For years, an association between white blood cell (WBC) count and cardiovascular disease has been recognized, and recent studies have shown that inflammation plays an important role in atherosclerosis and acute coronary artery syndromes. These new results have sparked renewed interest in the research of inflammatory markers, such as C-reactive protein and WBC count, in acute coronary syndromes. One study of patients with ST-segment elevation myocardial infarction found an association between elevated WBC count from baseline and worse angiographic findings as well as higher 30-day mortality rates. Sabatine and colleagues studied the relationship between elevated WBC counts from baseline and outcomes in patients with unstable angina/non–ST-segment elevation myocardial infarction, and whether the WBC count was a significant predictor of outcomes independent of other biomarkers.
Cumulative Mortality Incidence Curves
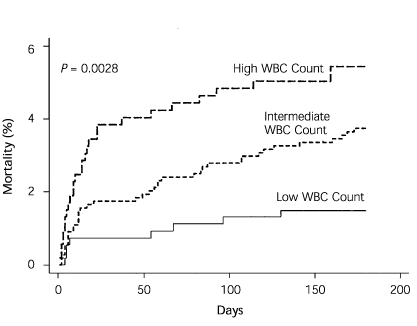
FIGURE. Cumulative mortality incidence curves at six months in relation to baseline white blood cell (WBC) count, categorized as low (less than 25th percentile), intermediate (25th to 75th percentiles), and high (greater than 75th percentile).
Adapted with permission from Sabatine MS, Morrow DA, Cannon CP, Murphy SA, Demopoulos LA, DiBattiste PM, et al. Relationship between baseline white blood cell count and degree of coronary artery disease and mortality in patients with acute coronary syndromes. A TACTICS-TIMI 18 substudy. J Am Coll Cardiol 2002;40:1766.
The study was part of the Treat Angina with Aggrastat and Determine Cost of Therapy with an Invasive or Conservative Strategy (TACTICS)-Thrombolysis in Myocardial Infarction (TIMI) 18 trial that included 2,220 patients with evidence of unstable angina/non–ST-segment elevation myocardial infarction who were randomized to receive invasive or conservative intervention. Baseline laboratory evaluation of these patients included WBC count, creatinine, cardiac troponin, and C-reactive protein measurements. The WBC count was treated as a continuous variable, but also was categorized as: low (less than 6,650 per mm3 [6.65 × 109 per L]); intermediate (6,650 to 10,110 per mm3 [6.65 to 10.11 × 109 per L]); and high (greater than 10.11 × 109 per L). Angiography data were recorded on all patients who were randomized into the invasive treatment arm of the study in whom routine angiography was mandated.
Higher baseline WBC counts were associated with lower TIMI flow grades, lower myocardial perfusion grades, and a greater extent of coronary artery disease. A higher WBC count also was associated with a higher six-month mortality rate (see accompanying figure). Patients with a low C-reactive protein level but an elevated WBC count remained at a significantly higher risk of mortality at six months while patients with a high C-reactive protein level were at an even higher risk for mortality at six months.
The authors conclude that an elevated WBC count was associated with impaired epicardial and myocardial perfusion, more extensive coronary artery disease, and higher risk for six-month mortality in patients with unstable angina/non–ST-segment elevation myocardial infarction. Two inflammatory markers, WBC count and C-reactive protein, can be used to stratify six-month mortality risk in patients with these conditions.

