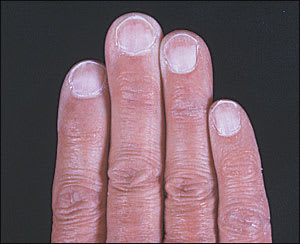
A 70-year-old man was having a routine skin cancer screening examination when an incidental finding of abnormal nail bed coloration was noted. The patient was unsure when the nail changes occurred and had no other skin or hair changes. The patient’s medical history was significant for type 2 diabetes and coronary artery disease. His nail beds (see accompanying figure) had a white discoloration with pink bands at the distal margins of the beds. The surface of the nails were smooth and without any defects.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Terry’s nails.
B. Onychomycosis.
C. Darier’s disease.
D. Onycholysis.
E. Malnutrition.
Discussion
The answer is A: Terry’s nails. Dr. R. Terry first reported this nail finding in 1954 in association with patients who had hepatic cirrhosis.1 His initial description detailed the nail bed as white in appearance with a ground-glass opacity. In addition, the nail bed contained a pink distal band that measured 1 to 2 mm in width.1,2
In 1984, Holzberg and colleagues2 revised the original inclusion criteria for classifying a patient as having Terry’s nails to what is used today. The affected nails have a nail bed that is white or light pink with a distal transverse band measuring 0.5 to 3.0 mm in width that is pink to brown in color. The lunula of the nail may or may not be present.2 The degree of pallor of the nail bed and the darkness of the distal band can vary based on how long the underlying systemic disease has affected the patient.
Terry’s nails are associated with several diseases and advancing age.1–4 Type 2 diabetes mellitus, congestive heart failure, chronic renal failure, and cirrhosis are all systemic diseases that are associated with Terry’s nails.1–4 The pathogenesis of these nail changes is unclear, but it is believed to involve changes in the microvascular system. In a study conducted by Holzberg,2 biopsies of nail beds that were performed on several patients showed dilated vasculature in the dermis of the distal band. Holzberg postulated that these vascular changes were related to the premature aging of the nail bed, which resulted in the abnormal appearance of the nail.2 While aging is a common cause of Terry’s nails, it is important for physicians to consider other disease entities that can lead to this abnormal nail appearance, especially in younger patients.
A patient with onychomycosis may present with whitened nails, but the discoloration is in the nail itself, rather than the underlying nail bed. A distal reddened band would not be seen. Diabetes, advancing age, and other relatively immunosuppressing conditions also are associated with onychomycosis.
Darier’s disease is a rare hyperkeratotic skin condition that may vary from subtle freckling to severe overgrowth of large papules and warty skin lesions, especially on the face and skinfold areas. When it affects the nails, it typically presents as longitudinal white and red streaks with V-shaped notches in the distal nail edge.
Onycholysis refers to a nail that has separated from the underlying nail bed, which often leads to a white or yellow discoloration of the nail. Trauma to the nail, fungal infection, psoriasis, and other conditions may lead to onycholysis. In onycholysis, the whitened area would be distal, with a proximal band of pinker, more normal appearing nail bed.
In malnutrition, the nails may become diffusely white. Usually, there also is evidence of muscle wasting, and the patient’s albumin level is below normal.
Selected Differential Diagnosis of Proximal White Finger Nails
| Condition | Characteristics |
|---|---|
| Terry’s nails | White proximal nail bed with a distal pink transverse band |
| Onychomycosis | Hyperkeratotic debris causing distal nail separation |
| Darier’s disease | Longitudinal white and red streaks with V-shaped notches distally |
| Onycholysis | Distal thickening and white discoloration of the nail after separation from the nail bed |
| Malnutrition | Diffusely white nails accompanied by muscle wasting |

