
Am Fam Physician. 2003;68(12):2433-2434
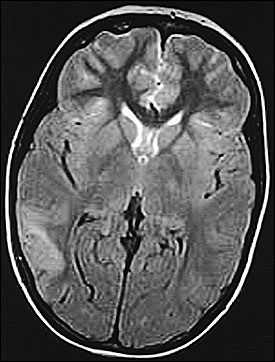
A 20-year-old woman with an unremarkable medical history presented to the emergency department with a right-sided headache and weakness of the left arm. She had felt warm intermittently during the previous week. She had no history of migraines, visual disturbances, neck stiffness, head trauma, or cancer. The headache was reported to be one of the worst headaches of her life. The physical examination revealed a temperature of 37.3°C (99.2°F) and mildly decreased strength in the left upper extremity. A computed tomography (CT) scan of her head was obtained, which revealed no apparent abnormalities. Several days later, the patient complained of persistent upper extremity weakness, and a magnetic resonance image (MRI) of the brain was performed, from which a single T2-weighted image is provided (see accompanying figure).
Question
Discussion
The answer is C: viral encephalitis. The single T2-weighted image of the brain shows abnormal asymmetric increased signal at the right temporal-parietal gray matter. There was little enhancement of the abnormal area after intravenous gadolinium contrast administration (not shown). This appearance of edema involving the temporal lobe was suggestive of viral encephalitis. The patient promptly received a course of antiviral therapy and recovered strength in her left upper extremity. Herpes simplex virus (HSV) was later confirmed as the causative agent by a rise in the cerebrospinal fluid antibody titer.
Meningitis has a different appearance on MRI. Dural, leptomeningeal, or ependymal enhancement are typical findings, none of which were present in this patient. Intracerebral hemorrhage usually appears as a hypointense area on T2-weighted imaging and likely would have been apparent on CT imaging as well. Cerebral abscesses are typically circumscribed lesions with surrounding vasogenic edema. Cerebral metastases most commonly appear as multiple lesions showing contrast enhancement on T1-weighted imaging, again not seen in this patient.
Viral encephalitis in adults usually involves HSV-1 infection. The virus resides in the trigeminal ganglion during the latent phase, likely having originated from a previous infection of the face. Symptoms of herpetic encephalitis may include headache, confusion, seizures, or lethargy. The most common parenchymal areas of involvement are the frontal and temporal lobes. The mechanism by which the virus reaches the brain remains controversial. Because herpetic encephalitis often has neurologic sequelae and may have a fulminant course in some cases, even with treatment, it is essential to obtain a diagnosis and begin treatment as early as possible.
Unfortunately, MRI and CT are not reliable for showing early signs of encephalitis. Treatment often must be started based on characteristic clinical manifestations alone, or demonstration of HSV DNA in cerebrospinal fluid by polymerase chain reaction testing, where available. Brain biopsy rarely is performed today, but it is occasionally indicated to confirm the diagnosis or to search for other less common causes of encephalitis.1 A rise in the cerebrospinal fluid antibody titer for HSV is diagnostic but may take up to 20 days to appear.
Although CT and MRI are not definitive for the diagnosis of encephalitis, parenchymal involvement of the temporal or frontal lobes is strong enough evidence to warrant initiating treatment with antiviral agents. CT may show hypodense involvement of the temporal or frontal lobes.2 MRI findings early in the course of infection include gyral swelling or high signal intensity on T2-weighted images, followed by extension of the infection, hemorrhage, and increasing areas of contrast enhancement. Eventually, atrophy of the affected areas of the brain occurs.3 Typically, gray and white matter are involved. It is unclear whether MRI will show findings earlier than CT imaging; however, positive findings are much more obvious on MRI. MRI is more sensitive than CT in suggesting the diagnosis of viral encephalitis and for demonstration of infection sequelae, such as gliosis and atrophy.4
Viral encephalitis caused by HSV-2 is much less common. It typically occurs in neonates who are inoculated during birth through the vaginal canal. Congenital HSV-2 infection is systemic, with generalized central nervous system involvement. CT of the brain demonstrates diffuse parenchymal hypodensity and, frequently, intracranial calcifications. MRI shows diffuse hypointensity on T1-weighted imaging, with corresponding hyperintensity on T2-weighted imaging.2