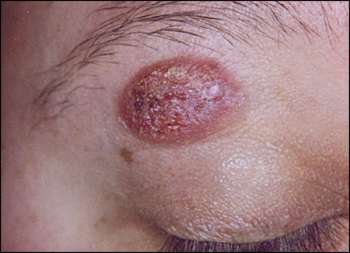
A 28-year-old woman presented with a red, scaly, itchy lesion on her right upper eye-lid (see accompanying figure). The lesion appeared one month earlier and grew rapidly. The patient denied a history of trauma to the area. She had occasional burning, bleeding, and white discharge around the lesion, but no fever or other systemic symptoms. The patient had no notable medical history and was taking no medication.
Question
Based on the history and physical examination, which one of the following is the most likely diagnosis?
A. Cutaneous blastomycosis.
B. Furuncle.
C. Orf (contagious ecthyma).
D. Pyogenic granuloma.
E. Squamous cell carcinoma.
Discussion
The answer is A: cutaneous blastomycosis. A biopsy confirmed the diagnosis. Cutaneous blastomycosis is an infection caused by the thermally dimorphic fungus Blastomyces dermatitidis. The infection occurs as pulmonary disease, disseminated extrapulmonary disease, or both.
Patients with pulmonary disease may have symptoms similar to those of tuberculosis, lung cancer, or pneumonia. After the spores are inhaled, they are cleared by the immune system, or they transition into yeast form and spread hematogenously. Symptomatic disease may develop after an incubation period of 30 to 45 days.1 Pulmonary infection is asymptomatic in up to 50 percent of patients with inhalation blastomycosis; therefore, pulmonary infiltrates on chest radiographs may be the only diagnostic clue to infection.2
Extrapulmonary involvement most commonly affects the skin, followed by the skeletal, urogenital, and central nervous systems. Cutaneous blastomycosis lesions usually occur on the face, with eyelid involvement often reported in patients with systemic disease.3
Cutaneous blastomycosis occurs in a verrucous or ulcerative form. The verrucous form begins as a small papule or pustule that slowly enlarges, becoming encrusted with irregular borders; microabscesses may form around the lesion. The ulcerative form is slightly raised with sharp borders; the base of the ulcer contains red granulation tissue that bleeds easily.4 Both forms may be painful. Diagnosis can be confirmed with microscopic examination of purulent material using potassium hydroxide preparation or the fungal stain calcofluor. A more definitive diagnostic method is a biopsy or culture of tissue or exudate that shows fungi.
Blastomycosis is endemic to states bordering the Ohio and Mississippi River basins, the Great Lakes, and the St. Lawrence River.1 Patients are exposed through contact with soil or decomposed timber, usually during leisure or occupational activities in humid endemic regions. Although most cases originate in the respiratory tract, direct inoculation of the skin after trauma has led to primary cutaneous blastomycosis.2
The recommended treatment for uncomplicated pulmonary or extrapulmonary blastomycosis is itraconazole (Sporanox; 200 mg daily for six months).3 Amphotericin B is used in children, patients who are pregnant or immunocompromised, patients with more severe blastomycosis or central nervous system blastomycosis, and patients who do not improve with oral azole therapy.3
A furuncle is an acute, inflammatory abscess of the hair follicle that is usually caused by Staphylococcus aureus infection. The lesion tends to occur in areas of friction or minor trauma.
Orf (contagious ecthyma) is a paramyxovirus caused by direct contact with infected livestock (e.g., sheep) or contaminated fomites. The lesion tends to occur on the fingers, beginning as a papule or pustule that develops over six stages into a flat, dry crust.
A pyogenic granuloma is a small, solitary, rapidly growing ulceration of the skin or mucosa. The lesion may be sessile or pedunculated, has a pronounced red color, and tends to bleed easily. It usually occurs on exposed skin or in areas of trauma.
Squamous cell carcinoma commonly begins as an actinic keratosis, an erythematous scaly plaque, on sun-exposed areas. The lesion enlarges over a few months, becoming deeply nodular and ulcerated. In the late stages, the lesion becomes more diffuse, depressed, and rigid.
Selected Differential Diagnosis of a Red, Scaly Lesion on the Upper Eyelid
| Condition | Characteristics |
|---|---|
| Cutaneous blastomycosis | Enlarging papule or pustule with variable borders; may contain red granulation tissue |
| Furuncle | Round, painful abscess of the hair follicle |
| Orf (contagious ecthyma) | Papule or pustule that develops over distinct stages into a flat, dry crust; systemic involvement is common |
| Pyogenic granuloma | Marked, red ulceration; usually secondary to trauma |
| Squamous cell carcinoma | Nonhealing plaque that develops into a nodular, ulcerated lesion |

