Atrial fibrillation increases the risk of stroke about fivefold, and mortality rates for stroke in these patients also are increased. Anticoagulation with warfarin has been shown repeatedly to reduce the incidence of stroke in patients with atrial fibrillation, but it carries the risk of intracranial hemorrhage. Recent guidelines have advocated lower intensity anticoagulation in some patients with atrial fibrillation. Hylek and colleagues investigated the relationship between anticoagulation intensity and stroke frequency, severity, and mortality.
The authors analyzed 13,559 patients with atrial fibrillation who had complete follow-up data available from a single integrated health care organization. Patients with recent hyperthyroidism, transient perioperative atrial fibrillation, and valvular disease were excluded. Medical records were reviewed retrospectively over three years for any diagnosis of stroke. The severity of stroke at the time of hospital discharge was scored by the modified Rankin scale, on which a score of 1 or 2 indicated a minor stroke, 3 or 4 indicated a major stroke that prevented independent living, and 5 indicated a severe stroke resulting in total dependence for all functional activities.
A total of 618 patients (4.6 percent) had strokes over the three-year study period. Incomplete data or hemorrhagic stroke excluded 22 patients from the severity and mortality analysis. When stroke occurred, 32 percent of the patients were taking warfarin, 27 percent were taking aspirin, and 42 percent were taking neither. The median International Normalized Ratio (INR) at the time of hospital admission was 1.7 in patients taking warfarin. The median INR over the six months before stroke was 2.2 in both groups and was nearly identical in the patients with an INR of less than 2.0 and in those with an INR of 2.0 or greater when stroke occurred.
FIGURE. Survival After Ischemic Stroke
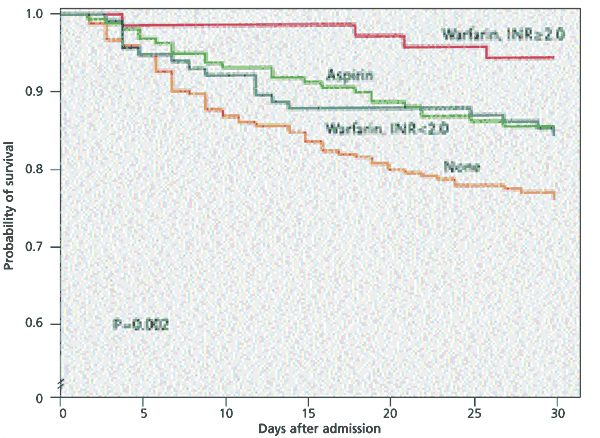
Kaplan-Meier estimates of survival in the 30 days after ischemic stroke among patients with atrial fibrillation, according to the antithrombotic medication status at admission. Patients who were taking warfarin are separated into two groups: those with an International Normalized Ratio (INR) of less than 2.0 and those with an INR of 2.0 or greater. The P value refers to the overall difference among the groups.
Reprinted with permission from Hylek EM, Go AS, Chang Y, Jensvold NG, Henault LE, Selby JV, et al. Effect of intensity of oral anticoagulation on stroke severity and mortality in atrial fibrillation. N Engl J Med 2003; 349:1024.
Stroke mortality was three times higher in patients with an admission INR of less than 2.0 (15 percent mortality) compared with patients with an INR of 2.0 or greater (5 percent mortality). The 30-day survival rate was similar in patients taking aspirin and in patients taking warfarin whose INR was less than 2.0 (see accompanying figure). The rate was better in both medication groups than in patients who were not taking antithrombotic medication. The severity of stroke also was significantly associated with the type of medication. Patients who were not taking medication and patients taking warfarin whose INR was less than 2.0 at admission had approximately double the risk of having a severe stroke.
The authors conclude that in patients with atrial fibrillation, those who are taking warfarin and whose INR is less than 2.0 at the time of stroke have twice the risk of severe stroke and three times the risk of mortality within 30 days as patients taking warfarin whose INR is 2.0 or greater.
editor's note: This is the third time in the past six months that the New England Journal of Medicine has published an article on lower intensity anticoagulation. One previous study1 suggested that lower intensity warfarin therapy (INR target, 1.5 to 1.9) was just as effective as standard anticoagulation (INR target, 2.0 to 3.0) in preventing recurrent venous thromboembolism, while causing less bleeding. A similar study2 published a few months later did not confirm these findings, describing higher rates of recurrent clotting with less warfarin and no improvement in bleeding rates compared with standard use. The current study of stroke in patients with atrial fibrillation provides another cautionary note to consider when contemplating aspirin or lower intensity warfarin for prophylaxis of thromboembolism.—b.z.

