
Am Fam Physician. 2004;70(4):753-754
A 33-year-old woman presented with a one-year history of erosions on her hands and wrists (see accompanying figure), and increased hair growth on her temples and zygomatic areas. She stated that minor physical trauma would lead to erosions or blisters on her hands. She admitted to being a heavy drinker. Her medical history was noncontributory, and she was not taking any medications.
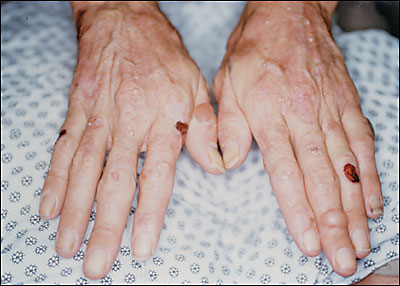
Question
Discussion
The answer is D: porphyria cutanea tarda. Porphyria cutanea tarda is the most commonly encountered type of porphyria. It may be acquired or hereditary (familial). The much less common familial form is inherited as an autosomal dominant trait. The onset of skin lesions in both forms typically occurs in adulthood. In the acquired form, hepatic uroporphyrinogen decarboxylase becomes deficient because of exposure to certain chemicals that inhibit the enzyme, leading to impaired heme-ring synthesis and a buildup of porphyrins. The most common inducer of this type of porphyria cutanea tarda is alcohol.
Other factors that may cause acquired porphyria cutanea tarda include estrogen supplements or excess iron stores (e.g., hereditary hemochromatosis, dietary iron supplements). Porphyria cutanea tarda also has been associated with hepatitis C virus infection.1 The mechanism for the relationship is unclear.
Patients with porphyria cutanea tarda complain of increased skin fragility on the dorsum of the hands. Skin lesions present initially as bullae, which then rupture, leaving slow-healing erosions and crusted lesions. Another presenting sign is hypertrichosis, which most commonly occurs on the temples and lateral cheeks. The etiology of the hypertrichosis is unknown, but it often improves after treatment.
A diagnosis can be made by checking for increased total plasma porphyrin levels (typically >10 mcg per dL [120 nmol per L]) or by a 24-hour urine collection for quantitation of urinary porphyrins. Most cases are not diagnosed by skin biopsy, because patients often present with only erosions and no bullae, and a serum porphyrin level is simpler to perform. If bullae are present, a biopsy will show a subepidermal cleavage with no inflammatory response in the papillary dermis.
The treatment of choice is phlebotomy, which works by depleting excess hepatic iron stores. Approximately 500 mL (1 pint) is removed every one to two weeks, until the hemoglobin level decreases to 10 to 11 g per dL (100 to 110 g per L). Patients also should be advised to stop ingesting the provoking agent. Without phlebotomy, discontinuing the provoking agent alone requires months to years for remission, because of large stores of excess porphyrins in the liver.
Low-dose antimalaria therapy also is helpful in clearing skin lesions, especially in patients without excess iron stores or in those who cannot tolerate repeated phlebotomy. Hydroxychloroquine, 200 mg twice weekly, is the most commonly used agent.2 Low-dose therapy is important, because higher doses may produce hepatotoxicity.
Bullous pemphigoid presents as pruritic tense bullae and urticarial plaques, most commonly occurring in intertriginous areas. Middle-aged or elderly persons are most likely to be affected.
Epidermolysis bullosa is the term given to a number of related genetic disorders that affect dermal or epidermal structures, leading to blister formation, especially in areas of friction or trauma. Epidermolysis bullosa may look like porphyria cutanea tarda on the hands, but it is not associated with hypertrichosis.
Contact dermatitis may present with vesicles, but they are usually on an erythematous base. Lesion onset usually occurs in a pattern related to the skin irritant or allergen initiating the reaction.
Pemphigus vulgaris usually presents with flaccid bullae that lead to large painful erosions after rupture. Lesions often begin in the mouth, then spread to skin surfaces. Like pemphigoid, pemphigus vulgaris usually affects older patients.
| Condition | Characteristics |
|---|---|
| Bullous pemphigoid | Tense bullae on urticarial plaques |
| Epidermolysis bullosa | Similar to porphyria cutanea tarda, but not associated with hypertrichosis |
| Contact dermatitis | Vesicles on an erythematous base |
| Porphyria cutanea tarda | Erosions, milia, vesicles on normal skin; hypertrichosis on face |
| Pemphigus vulgaris | Flaccid bullae, large painful erosions |