Am Fam Physician. 2007;75(10):1565-1568
Guideline source: American College of Cardiology, American Heart Association, European Society of Cardiology
Literature search described? Yes
Evidence rating system used? Yes
Published source: Journal of the American College of Cardiology, August 15, 2006
Atrial fibrillation is the most common arrhythmia in clinical practice and causes substantial morbidity and mortality. The prevalence of the condition is estimated to be 0.4 to 1 percent, and atrial fibrillation hospitalizations have increased by more than 60 percent over the past two decades. The condition is associated with increased risk of stroke, heart failure, and all-cause mortality. Although atrial fibrillation is commonly associated with structural heart disease, many patients have no detectable heart disease. This guideline assists physicians in clinical decision making by describing options for the diagnosis and management of atrial fibrillation.
Evaluation
The clinical evaluation of patients with suspected atrial fibrillation (Table 1) includes characterizing the arrhythmia pattern as paroxysmal or persistent, determining its cause, and defining associated cardiac and extra-cardiac factors. The evaluation usually can be completed in one outpatient visit, unless the rhythm pattern cannot be specifically documented and additional monitoring is needed.
| Minimal evaluation | |||
| History and physical examination to define: | |||
| Presence and nature of symptoms associated with atrial fibrillation | |||
| Clinical type of atrial fibrillation (e.g., first episode, paroxysmal, persistent, permanent) | |||
| Onset of the first symptomatic attack or date of discovery of atrial fibrillation | |||
| Frequency, duration, precipitating factors, and modes of termination of atrial fibrillation | |||
| Response to pharmacologic agents that have been administered | |||
| Presence of underlying heart disease or other reversible factors (e.g., hyperthyroidism, alcohol consumption) | |||
| Electrocardiography | |||
| To identify: | |||
| Rhythm (verify atrial fibrillation) | |||
| Left ventricular hypertrophy | |||
| P-wave duration and morphology or fibrillatory waves | |||
| Preexcitation | |||
| Bundle branch block | |||
| Prior myocardial infarction | |||
| Other atrial arrhythmias | |||
| To measure R-R, QRS, and Q-T intervals in conjunction with antiarrhythmic drug therapy | |||
| Transthoracic echocardiography to identify: | |||
| Valvular heart disease | |||
| Left and right atrial size | |||
| Left ventricular size and function | |||
| Peak right ventricular pressure (pulmonary hypertension) | |||
| Left ventricular hypertrophy | |||
| Left atrial thrombus (low sensitivity) | |||
| Pericardial disease | |||
| Blood tests (for a first episode of atrial fibrillation, when the ventricular rate is difficult to control) to evaluate thyroid, renal, and hepatic function | |||
| Additional testing (one or several tests may be necessary) | |||
| Six-minute walk test (if the adequacy of rate control is in question) Exercise test (if the adequacy of rate control is in question [permanent atrial fibrillation]) | |||
| To reproduce exercise-induced atrial fibrillation | |||
| To exclude ischemia before treatment of selected patients with a type IC* antiarrhythmic drug | |||
| Holter monitor test or event recording (if diagnosis of the type of arrhythmia is in question) to evaluate rate control | |||
| Transesophageal echocardiography | |||
| To identify left atrial thrombus (in the left atrial appendage) | |||
| To guide cardioversion | |||
| Electrophysiologic study | |||
| To clarify the mechanism of wide-QRS-complex tachycardia | |||
| To identify a predisposing arrhythmia (e.g., atrial flutter, paroxysmal supraventricular tachycardia) | |||
| To seek sites for curative ablation or atrioventricular conduction block/modification | |||
| Chest radiography to evaluate lung parenchyma and pulmonary vasculature, when clinical findings suggest an abnormality | |||
Physical examination findings suggestive of atrial fibrillation include irregular pulse, irregular jugular venous pulsations, variations in the intensity of the first heart sound, or absence of a fourth heart sound heard previously during sinus rhythm. A diagnosis must be confirmed with electrocardiography (ECG). Patients diagnosed with atrial fibrillation should receive two-dimensional Doppler echocardiography to assess left atrial and ventricular dimensions and left ventricular wall thickness and function and to exclude valvular heart disease and pericardial disease. Thyroid, renal, and hepatic functions should be measured during the evaluation.
If necessary, additional testing may include exercise or walking tests, a Holter monitor test or event recording, trans-esophageal echocardiography, and chest radiography.
Prevention of Thromboembolism
Antithrombotic therapy to prevent throm-boembolism is recommended for patients with atrial fibrillation unless the patient does not have heart disease or has contraindications to antithrombotic therapy. ECG may detect risk factors; however, the test's value for stratifying risk is limited because it is unclear whether the absence of abnormalities suggests low risk. Table 2 is a guideline for determining antithrombotic therapy in patients with atrial fibrillation. It is reasonable to regularly reevaluate the need for anticoagulation.
ANTICOAGULATION AGENTS
Therapy should be based on the patient's risk of stroke and bleeding. Patients with atrial fibrillation and a high risk of stroke who do not have a mechanical heart valve should receive a vitamin K antagonist. Aspirin is an alternative to a vitamin K antagonist in low-risk patients or in those who have contraindications to vitamin K antagonists.
The intensity of anticoagulation should be based on prevention of ischemic stroke versus avoidance of hemorrhagic complications. The recommended target is an International Normalized Ratio (INR) of between 2.0 and 3.0. INR should be measured at least weekly during therapy and monthly when anticoagulation is stable. Minimizing the risk of bleeding is particularly important in older patients.
INTERRUPTION OF ANTICOAGULATION
If anticoagulation is interrupted for more than one week because of surgery in high-risk patients, unfractionated or low-molecular-weight heparin may be administered to prevent thrombosis, although the effectiveness of these therapies has not been evaluated in controlled trials.
In patients undergoing percutaneous coronary intervention, anticoagulation may be interrupted to prevent bleeding; however, vitamin K anticoagulation should be reinstated as soon as possible after the procedure. Platelet-inhibitor drugs are valuable for preventing recurrent myocardial ischemia in patients undergoing percutaneous coronary intervention. Although aspirin may be given during the hiatus, maintenance therapy should consist of clopidogrel (Plavix) and warfarin (Coumadin); warfarin may be continued as monotherapy after nine to 12 months if no coronary events occur.
Cardioversion
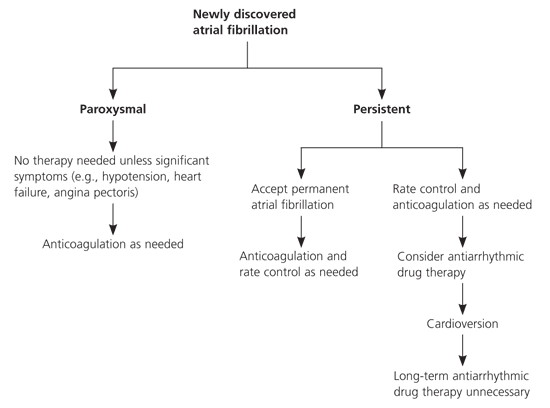
Cardioversion (via drugs or electric shock) may be used to restore sinus rhythm in patients with persistent atrial fibrillation; however, there is a risk of thromboembolism unless anticoagulation is initiated before the procedure. Cardioversion is recommended for hemodynamically stable patients with atrial fibrillation symptoms that the patient feels are unacceptable (Figure 1). Recommended agents for pharmacologic cardioversion of atrial fibrillation are flecainide (Tambocor), dofetilide (Tikosyn), propafenone (Rythmol), and ibutilide (Corvert). Direct-current cardioversion is recommended if rapid ventricular response does not occur with pharmacologic cardioversion in patients with ongoing myocardial ischemia, symptomatic hypotension, angina, or heart failure.