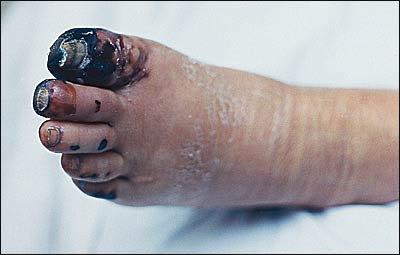
A 66-year-old man with alcoholism presented to the emergency department in January complaining of pain in his feet and an unsteady gait. The patient was sober, but did not remember the previous four days. Neighbors reported he was in an unheated home, smoking and drinking heavily. He denied trauma or previous problems with balance or dizziness. His medical history was significant for untreated hyperlipidemia and poorly controlled diabetes. Physical examination revealed normal vital signs. Muscle strength was intact in upper and lower extremities, but he had blunted pinprick and vibratory sensation below the ankles. He had a positive Romberg's sign. Distal to the ankles, the skin was cool and damp with cyanotic discoloration of the toes. There were a few vesicles and some sloughing of skin around the toes. His fingers, nose, and ears were without discoloration or lesions. Complete blood count and chemistry panel were normal. Within three weeks, his toes turned black and serous-filled bullae erupted (see accompanying figure).
Question
Based on the patient's history and physical examination, which one of the following is the correct diagnosis?
A. Frostbite.
B. Severe peripheral vascular disease.
C. Vitamin B12 deficiency.
D. Immersion foot.
E. Chilblains.
Discussion
The answer is D: immersion foot. This patient's pain, gait disturbance, and skin changes were secondary to the peripheral neuropathic changes and tissue injury that may occur with prolonged exposure to a damp cool environment.
Frostbite also can lead to neurologic and cutaneous damage, but this patient was indoors with no severe cold exposure. Damage caused by frostbite usually would not be isolated to the toes, but typically would affect other appendages as well, such as the nose, ears, and fingers.
Smoking and poorly controlled diabetes may lead to severe peripheral vascular disease, but this is typically an indolent, slowly progressive process and would not rapidly involve all 10 toes.
Vitamin B12 deficiency is seen more commonly in alcoholics and could account for the neuropathic changes seen with this patient, but not the necrotic skin change. A macrocytic anemia usually is seen with vitamin B12 deficiency, but was not present in this patient.
Chilblains are the mildest form of cold-induced injury. Repeated exposure to mildly cold temperatures can lead to the formation of shiny red plaques on the face, hands, or feet. Itching and pain are commonly seen in affected areas. Lesions can become swollen or boggy, but skin sloughing and gangrene do not occur.
This patient had immersion foot, also known as trench foot. Immersion foot, unlike frostbite, can occur without severe cold exposure. Prolonged exposure to damp, cool environments can lead to persistent, moderate vasospasm and tissue hypoxia. Even cold exposure as mild as 12.8°C (55°F) for 10 hours has been shown to cause immersion foot.1 This patient was in an unheated home in damp socks for days, which could easily cause trench foot. His ethanol use decreased his awareness and further predisposed him to exposure. Smoking also increased his risk for cold-induced skin injury. Nicotine is known to cause peripheral vasospasm and promote the development of peripheral vascular disease.
Patients who have immersion foot first complain of numbness without pain. After warming and drying, the injured area becomes painful and begins throbbing.1 This pain can persist for months before resolution. Patients with mild immersion foot sometimes suffer long-term neurovascular sequelae, such as Raynaud's phenomenon, cold intolerance, or paresthesias.2 In severe cases of trench foot, tissue injury is serious enough to cause skin sloughing and subsequent gangrenous change. After weeks or months, the necrotic boundary becomes demarcated. Surgical intervention typically is indicated at this stage.

