Almost one decade after the Institute of Medicine (IOM) defined primary care, only one third of the American public is able to identify any of the medical specialties that provide it, and only 17 percent were able to accurately distinguish primary care physicians from medical or surgical specialists and non-physicians. This lack of discrimination compromises the goal of achieving primary care for all and merits immediate attention.
When the IOM was charged to “provide guidance for augmenting and improving primary care as an essential component of an effective and efficient health care system,” it discovered primary care was so poorly understood in the United States that the charge could not be undertaken without updating the definition of primary care. This definition, published in 1996, defines primary care as the provision of integrated, accessible health care services by clinicians who are accountable for addressing a large majority of personal health care needs, developing a sustained partnership with patients, and practicing in the context of family and community. The IOM recognized those physicians trained in family medicine, general internal medicine, and general pediatrics, as well as many nurse practitioners and physician assistants, as key providers of primary care.
The Future of Family Medicine (FFM) project, a collaborative effort by national family medicine organizations, commissioned Roper ASW to survey 1,031 people between June 14 and July 1, 2002. The sample represents the general population of the United States with regard to race, ethnicity, gender, age, and location. Respondents were asked to identify “all the different kinds of primary care physicians (PCPs) you can think of.” Patients were permitted several responses (Figure 1). One half responded they “didn’t know.”Only 17 percent of the respondents were able to accurately identify at least one type of primary care physician without also misidentifying non-primary care specialists or non-physicians as primary care physicians (Figure 2).
FIGURE 1.
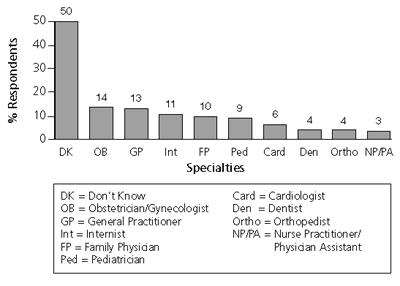
Specialties Identified as Primary Care Physicians
There is ample evidence that having a personal primary care physician is associated with improved health outcomes and that this is a relationship desired by people.1 The public deserves to be better informed about primary care and on whom they can rely to receive this care.
FIGURE 2.
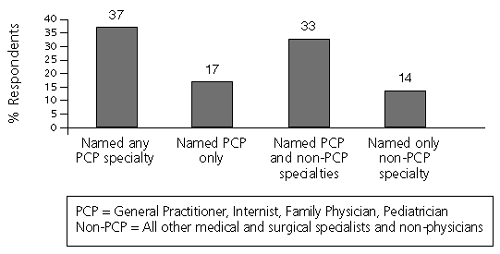
Aggregate Identification of Provider Types

