
Am Fam Physician. 2005;72(8):1569-1571
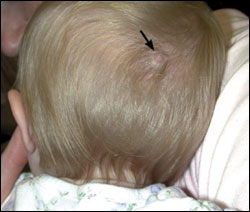
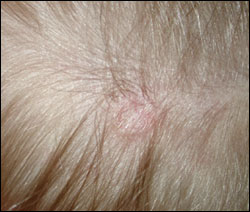
Shortly after an uncomplicated pregnancy and birth, a term female newborn was noted to have a midline lesion on the posterior aspect of her scalp (Figure 1). The lesion was hairless, measuring 0.5 cm in diameter, with a slightly denuded appearance and a rolled edge (Figure 2). The child also had an associated “stork bite” skin change surrounding the lesion. The lesion remained unchanged at subsequent well-child visits. The hair at the immediate periphery of the lesion seemed to grow much faster than the rest of the child’s hair, although the lesion remained hairless. The hair surrounding the lesion had a coarser, kinked texture compared with the remainder of the child’s hair. The child was neurodevelopmentally normal.
Question
Discussion
Aplasia cutis congenita presents as a well-demarcated, noninflammatory, circular or oval blister or eroded region, usually at the scalp vertex just lateral to the midline, although other areas of the body also may be involved. Although aplasia cutis congenita often appears as a solitary lesion (70 percent), the condition may present as multiple lesions, typically 1 to 2 cm in diameter.3 Solitary lesions range in size from 0.5 to 10 cm. The appearance varies depending on when the lesion occurred in utero. Lesions formed early in gestation might heal before delivery. Such a lesion may appear as an atrophic, fibrotic, alopecic scar. A more recent lesion, however, would present as an ulcer. The depth varies: more superficial defects have minimal scarring and hair loss, whereas others penetrate the deep dermis and subcutaneous tissue, reaching the skull and dura.1 Distorted hair growth surrounding a scalp lesion represents a “hair collar sign.” This can be a marker for underlying defects.3 Neuroimaging with ultrasonography often is recommended for further evaluation of an intracranial component.
Most patients with aplasia cutis congenita have no other abnormalities, although the condition may be associated with congenital malformations involving the cardiovascular, gastrointestinal, genitourinary, and central nervous systems. Larger lesions are more likely to be associated with other defects. Lesions with findings such as vascular flushing, tethering (which may be a sign of a dural attachment), or abnormal surrounding hair may signal further abnormalities and warrant evaluation.1,4
The etiology of this disease is unclear and appears to be multifactorial; teratogens, genetic factors, trauma, and compromised skin perfusion each seem to play a role.1 There are case reports of aplasia cutis congenita in infants of mothers receiving methimazole (Tapazole), although causation has not been established. Familial occurrences also are reported.5
There is no consensus concerning the treatment of aplasia cutis congenita. Management depends on the size of the defect and the physical condition of the child. Complications can include meningitis, hemorrhage, and local infection; however, small ulcers typically heal with formation of a hairless scar over several weeks, and bony defects tend to close spontaneously within the first year. A conservative approach often is adopted because of the self-limited course.1 Multiple or large ulcers require excision and surgical closure because of the risk of hemorrhage and infection.1
Langerhans cell histiocytosis (formerly histiocytosis X) is a proliferative disorder of Langerhans cells that can occur in many organ systems. The scalp often is affected in adults and infants. The lesions usually are multiple, erythematous, scaling patches that can, at times, resemble seborrheic dermatitis.6
Sebaceous nevus is a congenital lesion made up of excessive sebaceous glands and malformed hair follicles. Lesions typically are hairless and yellowish and often occur on the scalp or face. This lesion is rare, affecting only 0.3 percent of newborns. Sebaceous nevus lesions carry a 20 percent lifetime risk of cancerous transformation.3
Neonatal herpes infection may present as a scalp ulceration or erosion. The lesions usually are erythematous vesicles before ulceration and become crusted as they progress. Lesions often are multiple. There may be a history of maternal genital herpes infection, and the infant is often ill with signs of sepsis.1,3
Transient bullous dermolysis of the newborn is a rare, benign, blistering disease that presents at or near birth and resolves during the first few months of life.6 It is a form of dystrophic epidermolysis bullosa. Epidermolysis bullosa is a group of rare, inherited bullous disorders characterized by blister formation in the epidermal layer secondary to mechanical trauma. Blisters usually are precipitated by an identifiable traumatic event.1
Focal dermal hypoplasia is an uncommon genetic disorder in females that is characterized by distinct skin abnormalities and multisystem defects. Findings typically are apparent at birth. Skin lesions are prominent on the legs, forearms, and cheeks. They often appear as accumulations of fat and may be associated with raspberry-like papillomas and telangiectasias.1
| Condition | Characteristics |
|---|---|
| Langerhans cell histiocytosis | Scaling, erythematous patches; other organ systems may be involved; lesions usually multiple |
| Sebaceous nevus | Yellow, waxy appearance; usually on face or scalp; proliferation during puberty |
| Neonatal herpes infection | Erythematous, vesicular lesions; progression to ulcers, then become crusted; lesions usually multiple; associated with ill infant |
| Aplasia cutis congenita | Defect in dermal layer; erosion or may have thin skin layer if in utero; may extend to deeper structures (bone, dura); usually solitary |
| Focal dermal hypoplasia | Occurs only in females; multisystemic; fat accumulations, raspberry-like papillomas, telangiectasias |
| Transient bullous dermolysis of the newborn | Blisters on surfaces of subject precipitated by trauma; benign and self-limited |