Joint and soft tissue injection of the ankle and foot region is a useful diagnostic and therapeutic tool for the family physician. This article reviews the injection procedure for the plantar fascia, ankle joint, tarsal tunnel, interdigital space, and first metatarsophalangeal joint. Indications for plantar fascia injection include degeneration secondary to repetitive use and traumatic injuries that are unresponsive to conservative treatment. Diagnostic aspiration or therapeutic injection of the ankle or first metatarsophalangeal joints can be performed for management of advanced osteoarthritis, rheumatoid arthritis, and other inflammatory arthritides such as gout, or synovitis or an arthrosis such as “turf toe.” Persistent pain and disability resulting from tarsal tunnel syndrome, an analog of carpal tunnel syndrome of the wrist, respond to local injection therapy. A painful interdigital space, such as that occurring in patients with Morton's neuroma, is commonly relieved with corticosteroid injection. The proper technique, choice and quantity of pharmaceuticals, and appropriate follow-up are essential for effective outcomes.
This article, the final in a series on diagnostic and therapeutic injections, covers the ankle and foot. The rationale, indications, contraindications, and general approach to this procedure are covered in the first article in this series.1 Subsequent articles have covered injections of the shoulder, elbow, wrist and hand, hip, and knee regions.2–5
The ankle and foot are susceptible to multiple injuries and inflammatory conditions6 that are amenable to diagnostic and therapeutic injection.7 This article covers the anatomy, pathology, diagnosis, and injection technique at common sites for which these procedures are applicable. These areas include the plantar fascia, ankle joint, tarsal tunnel, interdigital space, and first metatarsophalangeal joint (Figure 1).
FIGURE 1.
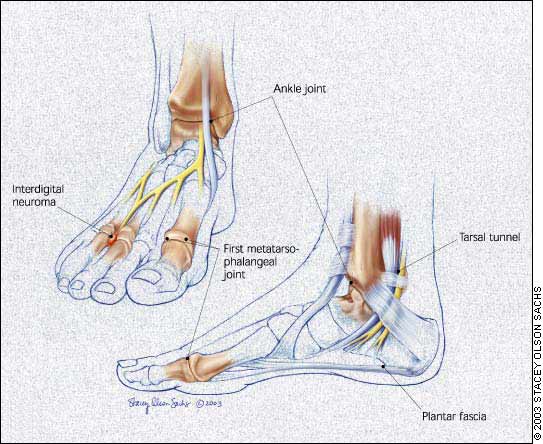
Injection target points.
Plantar Fascia
The plantar fascia, a band of connective tissue deep to the fat layer of the base (plantar aspect) of the foot, spans from the medial plantar tuberosity of the calcaneus to the base of the digits. It helps support the medial longitudinal arch of the foot.
INDICATIONS AND DIAGNOSIS
The plantar fascia is frequently a site of chronic pain.8,9 Patients typically complain of pain that starts with the first step on arising in the morning or after prolonged sitting. Pain onset is usually insidious but also may commence after a traumatic injury. Diagnosis is made by eliciting pain with palpation in the region of the origin of the plantar fascia. Pain may be worsened by passive dorsiflexion of the foot. Overpronation, pes cavus, and restricted foot dorsiflexion are common with this condition, although foot pronation itself has not been demonstrated to be a predisposing factor.10
TIMING AND OTHER CONSIDERATIONS
In plantar fasciitis, corticosteroid injection is a treatment option, usually after other therapeutic modalities have failed. These therapies include active stretching, and use of non-steroidal anti-inflammatory drugs (NSAIDs), cushioning heel cups, nighttime plantar fascia splints, and foot orthoses.11–13 Corticosteroid injection effectively provides pain relief,14 although it carries the risk of plantar fascia rupture15 and fat pad atrophy.
TECHNIQUE
Pharmaceuticals and equipment are listed in Table 1. The patient is placed in the lateral recumbent position with the affected side down. The physician identifies the medial aspect of the foot and palpates the soft tissue just distal to the calcaneus, locating the point of maximal tenderness or swelling.
TABLE 1 Equipment and Pharmaceuticals
| Site | Syringe | Needle | Anesthetic | Corticosteroid | Hydrocortisone equivalents per injection (mg) | |
|---|---|---|---|---|---|---|
| Plantar fascia | 5 mL | 25 gauge, 1.5 inch | 2 mL of 1% lidocaine (Xylocaine) or 0.25% or 0.5% bupivacaine (Marcaine) | 1 mL of Celestone* | 150 | |
| or | ||||||
| 1 mL of 40 mg per mL of methylprednisolone (Solumedrol) | 200 | |||||
| Ankle joint | 10 mL (30 to 60 mL if aspirating) | 25 gauge, 1 to 1.5 inch (18 gauge, 1.5 inch if aspirating)† | 3 to 5 mL of 1% lidocaine or 0.25% or 0.5% bupivacaine | 1 mL of Celestone | 150 | |
| or | ||||||
| 1 mL of Solumedrol | 200 | |||||
| Tarsal tunnel | 3 to 5 mL | 25 gauge, 1 or 1.5 inch | 1 to 2 mL of 1% lidocaine or 0.25% or 0.5% bupivacaine | 0.5 mL of Celestone | 75 | |
| or | ||||||
| 0.5 mL of Solumedrol | 100 | |||||
| Interdigital space | 3 to 5 mL | 25 gauge, 1.5 inch | 2 mL of 1% lidocaine or 0.25% or 0.5% bupivacaine | 0.5 mL of Celestone | 75 | |
| or | ||||||
| 0.5 mL of Solumedrol | 100 | |||||
| First metatarsophalangeal joint | 3 mL (10 mL if aspirating) | 25 to 27 gauge, 1 or 1.5 inch† | 1 mL of 1% lidocaine or 0.25% or 0.5% bupivacaine | 0.25 to 0.5 mL of Celestone | 37.5 to 57.5 | |
| or | ||||||
| 0.25 to 0.5 mL of Solumedrol | 50 to 100 | |||||
*—1 mL of Celestone is 3 mg each of betamethasone sodium phosphate and betamethasone acetate.
†—A hemostat is needed to immobilize the needle when injection follows aspiration.
APPROACH AND NEEDLE ENTRY
General technique, including premedication, is discussed in the first article in this series. At the defined soft tissue area, a 25-gauge, 1.5-inch needle is inserted perpendicular to the skin (Figure 2). The needle should be inserted directly down past the midline of the width of the foot. The physician should not inject into the fat pad at the base of the foot.
FIGURE 2.
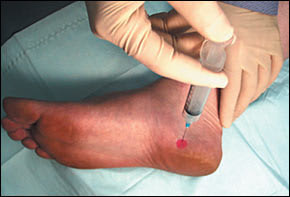
Plantar fasciitis injection.
The pharmaceutical material is injected slowly and evenly through the middle one third of the width of the foot while the needle is being withdrawn. The physician should avoid injecting through the base of the foot, because this approach can result in the complications of pharmaceutical leakage and fat pad atrophy.
The patient should remain in the supine position for several minutes after the injection. The physician may put the injected region through passive range of motion. The patient should remain in the office for 30 minutes after the injection to be monitored for adverse reactions. In general, patients should avoid any strenuous activity involving the injected region for at least 48 hours. Patients should be cautioned that they may experience worsening symptoms during the first 24 to 48 hours. This is related to a possible steroid flair, which can be treated with ice and NSAIDs (e.g., ibuprofen, naproxen). A follow-up examination within three weeks should be arranged.
Ankle Joint
The ankle joint is formed by the articulation of the talus with the tibia and fibula. The medial and lateral malleoli of the tibia and fibula stabilize the talus.
INDICATIONS AND DIAGNOSIS
Arthritis of the ankle joint may occur in athletes with a history of trauma to the area, and in older patients, and can be an indication for corticosteroid joint injection. Besides osteoarthritis, rheumatoid arthritis, and acute traumatic arthritides, other indications for joint injection include crystalloid deposition disease, mixed connective tissue disease, and synovitis.16,17 Pain and disability are the usual presenting complaints, and examination can reveal pain with limitation of motion, tenderness, swelling, crepitus, and deformity. Gait disturbance, erythema, and warmth to palpation also may be present. Radiographs may be helpful to support the diagnosis.
TIMING AND OTHER CONSIDERATIONS
Aspiration of the joint must be performed if infection is suspected. Infection is an absolute contraindication to corticosteroid joint injection. Aspiration also can be useful for confirming certain arthropathies such as crystalloid deposition disease and Lyme arthritis.
TECHNIQUE
Pharmaceuticals and equipment are listed in Table 1. The patient is placed in the supine position with the ankle relaxed. The physician identifies the space between the anterior border of the medial malleolus and the medial border of the tibialis anterior tendon and palpates this space for the articulation of the talus and tibia.
APPROACH AND NEEDLE ENTRY
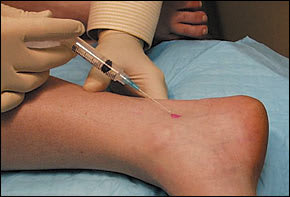
As with any joint aspiration or injection procedure, sterile technique must be followed. The needle is inserted into the identified space and directed posterolaterally (Figure 3). Reduced resistance will be felt on entering the joint space, making aspiration and the free flow of pharmaceuticals possible. When aspiration precedes injection, the needle is held with a hemostat while the syringe is changed. Follow-up care is the same as that described for injection of the plantar fascia.
FIGURE 3.
Ankle joint injection.
Tarsal Tunnel
The tarsal tunnel is formed by the medial malleolus and a fibrous ligament, the flexor retinaculum. The posterior tibial nerve passes through the tunnel and can be compressed by any condition that reduces the space of the tunnel. The medial plantar, lateral plantar, and calcaneal branches of the posterior tibial nerve innervate the base of the foot.
INDICATIONS AND DIAGNOSIS
Patients with arthritis of the tarsal tunnel may complain of a burning sensation, pain, and paresthesias over the distribution of the posterior tibial nerve and its branches that worsen with weight bearing.18 Symptoms are often related to chronic conditions such as impingement syndromes and hyperpronation, or may be secondary to acute trauma.19,20 Eliciting a positive Tinel's sign by tapping over the tarsal tunnel typically causes discomfort in the medial one third of the distal plantar foot, although the entire plantar foot surface may be affected.
TIMING AND OTHER CONSIDERATIONS
Injection is a modality that is performed after a treatment program that can include stretching, rest, and the use of shoe inserts or orthoses, and NSAIDs.21
TECHNIQUE
Pharmaceuticals and equipment are listed in Table 1. The patient is placed in the lateral recumbent position with the affected foot down. Behind the medial malleolus, the point over the posterior tibial nerve where percussion elicits the symptoms is identified. Having the patient actively invert the foot against resistance will help the physician identify the posterior tibial tendon. The nerve lies posterior to the tendon.
APPROACH AND NEEDLE ENTRY
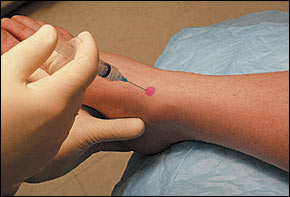
At approximately 2 cm proximal to the identified location, the needle is inserted at an angle of 30 degrees to the surface of the skin and directed distally (Figure 4). This injection is relatively superficial. The final needle depth will be determined by the amount of subcutaneous tissue. The physician should aspirate before injecting to ensure that the needle is not in an artery or a vein. The pharmaceutical agent is injected slowly. Follow-up care is the same as that previously described.
FIGURE 4.
Tarsal tunnel injection.
Interdigital Space
The interdigital spaces of the foot are sites for the occurrence of painful neuromas, a condition termed Morton's neuroma. The second and third common digital branches of the medial plantar nerve are the most frequent sites for development of interdigital neuromas.
INDICATIONS AND DIAGNOSIS
Morton's neuromas develop secondary to chronic trauma and repetitive stress, as occurs in persons wearing tight-fitting or high-heeled shoes.22 Pain and paresthesias are usually insidious at onset and are located in the interdigital space of the affected nerve. In some cases, the interdigital space between the affected toes may be widened as a result of an associated ganglion or synovial cyst. Pain is elicited in the affected interdigital space when the metatarsal heads of the foot are squeezed together. Injection with 1 percent lidocaine (Xylocaine) can be helpful in confirming the diagnosis.
TIMING AND OTHER CONSIDERATIONS
Treatment for Morton's neuroma can include the use of NSAIDs, metatarsal pads, orthoses, proper footwear, and injection. Injection may be considered as an early therapeutic option.23 Surgery is a last resort.
TECHNIQUE
Pharmaceuticals and equipment are listed in Table 1. The patient is placed in a supine position with the knee in a supported flexed position (e.g., with a pillow beneath it) and the foot in a relaxed neutral position. The physician palpates the area of tenderness and fullness on the dorsum of the foot between the affected metatarsal heads.
APPROACH AND NEEDLE ENTRY
Injection is performed by inserting the needle on the dorsal foot surface in the distal to proximal direction, at an angle of 45 degrees, and down to the area of fullness between the metatarsal heads (Figure 5). Position is key, because plantar fat pad atrophy can occur if the fat pad is injected.24 Follow-up care is the same as that previously described.
FIGURE 5.
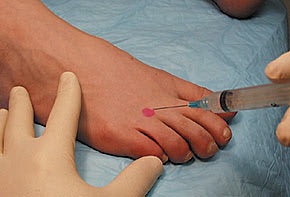
Interdigital neuroma injection.
First Metatarsophalangeal Joint
The first metatarsophalangeal joint varies in size and shape, and it may be difficult to palpate in patients with conditions such as advanced degenerative arthritis.
INDICATIONS AND DIAGNOSIS
Diagnostic aspiration or therapeutic injection of the first metatarsophalangeal joint can be performed in the management of advanced osteoarthritis, rheumatoid arthritis, and other inflammatory arthritides such as gout, or for synovitis or an arthrosis such as “turf toe.”25–27 Turf toe, a painful ligamentous injury resulting from hyperextension of the first metatarsophalangeal joint, often occurs in football linemen. Diagnosis of the specific underlying condition entails eliciting supporting historic and physical findings and, possibly, diagnostic laboratory tests and imaging studies.
TIMING AND OTHER CONSIDERATIONS
Treatment is specific to the underlying condition. Injection may be considered as a diagnostic or therapeutic adjunct. Aside from diagnostic aspiration, therapeutic injection may be used early in the course of certain inflammatory arthritides, such as gout.
TECHNIQUE
Pharmaceuticals and equipment are listed in Table 1. The patient is placed in a supine position with the knee in a supported flexed position (e.g., with a pillow beneath the knee), and the foot is firmly supported by the table. The physician palpates the joint line on the dorsum of the foot and passively flexes and extends the toe to locate the joint line.
APPROACH AND NEEDLE ENTRY
Distal traction may be applied to the great toe to open the joint space. The needle is inserted on the dorsomedial or dorsolateral surface (Figure 6). The needle should be angled 60 to 70 degrees to the plane of the foot and pointed distally to match the slope of the joint. The joint space is not deep below the skin surface. The physician should aspirate before injecting; the injectable agent should flow without major resistance when the needle is positioned properly in the joint space. Follow-up care is the same as that previously described.
FIGURE 6
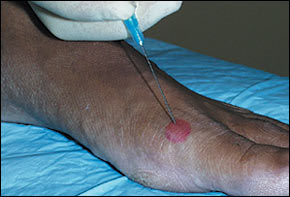
First metatarsophalangeal joint injection.

