Clinical Question
What is the predicted prognosis for a patient with end-stage liver disease?
Evidence Summary
Two scoring systems are widely used to predict prognosis in patients with end-stage liver disease: the Model for End-Stage Liver Disease (MELD)1 and the Child-Turcotte-Pugh (CTP) score.2,3 The MELD has had several iterations; the first included serum creatinine and bilirubin levels, International Normalized Ratio (INR), and cause of cirrhosis (alcoholic or cholestatic versus hepatitis or other causes). A modification of the MELD that prioritized patients on transplant lists eliminated the cause of cirrhosis. The United Network for Organ Sharing modification is the most current version of the MELD and is the most widely used score for predicting prognosis in patients with end-stage liver disease. The CTP score includes bilirubin and serum albumin levels, INR, and presence or absence of ascites and encephalopathy.
A German study compared the MELD, the CTP score, and the Emory score in predicting the prognosis of 162 patients with end-stage liver disease who were undergoing transjugular intrahepatic portosystemic shunting (TIPS).4 The study used the version of the MELD that included creatinine, bilirubin, INR, and cause of cirrhosis. The mean age of patients was 57 years, about two thirds were men, and most had alcoholic cirrhosis. The accuracy of each score was measured using the concordance-statistic (c-statistic): 1 was a score that perfectly predicted the outcome in question, and 0 was a score that failed to predict any outcome correctly. The study showed: (1) the MELD, the CTP score, and the Emory score were similar in accuracy for predicting three-month mortality; (2) the MELD was more accurate than the others for predicting 12-month mortality; and (3) the MELD and the CTP score were more accurate than the Emory score for predicting 36-month mortality.4 A study including 140 patients undergoing TIPS showed that the MELD was more accurate than the CTP score for predicting three-month mortality.5
A systematic review identified nine studies comparing the MELD with the CTP score: five of these studies included patients with end-stage liver disease undergoing TIPS, and four included a broader population of patients with cirrhosis.6 The MELD was similar to the CTP score in accuracy (measured by the c-statistic) in all studies except one, which showed that the MELD was superior for predicting three-month mortality.6
A prospective validation of the MELD reported three-month prognoses in different populations: ambulatory patients with noncholestatic liver disease largely caused by viral hepatitis; ambulatory patients with primary biliary cirrhosis; and hospitalized patients with cirrhosis (Table 1).7 This validation study used the older version of the MELD, which added 6.4 points to the score if a patient did not have cholestatic or alcoholic liver failure. Figure 1 is a tool for calculating the MELD score.6 Electronic calculators for the MELD and its pediatric counterpart are available at http://www.unos.org/resources/meldPeldCalculator.asp.
TABLE 1 Three-Month Mortality Rate Using the Model for End-Stage Liver Disease (MELD)
| MELD score | Number of patients who died at three months/total patients (%) | |||
|---|---|---|---|---|
| Cholestatic or alcoholic liver failure | Hepatitis or other liver failure | Hospitalized patients (n = 282) | Ambulatory noncholestatic patients (n = 491) | Ambulatory patients with primary biliary cirrhosis (n = 326) |
| ≤3 | ≤9 | 6/148 (4) | 5/213 (2) | 3/308 (1) |
| 4 to 13 | 10 to 19 | 28/103 (27) | 14/248 (6) | 2/16 (13) |
| 14 to 23 | 20 to 29 | 16/21 (76) | 15/30 (50) | 0/2 (0) |
| 24 to 33 | 30 to 39 | 5/6 (83) | No data | No data |
| ≥34 | ≥40 | 4/4 (100) | No data | No data |
Information from reference 7.
Figure 1.
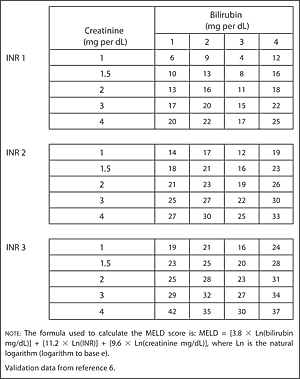
The Model for End-Stage Liver Disease (MELD), United Network for Organ Sharing modification. To calculate the MELD score for your patient: (1) locate the International Normalized Ratio (INR; 1, 2, or 3); (2) locate the serum creatinine level (1, 1.5, 2, 3, or 4); (3) locate the serum bilirubin level (1, 2, 3, or 4). The MELD score is the number at the intersection of these values.
Applying the Evidence
Your patient is hospitalized with cirrhosis caused by hepatitis C. He has an INR of 2, a creatinine level of 1.5 mg per dL, and a bilirubin level of 2 mg per dL. What is his predicted three-month mortality rate?
Answer:
The patient's MELD score is 21, giving him a three-month mortality rate of 76 percent. You begin the process for placing him on the liver transplant list.

