The recognizable appearance and the dermatomal distribution of herpes zoster lesions usually enable a clinical diagnosis to be made easily. Herpes zoster and postherpetic neuralgia occur mainly in older patients. The role of the varicella vaccine in preventing herpes zoster is uncertain, but is being studied. There is evidence to support using antiviral therapy and possibly low-dose tricyclic antidepressants to prevent postherpetic neuralgia. There is good evidence that treating herpes zoster with antiviral medication is beneficial, particularly in patients older than 50 years with severe outbreaks. The use of steroids has an unfavorable risk-benefit ratio. In patients who develop postherpetic neuralgia, there is good evidence to support treatment with gabapentin and tricyclic antidepressants. More evidence for treatment with capsaicin cream, lidocaine patch, and opioids is needed. Intrathecal methylprednisolone is an option for patients with persistent pain.
Herpes zoster (i.e., shingles) is a painful rash resulting from the reactivation of the varicella-zoster virus in the dorsal root ganglia. Risk factors for developing herpes zoster are increasing age, immunosuppression, intrauterine exposure to varicella (i.e., chickenpox), and outbreak of varicella at younger than 18 months. Herpes zoster is contagious to those who have not had varicella or have not received the varicella vaccine.
Approximately 500,000 cases of herpes zoster occur in the United States each year.1 In one large study2 of primary care patients, the annual incidence was two per 1,000 persons.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should treat acute herpes zoster with antiviral medication within 72 hours of symptom onset to increase the rate of healing and decrease the pain caused by the acute rash. | A | 9–11 |
| Physicians should treat herpes zoster with antiviral medications to decrease the incidence and duration of postherpetic neuralgia. | A | 9–11,14,15 |
| Tricyclic antidepressants and gabapentin (Neurontin) should be used to decrease the pain of postherpetic neuralgia. | A | 17–19 |
| Amitriptyline (Elavil) should be used to decrease the risk of posthepatic neuralgia in older patients. | B | 16 |
| The lidocaine patch (Lidoderm), capsaicin (Zostrix), and opioids should be used to decrease the pain from postherpetic neuralgia. | B | 22–25 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 983 orhttps://www.aafp.org/afpsort.xml.
Clinical Presentation
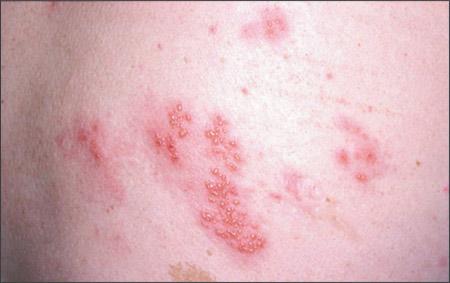
The prodrome of herpes zoster includes fever, malaise, and headache; these may precede the eruption by several days. Preherpetic neuralgia, including burning, itching, or hypersensitivity localized to the affected dermatome, can occur with the prodromal illness. This pain can be severe and may be misdiagnosed as myocardial infarction or renal colic. The skin eruption usually is limited to a single dermatome; the most commonly involved dermatomes are the thoracolumbar region and the face. Lesions may involve more than one dermatome and occasionally may cross the midline. The initial rash is erythematous, with multiple maculopapular lesions that subsequently become vesicular (Figure 1). New crops of vesicles may continue to appear for up to seven days. After a few days, the vesicular fluid becomes cloudy (i.e., pustulation). Finally, the lesion forms a crust that falls off after two to three weeks. The rash may leave scarring and changes in pigmentation.
Figure 1. Herpes zoster lesions.
COMPLICATIONS
The most common complication of herpes zoster is postherpetic neuralgia (i.e., pain along cutaneous nerves persisting more than 30 days after the lesions have healed). The incidence of postherpetic neuralgia increases with age and is uncommon in patients younger than 60 years (Table 13). Herpes zoster lesions can become secondarily infected with staphylococci or streptococci, and cellulitis may develop. Herpes zoster involving the ophthalmic division of the trigeminal nerve can lead to ocular complications and visual loss, so referral to an ophthalmologist is recommended. Other less common complications include motor paresis and encephalitis.
TABLE 1 Incidence of Postherpetic Neuralgia
| Age | Incidence at one month (%) | Incidence at three months (%) | Incidence at one year (%) |
|---|---|---|---|
| Younger than 60 years | 8.8 | 2.0 | 0.6 |
| Older than 60 years | 40.8 | 13.0 | 7.8 |
Information from reference 3.
Diagnosis of Herpes Zoster
The dermatomal pattern of distribution and the appearance of the herpes zoster rash are so distinctive that the diagnosis usually is clear. In cases where the diagnosis is in doubt, polymerase chain reaction (PCR) techniques are the most sensitive and specific diagnostic tests; however, these techniques are not widely available. PCR techniques detect the varicella DNA in fluid taken from the vesicles. Viral culture has a low sensitivity because the herpes virus is labile and difficult to recover from the vesicular fluid. The direct immunofluorescent antigen-staining test has a higher sensitivity and is more rapid than culture; it provides an alternative diagnostic test when PCR is not available (Table 24–6).
TABLE 2 Sensitivity and Specificity of Tests Used to Diagnose Herpes Zoster
Prevention of Herpes Zoster
Eradication of varicella with the vaccine should, in the long run, result in fewer cases of herpes zoster because the incidence of reactivation of the vaccine is lower than that of the virus. Because of the varicella vaccine, fewer patients will develop immunity from contact with infectious cases of the virus, potentially increasing the incidence of reactivation, at least in the short term.7 A double-blind, placebo controlled study8 of varicella vaccine in patients older than 60 years showed a 61 percent reduction in pain and discomfort from herpes zoster, a 51 percent reduction in the incidence of herpes zoster, and a 66.5 percent reduction in the incidence of postherpetic neuralgia. Before a recommendation to vaccinate middle-aged adults is made, future risk of herpes zoster in previously vaccinated adults and the cost-effectiveness of a vaccination program need to be evaluated. Ultimately, when wild-type varicella virus infection decreases to minimal levels, the incidence of herpes zoster will decrease as well.
Management of Acute Herpes Zoster Infection
Treatment of herpes zoster with antiviral medication appears to be more effective than treatment with corticosteroids.
ANTIVIRAL THERAPY
Three antiviral drugs are available for the treatment of herpes zoster: acyclovir (Zovirax), famciclovir (Famvir), and valacyclovir (Valtrex). Acyclovir, in its generic form, is significantly less expensive than famciclovir or valacyclovir (Table 3). Acyclovir accelerates resolution of all pain endpoints, especially in patients older than 50 years.9 Famciclovir, given within 72 hours of the onset of the rash and for seven days, hastens the healing of herpes zoster by one to two days; however, acute pain is diminished only in patients with more than 50 lesions.10 No differences have been found between famciclovir and valacyclovir.11 These medications are safe and well tolerated, with minimal side effects (e.g., headache, nausea). Valacyclovir and famciclovir usually are preferred because they are administered three times daily as opposed to acyclovir, which must be given five times daily.
TABLE 3 Antiviral Medications Used to Treat Herpes Zoster
| Medication | Dosage | Cost* |
|---|---|---|
| Acyclovir (Zovirax) | 800 mg five times daily for seven days | $234 ($45 to $128 for generic) |
| Famciclovir (Famvir) | 500 mg three times daily for seven days | 196 |
| Valacyclovir (Valtrex) | 1,000 mg three times daily for seven days | 207 |
*—Estimated cost to the pharmacist based on average wholesale prices in Red Book. Montvale, N.J.: Medical Economics Data, 2005. Cost to the patient will be higher, depending on prescription filling fee.
There are no data examining the effect of antiviral treatment given more than 72 hours after the onset of the herpes zoster rash. The “50-50-50 rule” can be used as a treatment guide: 50 hours or less since onset of lesions, 50 years or older, and 50 or more lesions.
STEROID THERAPY
Two large randomized, double-blind, placebo controlled studies12,13 evaluated 21 days of corticosteroids for the management of herpes zoster. One study12 found that patients treated with corticosteroids and acyclovir had a greater reduction in pain on days 7 and 14, but at day 21 there was no difference. The second study13 found that corticosteroids combined with acyclovir did not affect cutaneous healing but did result in a significant benefit in quality of life at day 30, including less time returning to normal activity and uninterrupted sleep. Many patients with chronic diseases such as diabetes, renal insufficiency, and hypertension were excluded from this study, limiting its applicability. Overall, it remains doubtful that the risks associated with steroids warrant these minimal benefits.
Prevention of Postherpetic Neuralgia
No treatment has been shown to prevent postherpetic neuralgia completely, but some treatments may shorten the duration or lessen the severity of symptoms.
ANTIVIRAL THERAPY
A systematic review14 of 42 trials evaluating treatment given at the time of acute herpes zoster concluded that there is marginal evidence that seven to 10 days of acyclovir treatment reduces the incidence of pain at one to three months. The most recent meta-analysis15 of five placebo-controlled trials comparing acyclovir with placebo in the prevention of postherpetic neuralgia reported a number needed to treat (NNT) of 6.3 to reduce the incidence of pain at six months. There is only one trial10 examining the effect of famciclovir on postherpetic neuralgia; it concluded that seven days of famciclovir had no effect on the overall incidence of postherpetic neuralgia but did reduce its duration. To prevent pain at six months, the NNT was 11.10 Another trial7 comparing seven days of valacyclovir with famciclovir showed equivalence in reducing the duration of postherpetic neuralgia.
STEROID THERAPY
Two double-blind, randomized, controlled trials12,13 concluded that corticosteroids given for 21 days did not prevent postherpetic neuralgia.
TRICYCLIC ANTIDEPRESSANTS
One randomized trial16 of patients older than 60 years who were diagnosed with herpes zoster compared 25 mg of amitriptyline (Elavil) initiated within 48 hours of the rash onset and continued for 90 days with placebo. The amitriptyline group showed a 50 percent decrease in pain prevalence at six months with an NNT of 5.16
Management of Postherpetic Neuralgia
TRICYCLIC ANTIDEPRESSANTS
A systematic review17 comparing amitriptyline or desipramine (Norpramin) with placebo in relieving pain showed a statistically significant benefit to using a tricyclic antidepressant over placebo. In the studies reviewed, the dosages of tricyclic antidepressants started at 12.5 to 25 mg daily and increased by 12.5 to 25 mg every three to five days, to a maximum of 250 mg daily. The range of effective dosages for desipramine was 12.5 to 250 mg daily, with the average effective dosage being 167 mg daily. The range of effective dosages for amitriptyline was 12.5 to 150 mg daily with the average dosage being 70 mg daily. The most common side effects were dry mouth, constipation, and sedation, although they were not a major problem at the relatively low doses needed for effect. There was no significant difference in benefits when maprotiline (Ludiomil) was compared with amitriptyline, but there was a higher incidence of side effects with maprotiline.
ANTICONVULSANTS
Two randomized controlled trials18,19 support the use of gabapentin (Neurontin) to treat postherpetic neuralgia with an NNT of 3 in one trial and 5 in the other. The dosage was started at 300 mg daily and titrated over two weeks to a maximum of 3,600 mg daily or intolerable side effects (e.g., sedation, dizziness). In the study using smaller doses,19 1,800 mg daily was as effective and better tolerated than 2,400 mg daily.
OPIOIDS
When oxycodone (Oxycontin) was compared with placebo, moderate or better pain relief was achieved in 58 percent of patients taking oxycodone versus 18 percent of patients taking placebo.20 The dosage was titrated from 10 mg twice daily to effect or a maximum of 60 mg twice daily or intolerable side effects. Common side effects included constipation, sedation, and nausea.20 Another study21 showed that morphine (MS Contin) and nortriptyline (Pamelor) provided better and equivalent pain relief, respectively, than placebo (decrease in baseline pain by 33 percent). Morphine and nortriptyline had an NNT of 3 and 4, respectively. Side effects for opioids included nausea, constipation, decreased appetite, and sedation.21
LIDOCAINE PATCH
One randomized study22 supports using a 5-percent lidocaine patch (Lidoderm) for postherpetic neuralgia.
TOPICAL CAPSAICIN
Two published studies23,24 evaluated topical capsaicin cream (Zostrix) and reported a statistically significant improvement in the number of patients experiencing pain relief from capsaicin cream verus placebo, with an NNT of 2 in one study and 3 in the other. Burning or stinging was the main side effect; this diminished after the first week with regular application of the cream. Both studies used 0.075 percent cream, which needed to be applied four times daily.23,24 One unpublished study25 did not show a benefit with capsaicin, but a lower strength cream (0.025 percent) was used for a shorter duration.
INTRATHECAL METHYLPREDNISOLONE
One randomized trial26 reported excellent results using intrathecal methylprednisolone for persistent postherpetic neuralgia. Only patients who have postherpetic neuralgia unresponsive to oral and topical therapy should be considered for intrathecal methylprednisolone.

