A 32-year-old white man who had tested positive for human immunodeficiency virus (HIV) presented with a two-year history of white papules and plaques on the lateral borders of his tongue (Figures 1 and 2). There were no lesions on the palate, the inner aspect of the cheeks, or the lips. The patient reported a history of smoking for several years. He denied a history of diabetes and was not taking any medications. Attempts to rub off these lesions with a tongue blade were unsuccessful, a potassium hydroxide preparation was negative for hyphae, and a rapid plasma reagin test was nonreactive.
Figure 1.
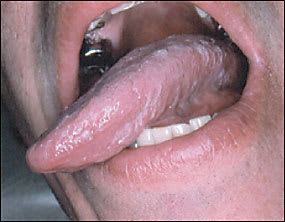
Figure 2.
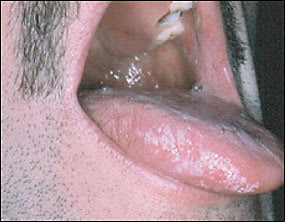
Question
Based on the patient’s history and physical examination, which one of the following is the most likely diagnosis?
A. Lichen planus.
B. Hairy leukoplakia.
C. Candidiasis.
D. Leukoplakia.
E. Secondary syphilis.
Discussion
The answer is B: hairy leukoplakia. Oral hairy leukoplakia is a distinctive condition strongly associated with Epstein-Barr virus (EBV). Often, it occurs in patients with HIV infection where it is believed to indicate more severe immunosuppression. It also has been reported in patients with other immunosuppressive conditions and rarely is seen in immunocompetent persons.
Hairy leukoplakia typically presents as bilateral corrugated, painless white thickening found on the lateral borders of the tongue, sometimes with hairy projections. It also may extend to the ventral or dorsal surfaces of the tongue, but rarely involves other oral mucosal sites, such as the floor of the mouth, palate, buccal mucosa, and oropharynx. Hairy leukoplakia results from a benign hyperplasia of the epithelial layer of the tongue. Lesion size can vary from a few millimeters to several centimeters.1 These whitish thickenings cannot be rubbed off with a tongue blade.
Oral hairy leukoplakia often has a recurrent clinical course that is thought to be a result of continuous reinfection by EBV. Treatment is not necessary in most cases, but these lesions often improve in patients with HIV when highly active antiretroviral therapy is initiated. Topical treatment with retinoids, podophyllin resin, trichloroacetic acid, or glycolic acid, and surgical removal have been used in some refractory cases.
Leukoplakia is not related to EBV infection and may be caused by repetitive trauma of the oral mucosa (e.g., sharp tooth edge, dental apparatus) or as a premalignant condition, especially in tobacco users. Hairy leukoplakia occasionally may be mistaken for leukoplakia, but the hairy projections, lateral border location, and associated immunosuppression typically will differentiate benign hairy leukoplakia from the premalignant risk of leukoplakia. Lesion biopsy may be needed to rule out squamous cell carcinoma, especially if the lesion is on the floor of the mouth or if there are speckled gray patches.2
Up to 70 percent of patients with lichen planus may have mucosal involvement. The classic intraoral manifestation of lichen planus is a network of lacy white lines on the buccal mucosa, but lesions also may be atrophic or erosive and the palate, lips, and tongue sometimes may be involved.
Oral candidiasis, or oral thrush, occurs in immunosuppressed patients, especially those with advanced HIV infection. Clinically, it appears as white, curd-like plaques on the mucosal surfaces, lips, dorsum of tongue, or palate. In more severe cases, involvement may extend from the oropharynx to the esophagus and tracheobronchial tree. The pseudomembranous material that accumulates in thrush can be rubbed off, revealing an erythematous or bleeding undersurface.
Secondary syphilis is caused by the hematogenous dissemination of Treponema pallidum. A widespread maculopapular rash that includes the palms and soles is highly suggestive of syphilis. Mucous patches also are common. These ulcerations can involve the tongue, buccal mucosa, and lips. The lesions are oval with raised borders, central erosions, and a gray membranous covering.3
Selected Differential Diagnosis of White Oropharyngeal Lesions
| Condition | Characteristics |
|---|---|
| Hairy leukoplakia | Lateral tongue borders, hairy projections, human immunodeficiency virus or other immunosuppression |
| Lichen planus | White lacy lines on buccal mucosa, with associated cutaneous rash |
| Candidiasis | Widespread intraoral plaques, erythematous base when removed |
| Leukoplakia | Intraoral trauma or premalignant lesion, may need biopsy |
| Secondary syphilis | Ulceration with gray membrane |

