Syphilis is a sexually transmitted disease with varied and often subtle clinical manifestations. Primary syphilis typically presents as a solitary, painless chancre, whereas secondary syphilis can have a wide variety of symptoms, especially fever, lymphadenopathy, rash, and genital or perineal condyloma latum. In latent syphilis, all clinical manifestations subside, and infection is apparent only on serologic testing. Late or tertiary syphilis can manifest years after infection as gummatous disease, cardiovascular disease, or central nervous system involvement. Neurosyphilis can develop in any stage of syphilis. The diagnosis of syphilis may involve dark-field microscopy of skin lesions but most often requires screening with a nontreponemal test and confirmation with a treponemal-specific test. Parenterally administered penicillin G is considered first-line therapy for all stages of syphilis. Alternative regimens for non-pregnant patients with no evidence of central nervous system involvement include doxycycline, tetracycline, ceftriaxone, and azithromycin. In pregnant women and patients with neurosyphilis, penicillin remains the only effective treatment option; if these patients are allergic to penicillin, desensitization is required before treatment is initiated. Once the diagnosis of syphilis is confirmed, quantitative nontreponemal test titers should be obtained. These titers should decline fourfold within six months after treatment of primary or secondary syphilis and within 12 to 24 months after treatment of latent or late syphilis. Serial cerebrospinal fluid examinations are necessary to ensure adequate treatment of neurosyphilis.
Syphilis is a sexually transmitted disease (STD) caused by the spirochete Treponema pallidum. Previously known as the “great imitator,” this disease can have numerous and complex manifestations. Family physicians should understand its presentations, stage-specific diagnostic testing, and appropriate antibiotic treatments, because missed or inappropriately treated syphilis can result in devastating cardiovascular and neurologic disease, as well as congenital syphilis.
Epidemiology
The incidence of syphilis decreased significantly with the introduction of penicillin in the 1940s but rose sharply again with the advent of human immunodeficiency virus (HIV) infection in the 1980s. From 1990 through 2000, primary and secondary syphilis infection rates decreased by 89.2 percent. Despite the overall decreases, outbreaks of syphilis have recently been reported in men who have sex with men. In the United States, syphilis is more prevalent in the South, in urban areas, in men, and in blacks.1
Stages of Syphilis
Primary syphilis most often manifests as a solitary, painless chancre that develops at the site of infection an average of three weeks after exposure to T. pallidum.
Without treatment, blood-borne spread of T. pallidum over the next several weeks to months results in secondary syphilis, which has numerous clinical manifestations. The most common features are fever, lymphadenopathy, diffuse rash, and genital or perineal condyloma latum.
During the latent stage of syphilis, skin lesions resolve, and patients are asymptomatic. However, serologic tests are positive for T. pallidum.
Tertiary or late syphilis develops years after the initial infection and can involve any organ system. The most dreaded complications are neurosyphilis and involvement of the aortic valve and root.
Diagnosis
DARK-FIELD MICROSCOPY
Dark-field microscopy is the most specific technique for diagnosing syphilis when an active chancre or condyloma latum is present.2 However, its accuracy is limited by the experience of the operator performing the test, the number of live treponemes in the lesion, and the presence of non-pathologic treponemes in oral or anal lesions.3
In preparation for dark-field microscopy, the lesion is cleansed and then abraded gently with a gauze pad. Once a serous exudate appears, it is collected on a glass slide and examined under a microscope equipped with a dark-field condenser.2 T. pallidum is identified by its characteristic corkscrew appearance.4 Given the inherent difficulties of dark-field microscopy, negative examinations on three different days are necessary before a lesion may be considered negative for T. pallidum.4
NONTREPONEMAL TESTS
Syphilitic infection leads to the production of non-specific antibodies that react to cardiolipin. This reaction is the basis of traditional nontreponemal tests such as the VDRL test and rapid plasma reagin test.
With nontreponemal tests, false-positive reactions can occur because of pregnancy, autoimmune disorders, and infections.5,6 In addition, these tests may show a “prozone” phenomenon in which large amounts of antibody block the antibody-antigen reaction, causing a false-negative test in the undiluted sample.2
Qualitative nontreponemal tests are widely used for syphilis screening. However, their usefulness is limited by decreased sensitivity in early primary syphilis and during late syphilis, when up to one third of untreated patients may be nonreactive.3
After adequate treatment of syphilis, nontreponemal tests eventually become nonreactive. However, even with sufficient treatment, patients sometimes have a persistent low-level positive nontreponemal test (referred to as a serofast reaction).
Titers are not interchangeable between different test types. Hence, the same nontreponemal test should be used for follow-up evaluations.
TREPONEMAL-SPECIFIC TESTS
Treponemal-specific tests detect antibodies to antigenic components of T. pallidum. These tests are used primarily to confirm the diagnosis of syphilis in patients with a reactive nontreponemal test. However, the enzyme immunoassay (EIA) test for antitreponemal IgG also may be used for screening.7 Treponemal-specific tests include the EIA for anti-treponemal IgG, the T. pallidum hemagglutination (TPHA) test, the microhemagglutination test with T. pallidum antigen, the fluorescent treponemal antibody-absorption test (FTA-abs), and the enzyme-linked immunosorbent assay.
Treponemal tests have sensitivities and specificities equal to or higher than those for nontreponemal tests.2,5 However, treponemal-specific tests are more difficult and expensive to perform, which limits their usefulness as screening tests. In addition, false-positive results can occur, especially when the FTA-abs test is used in patients with systemic lupus erythematosus or Lyme disease.2,8
Unlike nontreponemal tests, which show a decline in titers or become nonreactive with effective treatment, treponemal-specific tests usually remain reactive for life. Therefore, treponemal-specific test titers are not useful for assessing treatment efficacy.
Stage-Specific Diagnosis and Treatment
TREATMENT GUIDELINES
Guidelines from the Centers for Disease Control and Prevention (CDC) recommend parenterally administered penicillin G for the treatment of all stages of syphilis (Figure 1).9 [Evidence level C, consensus/expert guidelines] Alternative regimens may be used in patients who are allergic to penicillin. However, pregnant women and patients with neuro-syphilis require treatment with penicillin even if they are allergic to the drug. In these patients, desensitization is necessary before penicillin therapy is initiated.
FIGURE 1. Treatment of Syphilis
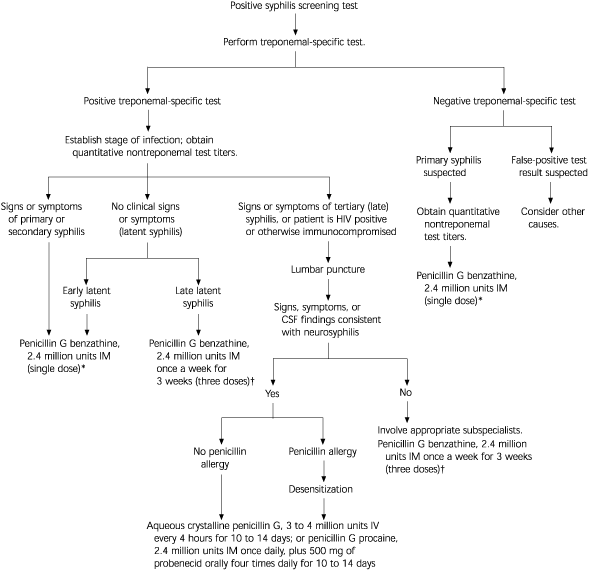
Recommended approach to the treatment of syphilis. (IM = intramuscular; HIV = human immunodeficiency virus; CSF = cerebrospinal fluid; IV = intravenous)
*--Alternative treatments for nonpregnant penicillin-allergic patients: doxycycline (Vibramycin), 100 mg taken orally twice daily for 2 weeks, or tetracycline, 500 mg taken orally four times daily for 2 weeks; limited data support efficacy for ceftriaxone (Rocephin), 1 g once daily IM or IV for 8 to 10 days, or azithromycin (Zithromax), 2 g orally (single dose).
†--Alternative treatments for nonpregnant penicillin-allergic patients: doxycycline, 100 mg taken orally twice daily for 4 weeks, or tetracycline, 500 mg taken orally four times daily for 4 weeks.
Information from reference 9.
The treatment of syphilis is similar in HIV-positive and HIV-negative patients. However, HIV-positive patients require more frequent follow-up because of an increased risk of treatment failure. In addition, a higher index of suspicion for central nervous system (CNS) involvement must be maintained.9
Treatment of syphilis in any stage should take into account the risks of acquiring other STDs. HIV testing should be considered in the initial evaluation of all patients with syphilitic infection.9Screening for hepatitis B and C, gonorrhea, and chlamydial infection also should be considered.
After appropriate treatment has been administered, patients should be followed with quantitative nontrepone-mal test titers to establish treatment response. Typically, nontreponemal test titers should become at least four times lower within six months after treatment of primary or secondary syphilis, and within 12 to 24 months after treatment of latent or late infection.10 [Evidence level B, cohort study]
PRIMARY SYPHILIS
Primary syphilis is most often associated with a single, painless chancre, although it can manifest in other ways (i.e., multiple chancres, painful papules or ulcers, or no lesions).4 The chancre is most commonly found on the external genitalia and develops 10 to 90 days (average: 21 days) after infection.11 Associated regional lymphadenopathy is common. The chancre usually resolves spontaneously in one to four months.
Lesions that can be confused with the chancre of primary syphilis include herpes simplex virus infection, chancroid, fixed drug eruption, lymphogranuloma venereum, granuloma inguinale (donovanosis), traumatic ulcer, furuncle (boil), and aphthous ulcer.12 A selected differential diagnosis is provided in Table 1.12,13
TABLE 1 Selected Differential Diagnosis of Genital Lesions
| Disorder or disease | Characteristics of genital lesion | Etiology |
|---|---|---|
| Primary syphilis: chancre | Solitary, painless ulcer with indurated border | Treponema pallidum |
| Secondary syphilis: condyloma latum | Slightly raised or flat, round or oval papules covered by gray exudate | T. pallidum |
| Genital herpes | Cluster of shallow, small, painful ulcers on a red base | Herpes simplex virus |
| Chancroid | Painful ulcer with sharp, undermined borders | Haemophilus ducreyi |
| Venereal warts | Soft, usually painless skin-colored or red papules | Human papillomavirus |
| Lymphogranuloma venereum: primary stage | Painless papule, shallow erosion, or ulcer; may be multiple or single | Chlamydia trachomatis |
Primary syphilis is diagnosed by dark-field microscopy of a suspected lesion or by serologic testing (Table 2).2,9 Either technique can have a false-negative result early in the course of the disease. Thus, if clinical suspicion is high, treatment for syphilis should be initiated.
TABLE 2 Stages of Syphilitic Infection
| Stage | Clinical manifestations | Diagnosis (sensitivity) | Treatment |
|---|---|---|---|
| Primary syphilis | Chancre | Dark-field microscopy of skin lesion (80%) Nontreponemal tests (78% to 86%) Treponemal-specific tests (76% to 84%) | Penicillin G benzathine, 2.4 million units IM (single dose) Alternatives in nonpregnant patients with penicillin allergy: doxycycline (Vibramycin), 100 mg orally twice daily for 2 weeks; tetracycline, 500 mg orally four times daily for 2 weeks; ceftriaxone (Rocephin), 1 g once daily IM or IV for 8 to 10 days; or azithromycin (Zithromax), 2 g orally (single dose) |
| Secondary syphilis | Skin and mucous membranes: diffuse rash, condyloma latum, other lesions Renal system: glomerulonephritis, nephrotic syndrome Liver: hepatitis Central nervous system: headache, meningismus, cranial neuropathy, iritis and uveitis Constitutional symptoms: fever, malaise, generalized lymphadenopathy, arthralgias, weight loss, others | Dark-field microscopy of skin lesion (80%) Nontreponemal tests (100%) Treponemal-specific tests (100%) | Same treatments as for primary syphilis |
| Latent syphilis | None | Nontreponemal tests (95% to 100%) Treponemal-specific tests (97% to 100%) | Early latent syphilis: same treatments as for primary and secondary syphilis Late latent syphilis: penicillin G benzathine, 2.4 million units IM once weekly for 3 weeks Alternatives in nonpregnant patients with penicillin allergy: doxycycline, 100 mg orally twice daily for 4 weeks; or tetracycline, 500 mg orally four times daily for 4 weeks |
| Tertiary (late) syphilis | Gummatous disease, cardiovascular disease | Nontreponemal tests (71% to 73%) Treponemal-specific tests (94% to 96%) | Same treatment as for late latent syphilis |
| Neurosyphilis | Seizures, ataxia, aphasia, paresis, hyperreflexia, personality changes, cognitive disturbance, visual changes, hearing loss, neuropathy, loss of bowel or bladder function, others | Cerebrospinal fluid examination | Aqueous crystalline penicillin G, 3 to 4 million units IV every 4 hours for 10 to 14 days; or penicillin G procaine, 2.4 million units IM once daily, plus probenecid, 500 mg orally four times daily, with both drugs given for 10 to 14 days |
IM = intramuscular; IV = intravenous.
Primary syphilis is treated with 2.4 million units of penicillin G benzathine delivered intramuscularly in a single dose. In nonpregnant patients who are allergic to penicillin, alternative regimens include doxycycline (Vibramycin), in a dosage of 100 mg taken orally twice daily for two weeks, or tetracycline, in a dosage of 500 mg taken orally four times daily for two weeks. Limited evidence indicates that ceftriaxone (Rocephin), in a dosage of 1 g delivered intramuscularly or intravenously once daily for eight to 10 days, or azithromycin (Zithromax), in a single 2-g dose taken orally, may be effective for the treatment of primary syphilis, although close follow-up is warranted to assess treatment efficacy.9
At six and 12 months after treatment, patients with primary syphilis should be reexamined and undergo repeat serologic testing. Treatment failure is defined as recurrent or persistent symptoms or a sustained fourfold increase in nontreponemal test titers despite appropriate treatment. Patients with treatment failure should be tested for HIV infection and evaluated for neurosyphilis with a cerebrospinal fluid (CSF) examination.9
SECONDARY SYPHILIS
Secondary syphilis develops several weeks to months after the chancre appears.4 The skin is most often affected. Patients may present with macular, maculopapular, or even pustular lesions, beginning on the trunk and proximal extremities. The rash of secondary syphilis may involve all skin surfaces, including the palms and soles. Condyloma latum also is associated with secondary syphilis. Involving mainly warm, moist areas such as the perineum and perianal skin, this soft, verrucous plaque is painless but highly infectious.
Other organs and systems that can be affected in secondary syphilis include the renal system (glomerulonephritis, nephrotic syndrome), the liver (hepatitis), the CNS (headache, meningitis, cranial neuropathy, iritis, and uveitis), and the musculoskeletal system (arthritis, osteitis, periostitis).4 Patients also may have constitutional symptoms such as fever, malaise, generalized lymphadenopathy, arthralgias, and weight loss.
The diagnosis of secondary syphilis is confirmed by nontreponemal and treponemal-specific tests. Treatment employs the same antibiotic regimens used for primary syphilis. Follow-up is the same as that for primary syphilis (Figure 2).9
FIGURE 2. Follow-up of Primary or Secondary Syphilis
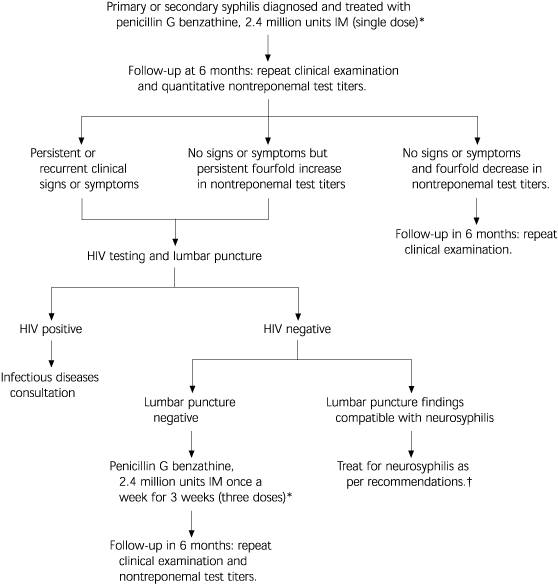
An approach to follow-up in patients treated for primary or secondary syphilis. (IM = intramuscular; HIV = human immunodeficiency virus)
*--See text for alternative treatment recommendations for nonpregnant penicillin-allergic patients.
†--See text for recommended treatments for neurosyphilis.
Information from reference 9.
LATENT SYPHILIS
It is important to distinguish between early and late latent syphilis, because relapse to secondary syphilis and recurrent infectivity are possible during the early latent stage. Early latent syphilis encompasses the first year after infection. This stage can be established only in patients who have seroconverted within the past year, who have had symptoms of primary or secondary syphilis within the past year, or who have had a sexual partner with primary, secondary, or early latent syphilis within the past year. Patients who do not meet any of these criteria should be presumed to have late latent syphilis.
CNS involvement may be asymptomatic. Therefore, the possibility of neurosyphilis should be considered in patients with early or late latent syphilis.
Early latent syphilis is treated in the same way as primary and secondary syphilis. Late latent syphilis is treated with 2.4 million units of penicillin G benzathine administered intramuscularly once a week for three weeks. Alternative regimens in nonpregnant patients with penicillin allergy include doxycycline, in a dosage of 100 mg taken orally twice daily for four weeks, or tetracycline, in a dosage of 500 mg taken orally four times daily for four weeks.9
After treatment of early or late latent syphilis, quantitative nontreponemal titers should be measured at six, 12, and 24 months. Neurosyphilis should be strongly considered in patients who show a fourfold increase in titers, patients who have an initially high titer (1:32 or greater) that fails to decline at least fourfold, patients who have HIV infection, and patients who develop signs or symptoms of neurosyphilis.9
TERTIARY SYPHILIS
Tertiary or late syphilis is classified into gummatous syphilis, cardiovascular syphilis, and neurosyphilis. Gummas are granulomatous-like lesions; they are clinically significant because they cause local destruction.4 These lesions may affect any organ system but most commonly occur in the skin, mucous membranes, and bones.
Cardiovascular syphilis results from destruction of the elastic tissue of the aorta, which leads to aortitis and the formation of aneurysms that rarely rupture. The ascending aorta is most often affected, with the potential complications of aortic valve insufficiency and coronary artery stenosis. A diagnostic clue is the presence of linear calcifications of the aorta on a chest radiograph. Approximately 11 percent of untreated patients progress to cardiovascular syphilis.14
Antibiotic therapy for gummatous and cardiovascular syphilis is the same as that for late latent syphilis, provided no evidence of neurologic involvement is present. Consensus is lacking on the appropriate follow-up in patients who have tertiary syphilis with no CNS involvement. Clinical response to treatment varies and depends on the type and location of gummatous or cardiovascular lesions.9
NEUROSYPHILIS AT ANY STAGE OF SYPHILIS
Neurologic involvement occurs in up to 10 percent of patients with untreated syphilis.14 Neurosyphilis should be considered in patients with signs or symptoms of neurologic involvement at any stage of T. pallidum infection and in all patients with late latent or tertiary syphilis, although asymptomatic neurosyphilis is the most common presentation.4 Neurologic involvement also should be suspected in patients who previously have been treated for neurosyphilis, patients who have not responded to treatment for primary, secondary, or latent syphilis, and patients who have HIV infection or other conditions that compromise immune status.
Lumbar puncture is required to establish the diagnosis of neurosyphilis. The CSF should be tested for white blood cell count and protein level, and for reactivity on a VDRL test.5,15 Although a positive CSF VDRL test result is specific for neurosyphilis, a negative result does not exclude the possibility of this infection, because sensitivity is less than 100 percent. A CSF white blood cell count greater than 10 per mm3(10 × 106per L) or a CSF protein level greater than 50 mg per dL (0.50 g per L) indicates possible neurosyphilis.
Treponemal-specific testing (e.g., TPHA) is helpful only when the result is negative (i.e., it rules out neurosyphilis). Because IgG can cross the blood-brain barrier, a positive test may falsely imply CNS involvement.5 TPHA testing to compare serum and CSF values (TPHA index) may prove beneficial in establishing the diagnosis of neurosyphilis. Testing for spirochete DNA via poly-merase chain reaction methods is an evolving technique that may be helpful because it detects organisms, rather than antibodies, in the CSF.16
In late neurosyphilis, both vascular lesions (meningo-vascular neurosyphilis) and neuronal degeneration (parenchymatous neurosyphilis) are possible.4 The clinical manifestations of neurosyphilis include seizures, ataxia, aphasia, paresis, hyperreflexia, personality and cognitive changes, visual changes, hearing loss, neuropathy, and loss of bowel and bladder functions.
Penicillin is the only drug that has proved effective in the treatment of neurosyphilis. The CDC endorses two regimens.9 The first is aqueous crystalline penicillin G, in a dosage of 3 to 4 million units administered intravenously every four hours for 10 to 14 days. The second regimen consists of penicillin G procaine, in a dosage of 2.4 million units administered intramuscularly once daily, plus probenecid, in a dosage of 500 mg orally four times daily, with both drugs given for 10 to 14 days.
Follow-up of patients treated for neurosyphilis depends on the initial CSF findings.9 If pleocytosis was present, the CSF should be reexamined every six months until the white blood cell count is normal. Retreatment should be considered if the CSF white blood cell count does not decline after six months or completely normalize after two years.9 [Evidence level C, consensus/expert guidelines]
The CSF also can be reexamined to look for serial decreases in antibodies on the VDRL test or serial decreases in protein levels, although the management of persistent abnormalities is not well established. It is expected that CSF parameters will normalize within two years. Failure to normalize may warrant retreatment. Most treatment failures occur in immunocompromised patients.

