Cutaneous warts are a common presenting complaint in children and adolescents. Common, plantar, or flat warts are cutaneous manifestations of the human papillomavirus. The treatment of wart s poses a therapeutic challenge for physicians. No single therapy has been proven effective at achieving complete remission in every patient. As a result, many different approaches to wart therapy exist. These approaches are discussed to demonstrate the evidence supporting common therapies and provide a guideline for physicians. Evidence supports the at home use of topical salicylicacid and physician administered cryotherapy. Intralesional immunotherapy for nongenital cutaneous warts may be an option for large or recalcitrant warts.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Topical salicylic acid therapy is recommended for nongenital cutaneous warts. | A | 4–6 |
| Cryotherapy is not recommended over salicylic acid for treatment of nongenital cutaneous warts. | A | 5 |
| There is poor evidence to recommend pulsed dye laser therapy for nongenital cutaneous warts. | B | 4,19,20 |
| There is insufficient evidence to recommend imiquimod (Aldara) for treatment of cutaneous warts. | B | 4 |
| There is inconsistent evidence to recommend bleomycin (Blenoxane) for treatment of cutaneous warts. | B | 5 |
| Intralesional immunotherapy with Candida skin test antigen can be used as a second-line therapy for cutaneous warts. | B | 3,4,6,26 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 555 orhttps://www.aafp.org/afpsort.xml.
Warts are the cutaneous manifestations of human papillomavirus (HPV). Warts may exist in different forms given the epithelial surface and HPV type responsible for the infection. Common warts (Verruca vulgaris) (Figures 1 and 2), plantar warts (Verruca plantaris) (Figure 3), flat or planar warts (Verruca plana), and genital warts (Condyloma acuminata) are some of the clinical manifestations of HPV infection.1
Figure 1.
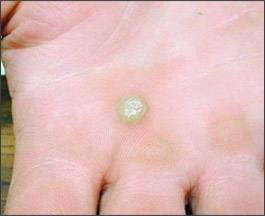
Verruca vulgaris (common wart) on palm of right hand.
Figure 2.
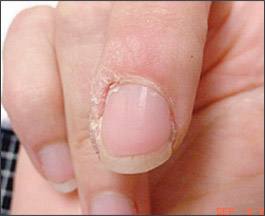
Third digit of right hand with Verruca vulgaris involving the periungual region (also referred to as periungual wart).
Figure 3.
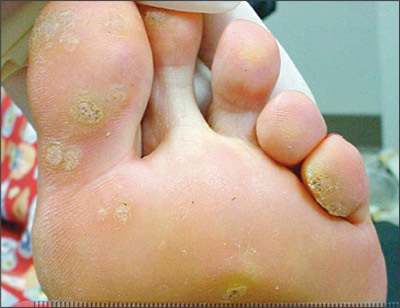
Verruca plantaris (plantar warts) on the sole of the foot.
Warts are estimated to occur in up to 10 percent of children and young adults. The range of greatest incidence is between 12 and 16 years of age.1 Warts occur with greater frequency in girls than in boys. The peak incidence is at 13 years of age in females and 14.5 years of age in males.1
A study2 examining the natural progression of warts indicated that warts will spontaneously clear after two years without treatment in 40 percent of children. Warts typically continue to increase in size and distribution and may become more resistant to treatment over time.3 Children with treatment resistant warts potentially may be reservoirs for HPV transmission. In addition, warts can be painful depending on their location (e.g., soles of the feet and near the nails) and viewed as socially unacceptable when located on visible areas (e.g., hands and face).4
Therapies and Treatment Strategies
Treating warts is a therapeutic challenge for family physicians. No single therapy has been proven effective at achieving complete remission in every patient.4 As a result, many different approaches exist, including observation and treatments that can be combined for greater effectiveness.4 The results of evidence-based approaches to wart therapy are discussed in this article to demonstrate the evidence for common therapies.4–6 A Cochrane review5 rated the randomized controlled trials (RCTs) of local treatments for cutaneous warts as generally weak because of poor methodology and reporting. Additionally, the average cure rate for placebo preparations was 30 percent.5 Each treatment decision should be made on a case-by-case basis according to the experience of the physician, patient preference, and the application of evidence-based medicine.6 Immunocompromised patients with warts may exhibit incomplete clearance, and the warts may be resistant to treatment.7 The two most common treatments for warts are patient-applied salicylic acid and physician-administered cryotherapy with liquid nitrogen.5
SALICYLIC ACID
The Cochrane review5 identifies topical therapy with salicylic acid as safe and effective and reports that no clear evidence exists to prove that other therapies have an advantage in regard to higher cure rates or fewer adverse effects. The pooled data from six RCTs demonstrated a cure rate of 75 percent in those treated with salicylic acid compared with 48 percent in the control group.5 Another guideline4 lists salicylic acid as the first-line therapy for flat warts on the face, plantar warts, and flat and common warts on the hands.
Various preparations of salicylic acid are available commercially. Over-the-counter preparations are less than 17 percent salicylic acid, whereas physician-prescribed preparations can contain as much as 70 percent salicylic acid.6 Because of the lack of data, comparing individual products is not possible. Treatment response rates of 40 to 84 percent (with an average of 61 percent) have been reported.8 The therapeutic benefit of topical therapies containing salicylic acid, whether over-the-counter or prescription, is supported by evidence from RCTs.7,9–11 Advantages and disadvantages of salicylic acid in comparison with other therapies are summarized in Table 1.4,6,12 There is consistent evidence that topical salicylic acid is an effective therapy for nongenital cutaneous warts (Table 2).6
TABLE 1 Treatment of Cutaneous Warts
| Treatment | Advantages | Disadvantages | Administration | Cost* |
|---|---|---|---|---|
| Salicylic acid | Available over the counter, inexpensive | Requires time to achieve response | Daily application of a 15 to 20 percent salicylic acid preparation | $5 to $7 |
| Cryotherapy | Easy | Scarring, painful | Average of three or four treatments in the office | Approximate cost for initial visit plus cryotherapy to one wart is $250; three follow-up visits for cryotherapy to one wart are $360; total is $610 |
| Pulsed dye laser therapy | Fewer treatments | Scarring, painful | Average of one to three treatments in the office | Approximate cost for initial visit with laser treatment plus two follow-up treatments is $360 |
| Imiquimod (Aldara) | At-home use; pregnancy category B | Erythema, pruritus, erosions, bacterial infections | Three times a week at home for nongenital warts | $177 for 12-packet box of 5 percent imiquimod |
| Bleomycin (Blenoxane) | Typically only one treatment needed | Pain during and after treatment, pigment changes, Raynaud’s phenomenon, expected necrotic eschar, scarring, nail damage, pregnancy category D | Intralesional injection of 0.3 mL (0.15 units) every three to fourweeks in the office† | Approximate cost for initial visit plus injection and possible follow-up injection is $495 15-unit vial is $304 (brand) or $192 to $309 (generic) |
| Retinoids | At-home use | Local irritation, pregnancy category C, systemic side effects | 0.05 percent tretinoin cream (Retin-A), three months oral at home | $48 to $54 for 45-g tube of topical tretinoin $447 for 30-day supply of acitretin (Soriatane) 25-mg tablets |
| Intralesional immunotherapy | Only need to treat one wart | Rare influenza-like symptoms | Inject every three to four weeks for an average of three treatments in the office | Approximately $190 for initial visit with injection of Candida and two follow-up injections |
*—Estimated cost to the pharmacist based on average wholesale prices in Red book. Montvale, N.J.: Medical Economics Data, 2005. Cost to the patient will be higher, depending on prescription filling fee.
†—Bleomycin comes in 15-unit vials and is typically diluted with 30 mL of saline; 0.3 mL (0.15 units) of this solution are injected into the wart.
Adapted with permission from Clemons RJ, Clemons-Miller A, Johnson SM, Williamson SK, Horn TD. Comparing therapy costs for physician treatment of warts. J Drugs Dermatol 2003;2:653, with additional information from references 4 and 6.
TABLE 2 Treatment Considerations for Nongenital Cutaneous Warts
| HPV infection | First-line therapy | Second-line therapy | Third-line therapy |
|---|---|---|---|
| Common warts(Verruca vulgaris) | Salicylic acid, cryotherapy | Cantharidin* | Bleomycin (Blenoxane), intralesional immunotherapy, pulsed dye laser therapy |
| Flat warts(Verruca plana) | Salicylic acid, imiquimod (Aldara) | Cryotherapy, retinoids | Intralesional immunotherapy, pulsed dye laser therapy |
| Plantar warts(Verruca plantaris) | Salicylic acid | Cryotherapy, intralesional immunotherapy, pulsed dye laser therapy | Bleomycin, surgical excision |
HPV = human papillomavirus.
*—Not discussed in this article because it has not been approved by the U.S. Food and Drug Administration.
Information from reference 6.
CRYOTHERAPY
Cure rates for cryotherapy vary widely, depending on the treatment regimen. In general, the wart is frozen for 10 to 30 seconds until a 1- to 2-mm iceball halo surrounds the targeted area.4,6 The highest cure rates are achieved when treatment occurs at a frequency of every two to three weeks.10,13 Benefit from therapy continuing for more than three months has not been documented.7,8 Optimal cure rates for plantar warts have been demonstrated by paring the hyperkeratotic surface and using two freezes with a complete thaw in between.7,10 For common warts not located on the palms or soles, a single freeze is preferred.6 One report4 states that cryotherapy is recommended as first-line therapy for flat and common warts.
Cryotherapy also is suggested as second-line therapy for common and flat warts on the face.4 Another review6 supports the use of cryotherapy as an effective treatment for common and plantar warts (paring with two cycles of freezing) and for flat warts. The Cochrane review5 reports that cryotherapy is no more effective than simple topical treatments for nongenital cutaneous warts.
PULSED DYE LASER
Treatment with a vascular lesion laser, also known as pulsed dye laser therapy, can selectively target hemoglobin contained in blood vessels within the wart.14 As the hemoglobin heats up, thermal energy is dissipated to surrounding tissues, leading to cauterization of blood vessels. The result is a necrotic wart that eventually sloughs off.14 Studies examining the effectiveness of pulsed dye laser therapy after an average of two or three treatments have reported overall cure rates of 48 to 93 percent for warts located at various sites.15,16 One study17 demonstrated an overall clearance rate of 72 percent. The highest clearance rate was 85.7 percent for periungual warts, and the lowest clearance rate was 50 percent for plantar warts.17
A separate study18 compared pulsed dye laser therapy with cryotherapy and cantharidin. Of the patients treated with cryotherapy or cantharidin, 70 percent demonstrated clearance after two treatments, whereas 66 percent of the patients treated with pulsed dye laser demonstrated clearance following two treatments.18 The authors concluded that pulsed dye laser therapy is as effective as conventional therapy.18 Pulsed dye laser therapy is recommended as second-line therapy for plantar warts and third-line therapy for common warts and flat warts.6 However, another review4 found poor evidence to support the use of a single pulsed dye laser treatment because of problems with study methodology and listed it for the treatment of warts located on the hands and feet only.
IMIQUIMOD
Imiquimod (Aldara) is a topical immune response modifier manufactured as a 5 percent cream. Although RCTs are lacking, imiquimod has demonstrated potential efficacy in the treatment of recalcitrant nongenital warts. In a study19 using imiquimod, cure rates of 88.9 percent were observed for recalcitrant nongenital warts in children when applied twice daily. The duration of treatment ranged from two to 12 months with a mean duration of 5.8 months.19 A separate small study20 demonstrated similar results. Imiquimod was applied once a day and occluded for a total of four weeks; of the 10 study participants, nine demonstrated complete clearance of recalcitrant common warts.20 RCTs are warranted to further examine the efficacy of imiquimod for nongenital warts. One review6 based on non-randomized historical cohort comparisons supported the use of imiquimod as first-line therapy for treatment of flat warts. Another review,4 however, found insufficient evidence to support the use of imiquimod for treatment of cutaneous nongenital warts.
BLEOMYCIN
Bleomycin (Blenoxane), a chemotherapeutic agent, inhibits DNA synthesis in cells and viruses. Bleomycin is an alternative therapy for warts that have not responded to other therapies or warts that may be difficult to surgically excise. Bleomycin comes in 15-unit vials; it typically is diluted with 30 mL of saline, and 0.3 mL (0.15 units) are injected into the wart.6 Additional injections can be given every three to four weeks until clearance is achieved.6 Pain is the major limiting factor to treatment. Potential side effects include scarring, change in pigmentation, nail damage, and Raynaud’s phenomenon.4,21 Bleomycin is listed as pregnancy category D, given its potential for significant absorption following injection.22 One study23 examined the use of bleomycin for the treatment of recalcitrant warts. Following application of a topical anesthetic, bleomycin was placed on the wart and “pricked” into the wart using a needle. A clearance rate of 92 percent was observed.23
Although the number of RCTs that demonstrate the efficacy of bleomycin is low, one review4 has concluded that there is fair evidence to support its use for recalcitrant hand and plantar warts. The Cochrane review5 states that there is no consistent evidence for the effectiveness of intralesional bleomycin for treatment of nongenital cutaneous warts, and the data could not be meaningfully pooled for analysis. Another review,6 based on four RCTs and multiple case series that provide evidence of the effectiveness of bleomycin, recommends its use as a third-line therapy for common and plantar warts.
RETINOIDS
Systemic retinoids have been used to treat warts because of their ability to alter keratinization and accelerate the clearing of warts by inducing an irritant dermatitis.24 A small study25 examined the efficacy of etretinate in children with extensive warts. Etretinate is no longer available in the United States; acitretin (Soriatane) is used now. A dose of 1 mg per kg per day of etretinate was given for no more than three months.25 Of the 20 children involved in the study, 16 demonstrated complete clearance of their warts without relapse. Warts recurred in four patients following partial regression.25
One review4 found fair evidence supporting the use of topical retinoids based on one cohort study that examined the effectiveness of topical retinoids using a number of case reports and a limited number of trials of systemic retinoids. Another review6 of several case studies recommended oral and topical retinoids as second-line therapy for the treatment of flat warts.
INTRALESIONAL IMMUNOTHERAPY
Intralesional immunotherapy employs the ability of the immune system to recognize certain viral and fungal antigens. Candida skin test antigen generally is used. It is believed that the delayed-type hypersensitivity reaction induced by these antigens increases the ability of the immune system to recognize and clear HPV. One study3 demonstrated complete resolution of warts in 47 percent of the participants and 75 to 99 percent resolution in 13 percent of the participants. In 34 percent of those enrolled in the study, complete clearance of all warts distant from the injection site was noted.3 In 22 percent of the study participants, clearance rates of 75 to 99 percent for distant warts also were noted.3 The regression of warts at distant sites has not been established with other therapies. An initial study26 examined the clearance rates for the mumps and Candida antigens separately compared with cryotherapy (mumps antigen has been discontinued). Complete clearance rates of 49 percent for mumps immunotherapy and 70 percent for Candida immunotherapy were observed, compared with the 42 percent clearance rate observed for cryotherapy.26 The most common side effect was itching at the injection site.3 Other side effects included an influenza-like illness that lasted less than 24 hours and improved with nonsteroidal anti-inflammatory drugs.26 Intralesional immunotherapy is a promising treatment that warrants more clinical trials to further evaluate its effectiveness.4 Although the number of published RCTs remains limited, one review6 recommended intralesional immunotherapy as second-line therapy for plantar warts and third-line therapy for common and flat warts.

