Exercise-induced bronchospasm is an obstruction of transient airflow that usually occurs five to 15 minutes after physical exertion. Although this condition is highly preventable, it is still underrecognized and affects aerobic fitness and quality of life. Diagnosis is based on the results of a detailed history, including assessment of asthma triggers, symptoms suggestive of exercise-induced bronchoconstriction, and a normal forced expiratory volume at one second at rest. A trial of therapy with an inhaled beta agonist may be instituted, with the subsequent addition of inhaled anti-inflammatory agents or ipratropium bromide. Nonpharmacologic measures, such as increased physical conditioning, warm-up exercises, and covering the mouth and nose, should be instituted. If symptoms persist, pulmonary function testing is warranted to rule out underlying lung disease.
The National Asthma Education and Prevention Program1 is a comprehensive statement of guidelines for the diagnosis and managemen of asthma. The expert panel1 uses the term exercise-induced bronchospasm (EIB) to describe a condition defined as the presence of symptoms in relation to athletic performance or a significant decrease in forced expiratory volume at one second (FEV1) in relation to exercise. Typically, EIB begins after several minutes of vigorous physical activity and reaches its peak in five to 10 minutes.
Epidemiology
Exercise-induced bronchospasm is caused by the loss of heat, water, or both from the lungs during exercise, stemming from hyperventilation of air that is drier and cooler than that in the respiratory tree. Between 80 and 90 percent of patients with asthma also have EIB.2 However, many patients have bronchospasm only during exercise. One study3 has found unrecognized EIB in as many as 29 percent of athletes presenting for athletic preparticipation examinations.
Diagnosis
The diagnosis of EIB is based on a detailed history suggestive of shortness of breath, decreased exercise endurance, chest tightness, cough, or wheezing during or immediately following sustained exercise (Table 1). Some patients also report having an upset stomach or a sore throat. Symptoms that occur during the first five minutes of exercise are usually not indicative of EIB; however, these symptoms may suggest other changes in pulmonary function, poorly controlled underlying asthma, poor conditioning, or injury to the chest wall muscle. Persons who engage in physical activities that involve only short bursts of exertion may perform well without becoming symptomatic. A detailed history should be obtained from family, coaches, and teammates, if possible, because the athlete may deny symptoms as a result of peer pressure or concerns about potential inadequacy or the inability to continue playing.
TABLE 1 Symptoms of Exercise-Induced Bronchospasm
| Shortness of breath or wheezing |
| Decreased exercise endurance |
| Chest pain or tightness with exercise |
| Cough |
| Upset stomach or stomachache |
| Sore throat |
note:Symptoms must occur during or following exercise of at least five minutes' duration.
Most patients with EIB have a normal physical examination, with no evidence of wheezing on auscultation. Nevertheless, a focused physical examination should be performed to exclude sinusitis, nasal polyps, a deviated septum, or vocal cord dysfunction.
The most objective measure of EIB is a pulmonary function test coupled with an appropriate exercise challenge (Table 2).4 However, full pulmonary function testing is rarely required. If symptoms are strongly suggestive of EIB, a trial of therapy using a short-acting bronchodilator may be useful to see if the patient significantly improves in performance and symptoms.
Management
The goal of management is to prevent or reduce the symptoms of EIB, to enable patients to exercise at all intensity levels without serious respiratory limitations. Interventions should be tailored to the patient; a school-aged child participating in recreational and school activities should be treated differently from an elite athlete. Persons should not be excluded from participating in sports or working at jobs with heavy physical demand based solely on EIB. For example, in a study of U.S. Army recruits,5 EIB symptoms did not hinder physical performance gains, even during basic training.
NONPHARMACOLOGIC THERAPY
Patients, and anyone involved in their care, should be educated about the nature of EIB, its triggers, and how to control it with or without medications. Table 3 lists simple nonpharmacologic methods for reducing the likelihood of EIB.6
Physical conditioning increases a patient's ability to work at a lower level of vital ca TABLE 3Nonpharmacologic Treatment Measures for Exercise-Induced Bronchospasm
Increase physical conditioning.
Warm up for at least 10 minutes before actual exercise begins.
Cover mouth and nose with scarf or mask during cold weather.
Exercise in warm, humidified environment, if possible.
Avoid aeroallergens and pollutants.
Cool down or gradually lower the intensity of the exercise before stopping.
Wait at least two hours after a meal before exercising.
Adapted with permission from Tan RA, Spector SL. Exercise induced asthma. Sports Med 1998;25:4.
pacity, decreasing the cooling and drying stimuli, resulting in less bronchospasm.7 Athletes should always warm up before vigorous exercise and take advantage of a “refractory period” induced by short bursts of exercise.7,8 Awareness of environmental allergens such as pollen or animal dander can prevent concomitant aggravation of asthma by allergens and exercise.
PHARMACOLOGIC THERAPY
Considerable data show that most asthma medications can effectively control EIB. Figure 1 is a comprehensive management algorithm that incorporates diagnostic and therapeutic issues.
FIGURE 1. Management of Exercise-Induced Bronchospasm
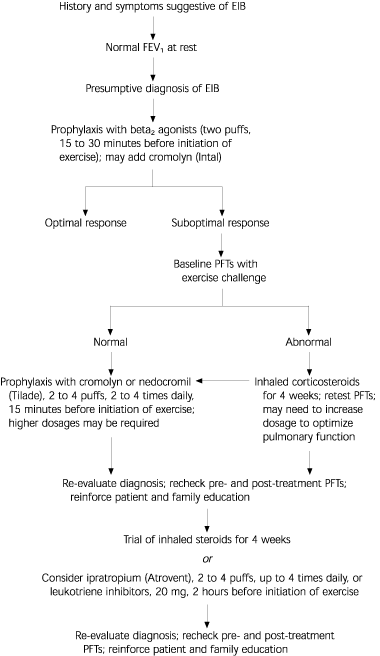
Algorithm for the diagnostic and therapeutic management of exercise-induced bronchospasm. (EIB = exercise-induced bronchospasm; FEV1 = forced expiratory volume at one second; PFTs = pulmonary function tests)
Traditionally, the diagnosis is based on a detailed history with symptoms suggestive of EIB and a normal FEV1 at rest. A therapeutic trial may be instituted in these patients. In patients whose response is less than optimal following an adequate therapeutic trial, the threshold for conducting baseline pulmonary function testing should be low. These patients may have undiagnosed asthma or other pulmonary conditions, and the first priority should be to optimize pulmonary function testing with the use of inhaled steroids. Table 4 lists the medications that are available to treat EIB.
TABLE 4 Medications for the Treatment of Exercise-Induced Bronchospasm
| Medication* | Dosage | Onset of action | Effectiveness | Approval of athletic organizations |
|---|---|---|---|---|
| Beta agonists | ||||
| Albuterol (Proventil, Ventolin) | MDI, 2 to 4 puffs as needed | 3 to 5 minutes | Most effective | NCAA/USOC † |
| Terbutaline (Bricanyl) | MDI, 2 to 4 puffs as needed | 3 to 5 minutes | Most effective | NCAA/USOC † |
| Bitolterol (Tornalate) | MDI, 1 to 2 puffs as needed | 3 to 5 minutes | Most effective | NCAA |
| Pirbuterol (Maxair) | MDI, 1 to 2 puffs as needed | 3 to 5 minutes | Most effective | NCAA |
| Formoterol (Foradil Aerolizer) | Inhalation of contents of one 12-mcg capsule every 12 hours | 1 to 3 minutes | Most effective | NCAA |
| Metaproterenol (Alupent) | MDI, 2 to 4 puffs as needed | 3 to 5 minutes | Very effective | NCAA |
| Salmeterol (Serevent) | MDI, 2 puffs as needed | 15 to 30 minutes | Most effective | NCAA/USOC † |
| Mast cell stabilizers | ||||
| Cromolyn (Intal) | MDI, 2 to 4 puffs, 4 times daily | 3 to 4 weeks | Moderately effective | NCAA/USOC |
| Nedocromil (Tilade) | MDI, 2 to 3 puffs, 2 to 3 times daily | 3 to 4 days | Moderately effective | NCAA/USOC |
| Inhaled corticosteroids | MDI, 2 to 4 puffs, 2 to 4 times daily | 3 to 4 weeks | Very effective | NCAA/USOC |
| Triamcinolone acetonide (Azmacort) | MDI, 2 puffs, 3 to 4 times daily | 3 to 4 weeks | Very effective | NCAA/USOC |
| Fluticasone (Flovent) | MDI, 1 puff, twice daily | 3 to 4 weeks | Very effective | NCAA/USOC |
| Budesonide (Rhinocort) | MDI, 1 to 2 puffs, 1 to 2 times daily | 3 to 4 weeks | Very effective | NCAA/USOC |
| Flunisolide (AeroBid) | MDI, 2 puffs, twice daily | 3 to 4 weeks | Very effective | NCAA/USOC |
| Other | ||||
| Theophylline, sustained release (Slo-Phyllin, Slo-bid) | 5 to 8 mg per kg twice daily | 2 to 3 days | Moderately effective | NCAA/USOC |
| Ipratropium (Atrovent) | MDI, 2 to 4 puffs as needed | 15 to 30 minutes | Possibly effective | NCAA/USOC |
MDI = metered-dose inhaler; NCAA = National Collegiate Athletic Association; USOC = United States Olympic Committee..
*—These medications come in various strengths, and dosages vary accordingly.
†—Approval by the USOC is dependent on a previous notification and independent assessment by the Olympic Medical Commission.
Information from Physicians' Desk Reference 2002 and Olympic Movement Anti-Doping Code, Appendix A (http://multimedia.olympic.org/pdf/en_report_541.pdf).
Beta Agonists
Inhaled beta agonists are first-line medications in the management of EIB, both as prophylaxis and to treat the bronchospasm that occurs with exercise. A short-acting beta agonist should be taken 15 minutes before exercise and may be repeated as necessary.9 Common beta agonists include metaproterenol (Alupent); albuterol (Ventolin); bitolterol mesylate (Tornalate); pirbuterol (Maxair); terbutaline sulfate (Bricanyl); and formoterol (Foradil Aerolizer).10 Formoterol, a long-acting agent, has bronchoprotective effects for up to 12 hours.11 It was approved by the U.S. Food and Drug Administration (FDA) in February, 2001, for pretreatment in children 12 years or older. Formoterol is available as an inhalation powder and is to be used with an aerolizer inhaler (Table 4).
Salmeterol (Serevent) is a long-acting beta agonist approved by the FDA for use in persons 12 years and older. It has been shown to protect against EIB for up to 12 hours after use.12 [Evidence level A: randomized controlled trial (RCT)] However, continuous use of beta agonists, especially salmeterol13 and formoterol,14 has been documented to cause tachyphylaxis.
Cromolyn and Nedocromil
Cromolyn sodium (Intal) and nedocromil (Tilade) are anti-inflammatory agents that can work in cooperation with beta agonists, inhibiting the early bronchospastic phase and the late inflammatory phase of EIB through inhibition of mast cell mediator release and calcium influx. These agents are effective in 70 to 85 percent of patients and have minimal side effects.15 A meta-analysis16 of eight RCTs showed no significant differences in efficacy between cromolyn and nedocromil; nedocromil has a more rapid onset of action and seems to have a greater effect on those with more severe disease but is often rejected because of its offensive taste.
Inhaled Corticosteroids
Inhaled corticosteroids have been demonstrated to be useful in the treatment of EIB17,18 (Table 4). These agents are safe and effective when used in the recommended dosage (below 400 mcg per day) and require four weeks to achieve maximal effect. Side effects such as oral candidiasis and hoarseness can be diminished or entirely eliminated by adding a spacer to the inhaler and by gargling with water after use and expectorating the fluid.19
Theophylline
Theophylline has a long and controversial history as a bronchodilator. Its adverse side effect profile, multiple drug interactions, and unpredictable absorption make it a tertiary agent in the treatment of EIB. Theophylline also has been anecdotally reported to affect concentration and learning behavior and should be used with caution in school-aged children.
Anticholinergics
Ipratropium bromide, a derivative of atropine with modest bronchodilating properties, is used as a tertiary agent.20 For optimal efficacy, patients should have baseline pulmonary function tests in the normal range.
Additional Agents
Evidence exists to show that leukotriene receptor antagonists, such as montelukast (Singulair)21 and zafirlukast (Accolate), and 5-lipoxygenase inhibitors, such as zileuton (Zyflo),22 provide substantial protection against EIB when used individually and in combination with inhaled cortico-steroids23; however, considerable variation was observed among patients. Other options, such as inhaled furosemide (Lasix),24 vitamin C,25 inhaled heparin,26 antihistamines, calcium channel blockers, and reduced dietary salt intake,27 have been studied as potential treatments for EIB. Physicians and patients should wait for results of clinical trials before choosing these potential therapies.
Final Comment
Exercise-induced bronchospasm results from a transient increase in airway resistance producing various symptoms (cough, wheezing, chest tightness, or pain) that may appear five to 10 minutes after initiation of exercise. EIB may present without symptoms, simply manifesting as a patient refusing to participate in exercise or competitive sports because of an unrecognized ability to breathe normally. The condition is usually treated with short-acting bronchodilators, with or without the addition of anti-inflammatory agents, taken 15 to 30 minutes before initiation of exercise. Medications should be accompanied by warm-up and cool-down exercises and nasal breathing to attenuate the symptoms.
Failure to respond positively to these initial measures should prompt pulmonary function testing with a bronchodilator, exercise challenge testing and, possibly, referral to a specialist. Alternative diagnoses, such as vocal cord dysfunction and glottic dysfunction, should be considered if the patient continues to be symptomatic.
The diagnosis and treatment of EIB is both simple and immensely rewarding for the family physician and the patient. Appropriate management allows most patients to enjoy the benefits of exercise and their chosen sports, leading to a healthier lifestyle.

