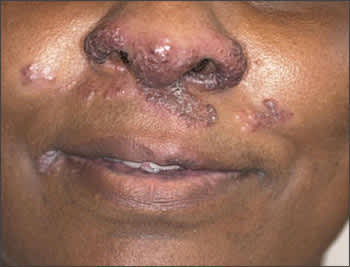
A 50-year-old woman came to her physician’s office with violaceous, smooth, shiny facial lesions (see accompanying figure). The lesions had been present for many years and recently had increased significantly in size. The patient had been diagnosed with sarcoidosis 10 years earlier and was being treated currently for pulmonary involvement. She denied any trauma to the nose, and results of a purified protein derivative test were negative.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Discoid lupus erythematosus.
B. Lupus pernio.
C. Lupus vulgaris.
D. Lupus profundus.
E. Adenoma sebaceum.
Discussion
The answer is B: lupus pernio. Although erythema nodosum is the most common nonspecific skin lesion in sarcoidosis, lupus pernio of the nose is the most characteristic cutaneous lesion.1,2 The term “lupus” originally described many lesions with an eroded or gnawed appearance and, thus, is not always related to systemic lupus erythematosus.3 Lupus pernio lesions are violaceous, smooth, shiny papules and plaques located on the head and neck, particularly the nose, cheeks, lips, forehead, and ears. This condition occurs more often in black women in their 30s and 40s and rarely resolves spontaneously. It can be cosmetically disfiguring.4 Additionally, extensive involvement of the nasal cavity and the maxillary sinuses may lead to nasal obstruction.5 Fibrotic pulmonary complications, granuloma formations in bones, and chronic ocular lesions also are common.
Controlling lupus pernio involves managing the underlying sarcoidosis, and no specific therapy for cutaneous sarcoidosis is available. Dermatology consultation may be helpful. Nonoral therapies for lupus pernio have included highly potent topical corticosteroids, topical corticosteroids with hydrocolloid occlusive dressings, intralesional triamcinolone (Aristocort), intralesional chloroquine (Aralen Phosphate), and carbon dioxide1,2,6 or pulsed-dye laser.4 Surgical approaches have included dermabrasion, excision with grafting for ulcerative sarcoidosis, and plastic surgery.
Systemic therapies may be used to manage generalized cutaneous involvement, disfiguring lesions, and cases refractory to localized nonoral therapies. Agents include prednisone, hydroxychloroquine (Plaquenil), chloroquine, methotrexate, allopurinol (Zyloprim), thalidomide (Thalomid), isotretinoin (Accutane), psoralen plus ultraviolet A therapy, N-(3,4-dimethoxycinnamoyl) anthranilic acid (tranilast [Rizaben]), melatonin, and tetracyclines.2,6,7 Cytotoxic agents such as azathioprine (Imuran) and cyclophosphamide (Cytoxan) also may be used to manage cutaneous sarcoidosis.
Discoid lupus erythematosus is a chronic, scarring skin atrophy associated with photosensitivity. Typical lesions begin as erythematous papules or plaques with scaling that becomes thick and adherent. Discoid lupus erythematosus may occur in patients with systemic lupus erythematosus, but less than 5 percent of patients with discoid lupus erythematosus progress to systemic lupus erythematosus. Patients with discoid lupus erythematosus rarely fulfill the criteria used to classify systemic lupus erythematosus, and serologic abnormalities are uncommon.
Lupus vulgaris, the most common form of cutaneous tuberculosis, is a solitary plaque formed by reddish-brown papules. A brownish yellow or “apple jelly” color may be seen in the lesion when blanched. The presence of acid-fast bacilli within the plaque is rare. If the underlying tuberculosis is untreated, the lesions heal with extensive fibrosis and atrophic scaring.
Lupus profundus, or lupus panniculitis, is a rare variant of lupus erythematosus. It involves the subcutaneous adipose tissue, typically presenting as nontender nodules over the face, arms, and buttocks. It occurs in 2 percent of patients with systemic lupus erythematosus but may occur without the presence of systemic involvement.
Adenoma sebaceum is a skin manifestation of tuberous sclerosis. Lesions arise in childhood or adolescence. These angiofibromas usually begin as pink macules and evolve into papules. They typically appear on the face, especially in the areas of the nasolabial folds, cheeks, and chin.8
Selected Differential Diagnosis of Facial Papules and Plaques
| Condition | Characteristics |
|---|---|
| Discoid lupus erythematosus | Erythematous papules or plaques with scaling; chronic scarring atrophy |
| Lupus pernio | Cutaneous sarcoidosis; violaceous, smooth, shiny papules and plaques |
| Lupus vulgaris | Cutaneous tuberculosis; solitary plaque formed by reddish-brown papules; “apple jelly” color when blanched |
| Lupus profundus | Lupus erythematosus; nontender nodules on face, buttocks, and arms |
| Adenoma sebaceum | Tuberous sclerosis; pink macules evolve into papules; may form plaques |

