 Dysmetria, nystagmus, and cranial nerve palsies, especially involving the sixth and third nerves, may result from lesions of the brain stem and cerebellum.
Nystagmus, which may be the first neurologic finding in patients with MS, is commonly horizontal but may also be rotary or vertical.19 Patients with suspected ocular involvement should receive magnetic resonance imaging (MRI), a full dilated-eye examination, and treatment with intravenous corticosteroids if the MRI is positive.20 Periodic follow-up evaluations should be done to monitor the progression of disease.
Giant Cell Arteritis
Up to 50 percent of patients with giant cell arteritis present with ocular symptoms that include pain, diplopia, visual loss, and amaurosis fugax, in addition to headache, jaw claudication, and neck pain.21,22 It is important to note that ocular involvement is common in the absence of systemic signs and symptoms.21,22 Patients may have temporal artery tenderness or a decreased temporal artery pulse, but diagnosis is confirmed with biopsy of the artery and elevated titers of erythrocyte sedimentation rate and C-reactive protein. Biopsy will remain positive for up to two weeks after the initiation of corticosteroid therapy.21 Intravenous corticosteroids should be used in patients with visual symptoms.21 Immediate therapy can be dramatic in effect and prevent further vasculitic complications, permanent blindness, or death.
Graves' Disease
Exophthalmos (Figure 11) occurs in approximately 50 percent of patients with thyroid disease23 (Table 2). It is strongly associated with smoking and may also be found in patients who are euthyroid or hypothyroid.23 If signs of optic nerve compression, such as decreased visual acuity, reduced visual fields, relative afferent pupillary defect, and loss of color vision are present, computed tomography or MRI of the orbit is recommended.23–25
Patients with suspected ocular disease should be referred to an ophthalmologist for a full dilated ocular examination. Mild ocular disease can be treated with simple methods such as lubrication drops applied hourly, sleeping with the head elevated, wearing sunglasses during the daytime, and taping eyelids closed at night. Systemic corticosteroid therapy or radiotherapy is reserved for more severe cases, and surgical decompression of the orbit or tarsorrhaphy may be required in patients with sudden visual loss or extensive corneal damage, respectively.23,25
Terms and Definitions
| Band keratopathy: calcium deposits in the anterior cornea, usually as a horizontal band within the palpebral fissure Choroiditis: inflammation of the choroid layer of the eye; usually painless but associated with blurred vision; can lead to scarring of the choroid and the retina, with permanent visual loss Dysmetria: multiple small and inaccurate eye movements Episcleritis: inflammation of the episclera, a membrane covering the sclera Hemianopia: defect in one half of the visual field of one or both eyes respecting the vertical midline Hypopyon: an accumulation of inflammatory cells in the anterior chamber producing a layered meniscus in the inferior aspect of the anterior chamber Internuclear ophthalmoplegia: limitation of adduction in one eye with nystagmus in the abducting eye; caused by a lesion in the medial longitudinal fasciculus Iridocyclitis: inflammation of the iris and ciliary body Keratic precipitates: an accumulation of inflammatory materials on the posterior surface of the cornea forming tiny, brownish clumps Keratoconjunctivitis sicca (dry eye): a breakdown in the aqueous (middle) layer of the tear film (normal tear film consists of three layers; the outermost layer is a lipid layer, the middle layer is an aqueous layer, and the innermost layer is a mucous layer). Prolonged dryness can permanently damage the cornea. Macular edema: inflammation of the macula, the area responsible for central vision. Edema is caused by fluid leaking from retinal blood vessels. The condition is painless but associated with visual changes. It may be referred to as cystoid when cyst-like formations are seen in the macula. Paracentral ulcerative keratitis: destructive ulceration of the clear central or paracentral cornea; associated with pain and photophobia Peripheral ulcerative keratitis: a peripheral corneal ulceration associated with a crescent-shaped destructive inflammation of the juxtalimbal cornea, with pain and photophobia Punctuate erosive keratopathy: see superficial punctate keratitis Scleritis: inflammation of the sclera, the white outer surface of the eye Scleromalacia perforans: a thinning of the sclera characterized by yellow or grayish nodules that gradually separate from the underlying sclera, leaving the choroid bare or covered only by a thin layer of conjunctiva Sclerosing keratitis: refers to keratitis associated with scleral disease Staphyloma: protrusion of the cornea or sclera, lined with uveal tissue; may cause visual changes Superficial punctate keratitis: breakdown or damage of the epithelium in a pinpoint pattern; also known as punctate erosive keratopathy or punctate epithelial erosions Uveitis: inflammation of the uvea (iris, ciliary body, and choroid); anterior uveitis refers to the iris and ciliary body and is frequently known as iritis, cyclitis, or iridocyclitis. Uveitis lasting less than three months is referred to as acute while inflammation lasting greater than three months is considered chronic. |

