A 71-year-old woman presented to the dermatology clinic with a 15-year history of a recurrent erythematous rash on her left knee and lower leg (see accompanying figure).
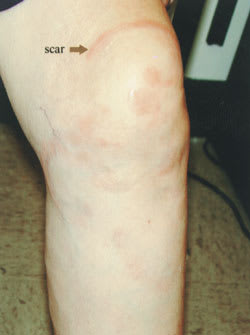
On physical examination, a 5-cm erythematous ring was noted on her left central knee and a serpiginous, papular, erythematous lesion was noted on the medial aspect of the knee. The patient had been treated with ivermectin four years earlier, and reported that the lesions resolved at that time. The lesions reappeared approximately one year later, this time with mild pruritus and slight hypersensitivity to touch.
Question
Based on the patient’s history and physical appearance of the rash, which one of the following is the correct diagnosis?
A. Hansen’s disease.
B. Granuloma annulare.
C. Sarcoidosis.
D. Cutanea larvae migrans.
E. Tinea corporis.
Discussion
The answer is B: granuloma annulare. A skin biopsy showed interstitial lymphocytic and histiocytic infiltrates with collagenolysis, consistent with granuloma annulare. The patient was treated with clobetasol steroid cream and instructed to follow up in four weeks.
Granuloma annulare is a benign, self-limited cutaneous condition. It is characterized by annular, flesh-colored or slightly erythematous plaques and papules that are generally asymptomatic.1,2 Some patients may report mild pruritus, as noted in this case.3,4 There are several forms of granuloma annulare, including localized, generalized, perforating, subcutaneous, and actinic.3 The localized form accounts for approximately 75 percent of all cases.3
The lesions of granuloma annulare can occur anywhere on the body, but most often involve the dorsal surfaces of the hands, feet, elbows, or knees.2 The condition usually begins with an asymptomatic, flesh-colored papule that undergoes central involution and slowly develops into a ring-shaped lesion.1 Over several months, the lesion gradually may increase in diameter, with a final size of 0.5 to 5 cm.1 The duration of the disease is highly variable. Approximately one half of patients experience spontaneous resolution without scarring, whereas, in other patients, lesions may last for years.1,3 Among those who experience resolution of lesions, the disease commonly recurs.2,3
The diagnosis of granuloma annulare often may be made by its characteristic clinical presentation. In uncertain cases where biopsy is necessary, the histology shows collagen degeneration caused by an inflammatory reaction that occurs around the blood vessels.1,2 Although the etiology of granuloma annulare is unknown, theories include vasculitis, trauma, monocyte activation, and type IV delayed hypersensitivity.3
Because lesions are usually asymptomatic, they are best left untreated. If cosmetic appearance is a concern, these lesions may be treated with intralesional corticosteroid injections, topical corticosteroids, electrodesiccation, cryotherapy, ultraviolet light therapy, or even systemic agents (e.g., dapsone, colchicine, chloroquine) for patients who have widespread lesions.1–3 None of these methods are curative.
Hansen’s disease (leprosy) is a chronic granulomatous disease that affects the skin and nerves.2 These lesions are typically well-defined, hypopigmented papules and may have slight scale.2,3 Additional clinical features that help distinguish this diagnosis are perilesional cutaneous anesthesia and exposure to an endemic area (especially Brazil, India, southern Africa, Myanmar, and Nepal).2,3 Diagnosis is made by demonstrating leprosy bacilli in the skin.2
Sarcoidosis can present with a number of different skin findings, including brownish-red plaques that wax and wane.2 The face is most commonly involved, but plaques also may occur on the trunk or the dorsal surfaces of the arms or legs.3 Diagnosis often is obvious from the usual clinical presentation (cough, dyspnea) and radiologic findings (hilar lymphadenopathy), but biopsy of cutaneous lesions may provide confirmatory information in unclear cases.2,3
Cutaneous larvae migrans is characterized by a thin, erythematous, serpiginous papular eruption caused by hookworm larvae traveling through the skin.1,2 Infection is acquired by skin contact with soil contaminated by dog or cat feces.1 It occurs most commonly in travelers returning from tropical locations.1 During larval migration, a local inflammatory response is provoked, which causes moderate to intense pruritus.1,2 If untreated, the larvae usually die within two to eight weeks, but may persist for up to one year.1,2
Tinea corporis classically begins as a flat, scaly spot that later develops a raised advancing border.1,2 The border may develop red, raised papules or vesicles, while the central area becomes hypopigmented and less scaly.1 A potassium hydroxide examination of skin scrapings may reveal hyphae, but this is often difficult to demonstrate because of the low fungal load.2 Resolution of lesions after empiric antifungal treatment is the most common means by which tineal infection is verified.
Selected Differential Diagnosis of Raised Leg Rash
| Condition | Characteristics |
|---|---|
| Hansen’s disease | Well-defined, hypopigmented papules with or without scale, hypesthesia, bacilli, travel history |
| Granuloma annulare | Circular, flesh-colored or erythematous plaques and papules, usually asymptomatic |
| Sarcoidosis | Brown-red plaques that wax and wane, clinical symptoms present |
| Cutanea larvae migrans | Thin, erythematous, serpiginous papules, pruritic, travel history |
| Tinea corporis | Flat, scaly, circular lesions with or without raised erythematous border |

