Patient registries are necessary for high-quality health care, but even in innovative practices, their presence and utilization is inadequate. Registry uptake in primary care may be enhanced by improving the functionality of electronic health records (EHRs) and implementing payment models that reward registry use.
Patient registries identify relevant subpopulations of patients for proactive care, which includes timely preventive and chronic care reminders and prompts to ensure that patients receive care at appropriate intervals. Registries are vital for providing high-quality care, and are identified as an important characteristic of the New Model practice in the Future of Family Medicine study.1
This analysis takes advantage of the Prescription for Health (P4H) initiative. It includes information on 72 P4H practices, 38 (53 percent) of which reported having registries for single or multiple conditions (see accompanying figure).2 Practices that have any registry almost always have a diabetes registry. Practices with pediatric populations more commonly have asthma registries. Few practices have registries to monitor health behaviors, such as smoking, diet, physical activity, and risky drinking.
Figure.
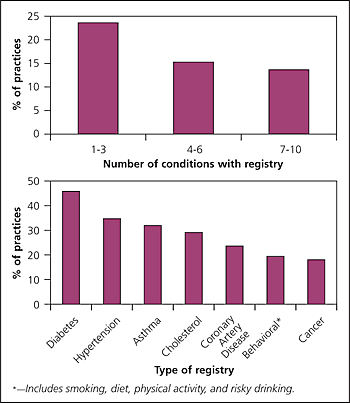
Percentage of Prescription for Health practices that use registries to track single or multiple conditions.
Information from reference 2.
The presence of a registry does not guarantee its effective use in managing and monitoring care. In only one half of the practices with a registry can subpopulations be sorted by clinical priorities, and only 14 of these practices (37 percent) link patient care to guidelines that provide prompts and reminders about needed services. In the 72 P4H practices, 47 percent of practices without registries and 42 percent of practices with registries have EHRs, and chi-square tests showed no association between the presence of an EHR and registry use.
Registries are widely used among family medicine practices in the United Kingdom, where payment systems cover their costs and reward their use.3 EHRs with integrated registries can provide a source of patient information and maintain multiple disease registries. Few EHR systems in the United States are equipped with these critical functions.4 Changes in EHR design, health care payment, and quality incentives could improve the use of patient registries in U.S. primary care practices.

