Musculoskeletal pain can be difficult for children to characterize. Primary care physicians must determine whether the pain may be caused by a systemic disease. Change in activity, constitutional symptoms such as fevers and fatigue, or abnormal examination findings without obvious etiology should raise suspicion for rheumatic disease. A complete physical examination should be performed to look for extra-articular signs of rheumatic disease, focusing on but not limited to the affected areas. A logical and consistent approach to diagnosis is recommended, with judicious use of laboratory and radiologic testing. Complete blood count and erythrocyte sedimentation rate measurement are useful if rheumatic disease is suspected. Other rheumatologic tests (e.g., antinuclear antibody) have a low pretest probability in the primary care setting and must be interpreted cautiously. Plain radiography can exclude fractures or malignancy; computed tomography and magnetic resonance imaging are more sensitive in detecting joint inflammation. Family physicians should refer children to a subspecialist when the diagnosis is in question or subspecialty treatment is required. Part II of this series discusses rheumatic diseases that present primarily with musculoskeletal pain in children, including juvenile arthritis, the spondyloarthropathies, acute rheumatic fever, Henoch-Schönlein purpura, and systemic lupus erythematosus.
Musculoskeletal pain during childhood is common; in population surveys, 16 percent of school-age children reported limb pain.1 Musculoskeletal pain can be difficult for children to characterize and can cause children and parents great anxiety. Although the cause of acute musculoskeletal pain in children usually is obvious, the cause of chronic musculoskeletal pain or pain that has associated systemic symptoms can be more difficult to determine. The term “growing pains” may be applied mistakenly to children who have a serious rheumatic or malignant disease. Children who have unusual symptoms or abnormal findings on physical examination should be evaluated carefully.
A logical and consistent approach to diagnosis is necessary to treat the pain and its cause effectively and to avoid the long-term complications of untreated disease. This article, part I of a two-part series, outlines a primary care approach to evaluating and diagnosing the child with musculoskeletal pain who may have a rheumatic illness. Part II2 discusses common rheumatic causes of musculoskeletal pain in children, as well as treatment and referral recommendations. Nonrheumatic causes of musculoskeletal pain are much more common than rheumatic causes. An exhaustive list of the many possible causes of musculoskeletal pain in children is beyond the scope of this series but should be considered when screening for underlying disease in children with joint complaints.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| CBC and ESR tests are recommended for children with chronic joint pain to help exclude infection and malignancy. | C | 16 |
| The ANA and rheumatoid factor tests have a low positive predictive value in the primary care setting and are not recommended for routine use in the initial diagnosis of joint pain. | C | 23,25,26,28,30 |
| Plain radiography should be the first radiologic study used. However, radiographs are typically more useful in excluding certain conditions (e.g., malignancy) than in making a positive diagnosis of arthritis. | C | 20,33 |
CBC = complete blood count; ESR = erythrocyte sedimentation rate; ANA = antinuclear antibody.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 17 orhttps://www.aafp.org/afpsort.xml.
Approach to the Child with Musculoskeletal Pain
A suggested approach to the child with musculoskeletal pain is provided in Figure 1. Key characteristics for distinguishing between benign and serious causes of musculoskeletal pain are listed in Table 1.3
Figure 1. Evaluation and Diagnosis of the Child with Musculoskeletal Pain
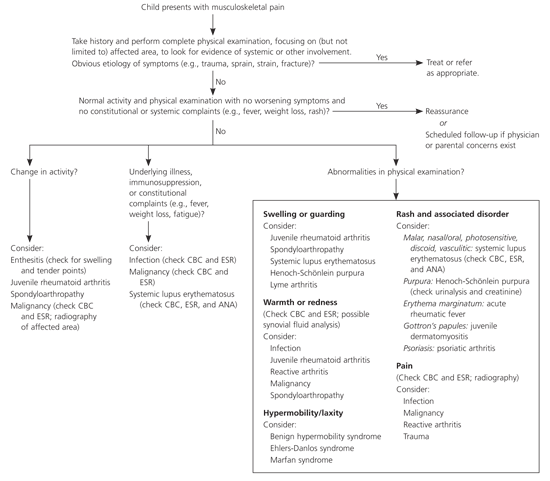
An approach to the child with musculoskeletal pain. (CBC = complete blood count; ESR = erythrocyte sedimentation rate; ANA = antinuclear antibodies.)
HISTORICAL FACTORS
Musculoskeletal disorders have multiple etiologies,4 and the history and physical examination greatly aid in narrowing the differential diagnosis.5,6 For example, mechanical joint pain is more likely to be acute, to involve point tenderness, and to be worse at the end of the day or with overuse, whereas inflammatory joint pain generally is less well defined or described as “stiff,” is worse in the mornings,7 and feels better with use.
The family physician must first determine the specific location of the pain. Pain localized to areas other than the joint may be related to connective tissue or muscle involvement.8 The possibility of referred pain, such as hip disease with associated groin or knee pain, should be considered. The joint distribution and the number of joints involved will help organize the evaluation.9,10 For example, arthritis in only one joint may be caused by pauciarticular juvenile arthritis, septic arthritis, or a seronegative spondyloarthropathy. Inflammatory diseases such as polyarticular juvenile rheumatoid arthritis, mixed connective tissue disease, and systemic lupus erythematosus usually cause symmetric arthritis affecting multiple joints.5,11
The next step is to determine whether the process is inflammatory. Prolonged morning stiffness, swelling, and constitutional symptoms (e.g., fever, weight loss, fatigue) suggest inflammatory processes such as arthritis or vasculitis. Other historical descriptors include alleviating and aggravating factors and frequency and duration of pain. Rapid onset of pain suggests trauma, sepsis, hemarthrosis, or malignancy. Onset of pain over several days suggests infectious or reactive arthritis. The physician should be concerned if a child limits daily activities.
Finally, the physician should search for extra-articular symptoms that would be helpful in making the diagnosis. Characteristic rashes accompany several rheumatic causes of musculoskeletal pain: parents may notice the malar rash of systemic lupus erythematosus or the heliotrope rash of juvenile dermatomyositis.8,12–14 Classic clinical scenarios may further indicate a systemic disease: the arthritis and rash of Henoch-Schönlein purpura typically follow an upper respiratory tract infection, whereas reactive arthritis typically follows a genitourinary or gastrointestinal tract infection. A painful red eye may accompany the spondyloarthropathies.
PHYSICAL EXAMINATION
A complete physical examination may disclose additional clinical signs that point toward a diagnosis. A general appearance of well-being is reassuring regarding multiorgan involvement; however, a child with only one or two joints affected by arthritis may appear well overall. Lymphadenopathy or hepatosplenomegaly can be associated with malignancy and inflammatory diseases such as systemic lupus erythematosus. Rashes are characteristic in patients with acute rheumatic fever, Henoch-Schönlein purpura, and the systemic form of juvenile arthritis. Gottron’s papules—erythematous plaques overlying extensor surfaces of knuckles—are pathognomonic for juvenile dermatomyositis.8,14,15 A comprehensive examination will help exclude infectious, traumatic, and oncologic etiologies of musculoskeletal complaints.16,17
The musculoskeletal examination may demonstrate arthritis or myositis. Specific findings of arthritis include warmth, swelling, loss of range of motion, and guarding of the joint. Although these are classic inflammatory signs, they may be minimal or difficult to detect even in juvenile arthritis. Muscle mass and strength also should be evaluated. Long-standing arthritis may have associated bony enlargement or muscle atrophy.18,19 Proximal muscle weakness is present in juvenile dermatomyositis and can be subtle without performing formal strength testing of axial muscles. Focal tenderness or abnormalities may suggest orthopedic or oncologic20 etiologies rather than inflammatory causes.
FOLLOW-UP
Many rheumatic clinical entities tend to develop over weeks or months (Table 1).3 Close follow-up to determine the child’s clinical course therefore is recommended. Resolution of symptoms and continued absence of worrisome features can reassure the child and family that a chronic inflammatory disease is not present; conversely, additional signs and symptoms noted at a follow-up visit may direct further evaluation or referrals, if warranted.
Adjunctive Tests
Laboratory tests and radiologic studies may help to support a diagnosis in a child with a high likelihood of inflammatory musculoskeletal illness and may exclude worrisome diagnoses such as infection and malignancy. The need for adjunctive tests is determined by the child’s clinical features. Selected tests used in the diagnosis of musculoskeletal pain are listed in Table 2.4,13,16,17,20–34
TABLE 2 Selected Adjunctive Laboratory and Radiologic Tests for Diagnosing Musculoskeletal Pain in Children
| Test* | Condition associated with positive or abnormal results | Diagnostic capabilities | When test should be conducted |
|---|---|---|---|
| Laboratory | |||
| CBC | Initial evaluation of chronic joint pain or clinical suspicion of SLE to check for cytopenias | ||
| ESR |
| Initial evaluation of chronic joint pain or pain out of proportion to clinical findings | |
| ANA |
| In a patient with juvenile RA to recommend frequency of iritis screening or when high clinical suspicion for SLE (see Table 3) | |
| Rheumatoid factor |
| To assist in diagnosis of juvenile RA, SLE, or mixed connective tissue disease, usually after referral | |
| Anti–double-stranded DNA |
|
| To quantify disease activity in patients with confirmed diagnosis |
| HLA-B27 genotype |
| To classify arthritis, usually after referral. | |
| Consider use if family history of psoriasis, inflammatory bowel disease, arthritis and back pain, or spondyloarthropathy | |||
| Radiology | |||
| Plain radiography |
| Initial evaluation of patient with significant joint or bone pain | |
| MRI, CT |
| When joint examination is equivocal or difficult (e.g., in temporomandibular or hip joints) | |
| Echocardiography |
|
| In patients with fever, rash, and arthritis34 |
| In patients who have SLE with cardiac symptoms | |||
*—Tests are listed by probable frequency of use.
CBC = complete blood count; SLE = systemic lupus erythematosus; RA = rheumatoid arthritis; ESR = erythrocyte sedimentation rate; ANA = antinuclear antibody; HLA = human leukocyte antigen; MRI = magnetic resonance imaging; CT = computed tomography.
LABORATORY TESTS
Rheumatologic laboratory tests can confirm a clinically suspected diagnosis for the cause of musculoskeletal pain in children but are not diagnostic in themselves. If a serious rheumatic cause is suspected, the family physician should use laboratory tests judiciously and interpret them in the context of the child’s clinical presentation. History and physical examination findings help determine whether laboratory tests are needed. A normal complete blood count (CBC) and erythrocyte sedimentation rate (ESR) and a negative antinuclear antibody (ANA) test result reduces the likelihood of infection, cancer, and systemic lupus erythematosus (Table 24,13,16,17,20–34).13,16,17 The ANA must be interpreted according to the patient’s pretest probability of rheumatic disease. In the primary care setting this usually is low, so most positive results are false-positive (Table 3).35
TABLE 3 Interpreting the ANA Test in Primary Care and Specialty Settings When Symptoms Suggest SLE
| ANA titer | Positive likelihood ratio* | Likelihood of disease (%) | |
|---|---|---|---|
| Primary care setting† | Specialty setting‡ | ||
| > 1:1280 | 9.9 | 17.0 | 81 |
| 1:640 | 2.2 | 4.2 | 49 |
| 1:320 | 1.1 | 2.1 | 32 |
| 1:160 | 0.8 | 1.6 | 26 |
| 1:80 | 0.8 | 1.6 | 26 |
| 1:40 | 0.7 | 1.4 | 23 |
| 1:20 | 0.4 | 0.8 | 15 |
ANA = antinuclear antibody; SLE = systemic lupus erythematosus.
*—Greater than 1 indicates an increased likelihood of disease, and less than 1 indicates a decreased likelihood.
†—Estimated 2 percent pretest probability of SLE.
‡—Estimated 30 percent pretest probability of SLE.
Information from reference 35.
The use of an arthritis or rheumatoid panel is not recommended because this can lead to false-positive results, unnecessary expense, and patient worry; each test is best used in the appropriate clinical setting. Some laboratory tests, such as the human leukocyte antigen B27 (HLA-B27) and rheumatoid factor, may help determine prognosis in rheumatic disease but cannot be used to make a diagnosis and therefore are most useful in the specialist setting. The tests most useful in the primary care setting include the CBC (to detect inflammation or cytopenias), ESR (a sensitive but not specific marker of inflammation), and ANA (with clinical suspicion for systemic lupus erythematosus).
RADIOLOGIC STUDIES
A worrisome history, atypical or systemic symptoms, or abnormal physical findings in a child with musculoskeletal pain warrant use of radiologic studies. Normal plain radiographs can be reassuring regarding fracture and some malignancies, such as bony lesions.20,32,36 However, certain cancers (e.g., leukemia, lymphoma) do not have characteristic radiographic abnormalities, and most children with malignancy therefore will not have abnormal radiographs.17,22,32
Various modalities may help identify the extent of musculoskeletal disease or exclude other causes of joint complaints. Magnetic resonance imaging (MRI) has the greatest sensitivity for inflammatory processes20,37 but is time-consuming and costly and should be used judiciously. Computed tomography or MRI may be helpful to characterize the anatomy when the location of the affected joint makes physical examination difficult (e.g., in the hip or temporomandibular joints).37,38 Echocardiography is useful in acute rheumatic fever to detect carditis and valvular lesions34 and in systemic onset juvenile rheumatoid arthritis or systemic lupus erythematosus to detect pericarditis.
Other Considerations
Several conditions are useful to note because they illustrate how a thorough history and detailed physical examination with adjunctive laboratory and radiologic tests can identify the diagnosis. These are malignancy, benign nocturnal limb pains, and benign hypermobility syndrome.
MALIGNANCY
Physicians must be alert to the possibility of malignancy as the cause of musculoskeletal pain in children. Cancer occurs in about one in 6,400 children annually, and acute lymphoblastic leukemia, the most common leukemia, has an annual incidence of one to five per 100,000.39 Patients with other types of cancers also may present with nonspecific complaints such as fever and bone or joint pain.40 Additionally, malignant musculoskeletal tumors account for 5 to 10 percent of malignant neoplasms of childhood; the most common of these lesions are osteosarcoma, Ewing’s sarcoma, and rhabdomyosarcoma.41
Cancer should be considered in a child who has pain out of proportion to clinical findings, or suggestive laboratory or radiologic test results. Pain is the most common presenting symptom of malignancy,16,20 with swelling and reactive arthritis over the involved bone occurring a few weeks or months after onset of pain. Children with fevers, weight loss, and abnormalities on laboratory evaluation may already have metastases. Tumors may be indicated on plain radiographs by abnormalities such as periosteal elevation, cortical destruction with a “moth-eaten” appearance, and an apparent soft tissue mass.32 A bone scan may localize involved areas, and computed tomography or MRI may further delineate the lesion. Steroids are contraindicated until malignancy has been excluded in children who appear ill and have joint pain or swelling.
BENIGN NOCTURNAL LIMB PAINS OF CHILDHOOD
Benign nocturnal limb pains of childhood (formerly known as “growing pains”) are cramping pains of the thigh, shin, and calf; they affect approximately 35 percent of children four to six years of age, although they may occur up to age 19.41 The exact pathophysiology of the pain is unknown: it is not associated with the pubertal growth spurt but theoretically may be associated with growth in general.42 The pain typically occurs in the evening or at night, may awaken the child from sleep, and disappears by morning. Benign nocturnal limb pains are not associated with a limp.
The classic clinical presentation in the absence of other inflammatory or chronic signs and symptoms should reinforce the benign nature of this entity. Physical examination of the child is normal. No further diagnostic testing is necessary in the absence of worrisome complaints or anatomic abnormalities. Parents should be reassured that there are no long-term sequelae.
BENIGN HYPERMOBILITY SYNDROME
Benign hypermobility syndrome occurs typically in young girls before or during adolescence. Patients with this condition present with musculoskeletal pain associated with generalized hypermobility of joints but no associated congenital syndrome. The prevalence of this condition is estimated to range from 8 to 20 percent.1,43 Connective tissue diseases such as Marfan syndrome and Ehlers-Danlos syndrome should be considered. Various criteria for hypermobility exist,1 including evaluation of mobility of the thumb onto the forearm; degree of hyperextension of the metacarpals, elbows, and knees; and the ability to place the palms on the floor with knees straight.
Hypermobility is diagnosed with reassuring history and specific physical examination findings. Close follow-up and review of the child’s complaints and physical examination findings usually will direct further referral or reassurance. Children with hypermobility syndrome should be reassured of the benign nature of their condition. If symptoms are significant enough to interfere with activities, the child may need to alter physical activity temporarily or receive formal physical therapy. Prolonged pain symptoms should prompt review of any applicable athletic program and evaluation for other diagnoses.

