Men who have sex with men often do not reveal their sexual practices or sexual orientation to their physician. Lack of disclosure from the patient, discomfort or inadequate training of the physician, perceived or real hostility from medical staff, and insufficient screening guidelines limit preventive care. Because of greater societal stresses, lack of emotional support, and practice of unsafe sex, men who have sex with men are at increased risk for sexually transmitted diseases (including human immunodeficiency virus infection), anal cancer, psychologic and behavioral disorders, drug abuse, and eating disorders. Recent trends indicate an increasing rate of sexual risk-taking among these men, particularly if they are young. Periodic screening should include a yearly health risk and physical assessment, as well as a thorough sexual and psychologic history. The physician should ask questions about sexual orientation in a nonjudgmental manner; furthermore, confidentiality should be addressed and maintained. Office practices and staff should be similarly non-judgmental, with confidentiality maintained. Targeted screening for sexually transmitted diseases, depression, substance abuse, and other disorders should be performed routinely. Screening guidelines, while inconsistent and subject to change, offer some useful suggestions for the care of men who have sex with men.
Men who have sex with men may identify themselves as homosexual, bisexual, or even heterosexual. No matter what label is used, the fact is that these men are at increased risk for sexually transmitted diseases (STDs) such as human immunodeficiency virus (HIV) infection, anal cancer, and psychologic and behavioral disorders.1
The rate of men who had sex with men in the previous year was thought to be 1.7 to 2 percent. However, surveys from 1996 to 2000 indicate that the rate is at least 3.1 to 3.7 percent.2 This discrepancy indicates that male-male sexual behavior often is underreported, and that previous estimates of the number of men who have sex with men may be too low. Therefore, a typical family physician can expect 3 percent or more of his or her male patients to be men who have had sex with men in the previous year.
Recent trends indicate a resurgence in risky behaviors that expose men who have sex with men to HIV infection and other STDs. The reported prevalence of men engaging in unprotected anal intercourse increased from 37 percent in 1993–1994 to 50 percent in 1996–1997.3 Disease risk frequently is not assessed, especially in younger men, in part because of numerous impediments to adequate care under the current health care system.4
Family physicians need an efficient system to identify and assess risk in men who have sex with men, so that appropriate screening and counseling interventions may occur. This article presents an organized risk-based preventive health assessment for men who have sex with men.
Compliance Issues
Although men who have sex with men can be at high risk for preventable diseases and disorders, they frequently do not receive appropriate preventive services. Numerous obstacles hinder compliance with screening guidelines5 (Table 1). For example, physicians may feel uncomfortable with the idea of sex between men or may not understand the issues that affect these patients. Patients, in turn, may be afraid to disclose their sexual orientation or practices. In addition, published, evidence-based screening guidelines for men who have sex with men are lacking or inconsistent, and reimbursement for screening services is limited. Younger men are thought to be at particularly high risk for HIV infection and other STDs because of low self-esteem, depression, and lack of peer support. Often, these men do not access the preventive services that are available to men who are more open about their homosexuality.4
TABLE 1 Obstacles to Achieving Compliance with Screening Guidelines and Limitations of Patient-Physician Communication
| Patient | Physician | Health care system |
|---|---|---|
| Embarrassment or fear about discussing the subject of sexual practices | Personal discomfort or perceived professional constraints; lack of training in how to discuss sexual risks and practices | — |
| Concern about the physician’s reaction to learning that the patient has sex with men | Possible open hostility toward the patient who reveals that he has sex with men | — |
| Belief that sexual practices (e.g., oral sex) are not risky | Lack of knowledge about the patient’s current sexual practices and related risks | — |
| Lack of awareness of the benefits of/need for screening services, and the benefits of discussing risks with the physician | Inability to provide complete screening because of constraints imposed by the patient’s insurance plan | Screening services not covered by most insurance plans |
| Belief that the health insurance company may learn about the patient’s sexual practices and cancel insurance coverage | — | Possible cancellation of the policy if the patient is determined to be “high risk” |
| Lack of interest in preventive health care services | Limited time; preventive health care services not routinely offered | Lack of evidence-based guidelines or conflicting guidelines for preventive health care services for men who have sex with men |
| Belief that the patient’s employer may learn of the patient’s sexual practices and terminate employment | — | Possible release of sensitive information by the insurance company to the patient’s employer |
TABLE 2 Approach to the Assessment of Sexual Risk
| Assess risk during every patient’s first visit, during all comprehensive health assessments, and when evidence suggests changing behavior. | |
| Qualify the discussion of sexual health by emphasizing that the discussion is routine with every patient. | |
| Underscore the importance of needing to know the patient’s sexual practices in order to determine appropriate screening and counseling interventions for optimal care. | |
| Remind the patient that the discussion is confidential. | |
| Negotiate with the patient about the information that will be included in the medical record; dispel the patient’s concerns about the accessibility of the information to insurers, employers, and others. | |
| Avoid terms such as “gay,” ”queer,” and “straight” when asking or talking about sexual practices or sexual identity. | |
| Avoid making assumptions about sexual behavior based on the patient’s age, marital status, disability, or other characteristics. | |
| Ask specific questions about sexual behavior in a direct, nonjudgmental manner: | |
| “Are you sexually active?” | |
| “Do you have sex with men, women, or both?” | |
| ”How many sexual partners do you have?” | |
| “How often do you use condoms?” | |
| “What kind of sexual acts do you engage in?” | |
| Assess the patient’s history of sexually transmitted infections. | |
Adapted with permission from Bradley-Springer L, ed. HIV: a sourcebook for the primary care provider. Denver: Mountain-Plains Regional AIDS Education and Training Center, 2000, and MSM: clinician’s guide to incorporating sexual risk assessment in routine visits. San Francisco: Gay and Lesbian Medical Association, 2002. Accessed online March 26, 2004, at:http://www.glma.org/medical/clinical/msm_assessment.shtml.
Communication between men who have sex with men and their family physician may be limited on several levels. Studies have shown that 20 percent or fewer of these patients had discussed their HIV risk with a physician in the previous five years.6 Many men, especially young men and those in minority groups, may be hesitant to disclose their sexual orientation in order “to avoid social isolation, discrimination, or verbal or physical abuse.”4(p81) Consequently, the physician often is unaware of a patient’s potential health risks. To provide appropriate long-term care, the physician should inquire sensitively about every patient’s sexual practices as part of the routine health risk assessment. Table 27,8 provides suggestions for approaching the sexual history and risk assessment.
Even when the family physician is aware of a patient’s potential health risks, the magnitude of the risks may be underestimated by the physician. There is evidence that many men are engaging in dangerous sexual practices that may jeopardize their health. These sexual practices include anal sex without a condom (“bare backing”), oral sex without a condom, oral stimulation of the anus (“rimming”) without protection, multiple sex partners at one time, and use of illicit drugs. Reasons for increased sexual risk-taking are listed in Table 3.3
When the physician learns that a patient may be taking serious sexual risks, commonly held misperceptions should be dispelled with accurate, scientifically validated data. For example, many men participate in oral sex, believing it to be “safer” than other sexual behaviors. However, oral sex can result in pharyngeal gonorrhea, chlamydial infection, and hepatitis A infection. In addition, there are persistent concerns that HIV might be spread by oral-genital contact.9
Prevalence of STDs and Other Conditions
Men who have sex with men are at significant risk of contracting HIV infection and acquired immunodeficiency syndrome (AIDS), as well as gonorrhea, syphilis, and herpes simplex virus type 2 (HSV-2) infection.
HIV and AIDS
Currently, 42 percent of new HIV infections are in men who have sex with men. In the United States, an estimated 365,000 to 535,000 of these men have HIV infection.3 Survey data indicate10 that HIV infection is present in nearly 10 percent of 22-year-old men who have sex with men.
Black and Hispanic men, in particular, are affected by the HIV epidemic. In 1999, they accounted for 53 percent of AIDS cases diagnosed in men who have sex with men.3 The incidence of AIDS is markedly higher in blacks and Hispanics than in men of other racial or ethnic backgrounds.
The presence of other STDs is an indicator of high-risk sexual practices that can facilitate the spread of HIV.
Gonorrhea
A diagnosis of gonococcal urethritis or rectal gonorrhea may indicate recent unsafe sexual practices. Gonococcal urethritis, which is usually symptomatic in men, is especially useful in risk determination because the infection has a short incubation period.11
The prevalence of gonorrhea is increasing in men who have sex with men. One study12 reported that the number of cases of gonorrhea among men who have sex with men increased from 4.5 percent of total gonorrhea cases in 1992 to 13.2 percent of total cases in 1999. Oral sex without condom use may be the reason for this increase.13 In addition, it is estimated that up to 50 percent of patients with gonococcal urethritis may have coexistent chlamydial infection.14
TABLE 3 Reasons for Increased Sexual Risk-Taking in Men Who Have Sex with Men
| AIDS burnout* |
| Outdated or overly simplistic safer-sex messages for men who have sex with men |
| Belief that HAART will be effective and easy to take |
| Media portrayals of HAART (i.e., successful at curing disease) |
| New HIV treatments and the potential for a vaccine |
| Lack of exposure to persons who are living with HIV infection or AIDS or who have died from AIDS |
| Belief that STDs “won’t happen to me” |
| Low self-esteem, depression, or lack of peer support |
| No access to preventive services that are available to men who are more open about their homosexuality |
AIDS = acquired immunodeficiency syndrome; HAART = highly active anti-retroviral therapy; HIV = human immunodeficiency virus; STDs = sexually transmitted diseases.
*—Tired of worrying about AIDS.
Information from reference3.
Syphilis
The number of cases of primary and secondary syphilis is increasing, especially in large cities. After a 10-year decline, syphilis cases more than doubled (from 117 to 282 cases) in New York City between 2000 and 2001.15 [Evidence level B, epidemiologic study] Overall, the increase in syphilis has occurred primarily in men who have sex with men. Many of the cases are in HIV-positive men, indicating a significant risk of HIV transmission.
HSV-2
It is estimated that HSV-2 has a positive seroprevalence rate of 22 percent in the U.S. adult population.15 Some studies indicate an infection rate of 26 to 40 percent in HIV-negative men who have sex with men.16 These men have frequent subclinical HSV-2 shedding, usually from the perianal area, and more frequent prodromal HSV-2 shedding.16 Recent reports indicate that HSV-2 may facilitate HIV transmission.17
Human Papillomavirus (HPV)
The prevalence of HPV infection ranges from 60 to 75 percent in men who have sex with men.18 Anal cancer is thought to arise from the progression of squamous intraepithelial lesions to invasive tumors associated with HPV infection.19 Anal cancer is uncommon; however, it is approximately 80 times more common in homosexual and bisexual men than in the general population. Anal cancer also is somewhat more common in men with HIV infection.
Hepatitis A Virus (HAV)
Studies indicate that men who have sex with men are at increased risk for HAV infection.20 Transmission is believed to be via oral-anal contact. Evidence of recent HAV infection is present is 3.3 percent of 17- to 22-year-old men who have sex with men.21 HAV virus antibodies are present in 28 percent in susceptible men who have sex with men.21 Hepatitis A vaccine is recommended, but most men are not immunized.
Hepatitis B Virus (HBV)
Despite current guidelines, the hepatitis B immunization rate is only about 9 percent in men who have sex with men.22 Most young men are not immunized. Markers of HBV infection are present in 11 percent of men who have sex with men22; in other studies, the prevalence of these markers ranges from 23 to 61.5 percent.23 The rate of HBV infection is 17 percent in 22-year-old men who have sex with men.22
Psychosocial Disorders
Homosexuality has been associated with higher rates of psychologic and behavioral disorders, including depression, anxiety, mood disorders, suicidal thoughts and plans, eating disorders, alcohol and substance abuse, and cigarette smoking.24 The stigmatization of homosexuality in American society, including frequent exposure of homosexual men to discrimination and victimization, is believed to be a causative factor in the development of psychologic and behavioral disorders. A number of studies have found elevated rates of suicidal thoughts and attempts,1 higher rates of eating disorders,25 and extremely high rates of tobacco use in homosexual men. In one U.S. study,26 the smoking rate in homosexual men was 47.8 percent; the smoking rate in all men in the United States has been found to be 28.6 percent.
Clinical Approach
The family physician should consider performing sexual, behavioral, and psychologic risk assessments at each patient’s first office visit and should repeat the assessment whenever there is evidence of changing behavior.3,27 [Reference 27—Evidence level C, consensus/expert guidelines] To gain accurate information, the physician should use a nonjudgmental approach that removes communication barriers (Table 1) and encourages the patient to be open and honest (Table 2).7,8 The physician should use gender-neutral language when inquiring about sexual partners or significant others.
The family physician must ensure that the office staff and the office environment also are nonjudgmental. Office forms should include terms such as “partner” in addition to “spouse,” “husband,” and “wife.”
The topics listed in Table 428 can serve as a guide in counseling men who have sex with men and in determining appropriate follow-up interventions.
TABLE 4 Topics to Discuss with Men Who Have Sex with Men
| Safer sexual practices (e.g., abstinence, condom use) |
| History of/risk for HIV, AIDS, and STDs and screening for these diseases |
| History of/risk for prostate, testicular, and colon cancer, and screening for these malignancies |
| History of hepatitis A or B, or need for immunization |
| History of/risk for anal papilloma and need for screening |
| Nutrition and exercise |
| Smoking cessation, if applicable |
| Previous or current depression or anxiety |
| Alcohol use or abuse |
| Substance use (i.e., illicit drugs) |
HIV = human immunodeficiency virus; AIDS = acquired immunodeficiency syndrome; STDs = sexually transmitted diseases.
Adapted with permission from Ten things gay men should discuss with their health care providers. San Francisco: Gay and Lesbian Medical Association, 2002. Accessed online March 10, 2004, at:http://www.glma.org/news/releases/n02071710gaythings.shtml.
Screening and Diagnosis
Screening and counseling interventions are listed in Table 5.5,14,27,29,30 The Centers for Disease Control and Prevention (CDC)27 suggests that physicians assess sexual risk in all male patients, with the assessment routinely including a question about the gender of sexual partners.27 [Evidence level C, consensus/expert guidelines]
Men who have sex with men should undergo routine, straightforward, nonjudgmental risk assessments for HIV infection and other STDs, along with patient-centered counseling on preventive measures to reduce the acquisition or transmission of these infections. Screening should be performed at least annually in sexually active men who have sex with men.
The CDC27 recommends more frequent STD screening (e.g., at three- to six-month intervals) in men at highest risk, including those who have multiple anonymous sexual partners, those who have sex in conjunction with illicit drug use, and those whose sexual partners participate in these activities. Screening tests usually are indicated even when patients have been using condoms consistently for insertive or receptive anal intercourse. Physicians should know the common manifestations of STDs in men who have sex with men; if symptoms are present, appropriate diagnostic tests should be performed.27
Vaccination against hepatitis A and B is recommended for all men who have sex with men. Prevaccination serologic testing may be cost-effective when the prevalence of hepatitis A and B is likely to be high.27
The U.S. Preventive Services Task Force30 does not give specific recommendations for screening of men who have sex with men. However, the infectious disease recommendations specifically address screening issues in men who are at high risk for STDs.
The California STD Controllers Association and the Public Health–Seattle and King County Agency have developed guidelines that are derived, in part, from systematic surveys of STD prevalence and sexual behaviors and practices among men who have sex with men.5 These guidelines are not universally accepted, but screening and treatment of curable STDs can be cost-effective by decreasing the period during which infected persons can transmit diseases to others.31 The guidelines provide another reasonable clinical approach to surveillance in men who have sex with men.5 [Evidence level C, consensus/expert guidelines] These guidelines are useful in the communities studied and are likely to be helpful in other large population centers. However, family physicians should use the guidelines in combination with regionally derived data to assist in the use of guidelines for their own geographic area or population. In addition, they should stay abreast of changes in sexual practices that may affect guidelines.
Screening guidelines have been suggested for anal intraepithelial neoplasia, although epidemiologic data suggest that most of these lesions do not progress to invasive anal cancer.19 Annual screening of HIV-positive men has been shown to be cost-effective, because these men have a much higher incidence of anal cancer; screening every two to three years could be cost-effective in HIV-negative homosexual men with a history of condyloma.32 [Evidence level C, consensus/expert guidelines] Clinical studies are inconclusive about the screening of HIV-negative men for anal cancer. An algorithm for use in screening men who have sex with men is provided in Figure 1.
TABLE 5 Recommended Surveillance and Intervention Strategies in Healthy Men Who Have Sex with Men*
| Disease | Intervention | AAFP29 | CDC27 | USPSTF14,30 | Public Health–Seattle and King County5 | California STD Controllers Association5 |
|---|---|---|---|---|---|---|
| STDs (low-risk patients) | Screening, counseling | Counsel patients about risks and preventive strategies. | Routinely inquire about gender of patient’s sexual partners; screen at least annually. | No recommendation provided | Screen all sexually active men who have sex with men. | Screen patients at initial visit. |
| STDs (high-risk patients) | Screening, counseling | Counsel patients about risks and preventive strategies. | At 3- to 6-month intervals, screen men who have multiple anonymous sexual partners, have sex in conjunction with illicit drug use, or have sexual partners who participate in these activities. | No recommendation provided Defines high-risk patients as men who have multiple sexual partners | Every 3 to 6 months, screen men with specific risk behaviors (multiple or anonymous sexual partners, substance abuse). | Every 3 to 6 months, screen patients who have an STD. |
| HIV | HIV serologic testing | Yes | Yes, if patient is HIV negative or not previously tested | Periodic screening in high-risk patients | Yes | Yes |
| Gonorrhea | Pharyngeal culture | No recommendation provided | Yes, in men with oralgenital exposure | No recommendation provided | Yes | Yes |
| Rectal culture | No recommendation provided | Yes, in men who have receptive anal intercourse; include Chlamydia culture | No recommendation provided | Yes, in men who have receptive anal intercourse | Yes, in men who have receptive anal intercourse | |
| Urethral culture | No recommendation provided | Yes, urethral or urine test (culture or nucleic acid amplification) | No; consider screening high-risk young men on other grounds. | No | Yes | |
| Syphilis | Serologic testing | Yes | Yes | No | Yes | Yes |
| Chlamydia | Rectal screening | There is insufficient evidence to recommend for or against routine screening of asymptomatic men for chlamydial infection. | Yes, in men who have receptive anal intercourse | No recommendation provided | Yes, in men who have receptive anal intercourse | No |
| Herpes simplex virus type 2 | Serologic test | Not recommended for asymptomatic patients | No | Not recommended for asymptomatic patients | Consider | Consider |
| Hepatitis A and B | Immunization | Yes † | Yes; serologic prevaccination testing may be cost-effective in men who have sex with men when there is a high prevalence of hepatitis A and B in the community. | Screen high-risk patients to assess eligibility for vaccination; immunize all high- risk patients and young adults notpreviously immunized. | Yes | Yes |
AAFP = American Academy of Family Physicians; CDC = Centers for Disease Control and Prevention; USPSTF = U.S. Preventive Services Task Force; STDs = sexually transmitted diseases; HIV = human immunodeficiency virus.
*—HIV negative or unknown HIV status.
†—See Recommended adult immunization schedule, United States, 2003, at:https://www.aafp.org/x14956.xml.
FIGURE 1. Screening in Men Who Have Sex with Men
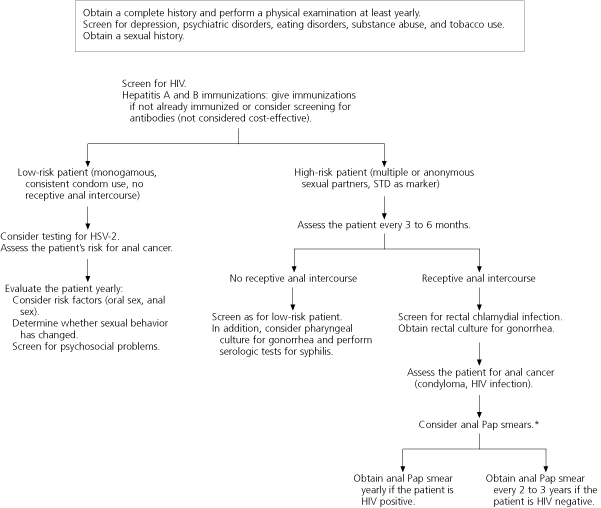
Suggested approach to screening in men who have sex with men. (HIV = human immunodeficiency virus; STD = sexually transmitted disease; HSV-2 = herpes simplex virus type 2; Pap = Papanicolaou)
Further studies are needed to determine effective, practical screening practices for family physicians to use in assessing men who have sex with men. In addition, specific data should be collected on the prevalence of anal neoplasia in men with a history of receptive anal sex, with special emphasis on HIV-infected men with HPV infection.31

