More than 13 million trauma patients are brought to U.S. and Canadian emergency departments annually with injuries initially requiring cervical spine (C-spine) precautions. Few patients end up having a C-spine fracture, yet many undergo immobilization on a backboard and radiographic imaging. Stiell and others compared the accuracy of their recently validated Canadian C-Spine Rule (CCR) (see accompanying figure) with that of a 12-year old guideline for C-spine imaging known as the NEXUS Low-Risk Criteria (NLC).
The authors conducted a prospective cohort study comparing the two C-spine decision rules at nine Canadian tertiary care hospital emergency departments. Alert and stable patients with or without neck pain, with any visible injury above the clavicles, or trauma related to a dangerous mechanism of injury were evaluated. Exclusion criteria were age younger than 16 years, pregnancy, unstable vital signs, or deduction of any points on the Glasgow Coma Scale.
Patients underwent plain radiography of the C-spine at the discretion of the treating physician. Any patient who was deemed not to need imaging at the time of injury was surveyed by telephone 14 days later, and radiographs were obtained if any high-risk clinical findings were present. A clinically important C-spine injury was defined as any fracture, dislocation, or ligamentous instability apparent on imaging.
Of the 12,521 eligible patients, complete analysis was possible in 8,283 cases. Treating physicians did not enroll 3,603 eligible subjects (28.8 percent), and outcome assessments were not available for 635 participants (5.1 percent). The CCR decision rule requires assessment of active neck rotation, but treating physicians declined to perform this maneuver in 845 patients (10.2 percent), and these subjects were excluded from the accuracy comparison of the two decision rules. Clinically important C-spine injuries were identified in 169 patients overall (2.0 percent).
FIGURE. Canadian C-Spine Rule
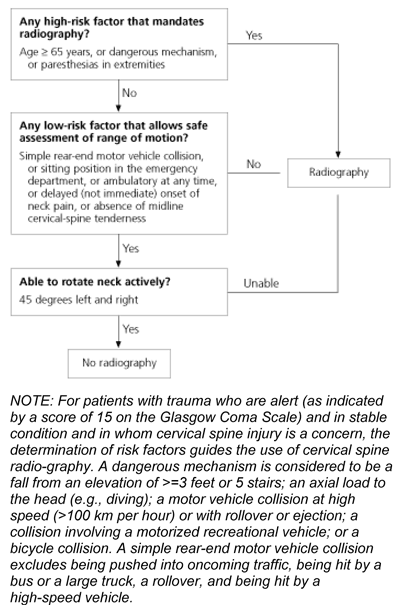
The Canadian C-Spine rule.
Adapted with permission from Stiell IG, Clement CM, McKnight RD, Brison R, Schull MJ, Rowe BH, et al. The Canadian C-Spine Rule versus the NEXUS low-risk criteria in patients with trauma. N Engl J Med 2003;349:2512.
The sensitivity of the CCR rule in identifying important injuries was 99.4 percent, and the specificity was 45.1 percent compared with 90.7 percent and 36.8 percent, respectively, for the NLC rule. Of the patients with important injuries, the authors calculated that 16 would have been missed by applying the NLC rule versus one patient missed by the CCR rule.
The authors conclude that the CCR decision rule is more sensitive than the NLC rule for identification of clinically important C-spine injuries and also is more specific, thereby decreasing the number of unnecessary C-spine radiographs.
editor’s note: The results of any study where almost 30 percent of eligible patients are not enrolled should be viewed with some skepticism. Yealy and Auble note in an accompanying editorial1 that the NLC rule was initially studied in over 34,000 patients, and a sensitivity of 99.6 percent was reported. He also notes that the CCR rule was developed at the same Canadian medical centers where this study was conducted. This rule may have been more familiar to the treating physicians than the U.S.–derived NLC guideline. Regardless of which rule is employed, one can see that with C-spine radiographs ordered in over two thirds of trauma cases and important injuries identified in only 2 percent of them, adoption of any validated C-spine decision rule would go some way toward limiting wasteful overuse of medical resources.—b.z.

