Viral croup is the most common form of airway obstruction in children six months to six years of age. The frightening nature of croup often prompts parents and caregivers to seek physician consultation. For children with mild croup, symptomatic care and mist therapy may be all that is necessary. Epinephrine has been used for decades to treat more severe cases of croup, but recent meta-analyses have found that glucocorticoid use is associated with shorter hospital stays, improvement in croup scores, and less use of epinephrine. Studies have shown that treatment with 0.6 mg per kg of oral dexamethasone is as effective as intramuscular dexamethasone or 2 mg of nebulized budesonide. Oral dexamethasone in dosages as low as 0.15 mg per kg also may be effective. While more studies are needed to establish guidelines, oral dexamethasone can be used to treat mild to moderate croup with close follow-up and instructions for further care, if needed.
Croup is a common childhood illness, and viral croup is the most common form of airway obstruction in children six months to six years of age.1 The annual incidence is up to six cases per 100 children younger than six years.2,3 Croup is a leading cause of hospitalization in children younger than four years,4 and study results show that 1.5 to 6 percent of children with croup require hospitalization.3,5,6 The annual cost of hospitalizations for croup in the United States is an estimated $56 million.4,5
Croup accounts for 15 percent of respiratory tract infections among children in practice,7 and during the second year of life, 1 to 5 percent of children will need outpatient evaluation for croup.6 Because the respiratory distress associated with croup is frightening for patients and caregivers, physicians in office or emergency department settings often are consulted. While steroids have been used for years to decrease respiratory distress in children with croup, new evidence suggests benefit from the use of oral steroids in the outpatient setting.
Definition
“Croup” is a generic term encompassing a heterogeneous group of illnesses affecting the larynx, trachea, and bronchi.1 Laryngotracheitis, laryngotracheobronchitis, laryngotracheobronchopneumonitis, and spasmodic croup are included in the croup syndrome. In children with croup, upper airway obstruction causes a barking cough, a hoarse voice, inspiratory stridor, and varying degrees of respiratory distress.
Viral croup affects children six months to 12 years of age, with a peak incidence at two years of age.8 Boys are affected more often than girls at a ratio of 1.5:1.0,9 and although the disease can occur throughout the year, it predominates in the fall and winter months.
Etiology
Parainfluenza viruses (types 1, 2, and 3) are the most frequent cause of croup, accounting for almost 75 percent of all cases.2,6–11 Human parainfluenza virus 1 (HPIV-1) is the most common, estimated to cause 18 percent of all cases of croup.6 HPIV-1 has had an unusual pattern of biennial epidemics during the autumn months of odd-numbered years since 1973.6 Adenovirus, respiratory syncytial virus, rhinovirus, enteroviruses, and influenza viruses A and B also may cause laryngotracheobronchitis.6,7,11 Rarely, Mycoplasma pneumoniae has been isolated from children with mild croup.7,9,11 Table 112 lists viral etiologic agents of croup and measures of their severity. Foreign body aspiration, trauma, and allergic reaction (acute angioneurotic edema) are among the noninfectious causes of airway obstruction and are included in the differential diagnosis of patients presenting with stridor.6
TABLE 1 Etiologic Agents of Viral Croup
| Etiologic virus | Frequency | Severity |
|---|---|---|
| Parainfluenza viruses | Most frequent | Mild to severe |
| Influenza A and B | Occasional to frequent | Variable, most severe cases are seen with influenza A |
| Adenovirus | Occasional | Mild to moderate |
| Measles | Occasional | Moderate to severe |
| Respiratory syncytial virus | Occasional | Mild to moderate |
Adapted from Cherry JD. Croup. In: Feigin RD, Cherry JD, eds. Textbook of pediatric infectious diseases. 4th ed. Philadelphia: Saunders,1998:230.
TABLE 2 Comparison of Viral Croup and Spasmodic Croup
| Characteristic | Viral croup | Spasmodic croup |
|---|---|---|
| Age | Six months to six years (most common) | Six months to six years (most common) |
| Prodrome | Common | Uncommon |
| Stridor, barking cough | Common | Common |
| Fever | Common | Uncommon |
| Wheezing | Common | Common |
| Duration | Two to seven days | Two to four hours |
| Family history | No | Yes |
| Predisposition to asthma | Uncommon | Common |
Adapted with permission from DeSoto H. Epiglottitis and croup in airway obstruction in children. Anesthesiol Clin North Am 1998;16:860.
Some authors have tried to differentiate spasmodic croup from viral croup, but often the distinction is not possible. Classically, patients with spasmodic croup develop symptoms suddenly, without a clearly identifiable viral prodrome. Histologic evaluation of the subglottic tissues in patients with spasmodic croup shows noninflammatory edema.6 Although associated with the same viruses that cause croup, spasmodic croup tends to recur and may represent an allergic reaction to viral antigens instead of a direct infection. Because croup is difficult to differentiate on clinical grounds and can be associated with recent viral infection, most authors feel that it should be considered within the spectrum of illness of viral croup.13 Table 21 compares viral and spasmodic croup.
Bacterial tracheitis most commonly involves infection with Staphylococcus aureus, Haemophilus influenzae, and Corynebacterium diphtheriae.9 Although bacterial tracheitis should be considered in the differential diagnosis of croup, it will not be discussed further in this article.
The anatomic makeup of the childhood larynx helps to explain how the symptoms of croup develop. The subglottic region of the larynx is held within the rigid ring of the cricoid cartilage. In children with croup, viral infection causes this area to become inflamed and edematous, which can lead to obstruction. Because small children have a very narrow larynx, even a small decrease in airway radius causes a large decrease in airflow, leading to the symptoms of croup.
Clinical Course
Viral croup typically is preceded by 12 to 72 hours of low-grade fever and coryza. As the illness progresses, hoarseness and the characteristic “croupy”or barking cough will develop. Other symptoms include dyspnea, hoarseness, stridor, and wheezing.1 Symptoms are worse at night, peak between 24 and 48 hours, and generally resolve within one week.5,10 Agitation and crying tend to aggravate symptoms, and children often prefer to sit up or be held upright. Current treatment methods have reduced the mortality and morbidity associated with viral croup, but approximately 15 percent of patients experience a complication of the illness,11 including otitis media, dehydration and, rarely, pneumonia.
TABLE 3 Differential Diagnosis of Croup
| Acute laryngeal fracture |
| Angioneurotic edema |
| Arnold-Chiari deformity |
| Bacterial tracheitis |
| Burns or thermal injury |
| Dandy-Walker syndrome |
| Diphtheria |
| Epiglottitis |
| Extrinsic obstruction by a vascular ring |
| Foreign body |
| Laryngeal papillomatosis |
| Laryngomalacia |
| Neoplasm or hemangioma |
| Peritonsillar abscess |
| Retropharyngeal abscess |
| Smoke inhalation |
| Subglottic stenosis |
| Viral croup |
| Vocal cord paralysis |
Information from DeSoto H. Epiglottitis and croup in airway obstruction in children. Anesthesiol Clin North Am 1998;16:853–68.
Diagnosis
The clinical diagnosis of croup is made when the symptoms match the clinical course already outlined. Table 31 lists a differential diagnosis of croup, and Table 41 compares the features of croup and epiglottitis.
Radiologic evaluation may or may not aid physicians in the diagnosis of croup. Only 50 percent of patients with croup show the classic steeple sign on plain neck radiography.7 The steeple sign is the result of a narrowed column of subglottic air seen on a posterior-anterior view and an overdistended hypopharynx on the lateral view (Figure 1). While radiography may help to confirm clinical suspicion of croup, computed tomography may be more sensitive in defining the cause of obstructive disease in more confusing clinical settings.14 These include stridor before six months of age, stridor with activity, or the suspicion of mass on plain radiography.
TABLE 4 Comparison of the Features of Epiglottitis and Croup
| Characteristic | Epiglottitis | Croup |
|---|---|---|
| Age | Can occur in infants, older children, or adults | Six months to six years |
| Onset | Sudden | Gradual |
| Location | Supraglottic | Subglottic |
| Temperature | High fever | Low-grade fever |
| Dysphagia | Severe | Mild or absent |
| Dyspnea | Present | Present |
| Drooling | Present | Absent |
| Cough | Uncommon | Characteristic cough |
| Position | Sitting forward with mouth open | Comfortable in different positions |
| Radiography | Positive thumb sign* | Positive steeple sign |
*—Enlarged round epiglottis that looks like a thumb print.
Adapted with permission from DeSoto H. Epiglottitis and croup in airway obstruction in children. Anesthesiol Clin North Am 1998;16:855.
Most children with croup have normal pulse oximetry. Alveolar gas exchange usually is unimpaired. Hypoxia and low oxygen saturation will not be detected until the condition is severe. Occasionally, children with spasmodic croup have lower than expected oxygen saturation.9
FIGURE 1.
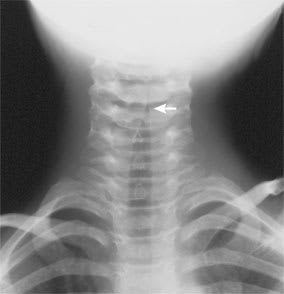
The classic steeple sign (arrow) of croup on radiograph.
The majority of children who have viral croup do not require direct visualization of the laryngeal area or intubation.7,9 However, visualization may be appropriate in children with symptoms suggestive of epiglottitis (e.g., acute, rapid respiratory distress; solid and liquid dysphagia; drooling), a deteriorating course of illness, or in those who do not improve as expected. Laryngoscopy also should be considered in children who have noisy breathing or an abnormal voice between episodes of croup, those who have frequent episodes or progressively more severe croup, and children who were intubated for any reason during the neonatal period. Children younger than four months or those with a longstanding history of stridor should be evaluated for anatomic obstruction.13 Abnormal findings include subglottic hemangiomas, laryngeal polyps, and vocal cord paralysis.9,13
The most useful monitoring method for children with croup is serial observation and frequent physical examination. Although a croup severity score was developed by Westley15 and some researchers have used pulsus paradoxus to evaluate treatment effect,16 neither method has been assessed for clinical usefulness.
Prognosis
Croup is usually a self-limiting disease with an excellent prognosis. Of children who develop croup, only a few will require inpatient care, and less than 5 percent of those will require intubation.9 Death from croup is rare, provided good airway management is carried out. However, it is unclear whether children with a history of croup are at increased risk of developing asthma.17–19 Studies in older children show that those with a history of hospital admission for croup have a higher prevalence of bronchial hyperresponsiveness, allergic skin response, and increased total serum IgE levels, compared with other children.18,19 Most of these studies were retrospective and did not take into account the severity of croup or its recurrence.
Management of Croup
The most important aspect in the treatment of patients with croup is airway maintenance. The standard management of croup includes mist therapy, corticosteroids, and racemic epinephrine. Any child with croup and evidence of respiratory distress should be considered a candidate for steroid treatment. Less frequently, hospitalization and intubation are necessary.
MIST THERAPY
Since the 19th century, mist treatment has been used to relieve croup symptoms.20 Theoretically, inspired air that is cooler than body temperature and less than 100 percent saturated with water vapor will result in mucosal cooling, vasoconstriction, and lessened edema.11 In addition, cool mist moistens secretions, soothes inflamed mucosa, and decreases the viscosity of mucous secretions.9 Many physicians recommend that parents take the symptomatic child into the bathroom while running a hot shower and filling the room with warm water vapor. Warm steam may ease symptoms. Bundling the child and taking him or her in the cool outside air also may be effective. In the inpatient setting, croup tents rarely are used because they increase anxiety and make observation more difficult.9
STEROIDS
Since the 1970s, corticosteroid use for croup has been debated. A 1989 meta-analysis by Kairys21 demonstrated benefit in the inpatient setting. More recently, results of a meta-analysis showed that treatment with glucocorticoids is effective in improving symptoms within six hours, for up to 12 hours, with significant improvement in croup scores, shorter hospital stays, and less use of epinephrine.2 [Evidence level A: meta-analysis of randomized controlled trials (RCTs)] A Cochrane review of 24 studies involving more than 2,000 children concluded that treatment with corticosteroids reduces the Westley croup score at six hours.22 [Evidence level A: meta-analysis of RCTs] However, most of the included studies took place in emergency departments or on the hospital floor after admission. While it seems clear that steroids provide benefit in the treatment of croup, more recent studies have tried to determine the optimal method of administration and the applicability of the treatment in the office setting.
To determine whether nebulized steroids are more effective than placebo in the treatment of croup, investigators performed a systematic review.23 The results indicated that, compared with the placebo group, children treated with nebulized steroids are significantly more likely to show an improvement in croup score by five hours and significantly less likely to require hospital admission after visiting the emergency department.23
One study24 compared nebulized and oral steroids in the treatment of croup. Investigators randomized 199 patients to receive oral dexamethasone (0.6 mg per kg) and nebulized placebo, oral placebo and 2 mg of nebulized budesonide, or oral dexamethasone and nebulized budesonide. All three groups had similar decreases in croup scores, indicating that the choice of oral versus nebulized corticosteroids should be based on availability, ease of administration, and cost.24
The outpatient treatment of croup with oral versus intramuscular dexamethasone also has been studied. In one study,8 investigators enrolled 277 patients who were in the emergency department to receive oral or intramuscular dexamethasone (0.6 mg per kg). No significant difference was detected in the need for further intervention, which led investigators to conclude that a single oral dose of dexamethasone can be used in the outpatient management of croup.8 [Evidence level B: uncontrolled clinical trial]
Two studies25,26 have been conducted to evaluate the most effective dosage of oral dexamethasone in the treatment of croup. In one study,25 investigators compared doses of 0.15 mg per kg, 0.3 mg per kg, and 0.6 mg per kg and found no difference. In another study,26 researchers found that oral dexamethasone in a dose of 0.15 mg per kg was more effective than placebo in reducing the need for a return to medical care in children with mild croup.
These studies provide convincing evidence that oral dexamethasone is beneficial in the outpatient management of mild to moderate croup in the outpatient setting.
EPINEPHRINE
For decades, nebulized racemic epinephrine has been the standard treatment for patients with moderate to severe croup. Racemic epinephrine, a 1:1 mixture of the d- and l-isomers of epinephrine, is an alpha- and beta-adrenergic receptor stimulator. In patients with croup, racemic epinephrine reduces bronchial and tracheal secretions and mucosal edema.5 The routine dosage of racemic epinephrine is 0.05 to 0.1 mL per kg per dose mixed with normal saline and delivered with humidified oxygen.27 The l-isomer of epinephrine alone may be more available and is used by nebulization (5 mL of 1:1,000 solution).
Decreased inspiratory stridor and intercostal retractions are observed within 30 minutes of administering epinephrine, and the duration of action is about two hours.27 Common adverse effects include tachycardia and hypertension, so it should be used with caution in patients who have heart conditions or arrhythmias. Because the effect of epinephrine is brief, croup symptoms may reappear, demonstrating a rebound phenomenon.7 In the emergency department, children who have received nebulized epinephrine may be discharged if they have been observed for three to four hours and have no stridor at rest, normal air entry, good color, normal level of consciousness, and have received steroid therapy.7 Table 511 lists indications for hospitalization of patients with croup.
TABLE 5 Indications for Hospitalization of Patients with Croup
| Actual or suspected epiglottitis | Progressive stridor |
| Cyanosis | Respiratory distress |
| Depressed sensorium | Restlessness |
| Hypoxemia | Stridor at rest |
| Pallor | Toxic-appearing child |
Information from Orenstein DM. Acute inflammatory upper airway obstruction. In: Behrman RE, Kliegman RM, Jenson HB, eds. Nelson Textbook of pediatrics. 16th ed. Philadelphia: Saunders, 2000:1274–8.

