Herpes zoster ophthalmicus occurs when the varicella-zoster virus is reactivated in the ophthalmic division of the trigeminal nerve. Herpes zoster ophthalmicus represents up to one fourth of all cases of herpes zoster. Most patients with herpes zoster ophthalmicus present with a periorbital vesicular rash distributed according to the affected dermatome. A minority of patients may also develop conjunctivitis, keratitis, uveitis, and ocular cranial-nerve palsies. Permanent sequelae of ophthalmic zoster infection may include chronic ocular inflammation, loss of vision, and debilitating pain. Antiviral medications such as acyclovir, valacyclovir, and famciclovir remain the mainstay of therapy and are most effective in preventing ocular involvement when begun within 72 hours after the onset of the rash. Timely diagnosis and management of herpes zoster ophthalmicus, with referral to an ophthalmologist when ophthalmic involvement is present, are critical in limiting visual morbidity.
Herpes zoster is a common infection caused by the human herpesvirus 3, the same virus that causes varicella (i.e., chickenpox). It is a member of the same family (Herpesviridae) as herpes simplex virus, Epstein-Barr virus, and cytomegalovirus. Reactivation of the latent virus in neurosensory ganglia produces the characteristic manifestations of herpes zoster, commonly known as shingles. Normal aging, poor nutrition, and immunocompromised status correlate with outbreaks of herpes zoster, and certain factors such as physical or emotional stress and fatigue may precipitate an episode.
Herpes zoster ophthalmicus occurs when reactivation of the latent virus in the trigeminal ganglia involves the ophthalmic division of the nerve. The virus damages the eye and surrounding structures by secondary perineural and intraneural inflammation of sensory nerves.1 Herpes zoster ophthalmicus represents approximately 10 to 25 percent of all cases of herpes zoster.2 Although herpes zoster ophthalmicus most often produces a classic dermatomal rash, a minority of patients may have only ophthalmic findings, limited mainly to the cornea. Direct ocular involvement is not specifically correlated with age, gender, or severity of disease. Serious sequelae include chronic ocular inflammation, vision loss, and disabling pain.
Extraocular Manifestations of Herpes Zoster Ophthalmicus
The prodromal phase of herpes zoster ophthalmicus includes an influenza-like illness with fatigue, malaise, and low-grade fever that lasts up to one week before the rash over the forehead appears.3 About 60 percent of patients have varying degrees of dermatomal pain in the distribution of the ophthalmic nerve.4 Subsequently, erythematous macules appear along the involved dermatome, rapidly progressing over several days to papules and vesicles containing clear serous fluid and, later, pustules. These lesions rupture and typically crust over, requiring several weeks to heal completely.5
Immunocompromised persons, particularly those with human immunodeficiency virus infection, have a much higher risk of developing herpes zoster ophthalmicus than the normal population.6 These patients may have a generalized vesicular rash and become severely ill one to two weeks after disease onset. In addition, such patients develop more serious visual sequelae.7
Viral transmission from patients with herpes zoster can occur, but it is less frequent than transmission from patients with chick-enpox.7 Virus particles can be transmitted through direct contact with secretions from vesicles and secretion-contaminated articles.
Ocular Manifestations of Herpes Zoster Ophthalmicus
The skin manifestations of herpes zoster ophthalmicus strictly obey the midline with involvement of one or more branches of the ophthalmic division of the trigeminal nerve, namely the supraorbital, lacrimal, and nasociliary branches (Figure 1). Because the nasociliary branch innervates the globe, the most serious ocular involvement develops if this branch is affected. Classically, involvement of the tip of the nose (Hutchinson's sign) has been thought to be a clinical predictor of ocular involvement. Although patients with a positive Hutchinson's sign have twice the incidence of ocular involvement, one third of patients without the sign develop ocular manifestations.8 A summary of ocular findings in patients with herpes zoster ophthalmicus is presented in Table 1.
FIGURE 1.
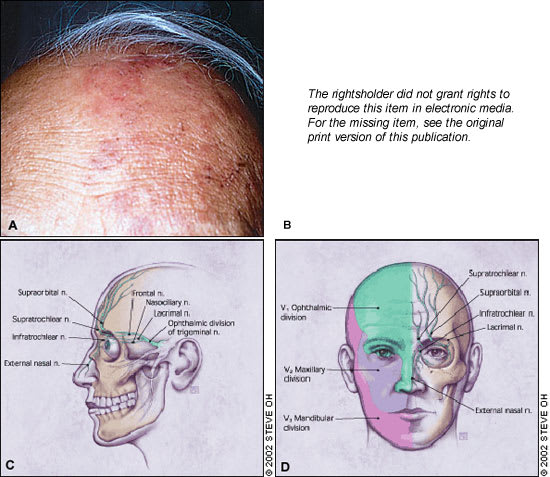
The hallmark of herpes zoster ophthalmicus is a vesicular rash that involves the first (ophthalmic) division of the fifth cranial nerve that presents in a dermatomal distribution and respects the midline (a). The upper eyelid is commonly involved with edema, inflammation, and resultant ptosis (b). The sensory distribution of the ophthalmic (V1) division of the trigeminal nerve (c,d).
TABLE 1 Ocular and Cranial Nerve Involvement in Herpes Zoster Ophthalmicus
| Structure involved | Signs | Time of onset (onset of rash = Day 0) |
|---|---|---|
| Eyelid/conjunctiva | ||
| Blepharoconjunctivitis | Cutaneous macular rash respecting midline and involving eyelids | Day 0 (preceded by dermatomal pain) |
| Conjunctival edema/inflammation | Two to three days | |
| Vesicular lesions/crusting | Six days | |
| Secondary Staphylococcus aureus infection | Yellowish crusting/discharge | One to two weeks |
| Episclera/sclera | ||
| Episcleritis/scleritis | Diffuse or localized redness, pain, and swelling | One week |
| Cornea | ||
| Punctate epithelial keratitis | Swollen corneal surface epithelial cells | One to two days |
| Dendritic keratitis | “Medusa-like” epithelial defect with tapered ends | Four to six days |
| Anterior stromal keratitis (nummular keratitis) | Multiple fine infiltrates immediately beneath corneal surface | One to two weeks |
| Deep stromal keratitis | Deep stromal inflammation with lipid infiltrates and corneal neovascularization | One month to years |
| Neurotrophic keratopathy | Punctate corneal surface erosions | Months to years |
| Persistent epithelial defects | ||
| Corneal ulcers | ||
| Anterior chamber | ||
| Uveitis | Inflammation and iris scarring | Two weeks to years |
| Retina | ||
| Acute retinal necrosis/progressive outer retinal necrosis | Coalescent patches of retinal necrosis | Independent/varied* |
| Occlusive vasculitis | ||
| Vitreous inflammation (acute retinal necrosis only) | ||
| Cranial nerves | ||
| Optic neuritis | Swollen, edematous optic nerve head | Independent/varied* |
| Oculomotor palsies | Extraocular motion abnormalities | Independent/varied* |
*— These syndromes may not be associated with acute herpes zoster ophthalmicus infection and/or can precede or follow at any time.
BLEPHARITIS AND CONJUNCTIVITIS
The eyelids are commonly involved in herpes zoster ophthalmicus ( Figure 1, part b). Patients may develop blepharitis and present with ptosis secondary to edema and inflammation. A vast majority of patients will have vesicular lesions on the eyelids that resolve with minimal scarring.
Conjunctivitis is one of the most common complications of herpes zoster ophthalmicus. The conjunctiva appears injected and edematous, often with petechial hemorrhages.9 The findings usually resolve within one week. However, secondary infection, usually Staphylococcus aureus, may develop and should be treated with broad-spectrum topical and/or systemic antibiotics.
CORNEAL DISEASE
Unlike eyelid or conjunctival involvement, corneal involvement can result in significant vision loss. The clinical features of corneal disease include direct viral infection, antigen-antibody reactions, delayed cell-mediated hypersensitivity reactions, and neurotrophic damage.7 Patients with corneal disease present with varying degrees of decreased vision, pain, and light sensitivity. Corneal complications occur in approximately 65 percent of cases of herpes zoster ophthalmicus.7
Epithelial Keratitis. The earliest corneal finding is punctate epithelial keratitis.10 On slit lamp examination, this appears as multiple, focal, swollen lesions that stain with rose bengal or fluorescein dye. These lesions probably contain live virus and may either resolve or progress to dendrite formation. Punctate epithelial keratitis may present as early as one or two days after the initial skin rash, while dendrites often present at four to six days but can appear many weeks later.11
Herpes zoster virus dendrites appear as elevated plaques and consist of swollen epithelial cells. They form branching or “medusa-like” patterns and have tapered ends ( Figure 2, part a) in contrast to herpes simplex virus dendrites, which often have terminal bulbs. Dendrites also stain with rose bengal and fluorescein dye ( Figure 2, part b) and can be viewed by Wood's lamp or slit lamp examination. Punctate and dendritic lesions can lead to anterior stromal corneal infiltrates.11,12
FIGURE 2.
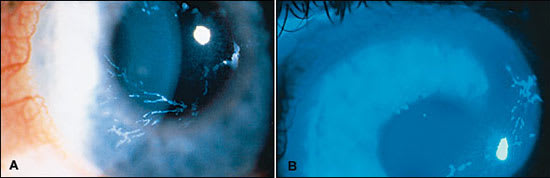
Slit lamp examination in a patient with herpes zoster ophthalmicus. Epithelial keratitis may have a dendritic appearance mimicking herpes simplex virus keratitis (a) and stains with fluorescein dye (b).
Stromal Keratitis— Anterior Stromal Keratitis. The earliest finding of corneal stromal involvement presents during the second week of disease, occurring in 25 to 30 percent of patients with herpes zoster ophthalmicus.13 The condition, known as anterior stromal keratitis or nummular keratitis, is characterized by multiple fine granular infiltrates in the anterior corneal stroma below the epithelial layer (Figure 3). Most of the infiltrates lie directly beneath pre-existing dendrites or areas of punctate epithelial keratitis. The infiltrates are thought to arise from antigen-antibody interaction resulting from viral proliferation in the overlying epithelium.10,12 Anterior stromal keratitis may be prolonged and recurrent.
FIGURE 3.
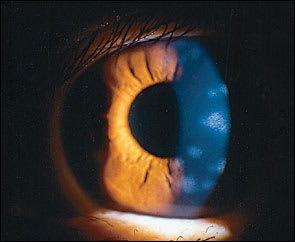
Slit lamp examination of a patient with nummular keratitis as a result of herpes zoster virus infection. Subepithelial infiltrates are located in the anterior stroma below areas of previous epithelial keratitis.
Stromal Keratitis—Deep Stromal Keratitis. This later stage of stromal keratitis is relatively uncommon and typically develops three to four months after the initial acute episode, but development can range from one month to many years later.7 It is usually central and preceded by anterior stromal keratitis. The keratitis may present as a lesion consisting of a localized area of inflammation affecting all levels of the stroma, or as peripheral infiltrates that may have a surrounding immune ring. Corneal edema may be a prominent feature at this stage, usually with associated anterior chamber inflammation. A rare necrotizing form can also occur. A chronic relapsing course is not unusual, especially without timely and adequate treatment. Corneal neovascularization and lipid infiltrates may occur in patients with uncontrolled chronic disease. The pathogenesis of stromal disease probably involves a delayed cell-mediated hypersensitivity reaction.
Neurotrophic Keratopathy. Neurotrophic keratitis is the end result of decreased corneal sensation from herpes zoster virus-mediated destruction, including susceptibility to mechanical trauma, decreased lacrimation, and delayed epithelial healing.7 Corneal thinning is a serious complication that may lead to corneal perforation. Such patients are at high risk for developing a secondary bacterial infection. Using preservative-free lubricating drops and ointment can prevent the development of epithelial defects.
UVEITIS
Anterior uveitis, which is diagnosed by slit lamp examination, refers to inflammation of the iris and ciliary body and occurs frequently with herpes zoster ophthalmicus. It may be isolated or associated with keratitis. The inflammation is generally mild and transient, but it frequently causes a mild elevation in intraocular pressure. Zoster uveitis can result in iris atrophy and an irregular pupil. As with stromal keratitis, the course of disease may be prolonged, especially without timely, adequate treatment. Herpes zoster uveitis may cause glaucoma and cataract formation. Chronic inflammation can lead to endothelial cell injury, resulting in corneal edema.
EPISCLERITIS AND SCLERITIS
Findings of episcleritis include localized or diffuse redness, as well as pain and swelling of the conjunctiva and episclera. Scleritis is a more serious condition with involvement of the sclera. Both conditions may be accompanied by localized stromal keratitis.
ACUTE RETINAL NECROSIS AND PROGRESSIVE OUTER RETINAL NECROSIS SYNDROMES
Herpes zoster virus is considered the offending agent in most cases of acute retinal necrosis and progressive outer retinal necrosis syndromes. Compared with acute retinal necrosis, progressive outer retinal necrosis is a more severe viral retinitis observed in immunocompromised persons, often in patients with acquired immunodeficiency syndrome.
Symptoms include blurred vision and/or pain in one or both eyes. Acute retinal necrosis is characterized by peripheral patches of retinal necrosis that rapidly coalesce (Figure 4), occlusive vasculitis, and vitreous inflammation. Conversely, immunocompromised patients with progressive outer retinal necrosis are unable to mount a vitreous inflammatory response, leading to rapid involvement of the macula. Both conditions commonly cause retinal detachment. The prognosis is extremely poor in patients with progressive outer retinal necrosis; most patients have no light perception vision.14 The visual prognosis in patients with acute retinal necrosis is better, with many patients achieving a visual acuity of 20/40.15 Bilateral involvement in both forms is observed in one third of patients but may be as high as 70 percent in patients with untreated disease.16 Treatment includes long courses of oral and intravenous acyclovir (Zovirax), and corticosteroids.
FIGURE 4.
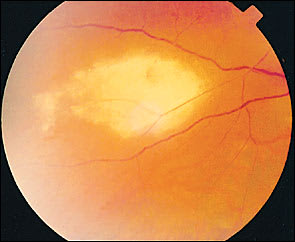
Zoster retinitis characterized by peripheral patches of retinal necrosis.
Postherpetic Neuralgia and Other Neurologic Complications
Postherpetic neuralgia affects about 7 percent of patients and is characterized by varying degrees of constant or intermittent pain in the distribution of the affected dermatome.17 Increased age and prodromal symptoms are associated with a higher prevalence of post-herpetic neuralgia. It generally improves with time but may last for months to years. In severe cases, patients may be depressed and suicidal. Treatment includes topical capsaicin cream, over-the-counter analgesics, tricyclic antidepressants, and anticonvulsants.18
Cranial nerve palsies involving the third (most common), fourth, and sixth nerves may occur rarely (Figure 5). A majority of the cases will have spontaneous resolution within six months. Optic neuritis has been noted in about one in 400 cases and may precede retinal disease or follow acute herpes zoster ophthalmicus infection (Figure 6).17,19,20
FIGURE 6.
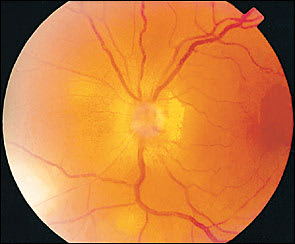
Edema and swelling of the optic nerve in a patient who had concomitant zoster retinitis.
Treatment of Herpes Zoster Ophthalmicus
Patients with herpes zoster ophthalmicus are treated with oral acyclovir (800 mg, five times daily) for seven to 10 days. Studies report alleviation of pain with oral acyclovir during the initial stages of the disease, especially if the drug is taken within the first three days of symptoms, and it may have a favorable effect on postherpetic neuralgia.21–23 [Reference 22—Evidence level A, randomized controlled tiral (RCT). Reference 23—Evidence level A, RCT] Additionally, acyclovir administered within 72 hours of onset has been found to speed resolution of skin lesions, reduce viral shedding, and decrease the incidence of dendritic and stromal keratitis as well as anterior uveitis.24,25
Valacyclovir (Valtrex) has higher bioavail-ability and has been shown to be equally safe and effective for the treatment of herpes zoster at a dosage of 1,000 mg three times daily for seven or 14 days.26 [Evidence level A, RCT] Valacyclovir in a seven-day dosage regimen was recently shown to prevent ocular complications of herpes zoster ophthalmicus, including conjunctivitis, superficial and stromal keratitis, and pain.27 [Evidence level A, RCT] Famciclovir (Famvir), 500 mg orally three times a day for seven days, may also be used.28 Intravenous acyclovir is recommended in immunocompromised patients.29,30 [Reference 29—Evidence level A, RCT] Acute pain control is achieved by local care and oral analgesics. Topical anesthetics should never be prescribed because of their corneal toxicity. A summary of treatment and management options for various ocular manifestations of herpes zoster ophthalmicus is presented in Table 2.

