Guideline source: American College of Chest Physicians
Literature search described? Yes
Evidence rating system used? Yes
Published source: Chest, January 2006
Available at: http://www.chestjournal.org/content/vol129/1_suppl/
On a typical day, a family physician will see at least one patient presenting with cough. Cough can be divided into three categories: acute (i.e., lasting less than three weeks), subacute (i.e., lasting three to eight weeks), and chronic (i.e., lasting longer than eight weeks).
Acute Cough
Acute cough is most commonly associated with the common cold, but it also can be associated with life-threatening conditions (e.g., pulmonary embolism, congestive heart failure, pneumonia). The first step in the treatment of acute cough is to determine if the cause of the cough is one of these serious conditions or an acute upper respiratory infection (i.e., common cold), lower respiratory tract infection, or an exacerbation of a preexisting condition (e.g., asthma, bronchiectasis, chronic obstructive pulmonary disease [COPD], or upper airway cough syndrome).
If the cough is due to the common cold, a first-generation antihistamine plus a decongestant should be prescribed. It has been shown that naproxen (Naprosyn) favorably affects cough. Newer-generation nonsedating antihistamines are not effective for reducing cough.
Patients must be symptomatic for a least one week before a diagnosis of bacterial sinusitis is made, because prior to that point bacterial overgrowth is unlikely.
Subacute Cough
The first step in diagnosing subacute cough is to determine whether the cough has followed a respiratory infection. If the cough does not appear to be postinfectious, it should be managed as if it were a chronic cough.
If the cough began with an upper respiratory tract infection and has lingered, it is usually considered a postinfectious cough. It is most probably caused by postnasal drip, upper airway irritation, mucus accumulation, or a manifestation of branchial hyperresponsiveness that may be associated with asthma. Ongoing allergen or irritant exposure, lingering effects of an infection, pneumonia, and acute exacerbation of chronic bronchitis should also be considered.
Patients suspected of being infected with B. pertussis (i.e., whooping cough) should have a nasopharyngeal swab for culture. Patients with confirmed whooping cough should receive macrolide antibiotics and should be isolated for five days beginning on the first day of treatment.
If the cough is not caused by bacterial sinusitis or Bordetella pertussis, treatment with inhaled ipratropium (Atrovent) should be initiated to attenuate the cough. If the cough persists, consider the use of inhaled corticosteroids. If the cough is severe, consider prescribing 30 to 40 mg of prednisone per day for a brief period. When other treatments fail, codeine or dextromethorphan (Delsym) should be considered.
Chronic Cough
Chronic cough is often caused by more than one condition. Figure 1 presents a diagnostic approach to chronic cough. The diagnosis should begin with a medical history, physical examination, and chest radiograph.
Figure 1. Management of Chronic Cough
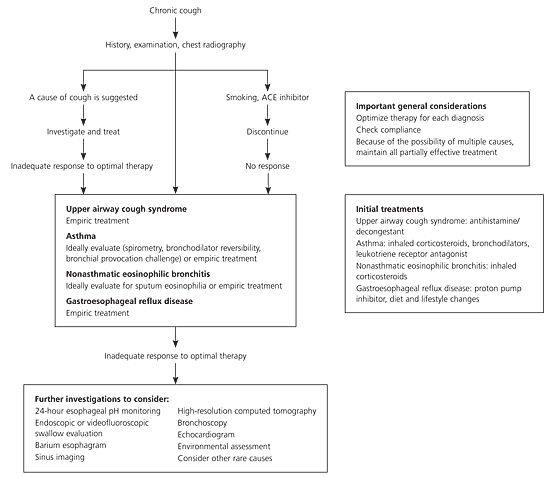
Approach to patients 15 years and older with cough lasting more than eight weeks. (ACE = angiotensin-converting enzyme)
Adapted with permission from Irwin RS, Baumann MH, Bolser DC, Boulet LP, Braman SS, Brightling CE, et al.; for the American College of Chest Physicians. Diagnosis and management of cough: ACCP evidence-based clinical practice guidelines. Chest 2006;129(1 suppl):4S.
HISTORY AND PHYSICAL EXAMINATION
The patient's description of the character or timing of cough is of limited diagnostic value. If the patient is taking an angiotensin-converting enzyme (ACE) inhibitor, treatment should be stopped to determine if the medication is the cause. Cough caused by an ACE inhibitor usually will stop within two weeks of ceasing the medication.
It is also important to determine if the patient is a current smoker. Smoking cessation is almost always successful in eliminating cough within four weeks. If the patient has severe COPD, cough may persist after smoking cessation. If the persistent cough is caused by an exacerbation of COPD, antibiotics or corticosteroids should be considered.
The history is also important for discovering if the patient is from an area where diseases that can cause cough (e.g., tuberculosis) are prevalent; has systemic signs of disease (e.g., fever, sweating, weight loss); or has a history of cancer, tuberculosis, or acquired immune deficiency syndrome.
CHEST RADIOGRAPHY
If the radiographic findings are abnormal, treatment depends on the specific finding. If a mass is found, the patient should receive chest computed tomography (CT), a bronchoscopy or transthoracic fine-needle aspiration, and possibly a positron emission tomography scan.
Findings consistent with congestive heart failure should be followed by a cardiovascular examination and possibly an empiric attempt at diuresis.
Evidence of infection should be followed by attempts to make a microbial diagnosis.
Most patients with chronic cough are otherwise healthy, and in these patients the four most common causes of cough are upper airway cough syndrome, asthma, gastroesophageal reflux disease (GERD), and nonasthmatic eosinophilic bronchitis.
UPPER AIRWAY COUGH SYNDROME–INDUCED CHRONIC COUGH
Patients with chronic cough should first be treated with a first-generation antihistamine/decongestant. If the patient has complete or partial resolution of cough after one to two weeks of antihistamine/decongestant therapy, then it is assumed that upper airway cough syndrome was the cause and therapy should be continued. If the patient has persistent nasal symptoms, it is appropriate to begin a topical nasal steroid. If symptoms still persist, it is an indication for sinus imaging.
Patients with mucosal thickening should be treated for sinusitis. If the patient does not respond to sinusitis therapy, she or he should be referred to an ear, nose, and throat specialist.
If the patient has only partial resolution of cough but no signs of upper airway cough syndrome, then an evaluation for asthma should be done.
ASTHMA-INDUCED CHRONIC COUGH
It has been shown that bronchoprovocation is useful in the evaluation for cough caused by asthma. A positive challenge usually warrants trial treatment for asthma and clinical monitoring. The majority of patients will respond to treatment with inhaled corticosteroids and beta agonists after one week of therapy; it may take up to eight weeks for complete cough resolution.
In patients who do not respond or cannot take inhaled medication, treatment with oral corticosteroids for five to 10 days is an option. Because oral leukotriene inhibitors may be effective, consideration should be given to adding a leukotriene inhibitor before an oral corticosteroid.
If treatment for upper airway cough syndrome and asthma have both failed, nonasthmatic eosinophilic bronchitis should be considered next.
NONASTHMATIC EOSINOPHILIC BRONCHITIS-INDUCED CHRONIC COUGH
To diagnose nonasthmatic eosinophilic bronchitis, an induced-sputum test should be performed to determine if the patient has an increased number of eosinophils. If the patient appears to have nonasthmatic eosinophilic bronchitis, treatment with inhaled corticosteroids is recommended. Cough should resolve within four weeks of therapy.
GERD-INDUCED CHRONIC COUGH
Any patient who responds only partially or not at all to the above therapies should be empirically treated for GERD. Treatment should include an antireflux diet and other lifestyle modification and a proton pump inhibitor. Some patients will respond in as little as two weeks, whereas others may not respond for several months. If there is little or no response to therapy, prokinetic therapy should be considered.
If none of these therapies has been successful for treating the cough, then an additional work-up is necessary, possibly including 24-hour esophageal pH monitoring, upper gastrointestinal tract endoscopy, a barium swallow, or a high-resolution CT scan.
Uncommon Causes of Cough
Uncommon causes of cough include nonacid reflux disease, a swallowing disorder, congestive heart failure, and habit cough. If a complete work-up fails to find a cause for the cough, the remaining diagnosis is unexplained cough. At this point, referral to a cough specialist is appropriate.

