
Am Fam Physician. 2005;72(3):491-492
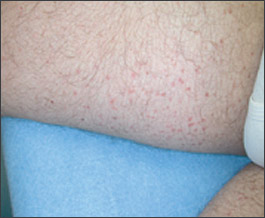
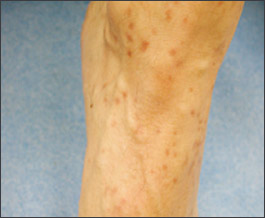
A 40-year-old man presented with a 15-year history of recurrent generalized papules and macules. On examination, the physician noted multiple brown-red macules and flat-topped papules, 5 to 10 mm in diameter, on the patient’s trunk and extremities (Figures 1 and 2). When these lesions were stroked, they became red, edematous, and pruritic, and some formed blisters.
Question
Discussion
The answer is D: urticaria pigmentosa. Urticaria pigmentosa is the most common type of cutaneous mastocytosis.1 Mastocytosis is a rare group of disorders resulting from the hyperplasia, infiltration, and accumulation of mast cells anywhere in the body. Urticaria pigmentosa may develop at any age; however, most cases affect children, often with initial manifestation at six to nine months of age.2,3 There is no known predisposition by race or sex.
Clinically, urticaria pigmentosa exhibits disseminated multiple brown-red macules and papules (rarely nodules and plaques), most often on the trunk and extremities. Usually the palms, soles, face, and scalp are spared.2 When the lesions are rubbed, they manifest erythema, edema, pruritus, and occasional bullae formation (i.e., Darier’s sign). The blisters heal without scarring.3 Patients often demonstrate prominent dermatographism and complain of generalized pruritus.3
The diagnosis is made clinically and confirmed with biopsy showing dermal infiltration by mast cells. Immunohistochemical stains may be used to detect mast cells.4
The etiology of urticaria pigmentosa is unclear. However, it is known to be related to a mutation of c-kit, a protooncogene that encodes for KIT, the receptor for stem-cell factor that determines mast-cell differentiation and proliferation.6
Management entails treating cutaneous lesions and minimizing associated systemic symptoms. The results of treating skin lesions with topical steroids under occlusion and PUVA (psoralen plus ultraviolet A) vary.5 To control associated systemic symptoms, histamine blockers (H1 and H2), aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), cromolyn sodium (Intal), and ketotifen (Zaditor) ophthalmic solution often are used.5 It also is crucial to emphasize avoidance of factors that trigger mast-cell degranulation (i.e., temperature and/or physical extremes, emotional stress, venoms, and certain medications [e.g., narcotics, salicylates, polymyxin sulfate, anticholinergics]). Patients at high risk for anaphylaxis should wear medical alert tags.
An adverse cutaneous drug reaction is a common immunologic response to medication. It often presents as a maculopapular or urticarial eruption within one to two weeks of starting the medication. Although this eruption may present clinically as generalized maculopapules, wheals, or both, the contrasting features include the recent onset and short-lived duration as well as the absence of pigmentation.
Acne vulgaris is an inflammatory disease of the pilosebaceous units that usually affects particular body regions (i.e., face, back, chest). It most often manifests in adolescents as comedones, papulopustules, and nodulocysts.
Syphilis presents in three stages. At the secondary stage, when the infection is systemic, it can mimic multiple cutaneous disorders. It usually is characterized by maculopapular, papulosquamous, pustular, or acneform eruptions that are prominent on the head, neck, palms, and soles.
Lymphocytoma cutis is a benign cutaneous inflammatory response to unknown stimuli. It usually presents in young adults as discrete nodules that may be pruritic or painful and are commonly localized to the face, chest, and upper extremities. Biopsy of the lesions demonstrates mixed inflammatory infiltrate. These lesions can be removed with excision or cryotherapy.
| Condition | Characteristics |
|---|---|
| Drug reaction | Maculopapular or urticarial eruption, short-lived, recent onset, no pigmentation |
| Acne vulgaris | Comedones, papulopustules, nodulocysts on the face, back, and chest |
| Secondary syphilis | Maculopapular, papulosquamous, pustular, or acneform eruptions mostly prominent on the head, neck, palms, and soles |
| Urticaria pigmentosa | Disseminated brown-red macules and papules on the trunk and extremities; may exhibit wheal and flare when lesions are rubbed |
| Lymphocytoma cutis | Discrete nodules that may be pruritic or painful; localized to face, chest, and upper extremities |