Intertrigo is inflammation of skinfolds caused by skin-on-skin friction. It is a common skin condition affecting opposing cutaneous or muco-cutaneous surfaces. Intertrigo may present as diaper rash in children. The condition appears in natural and obesity-created body folds. The friction in these folds can lead to a variety of complications such as secondary bacterial or fungal infections. The usual approach to managing intertrigo is to minimize moisture and friction with absorptive powders such as cornstarch or with barrier creams. Patients should wear light, nonconstricting, and absorbent clothing and avoid wool and synthetic fibers. Physicians should educate patients about precautions with regard to heat, humidity, and outside activities. Physical exercise usually is desirable, but patients should shower afterward and dry intertriginous areas thoroughly. Wearing open-toed shoes can be beneficial for toe web intertrigo. Secondary bacterial and fungal infections should be treated with antiseptics, antibiotics, or antifungals, depending on the pathogens.
Intertrigo is the clinical description of a cutaneous inflammatory process on opposing skin surfaces. The condition is most commonly found in the groin, axillae, and inframammary folds. It also may affect antecubital fossae; umbilical, perineal, or interdigital areas; neck creases; and folds of the eyelids.1,2 Intertrigo is a common disorder that can affect patients throughout life.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Advise patients to dry intertriginous areas after showering. | C | 2,7 |
| In general, treat simple intertrigo by minimizing moisture and friction. | C | 4 |
| Topical or oral antibiotics and antifungals should be used for intertrigo secondarily infected by bacteria, yeasts, or dermatophytes. | B | 6–8,17,18 |
A = consistent, good quality patient-oriented evidence; B = inconsistent or limited quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For more information about the SORT evidence rating system, see page 736 orhttps://www.aafp.org/afpsort.xml.
Etiology and Predisposing Factors
Intertrigo is primarily caused by skin-on-skin friction and is characterized by initial mild erythema that may progress to a more intense inflammation with erosions, oozing, exudation, maceration, and crusting.3 Intertrigo is facilitated by moisture trapped in deep skinfolds where air circulation is limited. The condition is particularly common in obese patients with diabetes who are exposed to high heat and humidity, but it can occur in anyone. Other predisposing risk factors include urinary and fecal incontinence, hyperhidrosis, poor hygiene, and malnutrition. Toe interweb intertrigo may be associated with closed-toe or tight-fitting shoes and commonly affects persons participating in athletic, occupational, or recreational activities. Infants are at high risk for intertrigo because they have short necks, relative chubbiness, and flexed posture.3,4 Drooling also can facilitate intertrigo in infants. Persons with prominent skinfolds on either side of the chin are at a high risk for intertrigo.5
Secondary Skin Infections
The moist, damaged skin associated with intertrigo is a fertile breeding ground for various microorganisms, and secondary cutaneous infections commonly are observed in these areas. Bacterial proliferation may be associated with keratinocytic necrosis. Staphylococcus aureus may present alone or with group A beta-hemolytic streptococcus (GABHS).6 Pseudomonas aeruginosa, Proteus mirabilis, or Proteus vulgaris also may occur alone or simultaneously.
A variety of fungi may exacerbate intertrigo, including yeasts, molds, and dermatophytes. Candida is the fungus most commonly associated with intertrigo. The inflammation may begin as a dermatophyte infection, which can damage the stratum corneum and encourage the proliferation of other, usually antibiotic-resistant bacteria.7
Dermatophytes (e.g., Trichophytonrubrum, Trichophyton mentagrophytes, Epidermophyton floccosum) commonly complicate interdigital intertrigo. Gram-positive and gram-negative bacteria also can worsen the effects of interdigital intertrigo. Gram-negative toe web infections often are caused by P. aeruginosa combined with other gram-negative bacteria such as Moraxella, Alcaligenes, Acinetobacter, and Erwinia.7,8 However, gram-negative and gram-positive infections occasionally occur simultaneously in interdigital areas. Gram-positive infections usually are caused by S. aureus and GABHS and occasionally are caused by Staphylococcus saprophyticus or other coagulase-negative staphylococci. Dermatophytes and bacterial infections often occur together in interdigital areas. Yeasts also are commonly found at the site of interdigital intertrigo.9 Sometimes seborrheic dermatitis is located in the folds. Whether Malassezia-complicated intertrigo is a distinct entity or a type of seborrheic dermatitis remains unclear.
Cutaneous erythrasma may complicate intertrigo of interweb areas, intergluteal and crural folds, axillae, or inframammary regions.10 Erythrasma is a bacterial infection caused by Corynebacterium minutissimum. Cutaneous erythrasma presents as small, red-brown macules that may coalesce into larger patches with sharp borders.1 These lesions often are asymptomatic but may be pruritic in some instances.
Clinical Manifestations
Intertrigo is characterized primarily by mild erythema that initially presents as red plaques, almost in a mirror image, on each side of the skinfold.3,11 The erythema may progress to more intense inflammation with erosions, oozing, fissures, exudation, maceration, and crusting. Patients may present with itching, burning, and pain in the affected areas.1,3 More prominent inflammation could be a sign of secondary infection. Well-demarcated red, weeping intertrigo may be mechanical or may be a sign of secondary GABHS infection.6 Streptococcal intertrigo may be difficult to recognize in children when it presents as an intense erythema with maceration on the neck folds, axillae, or inguinal regions; it is characterized by a foul odor and an absence of satellite lesions.6 Candidal intertrigo usually presents as typical satellite papules or pustules (Figure 1).
Figure 1.
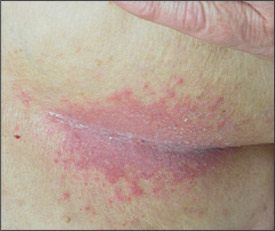
Intertrigo in the inframammary fold infected by Candida. Note satellite papules and pustules.
Toe web intertrigo usually is associated with a burning sensation between the toes, often with maceration.7.8 Toe web intertrigo may be simple, mild, and asymptomatic, but it also can be seen as intense erythema and desquamation, which sometimes is erosive, malodorous, and macerated (Figure 2). Patients also may have profuse or purulent discharge and be unable to ambulate. In severe examples, patients may have a purulent discharge with edema and intense erythema of tissues surrounding the infected area. Patients with severe toe web intertrigo who are overweight or who have diabetes are at a higher risk for cellulitis. Patients with advanced gram-negative infections may have green discoloration at the infection site. Erythematous desquamating infection may be more chronic than the acute form and may present with a painful, exudative, macerating inflammation that causes functional disability of the feet.
Figure 2.
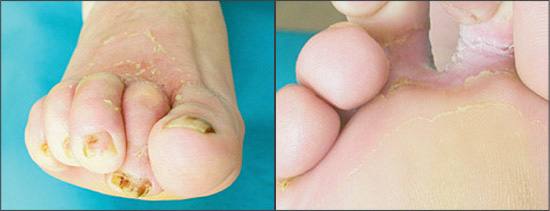
Toe web intertrigo complicated byCandida albicans infection. (Left) Anterior view (Right) Posterior view.
Acute genitocrural intertrigo with accompanying fever, fatigue, sore throat, and arthralgia may be a component of an acute febrile illness. Acute genitocrural intertrigo in patients with human immunodeficiency virus type 1 (HIV-1) infection may present as a maculopapular eruption.12
Diagnosis
Diagnosis of intertrigo and its secondary complications often is clear and is generally based on clinical manifestations. The characteristics of intertriginous lesions (e.g., erosions, vesicles, pustules, nodules, papules, plaques, macules) can indicate the type of disorder present.2 Skin biopsy specimens usually are not required because the histology of intertrigo shows no characteristic features. If secondary bacterial infections are suspected, culture with sensitivities should be performed. A Wood’s light examination may identify a Pseudomonas or erythrasma infection more quickly than would a culture. The Wood’s light characteristically shows a green fluorescence with Pseudomonas infection and a coral-red fluorescence with erythrasma. Potassium hydroxide cytologic examination is helpful in diagnosing secondary fungal infections. Hyphae should be apparent with dermatophytes, whereas pseudohyphae should appear if candidiasis is present.8 A mycologic culture may help identify the specific species.
Differential Diagnosis
Patients who do not respond to therapy should be reexamined for another primary or secondary dermatologic condition that may resemble intertrigo (Table 11,11,13,14). Seborrheic dermatitis and psoriasis vulgaris inversa may have presentations similar to intertrigo.13,14 Seborrheic dermatitis may involve the axillae or inguinal regions or the scalp. Psoriasiform lesions elsewhere on the body or pitting of the nails also may distinguish psoriasis from intertrigo. Rarely, skin biopsy specimens are needed to distinguish less common skin diseases from intertrigo. Atopic dermatitis, primary irritant contact dermatitis, allergic contact dermatitis, scabies, and pemphigus vegetans sometimes are mistakenly diagnosed as intertrigo because these conditions also may involve skinfolds. Unusual intertriginous involvement also may represent a localized drug eruption.15 The presence of widespread macular eruptions and eroded lesions in the inguinal folds, with negative cultures, may be an early marker of primary HIV-1 infection.12
TABLE 1 Differential Diagnosis of Simple Intertrigo
| Diagnosis | Differentiating characteristics |
|---|---|
| Allergic contact dermatitis | More intense pruritus; signs of eczema in other body locations; positive patch tests |
| Irritant contact dermatitis | More intense pruritus; signs of eczema in other body locations |
| Atopic dermatitis | More intense pruritus; coexisting atopic diseases (e.g., asthma, rhinitis) or family history of atopic diseases; wool intolerance; often in antecubital and popliteal fossae |
| Seborrheic dermatitis | Erythematous scaly patches on the scalp; dandruff |
| Psoriasis vulgaris inversa | Psoriasiform lesions elsewhere on the body (especially on the scalp, elbows, knees, and sacral area); typical nail changes (e.g., pitting, “oil spots,” nail dystrophy) |
| Vitamin deficiency | Other signs of hypovitaminosis (e.g., phrynoderma) |
| Pemphigus vegetans | Coexisting erosions and blisters on skin or mucosae; circulating antibodies of pemphigus type; histopathology with positive immunofluorescent examination |
| Hailey-Hailey disease (familial benign chronic pemphigus) | Small blisters at the edge of the lesions; palmoplantar keratoderma and longitudinal nail stripes may occur |
Treatment
The common approach to intertrigo management, particularly in infants, is a gentle one.2 The conventional therapy for simple intertrigo is minimizing moisture and friction. Some suggest the use of absorptive powders, such as talc and cornstarch, or barrier creams. These topical treatments, however, have little or no proven benefit and may cause irritation or facilitate yeast colonization.2 Obese patients should lose weight, if possible. Patients should wear light, noncon-stricting, and absorbent clothing and should avoid nylon and other synthetic fibers.3 Bio-textiles (e.g., cotton or polyester gauze with built-in antiseptic molecules) also may help patients with intertrigo.3 Table 2 illustrates the recommended therapies for patients with intertrigo.2–4,6,7,10,16
TABLE 2 Therapeutic Modalities for Intertrigo
| Type of intertrigo | Recommended therapy |
|---|---|
| Simple intertrigo | Drying agents such as talc or cornstarch; topical mild steroid lotion in cases of predominant inflammation |
| Intertrigo infected by bacteria | Topical or oral antibiotics |
| Intertrigo infected by yeasts | Topical antifungals (e.g., imidazoles, allylamines, ciclopirox [Loprox]); oral antifungals only if topical therapy was not effective (e.g., fluconazole [Diflucan], or itraconazole [Sporanox]) |
| Intertrigo infected by dermatophytes | Topical antifungals (e.g., imidazoles, terbinafine [Lamisil], ciclopirox); oral antifungals if topical therapy is not effective (e.g., terbinafine, itraconazole) |
| Intertrigo complicated by erythrasma | Topical or oral erythromycin |
Secondary bacterial and fungal infections also need to be treated. The best therapy for intertrigo patients (adults and children) with GABHS may be a concomitant or independent regimen of topical therapies (e.g., mupirocin [Bactroban], erythromycin); oral antibiotics (e.g., penicillin, first-generation cephalosporins); and low-potency topical steroids (e.g., hydrocortisone 1 percent cream).6,17 The latter may be particularly useful if the intertrigo is associated with seborrheic or atopic dermatitis. Cutaneous erythrasma is best managed with oral erythromycin (250 mg four times daily for two weeks). Topical clindamycin (Cleocin T), Whitfield’s ointment, sodium fusidate ointment, and antibiotic soaps also may be beneficial.10
Candida infections should be managed topically with antifungal lotions, creams, or ointments (e.g., imidazoles, terbinafine [Lamisil], ciclopirox [Loprox]). Oral terbinafine or oral triazoles (e.g., fluconazole [Diflucan], itraconazole [Sporanox]), may accompany the topical treatment.3,16,18 Topical terbinafine and ciclopirox have strong anti-inf lammatory properties, making a topical steroid, such as hydrocortisone 1 percent cream, unnecessary. If the patient does not improve after treatment, bacterial culture and sensitivity should be performed.
Toe web infections can be serious,7,8 and severe cases may warrant hospitalization. Proper identification of gram-negative organisms is critical so that effective antibiotic therapy can be initiated. Tissue removal may be needed to allow absorption of topical antibiotic agents, which promote healing and slow the spread of infection. Rare deep tissue infections need to be evaluated surgically. Antibiotic sensitivities should determine what topical and systemic therapies are used. Third-generation cepha-losporins and quinolones are active, together with aminoglycosides.7,8 Oral antibiotics combined with cleansing and debridement, 5 percent amikacin gel, and hot compresses of 2 to 5 percent acetic acid for 15 days may be effective. Ciprofloxacin (Cipro) (500 mg twice daily for 10 days) is another option, but some patients may need parenteral therapy instead (e.g., 1 to 3 g daily of intramuscular ceftazidime [Fortaz], 2 g daily of cefotaxime [Claforan] for 10 days).
Prevention
Little evidence-based literature supports any specific preventive measures for intertrigo.3 However, optimal prevention includes minimizing skin-on-skin friction, reducing heat and moisture around skinfolds, and keeping high-risk areas clean and dry.3 Patients should be warned about heat, humidity, and outside activities. Physical exercise usually is desirable, but patients should shower after exercise and keep intertriginous areas thoroughly dry. Wearing open-toed shoes may help prevent toe web intertrigo.

