The Recommended Adult Immunization Schedule1 for persons 19 years and older is the first harmonized schedule jointly approved by the Advisory Committee on Immunization Practices (ACIP), the American Academy of Family Physicians (AAFP), and the American College of Obstetricians and Gynecologists (ACOG). This schedule was developed in collaboration with members of AAFP, ACOG, the American College of Physicians/American Society of Internal Medicine (ACP-ASIM), ACIP, and the Centers for Disease Control and Prevention (CDC). Currently, the schedule is being reviewed by other adult health care organizations. The adult working group of the ACIP will annually review and update this schedule and provide recommendations to the ACIP and other organizations for their annual approval.
Similar to the Recommended Childhood Immunization Schedule,2 the Recommended Adult Immunization Schedule (Figure 1) provides age-based recommendations for routine vaccinations in a color-coded chart. In addition, it contains a color-coded chart that summarizes the recommendations and some contraindications of eight vaccines for adults with various medical conditions (Figure 2). The footnotes are summaries of the ACIP recommendations and also reflect any differences between health care organizations on use of these vaccines.
FIGURE 1. Recommended Adult Immunization Schedule, United States, 2002–2003
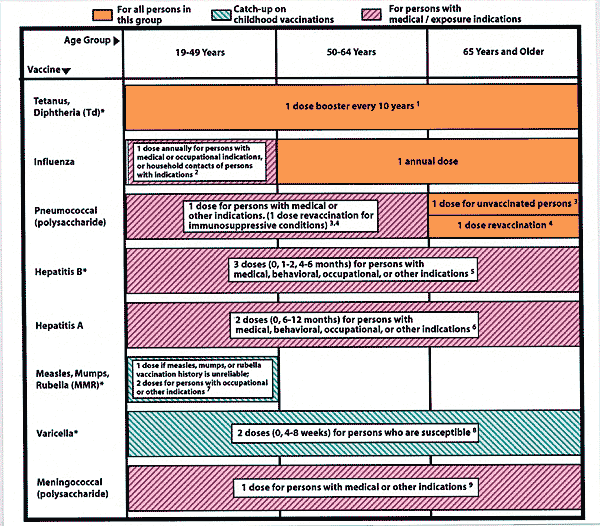
1. Tetanus and diphtheria (Td)—A primary series for adults is 3 doses: the first 2 doses given at least 4 weeks apart and the third dose, 6 to 12 months after the second. Administer 1 dose if the person had received the primary series and the last vaccination was 10 years ago or longer. MMWR 1991;40(RR-10):1–21. The ACP Task Force on Adult Immunization supports a second option: a single Td booster at age 50 years for persons who have completed the full pediatric series, including the teenage/young adult booster. Guide for Adult Immunization. 3rd ed. ACP 1994:20.
2. Influenza vaccination—Medical indications: chronic disorders of the cardiovascular or pulmonary systems including asthma; chronic metabolic diseases including diabetes mellitus, renal dysfunction, hemoglobinopathies, immunosuppression (including immunosuppression caused by medications or by human immunodeficiency virus [HIV]), requiring regular medical follow-up or hospitalization during the preceding year; women who will be in the second or third trimester of pregnancy during the influenza season. Occupational indications: health care workers. Other indications: residents of nursing homes and other long-term care facilities; persons likely to transmit influenza to persons at high risk (in-home caregivers to persons with medical indications, household contacts and out-of-home caregivers of children birth to 23 months of age, or children with asthma or other indicator conditions for influenza vaccination, household members and caregivers of elderly and adults with high-risk conditions); and anyone who wishes to be vaccinated. MMWR 2002;51(RR-3):1–31.
3. Pneumococcal polysaccharide vaccination—Medical indications: chronic disorders of the pulmonary system (excluding asthma), cardiovascular diseases, diabetes mellitus, chronic liver diseases including liver disease as a result of alcohol abuse (e.g., cirrhosis), chronic renal failure or nephrotic syndrome, functional or anatomic asplenia (e.g., sickle cell disease or splenectomy), immunosuppressive conditions (e.g., congenital immunodeficiency, HIV infection, leukemia, lymphoma, multiple myeloma, Hodgkin's disease, generalized malignancy, organ or bone marrow transplantation), chemotherapy with alkylating agents, antimetabolites, or long-term systemic corticosteroids. Geographic/other indications: Alaskan Natives and certain American Indian populations. Other indications: residents of nursing homes and other long-term care facilities. MMWR 1997;47(RR-8):1–24.
4. Revaccination with pneumococcal polysaccharide vaccine—One-time revaccination after 5 years for persons with chronic renal failure or nephrotic syndrome, functional or anatomic asplenia (e.g., sickle cell disease or splenectomy), immunosuppressive conditions (e.g., congenital immunodeficiency, HIV infection, leukemia, lymphoma, multiple myeloma, Hodgkin's disease, generalized malignancy, organ or bone marrow transplantation), chemotherapy with alkylating agents, antimetabolites, or long-term systemic corticosteroids. For persons 65 years and older, one-time revaccination if they were vaccinated 5 or more years previously and were younger than 65 years at the time of primary vaccination. MMWR 1997;47(RR-8):1–24.
5. Hepatitis B vaccination—Medical conditions: hemodialysis patients, patients who receive clotting-factor concentrates. Occupational indications: health care workers and public safety workers who have exposure to blood in the workplace, persons in training in schools of medicine, dentistry, nursing, laboratory technology, and other allied health professions. Behavioral indications: injecting drug users, persons with more than one sex partner in the previous 6 months, persons with a recently acquired sexually transmitted disease (STD), all clients in STD clinics, men who have sex with men. Other indications: household contacts and sex partners of persons with chronic hepatitis B virus (HBV) infection, clients and staff of institutions for the developmentally disabled, international travelers who will be in countries with high or intermediate prevalence of chronic HBV infection for more than 6 months, inmates of correctional facilities. MMWR 1991;40(RR-13):1–25. (www.cdc.gov/travel/diseases/hbv.htm)
6. Hepatitis A vaccination—For the combined HepA-HepB vaccine use (3 doses at 0, 1, and 6 months). Medical indications: persons with clotting-factor disorders or chronic liver disease. Behavioral indications: men who have sex with men, users of injecting and noninjecting illegal drugs. Occupational indications: persons working with hepatitis A virus (HAV)-infected primates or with HAV in a research laboratory setting. Other indications: persons traveling to or working in countries that have high or intermediate endemicity of hepatitis A. MMWR 1999;48(RR-12):1–37. (www.cdc.gov/travel/diseases/hav.htm)
7. Measles, Mumps, Rubella vaccination (MMR)—Measles component: Adults born before 1957 may be considered to be immune to measles. Adults born in or after 1957 should receive at least one dose of MMR unless they have a medical contraindication, documentation of at least one dose or other acceptable evidence of immunity. A second dose of MMR is recommended for adults who:
are recently exposed to measles or in an outbreak setting • were previously vaccinated with killed measles vaccinewere vaccinated with an unknown vaccine between 1963 and 1967 • are students in post-secondary educational institutionswork in health care facilitiesplan to travel internationally
Mumps component: 1 dose of MMR should be adequate for protection. Rubella component: Give 1 dose of MMR to women whose rubella vaccination history is unreliable, and counsel women to avoid becoming pregnant for 4 weeks after vaccination. For women of child-bearing age, regardless of birth year, routinely determine rubella immunity and counsel women about congenital rubella syndrome. Do not vaccinate pregnant women or those planning to become pregnant in the next 4 weeks. If pregnant and susceptible, vaccinate as early in the postpartum period as possible. MMWR 1998;47(RR-8):1–57.
8. Varicella vaccination—Recommended for all persons who do not have reliable clinical history of varicella infection, or serologic evidence of varicella zoster virus (VZV) infection; health care workers and family contacts of immunocompromised persons, those who live or work in environments where transmission is likely (e.g., teachers of young children, day care employees, and residents and staff members in institutional settings), persons who live or work in environments where VZV transmission can occur (e.g., college students, inmates and staff members of correctional institutions, and military personnel), adolescents and adults living in households with children, women who are not pregnant but who may become pregnant in the future, international travelers who are not immune to infections. Note: Greater than 90 percent of U.S. born adults are immune to VZV. Do not vaccinate pregnant women or those planning to become pregnant in the next 4 weeks. If pregnant and susceptible, vaccinate as early in the postpartum period as possible. MMWR 1996;45(RR-11):1–36, MMWR 1999;48(RR-6):1–5.
9. Meningococcal vaccine (quadrivalent polysaccharide for serogroups A, C, Y, and W-135)—Consider vaccination for persons with medical indications: adults with terminal complement component deficiencies, with anatomic or functional asplenia. Other indications: travelers to countries in which disease is hyperendemic or epidemic (“meningitis belt” of sub-Saharan Africa, Mecca, Saudi Arabia for Hajj). Revaccination at 3 to 5 years may be indicated for persons at high risk for infection (e.g., persons residing in areas in which disease is epidemic). Counsel college freshmen, especially those who live in dormitories, regarding meningococcal disease and the vaccine so that they can make an educated decision about receiving the vaccination. MMWR 2000;49(RR-7):1–20.
note: The AAFP recommends that colleges should take the lead on providing education on meningococcal infection and vaccination and offer it to those who are interested. Physicians need not initiate discussion of the meningococcal quadrivalent polysaccharide vaccine as part of routine medical care.
*—Covered by the Vaccine Injury Compensation Program. For information on how to file a claim, call 800-338-2382. Please also visitwww.hrsa.gov/osp/vicp. To file a claim for vaccine injury, write: U.S. Court of Federal Claims, 717 Madison Place, N.W., Washington, D.C. 20005. 202-219-9657.
This schedule indicates the recommended age groups for routine administration of currently licensed vaccines for persons 19 years and older. Licensed combination vaccines may be used whenever any components of the combination are indicated and the vaccine's other components are not contraindicated. Providers should consult the manufacturers' package inserts for detailed recommendations.
Report all clinically significant postvaccination reactions to the Vaccine Adverse Event Reporting System (VAERS). Reporting forms and instructions on filing a VAERS report are available by calling 800-822-7967 or from the VAERS web site atwww.vaers.hhs.gov.
For additional information about the vaccines listed above and contraindications for immunization, visit the National Immunization Program Web site atwww.cdc.gov/nip or call the National Immunization Hotline at 800-232-2522 (English) or 800-232-0233 (Spanish).
Approved by the Advisory Committee on Immunization Practices (ACIP), and accepted by the American College of Obstetricians and Gynecologists (ACOG) and the American Academy of Family Physicians (AAFP).
The success of the childhood immunization program is partly because of the annual publication of the Recommended Childhood Immunization Schedule that summarizes the current recommendations and that it can be posted in the office for quick reference. We suggest that physicians post the Recommended Adult Immunization Schedule in the office as a quick reference tool and that it be used as part of a larger office-based program to improve adult immunization rates.
One of the key immunizations on the schedule is the influenza vaccine. Taken together, influenza and pneumonia are the sixth leading cause of death nationally and the fifth leading cause in older adults. The fatality rate from influenza begins to rise in midlife and is highest in persons who have chronic medical conditions, such as chronic obstructive lung disease, cardiovascular disease, and diabetes mellitus, particularly if they are elderly. Many persons 50 to 64 years of age have a high-risk condition such as asthma, diabetes mellitus, or heart disease, but only a minority are vaccinated, despite recommendations that they should be.
Data from the 2000 National Health Interview Survey (www.cdc.gov/nchs/nhis.htm) show that only 32 percent of those 50 through 64 years of age who are at high risk for complications from influenza were vaccinated. Manual or computerized reminder systems based on high-risk conditions are more difficult to implement than those based on age. Many persons with a high-risk condition do not know that they have a high-risk condition, and high-risk vaccination strategies for other immunizations have had limited success. After considering these factors, the burden of influenza disease, and the cost-effectiveness of vaccination, in 1999 the AAFP became the first to lower the age for annual, routine influenza vaccination to age 50, a position that is now supported by other organizations.
FIGURE 2. Recommended Immunizations for Adults with Medical Conditions, United States, 2002–2003
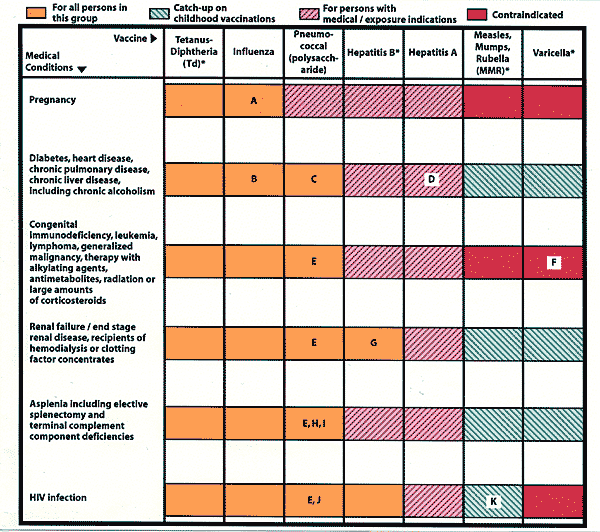
A. If pregnancy is at second or third trimester during influenza season.
B. Although chronic liver disease and alcoholism are not indicator conditions for influenza vaccination, give 1 dose annually if the patient is 50 years or older, has other indications for influenza vaccine, or if the patient requests vaccination.
C. Asthma is an indicator condition for influenza but not for pneumococcal vaccination.
D. For all persons with chronic liver disease.
E. Revaccinate once after 5 years or more have elapsed since initial vaccination.
F. Persons with impaired humoral but not cellular immunity may be vaccinated. MMWR 1999;48(RR-06):1–5.
G. Hemodialysis patients: Use special formulation of vaccine (40 mcg per mL) or two 1.0 mL per 20 mcg doses given at one site. Vaccinate early in the course of renal disease. Assess antibody titers to hepatitis B surface antigen (anti-HBs) levels annually. Administer additional doses if anti-HBs levels decline to less than 10 milli-international units (mIU)/mL.
H. Also administer meningococcal vaccine.
I. Elective splenectomy: vaccinate at least 2 weeks before surgery.
J. Vaccinate as close to diagnosis as possible when CD4 cell counts are highest.
K. Withhold MMR or other measles containing vaccines from HIV-infected persons with evidence of severe immunosuppression. MMWR 1996;45:603–606, MMWR 1992;41(RR-17):1–19.
Before vaccination, physicians should provide the patient with information about the benefits and the risks of adverse events of each vaccine to be administered. When administering any vaccine containing diphtheria, tetanus, pertussis, measles, mumps, rubella, poliovirus, varicella, hepatitis B, or Haemophilus influenzae type b antigens, the health care clinician is required to provide a copy of the relevant Vaccine Information Statement (VIS) to the patient before the vaccination. If there is not a VIS available for the vaccine being administered, the clinician should explain the risks of the disease, the protection afforded from the vaccination, the risk of vaccine adverse events, and what to do if a serious adverse event occurs.3 The following Web sites list every available VIS in multiple languages, which may be downloaded:www.cdc.gov/nip/publications/VIS/default.htm orwww.immunize.org/vis/index.htm. Physicians should report postvaccination adverse events to the Vaccine Adverse Event Reporting System, telephone: 800-822-7967.
Useful Web sites for current information include:www.immunizationed.org, a site developed by family physician educators, which will include free personal digital assistant software applications of the adult schedule;www.immunize.org;https://www.aafp.org/patient-care/clinical-recommendations/all/immunizations.html, which contains AAFP clinical policies on immunization;www.cdc.gov/nip; andwww.immunizationinfo.org.
The Recommended Adult Immunization Schedule complements the Recommended Childhood Immunization Schedule. Together, the two schedules provide a comprehensive summary of recommendations for prevention of vaccine-preventable diseases for Americans throughout their lifespan.

