A 27-year-old Caribbean-American woman, newly diagnosed with human immunodeficiency virus (HIV) infection, presented to the clinic with complaints of multiple cutaneous eruptions. The largest and oldest lesion was below her left calf (Figure 1), and newer lesions were present on her knee, elbow, and foot (Figure 2). It had been six months since the appearance of the first lesion, and she reported fevers up to 39°C (102°F) intermittently since that time. She did not have any lymphadenopathy or weight loss, but did note fatigue. Previous trials of oral cephalosporins had not improved the skin eruptions.
Figure 1.
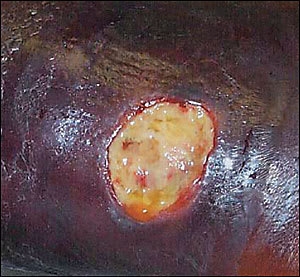
Figure 2.
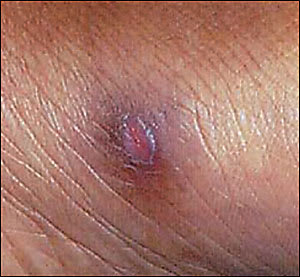
Her HIV viral load was 750,000 copies per mL by polymerase chain reaction and her CD4+ count was 50 per mm3 (50 × 106 per L). She had not previously used any medications for antiretroviral treatment or opportunistic infection prophylaxis, but subsequent to this visit she began taking lamivudine/zidovudine and lopinavir/ritonavir, with trimethoprim-sulfamethoxazole for Pneumocystis carinii pneumonia prophylaxis.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Mycobacterium haemophilum.
B. Pott’s disease with cutaneous fistula.
C. Cutaneous bacterial abscess.
D. Primary syphilis infection.
E. Kaposi’s sarcoma.
Discussion
The answer is A: Mycobacterium haemophilum. Skin swab sent for acid-fast bacillus staining came back positive, and culture eventually grew as M. haemophilum, sensitive to rifampin, clarithromycin, and ciprofloxacin. Resistance was noted to isoniazid, amikacin, and ethambutol. The patient was treated twice daily with rifabutin 300 mg, clarithromycin 500 mg, and ciprofloxacin 500 mg. One month after initiation of these antimycobacterial agents, she reported a 4 lb (1.8 kg) weight gain, cessation of fevers, and shrinking ulcer size.
M. haemophilum was first reported in 1978 as a cause of cutaneous ulceration in a patient with Hodgkin’s disease,1 and since then, more than 90 cases have been described. M. haemophilum is one of several nontuberculous mycobacterial species that are known to cause cutaneous infections. Laboratory characteristics of this species include optimal growth at 30°C (86°F) and a requirement for culture medium containing blood or iron.
Pott’s disease (Mycobacterium tuberculosis infection of the bone) is sometimes identified by an adjacent cutaneous fistula, and is a reasonable supposition in this case. Tuberculosis is a commonly encountered complication of advanced HIV infection, especially in persons who come from areas of the developing world where the disease is endemic. Laboratory culture, high pressure liquid chromatography, or DNA typing may be used to distinguish mycobacterial species.
Although bacterial infection may sometimes cause skin lesions or ulcerations similar to this case, empiric trials of antibiotics were unsuccessful for this patient, and subsequent bacterial cultures were negative.
Venereal Disease Research Laboratory studies also were negative, ruling out syphilis. In addition, this patient had multiple, painful ulcers on her extremities. In contrast, primary syphilis typically manifests as a single, painless chancre, most often located in genital or perineal areas caused by sexual contact.
If all the lesion cultures had been unrevealing, skin biopsy would have been the next step to rule out cutaneous malignancy or other abnormality. Kaposi’s sarcoma is the most common skin malignancy associated with HIV infection. As a tumor of vascular origin, Kaposi’s lesions tend to be reddish or purple in color and usually are raised. The large ulcerated lesion in this patient would not be typical.
Selected Differential Diagnosis of Cutaneous Ulceration In a Patient with HIV
| Condition | Characteristics |
|---|---|
| Mycobacterium haemophilum | Painful cutaneous ulcer in immunodeficient patients; systemic symptoms of fever, night sweats, mucopurulent drainage |
| Pott’s disease with cutaneous fistula | Tuberculosis of the bone (classically lumbar-sacral spine) with fever, weight loss, and draining fistula |
| Cutaneous bacterial abscess | Mucopurulent drainage with or without systemic symptoms (resembles classic impetigo, with honey-colored crust) |
| Primary syphilis infection | Painless ulcer with a firm outer rim |
| Kaposi’s sarcoma | Vascular origin, reddish or purple lesions that usually are raised |

