Oral ivermectin is an effective and cost-comparable alternative to topical agents in the treatment of scabies infection. It may be particularly useful in the treatment of severely crusted scabies lesions in immunocompromised patients or when topical therapy has failed. Oral dosing may be more convenient in institutional outbreaks and in the treatment of mentally impaired patients. Ivermectin has been used extensively and safely in the treatment of other parasitic infections, but the U.S. Food and Drug Administration has not approved the drug for the treatment of scabies infection. The safety of oral ivermectin in pregnant and lactating women and young children has yet to be established.
Scabies is a skin disease caused by infestation with the mite Sarcoptes scabiei. Although it may infest any human in any climate, it is most common in children younger than two years and is endemic in the tropics.1 The female mite, whose life expectancy is about 30 days, burrows into the epidermis to lay eggs. The eggs hatch into larvae in three to four days, and larvae mature into adults in 14 to 17 days.2 Male adult mites are smaller than females, remain on the skin surface, and die shortly after mating. There is evidence that mites can live for up to three days without a human host, and a reported outbreak of scabies among laundry workers provides evidence that fomites may spread disease.3 While animal strains of scabies exist and can infect humans, the mites cannot complete their life cycle or be passed to other hosts.4
Diagnosis
Symptoms of scabies infestation include rash and intense pruritus that is often worse at night. The lesions begin as tiny erythematous papules and can progress to vesicles or pustules. Linear burrows are a classic feature but are not seen commonly. Excoriation and ulceration also may be present, and a more generalized hypersensitivity reaction, including urticaria, may occur. In severe cases and in immunocompromised hosts, large areas of crusting may be seen.
Although outbreaks can occur almost anywhere, the axillae, web spaces between fingers, and flexor surfaces of the wrists are the most common areas. Male genitalia, female breasts, the gluteal crease, waistband, and antecubital fossae also are frequently affected. The face and scalp usually are spared except in infants.5
Typical distribution of lesions, intense pruritus, and patchy, discrete lesions with secondary excoriation signal scabies infection. The diagnosis usually is clinical but may be confirmed by skin scrapings near the newest and least disturbed skin lesions or under the fingernail edge.6 Light microscopy of the scrapings may detect the female mite, eggs, and feces pellets (Figure 1).
FIGURE 1.
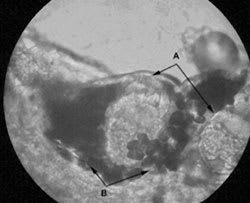
Photomicrograph of skin scraping of scabies larvae (A) surrounded by eggs and feces (B). (10 × 10)
Treatment
Topical sulfur treatments have been used for centuries to treat scabies infection. More recently, topical benzyl benzoate and lindane (Kwell) were mainstays of therapy. In 1990, a study7 comparing lindane with topical permethrin (Nix) showed improved efficacy of permethrin at 28 days, with a lower risk for neurotoxicity. Topical permethrin was subsequently compared favorably with 10 percent crotamiton (Eurax)8 and has became a widely used treatment for scabies (Table 1).9
TABLE 1 Comparison of Treatments for Scabies
| Drug | Cost* | Efficacy (%) | Adverse reactions | Use in children | Use in nursing women | Pregnancy category |
|---|---|---|---|---|---|---|
| Ivermectin (Stromectol) | $38 for 3 tablets at 6 mg† | 73 to 98 | Nausea, rash, dizziness, itching, eosinophilia, abdominal pain, fever, tachycardia‡ | Safety not proved in children <15 kg (33 lb) | Not recommended | C |
| Lindane (Kwell) | $17 for 60 mL (2 oz) 1% lotion | 85 to 98 | CNS toxicity, dizziness, seizures, renal and hepatic toxicity reported with overdosage | Safe in children ≥2 years of age | Not recommended | C |
| Permethrin (Nix) | $38 for 60 g (2.1 oz) 5% cream | 91 to 98 | Pruritus, burning, stinging; use with caution in patients with asthma. | Safe in children ≥2 months of age | Not recommended | B |
| CNS toxicity much less than with lindane |
CNS = central nervous system.
*— Retail costs supplied by the author, rounded to the nearest dollar.
†—Recommended dosage for 70 kg (154 lb) adult.
‡—Symptoms may be the result of an allergic reaction from the death of the parasites rather than a reaction to the drug.
Ivermectin (Stromectol) is related to macrolide antibiotics; it was developed in the 1970s as a veterinary treatment for animal parasites.10 Ivermectin also has been used to treat animal scabies, which causes mange.11 Ivermectin has been used in humans to treat millions of cases of onchocerciasis, other filariases, and intestinal nematodal infections such as strongyloidiasis.12
In 1993, a study13 comparing oral ivermectin with topical 10 percent benzyl benzoate found that absolute results favored the use of ivermectin, but the difference was not statistically significant. Studies in Africa14 and India15 have suggested that an effective dosage of ivermectin is 200 mcg per kg; at least three additional studies16–18 of the same dosage have confirmed ivermectin's efficacy as a treatment for scabies infection.
A small study of healthy patients and patients infected with human immunodeficiency virus (HIV)16 showed that a single dose of ivermectin (200 mcg per kg) was curative in most patients. Several HIV-infected patients required a second dose two weeks later, and one patient needed a third dose of ivermectin plus topical permethrin to cure the infection. A randomized study of 53 patients that compared topical lindane with oral ivermectin showed that 15 days after treatment, 74 percent of patients who took ivermectin a n d 59 percent of patients who used topical lindane were cured; this difference was not statistically significant.17 [Evidence level A, randomized controlled trial (RCT)] Four weeks after treatment, one patient treated with ivermectin and two patients treated with lindane had evidence of continuing infection. Another trial randomized 200 patients to oral ivermectin or topical lindane; 83 percent of patients treated with ivermectin were cured at four weeks compared with 44 percent of patients treated with lindane.18 [Evidence level B, lower quality RCT] However, complete follow-up was available in only 75 percent of patients.
Only one published study is available comparing oral ivermectin with topical permethrin. Patients were randomized to take a single dose of ivermectin (200 mcg per kg) or use topical 5 percent permethrin.19 [Evidence level A, RCT] Fewer patients responded to ivermectin at the one- and two-week follow-ups than to permethrin. At the end of the second week, patients who did not respond to either treatment (12 in the ivermectin group and one in the permethrin group) repeated the dose. At the end of four and eight weeks, all but two patients in the ivermectin group and all patients in the permethrin group had been cured; this difference was not statistically significant. The study concluded that a single dose of permethrin was superior to a single dose of ivermectin.
Safety
An estimated 6 million people worldwide have taken ivermectin for various parasitic infestations.15 No serious drug-related adverse events have been reported. Side effects of ivermectin include fever, headache, chills, arthralgia, rash, eosinophilia, and anorexia.15 Many of these symptoms are thought to result from the death of parasites rather than as a reaction to the drug.
Ivermectin seems to be concentrated in the liver and fat tissue, with very low levels reaching the central nervous system.20 No significant drug interactions have been reported.21
A study of elderly nursing home patients treated for scabies infection showed an increased death rate among ivermectin-treated patients,22 but it was noted that this finding has not been confirmed in multiple subsequent trials.
Ivermectin is not approved for treatment of scabies by the U.S. Food and Drug Administration. There are concerns regarding its use in young children and pregnant women, because there may be more drug penetrance of the immature blood-brain barrier.
Role of Ivermectin
Although standard topical treatment of scabies is effective in many patients, there may be a particular role for oral ivermectin in refractory infestations or when compliance with head-to-toe application of topical agents is logistically difficult (e.g., large institutional outbreaks or mentally impaired patients). Immunocompromised patients with crusted scabies have very high parasite loads and also may benefit from oral treatment. Some authors recommend concomitant oral and topical treatment because systemic medication may not effectively penetrate thick, crusted areas.22 Topical formulations of ivermectin also exist but have been less widely studied.
Cost
A single dose of ivermectin for a 70-kg (154-lb) adult costs about $38 (for three 6-mg pills) or about $67 for the same dose in 3-mg pills. Lindane (2 oz of 1 percent lotion) costs about $17, and permethrin (2 oz of 5 percent cream) costs about $38. (Retail prices provided by the author, rounded to the nearest dollar.)

