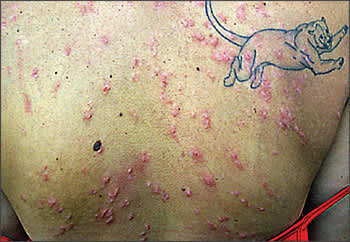
A 23-year-old woman presented after returning from a beach vacation in Thailand. Before leaving Thailand, she developed a severe, widespread, pruritic eruption. On examination, she had erythematous, edematous, infiltrative papules and papulopustules over her entire body, most densely concentrated on her buttocks and back (see accompanying figure). Skin biopsy showed an intraepidermal pustule rich in eosinophils and necrotic keratinocytes and an epidermal and upper dermal chronic infiltrate with many eosinophils. There were no traces of parasites.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Bacterial folliculitis.
B. Gnathostomiasis (Gnathostoma spinigerum).
C. Larva currens (Strongyloides stercoralis).
D. Scabies.
E. Hookworm folliculitis.
Discussion
The answer is E: hookworm folliculitis. This is an example of the follicular type of cutaneous larva migrans. Folliculitis is an uncommon clinical manifestation of cutaneous larva migrans,1,2 first described in 1991.3 The clue to the diagnosis is the extreme, unbearable pruritus that worsens at night in patients who develop a “folliculitis” after visiting an endemic area.
Cutaneous larva migrans is the most common tropically acquired dermatosis.4 It is known as a “creeping eruption,” a distinctive pruritic, linear, cutaneous eruption that results from penetration of the skin by the nematode larvae, most commonly dog and cat hookworms (Ancylostoma caninum and Ancylostoma braziliense). The clinical presentation is usually a localized, intensely pruritic, serpiginous, thin, raised, erythematous, tunnel-like lesion on the feet and buttocks. The primary treatment options are ivermectin (Mectizan) and albendazole (Valbazen).
Travelers who walk around barefoot or who sit or lie on contaminated sand are at risk. The increased popularity of rapid international air travel to tropical areas has produced a rise in imported diseases formerly restricted to the equatorial zones. This increases the chance that Western physicians will see these “exotic” conditions.
In contrast to follicular larva migrans, bacterial folliculitis is not as intensely pruritic and will not interfere with sleep. Gnathostomiasis (G. spinigerum) and larva currens (S. stercoralis) can mimic the common form of cutaneous larva migrans; however, both infections are migratory and do not have a follicular form.
Scabies also is characterized by pruritic papulonodular lesions and increasing pruritus at night, and it should be considered as the main differential diagnosis. Patients with scabies, however, have fewer lesions (usually fewer than 20) than in the described cases of follicular cutaneous larva migrans.
Selected Differential Diagnosis of Widespread Pruritic Papulopustules
| Condition | Characteristics |
|---|---|
| Bacterial folliculitis | Small, dome-shaped, erythematous, inflamed papules and papulopustules in follicular arrangement |
| Gnathostomiasis (Gnathostoma spinigerum) | Intermittent, migratory swelling and indurated, erythematous, urticarial plaques that move about 1 cm per hour |
| Larva currens (Strongyloides stercoralis) | Intensely itchy wheal in a serpiginous line that progresses rapidly (5 to 15 cm per hour) |
| Scabies | Pruritic papular or linear lesions in sites of predilection: finger webs, wrists, antecubital fossae, axillae, areolae, around the umbilicus, lower abdomen, genital area; usually fewer than 20 lesions |
| Hookworm folliculitis | Erythematous, edematous, infiltrative papules and papulopustules; endemic exposure |

