Numerous guidelines recommend physical therapy for the management of musculoskeletal conditions. However, specific recommendations are lacking concerning which exercises and adjunct modalities to use. Physical therapists use various techniques to reduce pain and improve mobility and flexibility. There is some evidence that specific exercises performed with the instruction of physical therapists improve outcomes in patients with low back pain. For most modalities, evidence of effectiveness is variable and controlled trials are lacking. Multiple modalities may be used to treat one clinical condition; decisions for the treatment of an individual patient depend on the expertise of the therapist, the equipment available, and the desire of the attending physician. A physical therapy prescription should include the diagnosis; type, frequency, and duration of the prescribed therapy; goals of therapy; and safety precautions.
Physical therapists are an integral part of inpatient and outpatient treatment of neurologic and musculoskeletal injuries and disabilities. They also can assist with and augment the care of patients with cardiac, pulmonary, and developmental disorders. Family physicians should have some understanding of the various treatments and modalities used by physical therapists.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Supervised therapeutic exercise improves outcomes in patients with osteoarthritis of the knee or claudication. | B | 3, 4 | Supervised therapeutic exercise has been shown to improve walking speed and distance compared with home exercise. |
| Iontophoresis improves outcomes in patients with myositis ossificans compared with usual care. | B | 23 | — |
| Low-level laser therapy has been shown to provide limited benefit in the treatment of osteoarthritis and rheumatoid arthritis. | B | 31, 32 | This therapy has no adverse effects and has been shown to have symptomatic benefit in the treatment of several inflammatory conditions; standardization of therapy will help in defining the role of this modality. |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1595 or https://www.aafp.org/afpsort.xml.
Physical Therapy
Modalities are adjunctive treatments to exercise and manual therapy; the use of modalities alone is not considered physical therapy. The American Physical Therapy Association states: “Without documentation which justifies the necessity of the exclusive use of physical agents/modalities, the use of physical agents/modalities in the absence of other skilled therapeutic or educational interventions should not be considered physical therapy.”1 The ultimate goal of any physical therapy intervention is to improve the long-term function of the patient, which is best accomplished with the use of exercise, manual therapy, and modalities.
Research conducted during the development of several physical therapy modalities focused on how they affect inflammation. Many of the conditions that were thought to be inflammatory (e.g., patellar tendonitis) are in fact not histologically inflammatory. However, these tendinopathies (a more accurate classification) continue to be treated with modalities designed to decrease inflammation. There is some evidence that these modalities may be beneficial, but this may not be related to a true anti-inflammatory effect.
Exercise and Adjunct Modalities
A working knowledge of the uses and limitations of different modalities will assist family physicians in prescribing physical therapy. Table 1 summarizes some of the physical therapy modalities that are available. The practicality of individual modalities may vary, and physicians are encouraged to discuss the options with qualified physical therapists.
Table 1 Commonly Used Physical Therapy Modalities
| Modality | Description | Potential therapeutic uses | Contraindications/cautions |
|---|---|---|---|
| Ultrasound | High-frequency sound waves are used to warm superficial soft tissues or to accelerate tissue healing at the cellular level | Tendon injuries, short-term pain relief of muscle strain or spasm | Do not use near malignant tumors, nerve tissue following laminectomy, joint replacements, permanent pacemakers, thrombophlebitis, eyes, reproductive organs, acute inflammation, epiphyseal plates, or over breast implants; exemption is needed for Olympic athletes |
| Phonophoresis | Ultrasound is used to deliver therapeutic medications to tissue under the skin | Inflammatory conditions such as tendonitis, arthritis, and bursitis | Same as for ultrasound |
| Iontophoresis | Electric current is used to deliver ionically charged substances through the skin to deeper tissues | Calcific tendinopathy, inflammatory conditions, hyperhidrosis | Do not use in patients with an allergy or sensitivity to the substance applied, open wounds, or decreased sensation; do not use in the immediate vicinity of metallic implants, wires, or staples |
| Electrical stimulation | Generates an action potential in nerve tissue, causing a muscle contraction or altering sensory input | Muscle spasm or contusion (electronic muscle stimulation), neuropathic pain relief (transcutaneous electrical nerve stimulation) | Do not use in patients with cardiac pacemakers, known cardiac arrhythmias, or thrombophlebitis/thrombosis; do not use on the abdomen or pelvis of pregnant patients; use with caution in patients with cardiac disease, malignant tumors, open wounds, decreased sensation, or decreased mentation or communication ability |
| Low-level laser therapy | Absorption of photon radiation, altering cellular oxidative metabolism and decreasing prostaglandin E2 concentration | Minor musculoskeletal pain, carpal tunnel syndrome, osteoarthritis, rheumatoid arthritis | Use with caution in patients with malignant tumors or in patients taking anticoagulant, corticosteroid, or immunosuppressive drugs; do not use on the uterus of pregnant patients; patients and therapists should use safety goggles to limit eye exposure to therapeutic wavelengths |
THERAPEUTIC EXERCISE
Exercises that target muscle deficiencies or that help rehabilitate patients after surgery or injury are a mainstay of many physical therapy protocols. Therapeutic exercise is used to improve strength, mobility, and function and to decrease pain and swelling.
Family physicians often prescribe simple home-based rehabilitation exercises by providing patients with brief instruction and handouts. Supervised therapeutic exercise has been shown to be more beneficial than home-based exercise in patients with low back injury,2 osteoarthritis of the knee,3 or intermittent claudication.4 Other studies, however, have found that home-based exercise is as beneficial as supervised physical therapy for postoperative recovery after anterior cruciate ligament reconstruction.5,6 Table 2 includes common therapeutic exercises.
Table 2 Common Therapeutic Exercises
| Exercise type | Description | Therapeutic uses |
|---|---|---|
| Closed kinetic chain | Proximal segment of the extremity moves on a fixed distal segment (e.g., leg press, squats, elliptical walker) | Shoulder and knee rehabilitation, dynamic stability |
| Concentric | Muscle contracts as it shortens (e.g., flexion phase of a biceps or hamstring curl) | Increase muscle mass and strength |
| Core stability | Targets low back, trunk, and abdominal muscles (e.g., sit-up, back extension, abdominal crunch, Pilates) | Relief of low back pain or pregnancy-related pelvic pain |
| Eccentric | Muscle contracts as it lengthens (e.g., extension phase of a biceps or hamstring curl) | Sport-specific strengthening to prevent injury |
| Isometric | Muscle contracts, but its length stays the same (e.g., holding a weight in a stationary position for a few seconds) | Muscle toning and strengthening when joint mobility is not advised; quadriceps exercises to treat patellofemoral pain syndrome |
| Isotonic | Constant resistance applied to a muscle through a joint range of motion (e.g., free-weight lifting) | General muscle conditioning |
| Open kinetic chain | Distal segment of the extremity moves about the proximal segment (e.g., long arc quadriceps extension, most weight-lifting exercises using the arms) | Functional improvement in activities of daily living |
ULTRASOUND
Therapeutic ultrasound is another commonly employed technique. Modifying the application parameters (i.e., intensity, wavelength, duty cycle, and frequency) provides a variety of local effects on tissues.
Ultrasound provides therapeutic benefit via thermal (continuous ultrasound) and nonthermal (pulsed ultrasound) effects.7,8 Continuous ultrasound heats the tissue. Pulsed ultrasound is thought to accelerate tissue healing at the cellular level, primarily through alteration of membrane permeability, ionic concentration gradients, and cellular biochemical activity.7,8 Higher-frequency ultrasound waves treat superficial tissues such as patellar tendons. Lower frequencies penetrate deeper (up to 2 in [5 cm]) to treat deep muscle bruising, spasms, and strains.7 Selection of ultrasound application parameters is based on the desired effect and the location and density of the tissue to be treated. These decisions are best made by a therapist experienced in performing therapeutic ultrasound.
Common indications for ultrasound therapy include treatment of tendon injuries and short-term pain relief.7,9–11 Ultrasound has also been shown to promote healing of some acute bone fractures, venous and pressure ulcers, and surgical incisions.7,8,12,13 Therapeutic ultrasound can cause burns or endothelial damage if applied incorrectly.7,8,14
Despite the widespread use of therapeutic ultrasound in the physical therapy setting, evidence of its clinical effectiveness is lacking. Although there is limited evidence that ultrasound benefits musculoskeletal pain and soft tissue injury, more well-designed studies of its clinical effects are needed.9,15–17 In the absence of more definitive evidence, family physicians should prescribe therapeutic ultrasound only as symptomatic treatment.
PHONOPHORESIS
Phonophoresis uses high-frequency sound waves (i.e., ultrasound) to deliver therapeutic medications, usually topical analgesics or steroids, through the skin to deeper tissues. It is used for the treatment of conditions that may also be treated with local anesthetic or steroid injections. There is a risk of thermal injury, which increases with the amount and intensity of the energy applied.18
A corticosteroid or nonsteroidal anti-inflammatory drug usually is mixed with an appropriate aqueous base in a 10 percent concentration and is applied with ultrasound at 1 to 2 watts per cm2.18 One study showed an increased level of ketoprofen in tissues following phonophoresis compared with topical application alone.19 Studies of the systemic effects of phonophoresis with steroids have had contradictory results. One study demonstrated a possible systemic decrease in collagen deposition after phonophoresis with dexamethasone, but another study showed no effect on adrenal function.20,21
IONTOPHORESIS
This modality uses an electric current to deliver an ionically charged substance through the skin to deeper tissues. Iontophoresis is often used to treat arthritis, bursitis, and tendinopathy. It can also be used to treat edema, hyperhidrosis, and certain dermatophytoses.18 Hypersensitivity to direct current may cause a characteristic galvanic skin response.
Dexamethasone 0.4% solution is the most commonly prescribed medication used to treat tendinopathies and possible inflammatory conditions. Cathodes are used for negatively charged substances, and anodes are used for positively charged substances. The amperage used depends on the natural resistance provided by the skin.
Iontophoresis in conjunction with traditional modalities can shorten treatment time for plantar fasciitis.22 One small case report showed that acetic acid iontophoresis in conjunction with ultrasound was beneficial in the treatment of myositis ossificans.23 However, a small randomized controlled trial showed no difference in the clinical outcome of patients with calcific tendinopathy in the shoulder.24
ELECTRICAL STIMULATION
There are several electrical stimulation methods used in physical therapy. Family physicians usually are most familiar with electrical muscle stimulation and transcutaneous electrical nerve stimulation. The theoretical goal of electrical stimulation is to generate an action potential in nerve tissue, causing a muscle contraction or altering sensory input.7
Muscle contraction allows for isometric activation, making electrical stimulation useful for the treatment of muscle spasm or atrophy and for strengthening muscles.7,8,25 In addition, electric currents are thought to affect ionic tissue and alter vascular membrane permeability, which promotes tissue healing, decreases edema, and improves drug penetration.7,8 Pain reduction is thought to be achieved by altering the gate mechanism and through endogenous opioid and cortisol release.7,8
Electrical stimulation may also help reduce inflammation and edema and facilitate chronic wound healing.7,8,26–28 Basic transcutaneous electrical nerve stimulation uses multiple electrodes that are impregnated with a conduction medium and applied over muscle groups. The location and spacing of the electrodes varies depending on treatment area and desired effect. Specific electrode placements are needed to create pain control, isometric muscle contraction, wound healing, and edema reduction.7,25–27
Although there are few risks with electrical therapy, potential adverse effects primarily include burns from improper parameter settings, allergic reaction to electrodes or the conduction medium, and pain during treatment.7,8,28 Expert opinion and anecdotal reports support the use of this modality; however, studies are lacking, limited, or conflicting. More evidence is needed on the long-term benefits, ideal parameters, and overall effectiveness of electrical stimulation methods.16,25,28,29
LOW-LEVEL LASER THERAPY
The mechanism of low-level laser therapy is not well understood, but it appears to be related to a photochemical reaction at the cellular level rather than a thermal effect. According to one theory, cytochrome oxidase acts as an acceptor of photon radiation in the 600 to 900 nm range. This stimulation increases adenosine triphosphate production and cellular oxidative metabolism. A recent study showed a significant decrease in prostaglandin E2 concentration in peritendinous fluid in patients treated with low-level laser therapy compared with those treated with sham therapy.30 Larger studies are needed to confirm this mechanism.
Low-level laser therapy is used to treat musculoskeletal disorders, including muscle strains, epicondylitis, rheumatoid arthritis, osteoarthritis, and carpal tunnel syndrome. This therapy is approved by the U.S. Food and Drug Administration for the treatment of hand and wrist pain associated with carpal tunnel syndrome and for minor musculoskeletal pain. Although nausea has been reported with prolonged use, there are no other known adverse effects.
Differences in studies of low-level laser therapy (e.g., device used, end points, control group) make it difficult to determine the effectiveness of this modality. A Cochrane review of low-level laser therapy in patients with osteoarthritis showed minimal improvement in pain and joint movement, but study results were conflicting.31 A similar Cochrane review of the therapy in patients with rheumatoid arthritis showed limited benefit but stated that it could be considered for short-term relief of pain and morning stiffness.32 In general, low-level laser therapy has not been shown to cause adverse effects, but a benefit has not been clearly established.
Physical Therapy Prescription
Table 3 lists the components of a physical therapy prescription. Proper coding should be used to ensure correct insurance reimbursement (online Table A). Physical therapy clinics often provide standard forms that facilitate prescribing of therapy. These forms can improve teamwork and communication between the physician and the therapist. Usually, there is an “evaluate and treat” option that allows the therapist to use discretion in the application of therapeutic interventions.
Table 3 Components of a Physical Therapy Prescription
| Diagnosis to be treated with physical therapy; proper coding should be used to allow for accurate insurance billing and reimbursement |
| Frequency and duration of therapy (e.g., daily for five days, three times per week for four weeks) depending on the condition being treated |
| Specific protocols or treatments that the physician wants the therapist to use |
| Safety precautions (e.g., joint range-of-motion limitations, weight-bearing limitations, illnesses that impact therapy decisions) |
| Physician signature and date are required for a therapist to perform the requested services |
The frequency and duration of physical therapy treatments will vary based on the patient's condition. Acute muscle strains often benefit from daily treatment over a short period, whereas chronic injuries are usually addressed less frequently over an extended period. Figure 1 is a general algorithm for prescribing physical therapy interventions to treat musculoskeletal injury; however, individual prescriptions are based on the patient's specific condition and comorbidities and on the availability of modalities.
Figure 1. Prescribing Physical Therapy for Musculoskeletal Injury
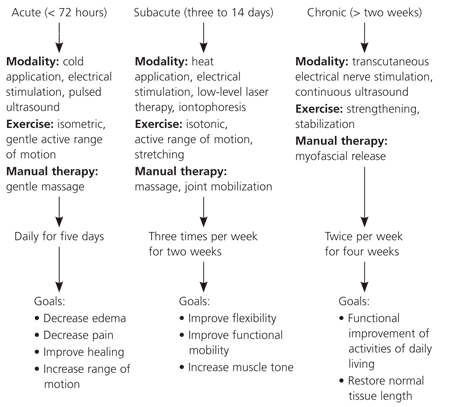
Algorithm for the selection of physical therapy interventions to treat typical musculoskeletal injury.
It is important for the physical therapist to document the patient's progress so that the physician can modify the care plan, if needed. This documentation is typically given to the physician every 30 days or before the patient sees the physician for a follow-up visit.

