
Am Fam Physician. 2004;69(1):175-176
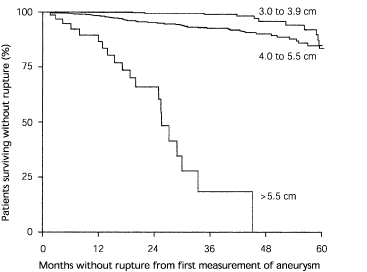
In patients with abdominal aortic aneurysms with a diameter larger than 6 cm, the risk of rupture is increased markedly, and surgical repair is indicated if the patient can tolerate the intervention (see accompanying figure). However, only 10 percent of abdominal aortic aneurysms are this large when detected by screening examinations. Powell and Greenhalgh review the epidemiology of abdominal aortic aneurysms and give recommendations for management of smaller aneurysms (3 to 6 cm in diameter).
Abdominal aortic aneurysms are found three times as often in men as in women. Smoking is the strongest risk factor; 90 percent of all patients with abdominal aortic aneurysms have smoked. The incidence of aneurysm increases sevenfold in those who smoked more than one pack of cigarettes per day. Atherosclerosis also is believed to be a cause of abdominal aortic aneurysms. Overall, more than one half of these patients die from a cardiovascular cause rather than from a ruptured aneurysm.
Screening all men more than 55 years of age would reveal clinically significant aneurysms (larger than 4 cm) in only 1 percent of the population. Selectively screening patients with intermittent claudication roughly doubles this yield. There is also a familial tendency toward abdominal aortic aneurysms. Screening the siblings (older than 50 years of age) of a patient with abdominal aortic aneurysm detects aneurysms in approximately 29 percent of brothers and 6 percent of sisters.
Two large randomized trials have examined the efficacy of surgical management of smaller aneurysms (diameter, 4.0 to 5.5 cm). A U.K. study found a perioperative mortality rate from surgical repair of 5.6 percent compared with a mortality rate of 2.7 percent in a study of U.S. veterans. Neither study showed an overall survival benefit to surgical intervention after six-year follow-up. Nine-year follow-up from the U.K. trial revealed a slight trend toward better survival with surgical repair, but it was not statistically significant. Investigators attributed the difference to the greater rate of smoking cessation among those who had surgical treatment. The majority of patients who were randomized to observation eventually required surgical repair when their aneurysms increased beyond a diameter of 5.5 cm.
The review authors recommend delaying surgical repair of abdominal aortic aneurysms 5.5 cm in diameter. The risk of aneurysm rupture is four times as high in women. Although there should be a lower threshold for surgical repair in women, the authors did not think that a specific numeric cutoff could be recommended, based on the data.
Smoking is the most important risk factor to be modified in patients with an abdominal aortic aneurysm. Unexpectedly, the authors found that hypertension, hyperlipidemia, and diabetes are not associated with greater rates of aneurysm dilation. There may even be a future role for antibiotic therapy in slowing abdominal aortic aneurysm growth, perhaps through inhibition of macrophage proteolytic enzymes.
The authors recommend ultrasound examination as a safe, noninvasive, and cost-effective method for abdominal aortic aneurysm screening and surveillance. However, data from a screening trial of more than 67,000 men showed that although screening reduced aneurysm-related mortality by one half within four years, there was no overall reduction in mortality. The study also found that patients with a detected abdominal aortic aneurysm reported a reduced quality of life.
Surgical repair of abdominal aortic aneurysms typically involves either open repair or use of an endovascular stent. Currently, no data shows that either method is superior overall.