Foreign bodies in the ear, nose, and throat are occasionally seen in family medicine, usually in children. The most common foreign bodies are food, plastic toys, and small household items. Diagnosis is often delayed because the causative event is usually unobserved, the symptoms are nonspecific, and patients often are misdiagnosed initially. Most ear and nose foreign bodies can be removed by a skilled physician in the office with minimal risk of complications. Common removal methods include use of forceps, water irrigation, and suction catheter. Pharyngeal or tracheal foreign bodies are medical emergencies requiring surgical consultation. Radiography results are often normal. Flexible or rigid endoscopy usually is required to confirm the diagnosis and to remove the foreign body. Physicians need to have a high index of suspicion for foreign bodies in children with unexplained upper airway symptoms. It is important to understand the anatomy and the indications for subspecialist referral. The evidence is inadequate to make strong recommendations for specific removal techniques.
Most patients with ear, nose, and throat foreign bodies are children; intellectually challenged or mentally ill adults are also at increased risk. Often, family physicians are able to remove the foreign body in the office. Successful removal depends on several factors, including location of the foreign body, type of material, whether the material is graspable (i.e., soft and irregular) or nongraspable (i.e., hard and spherical), physician dexterity, and patient cooperation. Table 1 provides an overview of common foreign bodies, removal techniques, and indications for referral.1–18
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Directly visible, “graspable” foreign bodies in the ear or nose can often be removed without subspecialist referral. | C | 1 |
| Removal of hard, nongraspable, spherical foreign bodies in the ear canal against the tympanic membrane will most likely require subspecialist referral. | C | 1, 23 |
| If a foreign body in the ear, nose, or throat cannot be directly visualized or if attempts at removal have been unsuccessful, the patient should be referred to a subspecialist. | C | 1, 3, 12 |
| Patients with a suspected foreign body in the throat should be referred to a subspecialist unless the item is easily visible and graspable. | C | 14, 18 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1095 or https://www.aafp.org/afpsort.xml.
Table 1 Management of Common Foreign Bodies in the Ear, Nose, and Throat
| Location | Common foreign bodies | Removal technique | Indications for referral |
|---|---|---|---|
| Ear | Beads, plastic toys, pebbles, popcorn kernels2 |
| |
| Nose | Beads, buttons, toy parts, pebbles, candle wax, food, paper, cloth, button batteries5,6 |
| |
| Throat (pharynx)* | Plastic, metal pin, seeds, nuts, bones, coins, dental appliances14–18 |
PPV = positive pressure ventilation.
*— Most foreign bodies in the throat require consultation with a subspecialist.
Ear Foreign Bodies
The external auditory canal is a cartilaginous and bony passage lined with a thin layer of periosteum and skin. The osseous portion is extremely sensitive because the skin provides little cushion over the underlying periosteum. Thus, attempts at foreign body removal can be extremely painful.
The external auditory canal narrows at the bony cartilaginous junction (Figure 1). Foreign bodies can become impacted at this point, increasing the difficulty of removal. Attempts to remove the foreign body may push it further into the canal and lodge it at this narrow point. In addition, the tympanic membrane can be damaged by pushing the foreign body further into the canal or by the instruments used during removal attempts. Adequate visualization, appropriate equipment, a cooperative patient, and a skilled physician are the keys to successful foreign body removal.
In many cases, patients with foreign bodies in the ear are asymptomatic, and in children the foreign body is often an incidental finding.1,19 Other patients may present with pain, symptoms of otitis media, hearing loss, or a sense of ear fullness. In several large case series focusing on children, researchers found that 75 percent of patients with ear foreign bodies were younger than eight years.1,2,19 Similar studies on adult patients are lacking.
The most common ear foreign bodies include beads, plastic toys, pebbles, and popcorn kernels.2 Insects are more common in patients older than 10 years. In one series, 30 percent of patients required general anesthesia to facilitate removal of an ear foreign body; the majority of those patients were younger than seven years.2 Graspable foreign bodies (e.g., foam rubber, paper, vegetable material) have higher rates of success for removal under direct visualization. In contrast, nongraspable foreign bodies (e.g., beads, pebbles, popcorn kernels) have lower rates of successful removal and are associated with more complications, particularly canal lacerations.3
Many techniques to remove ear foreign bodies are available, and the choice depends on the clinical situation, the type of foreign body suspected, and the experience of the physician. Options include water irrigation, forceps removal (e.g., alligator forceps), cerumen loops, right-angle ball hooks, and suction catheters. Live insects can be killed rapidly by instilling alcohol, 2% lidocaine (Xylocaine), or mineral oil into the ear canal. This should be done before removal is attempted but should not be used when the tympanic membrane is perforated.20
Irrigation should be avoided in patients with button batteries in the ear because the electrical current and/or battery contents can cause a liquefaction tissue necrosis.21 Acetone may be used to dissolve Styrofoam foreign bodies4 or to loosen cyanoacrylate (i.e., superglue).22
The first attempt at removal is critical because success rates markedly decrease after the first failed attempt. Accordingly, complications increase as the number of failed removal attempts increases.23,24 Removal attempts are often painful, can cause bleeding that limits visualization, and can further wedge the foreign body into the canal. An otolaryngology referral should be obtained for patients requiring sedation or anesthesia. Other indications for referral include patients with trauma to the canal or tympanic membrane; a nongraspable foreign body that is tightly wedged in the medial two thirds of the canal or is suspected of touching the tympanic membrane; foreign bodies with sharp edges (e.g., pieces of glass); or unsuccessful removal attempts.1–3
Multiple foreign bodies are not uncommon, especially in small children. Thus, all other orifices of the head should be inspected after removal of a foreign body from the external auditory canal.3 Otic antibiotic drops are needed in patients with concurrent otitis externa and should be considered when canal lacerations or trauma is present. Audiography should be considered if tympanic membrane trauma or hearing loss is suspected.
Nasal Foreign Bodies
The nose consists of two nasal fossae separated by a vertical septum and subdivided into three passages by the nasal turbinates. Nasal foreign bodies tend to be located on the floor of the nasal passage, just below the inferior turbinate, or in the upper nasal fossa anterior to the middle turbinate5 (Figure 2). Most nasal foreign bodies can be easily removed in the office or emergency department. Patients often present with unilateral, foul-smelling nasal discharge.25 Common nasal foreign bodies include beads, buttons, toy parts, pebbles, candle wax, food, paper, cloth, and button batteries.5,6
Figure 1.
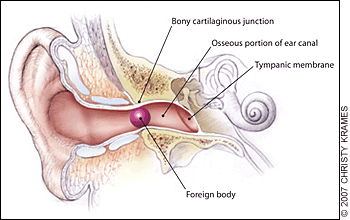
The external auditory canal. Foreign bodies may become lodged in the narrowing at the bony cartilaginous junction.
Before foreign body removal, 0.5% phenylephrine (Neo-Synephrine) can be used to reduce mucosal edema, and topical lidocaine may be applied to provide analgesia. Techniques include removal with direct visualization using forceps, curved hooks, cerumen loops, or suction catheters. Additionally, successful removal has been achieved by passing a thin, lubricated, balloon-tip catheter (5 or 6 French Foley) past the foreign body, inflating the balloon, and pulling the inflated catheter balloon forward, thus moving the foreign body into the anterior nares where removal can be completed.7
Figure 2.
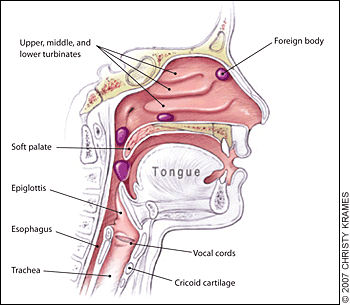
Nasopharyngeal and tracheal anatomy. Highlighted areas indicate points at which nasal foreign bodies may become lodged.
Patients may be able to expel the nasal foreign body simply by “blowing their nose” while blocking the opposite nostril. If this fails, or if a nasal foreign body is present in a small child unable to cooperate, positive pressure ventilation can be delivered through the patient's mouth. In this technique, the parent covers the child's mouth with his or her mouth, plugs the unobstructed nostril with a finger, and gives a rapid, soft puff of air.8,9 Although the child will reflexively close the glottis to protect his or her lungs from the pressure, it is important that the parent not use a large-volume or high-pressure breath.
Barotrauma to the ear is a theoretical risk of positive pressure ventilation, but this complication has not been reported. Appropriate infection-control precautions must be taken because the foreign body will likely be expelled against the parent's cheek and will be covered with mucus and possibly blood. Positive pressure can also be delivered through the mouth using a bag mask (Ambu Bag)10 or through the nose using oxygen tubing.11 Button batteries must be removed from the nose immediately because of the danger of liquefaction necrosis of the surrounding tissue.26
Attempts at removal may push the nasal foreign body into the pharynx, creating an airway hazard. Sedation is discouraged because it can increase complications by reducing the gag and cough reflexes.12 Consultation should be obtained when the foreign body cannot be removed or adequately visualized, or when a tumor or mass is suspected.
Throat Foreign Bodies
The throat (pharynx) is bound superiorly by the base of the skull (nasopharynx) and inferiorly by the cricoid cartilage/inferior border of the C6 vertebra (hypopharynx; Figure 2). The hypopharynx contains the larynx and the upper openings of the trachea and the esophagus.
All pharyngeal foreign bodies are medical emergencies that require airway protection. Because complete airway obstruction usually occurs at the time of aspiration and results in immediate respiratory distress, emergency intervention is essential. Common obstructing foreign bodies in children include balloons, pieces of soft deformable plastic, and food boluses.15 Patients with nonobstructing or partially obstructing foreign bodies in the throat often present with a history of choking, dysphagia, odynophagia, or dysphonia.13 Pharyngeal foreign bodies should also be suspected in patients with undiagnosed coughing, stridor, or hoarseness.14
Parents and caregivers of children with symptoms of partial airway obstruction should be asked whether choking and aspiration have occurred. Diagnosis is often complicated by delayed presentation. Case reports describe foreign bodies in the throat that were misdiagnosed and treated as croup.15,27 Thus, physicians must have a high degree of suspicion in patients with unexplained upper airway symptoms, especially in children who have a history of choking.
The most common foreign bodies in the throat are pieces of plastic, metal pins, seeds, nuts, bones, coins, and dental appliances.14–17 Radiography can be helpful in localizing coins, button batteries, and other radiopaque objects, but most laryngeal foreign bodies, including many fish bones, are radiolucent.13,28 Therefore, the decision to pursue surgical intervention should be based on the patient's history and a physical examination that suggests the presence of a foreign body rather than based on radiography alone.29
Early consultation is advisable because pharyngeal foreign bodies are difficult to visualize without the use of flexible or rigid endoscopy. Furthermore, removal attempts are difficult and are complicated by the gag reflex. Because the airway must be protected, most foreign bodies in the throat require otolaryngology intervention with sedation and endoscopic removal.14,18 Complications include airway obstruction, laryngeal edema, and pushing the foreign body into the subglottic space, esophagus, or trachea.14,18

