A 20-year-old military recruit presented for follow-up of anterior knee pain. Previously, he presented with three weeks of right knee pain without trauma, swelling, locking, or instability. At that visit, he was referred for physical therapy, but the knee did not improve during treatment. On recent examination, the patient had a positive “theater sign” (i.e., knee pain upon arising after prolonged sitting), positive patellar compression and inhibition tests, stable ligaments, pain with McMurray's test, and tenderness of the medial tibial plateau. Radiography was performed (Figures 1 and 2).
Figure 1.
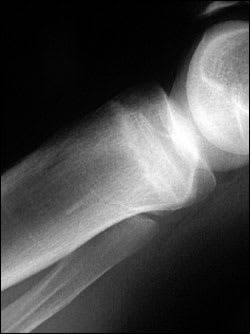
Figure 2.
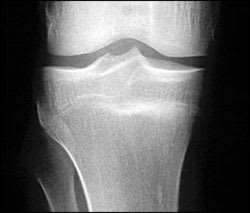
Question
Based on the patient's history, physical examination, and radiography results, which one of the following is the most likely diagnosis?
A. Medial plica syndrome.
B. Patellar tendinopathy.
C. Patellofemoral pain syndrome.
D. Pes anserine bursitis.
E. Proximal tibial stress fracture.
Discussion
The answer is E: proximal tibial stress fracture. Most tibial stress fractures occur in the tibial diaphysis. However, proximal tibial stress fractures, typically involving the medial condyle, can occur in athletes. Stress fractures may result from weaker bone that fails under normal loading (i.e., an insufficiency fracture) or normal bone that fails under new or increased repetitive loading (i.e., a fatigue fracture). Athletes are more likely to experience a fatigue fracture1; military recruits are also at risk.2
Medical history that suggests a stress fracture will include persistent pain following an acute increase in physical activity (i.e., time, distance, or pace). Physical examination may reveal tenderness at or near the medial joint line, tenderness with a leverage motion, and tenderness with hopping on the affected leg. A joint effusion may also be present.1
Plain radiographs can appear normal for weeks or even months.1,3 Because the metaphyseal portions of long bones are mostly cancellous bone, the typical periosteal/endosteal reaction will not be visible. In this type of bone, the features of a stress fracture manifest as a band-like area of sclerosis.3,4 If a stress fracture is suspected but radiographic results are normal, then magnetic resonance imaging (MRI) or a bone scan is the next diagnostic study. Of the two, MRI is more sensitive for diagnosing stress fracture.1 Bone scans can be non-specific; therefore, a positive scan should be viewed in the context of the clinical history.3,4
Treatment of tibial stress fracture involves reducing the physical load on the involved area. Thus, patients need to avoid the inciting exercise. Cardiovascular exercise that does not load the injury (e.g., swimming) may be substituted. A gradual return to full activity is guided by the level of pain, with incremental increases in activity if the patient remains pain-free.1,2
Plica syndrome describes a thickening of the medial retinaculum that may be painful or painless. It usually is palpated on the medial joint line and can result from direct trauma to a flexed knee, although plica syndrome related to twisting and overuse also has been reported.5 History indicating plica syndrome includes a painful arc of 30 to 60 degrees, pain with stair climbing, activity, and “pseudolocking.”5 Whether or not it causes knee pain is debated.
Patellar tendinopathy (also known as “jumper's knee”) presents with a theater sign and an insidious onset of pain when climbing stairs. However, a history of acute increases in physical activity, especially jumping, will be elicited. Physical examination will reveal a tender patellar tendon, especially at the inferior pole.6
Patellofemoral pain syndrome is the most common cause of anterior knee pain, although it can be considered a diagnosis of exclusion. The patient may have or describe a theater sign. Tenderness can be elicited with compression of the patella into the femoral groove. Patients may have pain with McMurray's test when the knee is fully flexed because this engages the patella into the trochlear groove.7
Pes anserine bursitis is the result of irritation from trauma or overuse of the tendons of the gracilis, semitendinosus, and sartorius muscles as they cross over the medial femoral condyle and insert on the medial tibia.8
Summary Table
| Condition | Characteristics |
|---|---|
| Medial plica syndrome | Palpable tissue band, generally at the joint line, similar to a bowstring |
| Patellar tendinopathy | Tenderness in the patellar tendon with increased activity, especially jumping |
| Patellofemoral pain syndrome | Anterior knee pain, pain with stair climbing, absence of radiographic pathology |
| Pes anserine bursitis | Tenderness and edema at the tendon insertion at the medial proximal tibia |
| Proximal tibial stress fracture | Tenderness at site of fracture, radiographic finding of sclerosis |

