The constellation of dyslipidemia (hypertriglyceridemia and low levels of high-density lipoprotein cholesterol), elevated blood pressure, impaired glucose tolerance, and central obesity is identified now as metabolic syndrome, also called syndrome X. Soon, metabolic syndrome will overtake cigarette smoking as the number one risk factor for heart disease among the U.S. population. The National Cholesterol Education Program–Adult Treatment Panel III has identified metabolic syndrome as an indication for vigorous lifestyle intervention. Effective interventions include diet, exercise, and judicious use of pharmacologic agents to address specific risk factors. Weight loss significantly improves all aspects of metabolic syndrome. Increasing physical activity and decreasing caloric intake by reducing portion sizes will improve metabolic syndrome abnormalities, even in the absence of weight loss. Specific dietary changes that are appropriate for addressing different aspects of the syndrome include reducing saturated fat intake to lower insulin resistance, reducing sodium intake to lower blood pressure, and reducing high-glycemic–index carbohydrate intake to lower triglyceride levels. A diet that includes more fruits, vegetables, whole grains, monounsaturated fats, and low-fat dairy products will benefit most patients with metabolic syndrome. Family physicians can be more effective in helping patients to change their lifestyle behaviors by assessing each patient for the presence of specific risk factors, clearly communicating these risk factors to patients, identifying appropriate interventions to address specific risks, and assisting patients in identifying barriers to behavior change.
Metabolic syndrome, also called insulin resistance syndrome or syndrome X, is a cluster of risk factors that is responsible for much of the excess cardiovascular disease morbidity among overweight and obese patients and those persons with type 2 diabetes mellitus.1 Differences in body-fat distribution (i.e., gynecoid versus android) associated with an altered metabolic profile were documented in the medical literature 50 years ago. Given the name syndrome X in 1988,2 each component of the syndrome has been associated with an increased risk of cardiovascular disease.3 A report4 from the National Cholesterol Education Program–Adult Treatment Panel (NCEP–ATP III) identified metabolic syndrome as an independent risk factor for cardiovascular disease and considered it an indication for intensive lifestyle modification.
Definition
The major characteristics of metabolic syndrome include insulin resistance, abdominal obesity, elevated blood pressure, and lipid abnormalities (i.e., elevated levels of triglycerides and low levels of high-density lipoprotein [HDL] cholesterol). Initially defined by an expert panel of the World Health Organization in 1998,5 the NCEP–ATP III4 has created an operational definition of metabolic syndrome: the co-occurrence of any three of the abnormalities mentioned above (Table 14,5).
Metabolic syndrome is associated with a proinflammatory/prothrombotic state that may include elevated levels of C-reactive protein, endothelial dysfunction, hyperfibrinogenemia, increased platelet aggregation, increased levels of plasminogen activator inhibitor 1, elevated uric acid levels, microalbuminuria, and a shift toward small, dense particles of low-density lipoprotein (LDL) cholesterol. Insulin resistance also has been implicated in polycystic ovary syndrome and nonalcoholic steatohepatitis (NASH).
Epidemiology/Prevalence
The prevalence of metabolic syndrome varies by definition used and population studied.6 Based on data from the Third National Health and Nutrition Examination Survey (1988 to 1994), the prevalence of metabolic syndrome (using the NCEP–ATP III criteria) varies from 16 percent of black men to 37 percent of Hispanic women (Figure 1).7 The prevalence of metabolic syndrome increases with age and increasing body weight. Because the U.S. population is aging, and because more than one half of adults are overweight or obese, it has been estimated that metabolic syndrome soon will overtake cigarette smoking as the primary risk factor for cardiovascular disease.8 Metabolic syndrome is an even stronger predictor of risk for type 2 diabetes mellitus.9
FIGURE 1. Prevalence of the Metabolic Syndrome
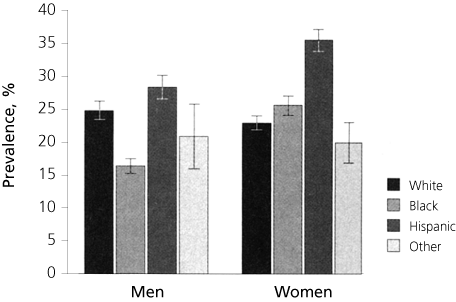
Age-adjusted prevalence of the metabolic syndrome among 8,814 U.S. adults at least 20 years of age, by sex and race or ethnicity, from the National Health and Nutrition Examination Survey III, 1988–1994.
Adapted with permission from Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among U.S. adults: findings from the Third National Health and Nutrition Examination Survey. JAMA 2002;287:358.
Etiology
The etiology of the metabolic syndrome has not been established definitively. One hypothesis presumes that the primary cause is insulin resistance. Insulin resistance correlates with visceral fat measured by waist circumference or waist to hip ratio. The link between insulin resistance and cardiovascular disease probably is mediated by oxidative stress, which produces endothelial cell dysfunction, promoting vascular damage and atheroma formation.10
The second hypothesis blames hormonal changes for the development of abdominal obesity. One study11 demonstrated that persons with elevated levels of serum cortisol (caused by chronic stress) developed abdominal obesity, insulin resistance, and lipid abnormalities. The investigators concluded that this inappropriate activation of the hypothalamic-pituitary-adrenal axis by stress is responsible for the link between psychosocial and economic problems, and acute myocardial infarction.
Clinical Evaluation
The routine medical and family history helps to identify patients at risk for cardiovascular disease or diabetes mellitus. Questions about recent or past weight changes, and a brief diet and physical activity history,12 including occupational and leisure-time physical activity, are important. The patient should be asked to estimate how many hours a day he or she is sedentary. Questions about typical food intake and efforts to reduce dietary fat or other specific dietary changes allow the physician to estimate the patient’s readiness to change lifestyle habits.
The patient’s height, weight, and blood pressure should be measured. Body mass index (BMI) should be determined by calculating weight (kg)/height (m2), and waist circumference should be measured at the narrowest point between the umbilicus and the rib cage. Waist circumference appears to be a better predictor of cardiovascular risk than waist-to-hip ratio.13 Patients suspected of having metabolic syndrome should have a fasting glucose level and a fasting lipid profile level obtained. A euglycemic clamp or homeostasis model assessment is used in research studies to accurately assess insulin resistance, but is impractical for use in the clinical setting.14
Fasting insulin levels and glucose challenge tests are indicators of insulin resistance but do not need to be measured in most situations because a fasting glucose level alone suffices for the definition of metabolic syndrome. If LDL cholesterol is normal, measuring levels of apolipoprotein B is not necessary. New tests that measure LDL particle size are expensive and unnecessary, because low HDL cholesterol levels and high triglyceride levels predict small, dense LDL particles.
The American Heart Association recommends measurement of highly sensitive C-reactive protein for risk stratification in patients at high risk of cardiovascular disease.15 Baseline uric acid levels and routine liver function tests will screen for NASH, but abdominal ultrasonography is required to diagnose fatty liver because it may be present even in the absence of elevated liver function test results.
Treatment Strategies
Currently, no randomized controlled trials specifically examining the treatment of metabolic syndrome have been published. Based on clinical trials, aggressive management of the individual components of the syndrome should make it possible to prevent or delay the onset of diabetes mellitus, hypertension, and cardiovascular disease.4,16,17 All patients diagnosed with metabolic syndrome should be encouraged to change their diet and exercise habits as primary therapy. Weight loss improves all aspects of the metabolic syndrome, as well as reducing all-cause and cardiovascular mortality18 (Table 2). While many patients find weight loss difficult to achieve, exercise and dietary changes that can lower blood pressure and improve lipid levels will improve insulin resistance, even in the absence of weight loss.19
EXERCISE
Skeletal muscle is the most insulin-sensitive tissue in the body and, therefore, a primary target for impacting insulin resistance. Physical training has been shown to reduce skeletal muscle lipid levels and insulin resistance, regardless of BMI.20 The impact of exercise on insulin sensitivity is evident for 24 to 48 hours and disappears within three to five days. Thus, regular physical activity should be a part of any effort to reverse the effects of insulin resistance.
EXERCISE PRESCRIPTION
Patients should be encouraged to focus on improving their personal level of physical activity. The greatest health benefits occur when sedentary persons incorporate moderate-intensity exercise into their lifestyle. Low-intensity exercise can have a significant impact on health and studies show that as the recommended frequency of exercise increases, actual participation declines.21
The goal for family physicians is to help patients find a level of activity that they can accomplish over the long term.22 A combination of resistance and aerobic exercise is best, but any activity is better than none, and patients who have been sedentary need to start with walking and gradually increase duration and intensity.23 Use of low-weight dumbbells, elastic exercise bands, or even heavy food containers can provide the needed weight for resistance training. Walking or light jogging for one hour per day will produce significant losses of abdominal (visceral) fat in men without caloric restriction.24
Diet
No single diet is currently recommended for patients with metabolic syndrome; therefore, it may be best for physicians to focus on each patient’s specific metabolic alterations when offering dietary advice25 (Table 2). Sustained dietary changes may require referral to a registered dietitian to help implement suggestions and ensure adequate micronutrient intake (e.g., calcium, iron, folate) while reducing calories. There is debate about what proportions of macronutrients (i.e., protein, fat, and carbohydrates) will produce the best outcome (low-fat, low-carbohydrate, or Mediterranean diets). If a patient is consuming fewer calories than he or she is expending, the macronutrient composition of the diet is probably of secondary importance, because weight loss improves metabolic syndrome.
The primary goals of dietary change for metabolic syndrome are to reduce the risk of cardiovascular disease and diabetes mellitus. Two recent Cochrane Database systematic reviews support the role of dietary interventions in helping to reduce cardiovascular risk. Evidence26 from one large and one small trial showed that a low-sodium diet helps to maintain lower blood pressure following withdrawal of antihypertensive medications. Results27 from clinical trials of low-fat diets in which participants were involved for more than two years showed significant reductions in the rate of cardiovascular events and suggested protection from total mortality. The degree of protection from cardiovascular events was statistically significant in patients with a higher risk of cardiovascular disease.
For patients with elevated blood pressure, the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7)16 states that a systolic blood pressure of 120 to 139 mm Hg or a diastolic pressure of 80 to 89 mm Hg should be considered prehypertensive and trigger lifestyle modifications to prevent cardiovascular disease.
According to the Dietary Approaches to Stop Hypertension (DASH) study,28 patients who consumed a diet low in saturated fat and high in carbohydrates experienced a significant reduction in blood pressure, even without weight reduction. The DASH diet emphasizes fruits, vegetables, low-fat dairy foods, whole grains, poultry, fish, and nuts, while reducing saturated fats, red meat, sweets, and sugar-containing beverages. Reducing sodium intake can further reduce blood pressure or prevent the increase in blood pressure that may accompany aging.
The Coronary Artery Risk Development in Young Adults study29 demonstrated that consumption of dairy products was associated with a significantly reduced risk of metabolic syndrome.
Low-fat, high-carbohydrate diets have been criticized because they may raise triglyceride levels and lower HDL-cholesterol levels in some patients, thus aggravating the dyslipidemia of metabolic syndrome. To treat hypertriglyceridemia, or if HDL-cholesterol levels decline on a low-fat diet, carbohydrate intake can be reduced and replaced with foods high in monounsaturated fats30 or low-glycemic–index carbohydrates. These changes create a diet similar to the Mediterranean-style diet, which also has been shown to reduce mortality from cardiovascular disease.31
For sedentary patients with hypertriglyceridemia and insulin resistance (particularly those who are obese or who have an abnormal waist circumference; Table 14,5), a lower carbohydrate diet that limits sodas, juice drinks, and refined grains (such as sweetened cereals, baked goods, and desserts) may be beneficial (seehttp://www.ttuhsc.edu/SOM/FamMed/wholefoods.html).
TABLE 2 Practical Advice for Lifestyle Interventions in Patients with Metabolic Syndrome
| Abnormality | Diet and physical activity interventions | Practical advice |
|---|---|---|
| Abdominal obesity | Reduce weight. | Reduce portion sizes to lower calorie intake. |
| Increase physical activity. | 30 minutes of moderate-intensity exercise daily | |
| Hypertriglyceridemia | Reduce weight. | Reduce portion sizes to lower calorie intake. |
| Increase physical activity. | 30 minutes of moderate-intensity exercise daily | |
| Increase intake of low-glycemic–index foods. | Replace refined carbohydrates (white bread, potatoes, pasta) with legumes, whole grains, and monounsaturated fats (nuts, avocado, canola oil, olive oil). | |
| Reduce total carbohydrate intake. | Replace soda and juices with water, seltzer, and diet beverages. | |
| Increase omega-3 fatty acids. | Eat fish at least once per week. | |
| Limit alcohol consumption. | Limit alcohol to no more than two drinks per day for men, or one drink per day for women. | |
| Low HDL cholesterol level | Reduce weight. | Reduce portion sizes to lower calorie intake. |
| Increase physical activity. | 30 minutes of moderate-intensity exercise daily | |
| Increase consumption of monounsaturated fats. | Eat fish, nuts, and avocados. Use olive or canola oils in salad dressing and for cooking. | |
| Stop smoking. | Join a smoking cessation program. | |
| High blood pressure | Reduce weight. | Reduce portion sizes to lower calorie intake. |
| Increase physical activity. | 30 minutes of moderate-intensity exercise daily | |
| Reduce saturated fat intake. | Choose low-fat dairy products and reduce consumption of red meat, butter, and full-fat dairy products. | |
| Reduce sodium intake. | Reduce sodium intake to no more than 2.4 g per day or 6 g per day of salt by using more herbs in cooking; read labels for sodium content; skip the salt shaker. | |
| Increase consumption of fruits and vegetables. | Consume more than five servings of fruits and vegetables every day. | |
| Increase low-fat dairy products. | Consume three servings of low-fat dairy products daily. | |
| Limit alcohol consumption | Limit alcohol to no more than two drinks per day for men and one drink per day for women. | |
| High fasting glucose level | Reduce weight. | Reduce portion sizes to lower calorie intake. |
| Increase physical activity. | 30 minutes of moderate-intensity exercise daily | |
| Reduce total carbohydrate intake; replace carbohydrates with monounsaturated fat. | Replace refined grains with whole grains (oatmeal, brown rice, corn, and whole wheat) and monounsaturated fats (nuts, avocados, canola oil, olive oil). | |
| Increase dietary fiber (more than 30 g per day). | Add legumes and fruit for soluble fiber. |
HDL = high-density lipoprotein.
Supplied with permission by Darwin Deen, M.D., M.S., Albert Einstein College of Medicine, and Lisa Hark, Ph.D., R.D., University of Pennsylvania School of Medicine.
One study32 demonstrated a correlation between cardiovascular disease and the intake of refined grain products and potatoes. The investigators recommend a diet high in minimally processed plant-based foods, such as whole grains, fruits, and vegetables. Results of a recent pooled analysis of cohort studies33 concluded that increasing dietary fiber from fruits, vegetables, and grains lowers the risk of developing cardiovascular disease.
The long-term effects of low-carbohydrate diets have not been studied adequately, but in the short-term, these diets have been shown to lower triglyceride levels, raise HDL-cholesterol levels, and reduce body weight.34 An alternative to lowering consumption of all carbohydrates is to replace high-glycemic–index foods with less refined lower-glycemic–index foods that contain more fiber.33 Low-glycemic–index foods produce lower levels of post-prandial glucose and insulin. Current fiber intakes are below recommended levels and limiting grains will make this worse.
While alcohol consumption has been associated with elevations of serum triglyceride levels, moderate alcohol intake, defined as one drink per day for women and two drinks per day for men, need not be discouraged unless fatty liver is present,35 because this level of alcohol intake reduces insulin resistance and cardiovascular disease.36
TABLE 3 ATP III Guidelines for the Treatment of Patients with Metabolic Syndrome
| Targeted area | Goal | |
|---|---|---|
| Treat LDL cholesterol first. | ||
| CHD and CHD risk equivalent (10-year risk for CHD >20 percent) | <100 mg per dL (< 2.60 mmol per L) | |
| At least two risk factors and 10-year risk 20 percent | <130 mg per dL (< 3.35 mmol per L) | |
| Institute weight control. | –10 percent from baseline | |
| Institute physical activity. | 30 to 40 minutes per day, three to five days per week | |
| Monitor treatment of hypertension. | <130/85 mm Hg | |
| Treat elevated triglyceride levels and low HDL cholesterol levels. | ||
| Goal of non-HDL cholesterol for patients with triglyceride levels of ≥200 mg per dL (≥5.20 mmol per L) and ≤499 mg per dL (≤12.90 mmol per L) | High CHD risk: <130 mg per dL | |
| Intermediate CHD risk: <160 mg per dL (4.15 mmol per L) | ||
| Low CHD risk: <190 mg per dL (4.90 mmol per L) | ||
ATP = Adult Treatment Panel; LDL = low-density lipoprotein; CHD = coronary heart disease; HDL = high-density lipoprotein.
Adapted with permission from Vega GL. Obesity, the metabolic syndrome, and cardiovascular disease. Am Heart J 2001;142:1108–16.
USING EDUCATIONAL STRATEGIES
Family physicians recognize that there are significant barriers to lifestyle counseling,37 but patient-centered methodologies accompanied by supportive office systems can make the primary care physician more effective.38,39 Physicians should assess patients’ knowledge about the relationship of their lifestyle to their health, then provide a clear message about the importance of diet and exercise for their specific problem.
Next, physicians should try to help patients identify short- and long-term goals and barriers to change. Questions such as: “How do you think that your diet (or exercise level) affects your health?” or “What problems did you encounter in trying to change your diet (or level of activity)?” can help the physician identify effective next steps for each patient. The answers to these questions should be recorded in the medical record and reviewed at subsequent visits to help patients identify and address barriers to lifestyle changes. ICD-9 codes (97802 and 97803) are available for physician reimbursement for these counseling efforts.
PHARMACOTHERAPY
For patients whose risk factors are not reduced adequately by lifestyle changes (Table 31), pharmacologic interventions to control their blood pressure and lipid levels are indicated.40 Use of aspirin and statins lowers C-reactive protein levels, but so does weight loss. Aggressive pharmacologic management of risk factors has been shown to be more effective than routine care in preventing cardiovascular disease in patients with type 2 diabetes mellitus.41
Prevention
The U.S. Preventive Services Task Force recommends intensive behavioral dietary counseling for adult patients with known risk factors for cardiovascular disease.42 The evidence for counseling for physical activity is not yet strong enough to merit a recommendation.43 Family physicians need to be more effective at helping patients adopt healthy lifestyle habits. The Diabetes Prevention Program19 demonstrated that vigorous lifestyle intervention in patients who are prediabetic could reduce the rate of developing diabetes by more than 50 percent (from 11 to 4.8 percent).
Strength of Recommendations
| Key clinical recommendation | Strength of recommendation | References |
|---|---|---|
| The American Heart Association recommends measurement of highly sensitive C-reactive protein for risk stratification in patients at high risk of cardiovascular disease. | C | 15 |
| Evidence from a large and small trial showed that a low-sodium diet helps to maintain lower blood pressure following withdrawal of antihypertensive medications. | A | 26 |
| Results from clinical trials of low-fat diets in which participants were involved for more than two years showed significant reductions in the rate of cardiovascular events and suggested protection from total mortality. | A | 27 |
| The U.S. Preventive Services Task Force recommends intensive behavioral dietary counseling for adult patients with known risk factors for cardiovascular disease. | B | 42 |

