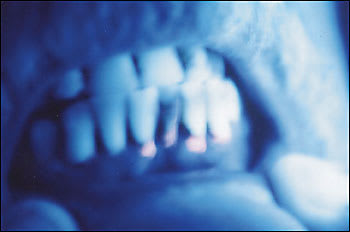
A 45-year-old white man presented for evaluation because of blistering and scarring of the dorsal hands for the past several months. The patient also noticed darker urine but otherwise felt healthy. A Wood’s lamp examination of the patient’s teeth showed a characteristic glow (see accompanying figure).
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Pemphigus vulgaris.
B. Tetracycline discoloration of teeth.
C. Epidermolysis bullosa.
D. Bullous pemphigoid.
E. Porphyria cutanea tarda.
Discussion
The answer is E: porphyria cutanea tarda. In this photograph, the patient’s teeth are illuminated with a Wood’s lamp (ultraviolet light). The resultant pink fluorescence is caused by buildup of excess porphyrins in the teeth. Excess porphyrins also are apparent in urine, where they are excreted as a water-soluble product. Wood’s lamp illumination of urine from an affected patient may reveal a similar fluorescent effect.1
Porphyria cutanea tarda belongs to a group of disorders characterized by deficient enzyme activity of uroporphyrinogen decarboxylase, which is involved in breakdown of the heme ring. There are inherited and acquired types of porphyria cutanea tarda, with the latter occurring more frequently. Factors associated with acquired porphyria cutanea tarda include alcohol use, hepatitis C, human immunodeficiency virus infection, hereditary hemochromatosis, and use of estrogen-containing medications.1–3
Porphyria cutanea tarda usually presents as blistering lesions of sun-exposed areas, such as the hands, arms, and face, often appearing after minor skin trauma. The bullae are thin-walled and rupture easily, leaving ulcerated skin lesions that heal slowly.
The diagnosis usually is confirmed by checking for elevated porphyrin levels in a 24-hour urine sample or by blood testing for plasma total porphyrin. Fecal studies also may be helpful.
Skin biopsy usually is not diagnostic because a number of other entities may have findings similar to porphyria cutanea tarda. Histopathology findings on biopsy include a cleavage plane at the dermoepidermal junction with scant inflammatory cells.
Treatment of porphyria cutanea tarda usually involves avoidance of inducing agents (i.e., sunlight, alcohol, and skin trauma). Therapeutic phlebotomy addresses the mild iron overload that is often present.3 Oral chloroquine or hydroxychloroquine may be used for patients who cannot tolerate phlebotomy.1
Tetracycline discoloration of teeth presents as a darkening of the dental enamel that is present in visible light and does not fluoresce on ultraviolet Wood’s lamp examination.
Epidermolysis bullosa is an uncommon hereditary skin disorder usually evident in infancy. It may present with bullae in areas of skin trauma.
Bullous pemphigoid and pemphigus vulgaris also cause blistering skin lesions that appear in later adulthood, similar to porphyria cutanea tarda. In these disorders, however, bullae typically are more widespread and often involve areas not exposed to the sun. Patients usually are more symptomatic, with pain or pruritus noted at sites of skin lesions. Both may have oral lesions, but dentition is not involved.
Summary Table
| Condition | Characteristics |
|---|---|
| Pemphigus vulgaris | Often with oral lesions |
| Epidermolysis bullosa | Family history |
| Bullous pemphigoid | Tense blisters |
| Porphyria cutanea tarda | Blistering in sun-exposed areas |

