The fusiform excision technique is commonly used by physicians for removing skin and subcutaneous lesions. The technique requires basic skills in anesthetic administration, lesion excision, and suture closure. Physicians experienced in skin surgery can often perform the procedure unsupervised after two to five precepted sessions. The fusiform excision technique should be used to biopsy any suspicious pigmented lesions because prognosis may depend on the depth of the lesion. A properly designed fusiform excision has a length-to-width ratio of 3 to 1 and produces a 30-degree angulation at both edges of the wound. The skin edges should be everted during the closure to improve final scar appearance. Malignant growths may require a second procedure to provide a wider margin of excision around the lesion. Post-excisional wound infections are uncommon with use of proper aseptic technique.
The fusiform excision technique is commonly used by family physicians for removing skin and subcutaneous lesions. This office procedure offers the advantages of a definitive, single-stage diagnostic and therapeutic intervention. The fusiform excision has previously been referred to as an elliptical excision, but the true biconcave appearance of the wound is more appropriately described as fusiform. Shave excision is a simpler procedure, but the fusiform excision technique offers cosmetic and diagnostic advantages in certain clinical situations. The fusiform technique should be used to obtain biopsy specimens of any pigmented lesions that potentially could be melanoma, because the future therapy of melanoma is dependent on the depth of the lesion.
The classical fusiform excision has a 3 to 1 length-to-width ratio. This technique produces an angle of 30 degrees or less at the end of the wound. The long axis of the wound should be oriented parallel to the lines of least skin tension to improve the final scar outcome. A properly designed fusiform excision can be closed primarily and should not result in the formation of raised tissue at the ends of the wound (known as “dog ears”).
Gentle handling of the wound edges with skin hooks produces good cosmetic results. The skin should not be grasped with forceps, because the resulting skin damage can produce necrosis and scarring. Disposable skin hooks can be created by bending the end of a 21-gauge needle. Disposable skin hooks are preferred by nursing personnel because accidents frequently occur in the process of autoclaving when nondisposable skin hooks break through the sterile wraps.
Hematomas at the base of an excision inhibit wound healing, create excessive scarring, and produce a depressed and more noticeable scar following normal scar retraction. Subcutaneous bleeding sites can be controlled with instrument clamps, electro-cautery, or absorbable suture ligation. Interrupted, deep-buried absorbable sutures placed down to the level of the fascia eliminate dead space, provide excellent hemostasis, reduce tension on the skin sutures, and generally improve the cosmetic and functional result.
Methods and Materials
PATIENT PREPARATION
The patient is seated or lying comfortably on the examination table with the skin lesion exposed.
EQUIPMENT
Nonsterile Tray for Anesthesia and Designing the Fusiform Excision
- Place the following items on a nonsterile drape covering a Mayo stand:
- Nonsterile gloves
- Skin-marking pen
- 4 × 4 gauze
- Povidone-iodine solution
- 10-mL syringe filled with 1 or 2 percent lidocaine (Xylocaine) with or without epinephrine with a 30-gauge needle
- Mask
Sterile Tray for the Procedure
- Place the following items on a sterile drape covering a Mayo stand:
- Sterile gloves
- Fenestrated disposable drape
- Additional nonfenestrated disposable drape (if desired)
- 2 sterile bandages to anchor the fenestrated drape
- 3 hemostats (mosquito clamps)
- No. 15 scalpel blade and handle
- Needle holder
- Mayo or tissue scissors
- Iris scissors for cutting sutures
- Adson forceps
- 21-gauge, 1 ½-inch needle (to be bent into a skin hook)
- 2 inches of 4 × 4 gauze
- Suture materials
Procedure Description
- The fusiform excision is designed with a 3 to 1 length-to-width ratio, oriented in the direction of the lines of least skin tension (Figures 1 and 2). The excision lines can be marked on the skin using a skin-marking pen.
- The skin is prepped with povidone-iodine solution and anesthetized with 1 or 2 percent lidocaine with or without epinephrine. The hemostatic benefit of epinephrine is added for most procedures, except when the surgery is performed on the digits or the tip of the nose. The anesthetic can be administered with a 10-mL syringe and a 30-gauge needle for enhanced patient comfort.
- Following administration of the anesthetic, sterile gloves can be applied, the skin can be reprepped with povidone-iodine solution, and a sterile fenestrated paper drape placed over the surgical field. Sterile bandages can be used at the edge of the fenestration to keep the drape from shifting and prevent unprepped skin from appearing through the drape hole.
- The incision is made with a no. 15 scalpel blade held vertical to the skin. Inward beveling, or “wedging,” is discouraged. The first pass of the scalpel on each wound edge should be smooth and continuous to prevent notching of the skin. A second pass of the blade may be needed to extend these incisions down to the level of the fat. Some 4 × 4 gauze can be used to wipe the surgical field clear of blood.
- The scalpel is turned parallel to the skin surface to undermine the central fusiform island of skin. The central island of skin is lifted with Adson forceps with teeth as the scalpel is moved in the level of the upper fat. Once the central island of skin is removed, it is immediately placed in formalin and retained for histologic evaluation.
- Bleeding sites in the wound base can be controlled by applying hemostats or suture ligation. The physician should not be overly preoccupied with bleeding and should continue efforts to prepare the wound for closure. The lateral tissues are elevated with a nondisposable skin hook or a disposable hook (created by curling the end of a 21-gauge, 1½-inch needle). The lateral skin edges are not lifted with Adson forceps because the forceps may cause tissue necrosis. The lateral skin edges are undermined with horizontally held scalpel or scissors in the level of the upper fat; 3 cm of lateral undermining is required for every 1 cm of skin edge relaxation.
- Interrupted, deep-buried sutures are placed to eliminate dead space at the wound base, promote healing, reduce tension on the skin sutures, and improve the final cosmetic appearance of the scar (Figure 3). In the office setting, polyglactin (Vicryl) sutures (3–0, 4–0, 5–0, or 6–0) are the most commonly selected absorbable sutures for closure. Proper placement of these sutures produces close approximation of the skin edges.
- The skin edges should be everted (upward lifting of the skin edges) to improve the final scar appearance. Interrupted nylon sutures (3–0, 4–0, 5–0, or 6–0) are the most commonly selected nonabsorbable sutures for skin closure in the office setting. Eversion often can be accomplished without grasping the skin edges with forceps, by entering and exiting the skin vertically with the suture needle while depressing lateral tissue with a finger of the nondominant hand.
- Once the suturing is completed, the wound should be squeezed gently to remove any residual blood from beneath the wound that will interfere with healing. Direct pressure can be applied with gauze by the patient for 10 minutes or more to assist with hemostasis. The assistant then cleans the site with saline solution, applies antibiotic ointment, and places a pressure dressing (elastic bandage over gauze).
FIGURE 1.
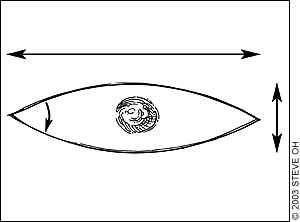
Fusiform excision. A properly designed fusiform excision has a length-to-width ratio of 3 to 1. In addition, the angle at the corner of the fusiform island of tissue should be 30 degrees or less.
FIGURE 2.

Fusiform excision designed to follow the lines of least skin tension. The lines of least skin tension are influenced by the contractions of the underlying muscles and tend to follow skin creases and wrinkles.
FIGURE 3.
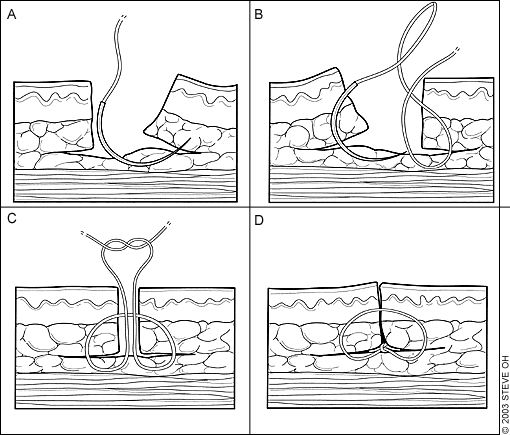
Use of interrupted, deep-buried sutures following fusiform excision. (A) Buried knots are created with absorbable subcuticular sutures by taking the first bite on the far side of the wound from bottom to top. (B) The bite includes tissue at the base of the wound to close the deep space. The needle is then placed in the needle holder upside down and backwards, and a reverse bite is created going from top to bottom on the near side. (C) The free end of the suture and the needle end must exit the wound on the same side of the suture across the top of the wound. (D) This technique allows the final knot to be buried in the wound base.
Follow-Up
- Malignant growths may require a second procedure to provide a wider margin of excision around the original lesion. For instance, a melanoma-in-situ requires removal of a 0.5-cm margin of normal skin surrounding the lesion. A thicker melanoma may require removal of a 3-cm margin of normal skin in all directions around the lesion.
- Malignancies that are not completely excised at the original biopsy site may require re-excision. When the pathologist reports positive margins, consideration should be given to a second procedure. Basal cell carcinomas that infiltrate through the skin, such as the morpheaform type, may not have visible margins and may require Mohs' surgery or wide excision for complete removal. Squamous cell carcinomas that have positive margins at the original excision should be removed with an excision of the suture line and surrounding tissue on the sides and below the original surgical site.
- Some pathology reports describe rare or unusual tumors that may be unfamiliar to the family physician. Pathologists may also use ambiguous terminology in describing a lesion. If there is confusion or uncertainty, the physician should speak directly to the pathologist. Many pathologists welcome the clinical interchange with the physician. Patients can be referred to more experienced surgeons for management of unfamiliar findings.
- Skin suture removal should be performed after an appropriate interval following the original surgery. Many factors influence the timing of suture removal, including the patient's age, nutritional status, and other medical problems (e.g., diabetes). A general guide for suture removal based on the body site is listed in Table 1.
- Patients may be upset if their wound undergoes dehiscence. Physicians should be careful when early suture removal is attempted, especially on a lower extremity. Surgical wounds generally have only 8 to 15 percent of their final wound strength two weeks following the procedure. At the time of suture removal, the physician might consider applying tincture of benzoin solution to the skin and Steri-Strips to provide extra wound strength for an additional seven to 10 days.
Procedure Pitfalls/Complications
- Excessive Bleeding Occurred During the Procedure. Excision of the fusiform island of skin and lateral edge undermining can produce vigorous bleeding, which can sidetrack inexperienced physicians. Avoid wasting time in repetitive blotting of the wound bed with gauze. Learn to work around the bleeding. Bleeding vessels in the wound base can be briefly clamped with hemostats while undermining is performed. Placing the deep-buried absorbable sutures to approximate skin edges and closing the dead space almost always stops wound bleeding.
- The Wound Only Closes in the Center with Hard Tugging on the Tissues. Novice physicians often fail to undermine the lateral tissues adequately. Each skin edge must be undermined 3 cm for every 1 cm gained in tissue relaxation. Extensive undermining does produce some bleeding, but the bleeding is easily controlled with placement of the deep sutures. Failure to perform adequate undermining can cause excessive tension on the center of the wound and subsequent skin breakdown or suture tension marks.
- Wound Infection Occurred Following the Procedure. Wound infections are uncommon if proper aseptic technique is followed. The operative time should be as short as possible. Antibiotic ointment applied to the wound immediately following the surgery and then daily until the sutures are removed can aid in wound healing and infection prevention. Wound-edge redness that is within one-half inch of the wound and not associated with pus or drainage often is not infection but instead is reparative or inflammatory changes associated with healing. Care must be taken when performing procedures in certain areas at high risk for infection, such as the groin or lower legs.
- The Wounds Frequently Have “Dog Ears” at the Ends. “Dog ears”are mounds of elevated tissue that occur at the ends of some linear wounds after closure. Dog ears can occur with excisions on convex surfaces such as the arms and legs and most commonly develop from an improperly designed fusiform excision. The wound should be long enough to have at least a 3 to 1 length-to-width ratio. Dog ears can be removed by excising a fusiform island of skin in the direction of the original wound or by removing a lateral piece of redundant skin and extending the wound laterally.
- A Seroma Developed Beneath the Wound. Failure to close the dead space beneath a wound can result in the formation of a seroma (a thin-walled pseudocyst that represents a collection of serous fluid in an open space). The placement of deep-buried sutures generally eliminates this complication.
- The Excision Damaged Nerves or Arteries Beneath the Wound. Incisions that extend deep into tissues have the potential to cause permanent nerve and artery damage. Placing a generous volume of anesthetic beneath a lesion effectively increases the thickness of the skin and subcutaneous tissues, thereby keeping the incisions more superficial. The anesthetic also displaces downward structures in the deep fat, such as arteries and nerves. Undermining the wound edges in the level of the upper fat also helps avoid damaging deeper structures.
- The Patient Experiences Discomfort During the Procedure. Novice physicians often do not adequately anesthetize the wound before starting the procedure. Five to 10 mL of anesthetic should be administered before most procedures. The sides of the wound must be infiltrated to provide coverage for the lateral undermining. Intradermal blanching produced by anesthetic administration can be a useful indication that the incision lines are ready for the procedure.
- The Final Scar Is Thick and Unsightly. Properly designed incisions that follow the lines of least skin tension usually result in cosmetically acceptable scars. Wounds that cross flexion creases or are perpendicular to the lines of least tension can thicken into hypertrophic scars. Physicians may need to consult reference diagrams that describe the orientation of skin tension lines in complex areas (e.g., the face).
- The Final Scar Has Cross-Hatch or Railroad Marks. Cross-hatching of the final scar often results from too much tension on the wound from the skin sutures. Placing deep subcutaneous sutures can reduce tension on the wound. Placing smaller caliber skin sutures (5–0 and 6–0) closer to the wound edge can reduce the tension across the wound and reduce the formation of cross-hatch marks. The sutures should not be tied too tightly.
TABLE 1 Timing of Suture Removal
| Facial sutures | Three to five days |
| Scalp and neck sutures | Seven days |
| Upper extremity sutures | Seven to nine days |
| Upper extremity over a joint crease suture | Eight to 14 days |
| Trunk sutures | Eight to 12 days |
| Lower extremity sutures | 14 to 28 days |
Physician Training
Formal training is needed for the techniques of anesthetic administration, lesion excision, and closure. Most family physicians receive this training during their residency programs. Others can obtain this training with an experienced preceptor. Physicians experienced in skin surgery can often perform these excisions unsupervised after two to five procedures. Inexperienced physicians may require 20 to 40 precepted procedures before attempting unsupervised excisions.

