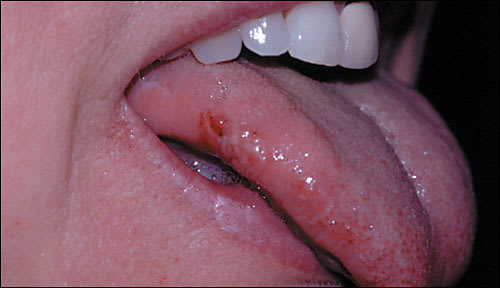
A 32-year-old woman is brought to the emergency department because of a blackout episode. This is her third visit in five months. She recalls nothing unusual before the episode, and had no warning symptoms. As with previous blackouts, she found herself on the floor and confused. There have been no witnesses to any of the episodes. She has no medical history and takes no medication, but does report a sore on her tongue (see accompanying figure).
Question
Based on the patient’s history and physical examination, which one of the following is the most likely diagnosis?
A. Transient ischemic attacks.
B. Syncopal episodes.
C. Epileptic seizures.
D. Psychogenic seizures.
E. Hypoglycemia episodes.
Discussion
The answer is C: epileptic seizures. Tongue biting should be asked about in regard to loss of consciousness or seizures, and it should be looked for during examination, especially when the patient presents to the emergency department shortly after an attack. When tongue lacerations are severe and painful, patients may report them, but when a tongue injury is less severe, patients may be unaware of its occurrence. Tongue biting in a possible seizure patient is a helpful finding, but it only occurs in about 20 to 30 percent of generalized tonic-clonic seizures (usually during the tonic phase), so its absence does not exclude a seizure diagnosis. Patients who incur injuries during blackouts, including tongue biting, tend to have an organic rather than psychogenic cause for their loss of consciousness.
Tongue lacerations do not occur with a transient ischemic attack (TIA). Loss of consciousness may occur with a vertebrobasilar TIA, but this is uncommon.
Tongue biting may occur with epileptic seizures and syncope. However, in syncope it is usually on the tip of the tongue because of a sudden fall on the chin that causes sudden mouth closure. Lateral tongue biting, however, is more specific for generalized tonic-clonic seizures.1,2
Patients with pseudoseizures may have dramatic and prolonged motor activity with their episodes and even throw themselves to the ground. While tongue, lip, or cheek biting occasionally is reported with pseudo-seizures, it is less common and typically less severe than the oral injuries that occur with tonic-clonic seizures.
Hypoglycemia gradually may cause loss of consciousness, but there are obvious premonitory symptoms, such as tremulousness, diaphoresis, and confusion. Tongue lacerations or other injuries are uncommon.
Selected Differential Diagnosis of Tongue Lacerations
| Condition | Characteristics |
|---|---|
| Transient ischemic attacks | Sudden onset of a focal neurologic deficit lasting a few minutes to a few hours; abrupt loss of consciousness is not a focal symptom and is not suggestive of an attack. |
| Syncopal episodes | Usually have prodromes and do not often cause tongue lacerations; if the tongue is bitten, it is on the tip rather than the side. |
| Epileptic seizures | Generalized tonic-clonic (“grand mal”) seizures cause lateral tongue lacerations; typical sequence is body stiffening (tonic) followed by generalized jerking (clonic) lasting one to two minutes, followed by a deep sleep (postictal phase). |
| Psychogenic seizures | Can vary but usually do not cause any type of injuries; tongue biting is rare. |
| Hypoglycemia episodes | Usually abundant prodromes of malaise, fatigue, dizziness; tongue biting is rare. |

