When patients are diagnosed with cancer, primary care physicians often must deliver the bad news, discuss the prognosis, and make appropriate referrals. When delivering bad news, it is important to prioritize the key points that the patient should retain. Physicians should assess the patient's emotional state, readiness to engage in the discussion, and level of understanding about the condition. The discussion should be tailored according to these assessments. Often, multiple visits are needed. When discussing prognosis, physicians should be sensitive to variations in how much information patients want to know. The challenge for physicians is to communicate prognosis accurately without giving false hope. All physicians involved in the patient's care should coordinate their key prognosis points to avoid giving the patient mixed messages. As the disease progresses, physicians must reassess treatment effectiveness and discuss the values, goals, and preferences of the patient and family. It is important to initiate conversations about palliative care early in the disease course when the patient is still feeling well. There are innovative hospice programs that allow for simultaneous curative and palliative care. When physicians discuss the transition from curative to palliative care, they should avoid phrases that may convey to the patient a sense of failure or abandonment. Physicians also must be cognizant of how cultural factors may affect end-of-life discussions. Sensitivity to a patient's cultural and individual preferences will help the physician avoid stereotyping and making incorrect assumptions.
Primary care physicians have the opportunity to maintain long-term, trusting relationships with patients and are well positioned to discuss difficult issues such as newly diagnosed cancer or terminal illness.1 However, primary care physicians may not feel equipped to discuss end-of-life care. The lack of physician training in this area and patient or physician fear may lead to discomfort when communicating bad news.2 Providing care throughout a patient's illness can be highly gratifying for physicians and may lead to better patient outcomes. Using a systematic approach can help primary care physicians discuss prognosis appropriately, offer realistic hope, provide therapeutic options, coordinate disease transitions, and relieve patient suffering.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| When preparing to give bad news, it is important for physicians to assess the patient's level of understanding about the disease and expectations for the future. | C | 2, 11, 12, 14 |
| When preparing to give bad news, it is important for the physician to assess how much information the patient wants to know and to tailor the discussion appropriately. | C | 3, 15 |
| The primary care physician should remain involved with patient care during the early, middle, and late stages of cancer. | C | 22 |
| Physicians should initiate discussions about the availability of coordinated, symptom-directed services such as palliative care early in the disease process; as the disease progresses, physicians should transition from curative to palliative therapy. | C | 23, 24 |
| Physicians should avoid phrases and words that can be misconstrued by the patient and lead to negative interpretations such as abandonment and failure. | C | 12, 14, 27 |
| During end-of-life communication, physicians should assess and be sensitive to the patient's cultural and individual preferences. | C | 28–34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 131 or https://www.aafp.org/afpsort.xml.
Communicating Bad News
Illustrative case, part A: A 57-year-old female schoolteacher recently received a screening colonoscopy. During the procedure, a 2-cm × 2-cm sigmoid mass was biopsied. The mass was diagnosed as a poorly differentiated adenocarcinoma. The patient is waiting at the clinic to see her primary care physician to discuss the results.
Breaking bad news, particularly discussing prognosis, requires a combination of disease-specific biomedical knowledge and excellent communication skills.3 When bad news is delivered incorrectly, it can lead to long-term consequences such as poor psychological adjustment for patients.4,5 Therefore, recommendations have been developed to help physicians appropriately deliver bad news (Table 1).2,5–14
Table 1 Recommendations for Patient-Centered Communication When Discussing Bad News
| Recommendation | Comments |
|---|---|
| Prioritize: Prioritize what you want to accomplish during the discussion | Ask yourself: What are two to four key points that the patient should retain? What decisions should be made during this encounter? What is reasonable to expect from the patient during this encounter? |
| Practice and prepare: Practice giving bad news; arrange for an environment conducive to delivering the news | Rehearse the discussion; arrange for a private location without interruptions; set cell phones and pagers to vibrate or turn them off; ask the patient if he or she wants to invite family members |
| Assess patient understanding: Start with opening questions, rather than medical statements, to determine the patient's level of understanding about the situation | Ask the patient: “What do you already know about your condition?” “What does it mean to you?” “What do you think will happen?” |
| Determine patient preferences: Ask what and how much information the patient wants to know | Assess how the patient wants the information presented; ask the patient, “Some of my patients prefer hearing only the big picture, whereas others want a lot of details. Which do you prefer?” |
| Present information: Deliver information to the patient using language that is easy to understand (do not use medical jargon); provide a small amount of information at a time; check periodically for patient comprehension | Provide a few pieces of information, and then ask the patient to repeat it back to you |
| Provide emotional support: Allow the patient to express his or her emotions; respond with empathy | Assess the patient's emotional state directly and often (ask the patient: “How are you doing?” “Is this hard for you?” “You look frustrated/disappointed/angry—is that true?” “Let me know when we should continue”); use nonverbal cues such as eye contact; listen to what the patient says and validate his or her reactions with empathic statements such as “I understand that this is very difficult news.” |
| Discuss options for the future: Devise a plan for subsequent visits and care | Help the patient understand the expected disease course and how the disease may or may not respond to treatment; schedule follow-up visits (ask the patient: “Can we meet next week to discuss treatment options and any questions you may have?”) |
| Offer additional support: Provide information about support services | Bring handouts and pamphlets to the visit; refer the patient to support groups, psychologists, social workers, or chaplains |
| Consider individual preferences: Assess patient preferences, and tailor the discussion appropriately | Consider the patient's sex, age, health literacy, health status, previous health care experiences, social status, culture, and race/ethnicity; avoid assumptions about what the patient is likely to want; ask the patient directly about values and preferences |
Physicians should customize discussions, especially in situations that are stressful for the patient. Specifically, physicians should assess the patient's understanding (“Tell me what you know about this disease.”); emotional state (“This is a lot to take. How are you doing?”); and readiness to engage in the discussion (“Let me know when you're ready to continue.”). At each visit, physicians should assess whether patients have physical or psychological symptoms that need to be addressed (“How are you doing/coping?” “Is anything interfering with your quality of life?”).2,6–13
Discussing Prognosis
Illustrative case, part B: After surgery, the patient was diagnosed with stage III, two–node-positive colon cancer. Her oncologist discussed the prognosis with her and recommended adjuvant chemotherapy. The patient is still confused about what to do. Distraught, she calls her primary care physician and asks, “What should I do? Will I die soon?”
It is best to discuss prognosis after accurate cancer staging. In preparation, all physicians involved in the patient's care should coordinate their key prognosis messages to avoid confusing the patient. Physicians should be prepared to discuss the natural history of the disease, treatment and its adverse effects and outcomes, and the patient's probable quality of life. Additionally, physicians should discuss expected five- to 10-year survival rates, with and without treatment, and should address patient fears (e.g., fear of undergoing treatment, suffering, abandonment, or death). Empathic listening can ease and comfort patients.
Physicians should assess the patient's desire and readiness to receive the prognosis.3,15,16 The desired amount of information varies among patients. Approximately 80 percent of patients want detailed information about their prognosis, whereas 20 percent prefer not to know complete prognostic information.17,18 Thus, physicians should assess how much information to provide using patient-centered communication (Figure 13,15,16 ).
Figure 1. Patient-Centered Communication When Discussing a Bad Prognosis.
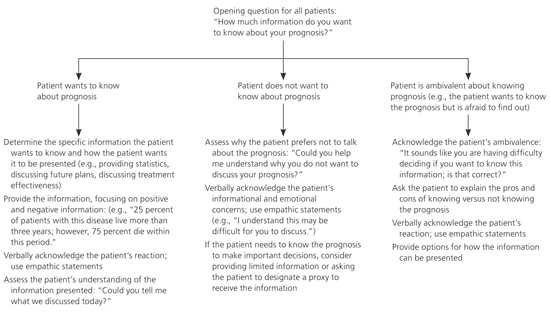
Algorithm for patient-centered communication when discussing a bad prognosis.
Information from references 3, 15, and 16.
After assessing the patient's readiness to receive prognostic information, the physician should focus on communicating the prognosis without giving false hope.19 One approach focuses on expectations (hoping for the best, planning for the worst), which allows physicians to discuss the worst-case scenario with the patient without taking away the possibility of the best-case scenario. After acknowledging the patient's expression of hope, the physician can ask whether the patient thinks that hope is realistic or probable.
Another approach focuses on providing the patient with a full spectrum of treatment options. A recent study showed that some patients elected to participate in phase I clinical trials of chemotherapy, even though the likelihood of benefit was low. When asked why they chose to participate in these trials, patients reported feeling like they had to do something.20 Providing options can validate the patient's need to be actively involved in his or her care.
Similarly, another approach focuses on sequential treatment options. In this approach, the physician supports the patient in undergoing a treatment, but also discusses what the next step would be if the initial treatment is unsuccessful. This approach sets practical parameters and allows discussion of alternatives if the goals of care are not attained.
The goals of care change as the disease progresses. At each stage, the physician should help the patient create realistic, achievable goals and hopes. Initially, patients might hope that the cancer responds to chemotherapy or surgery. When disease control is no longer possible, patients might hope to live pain free, achieve closure on personal issues, or die surrounded by friends and family. Focusing on stage-specific goals and hopes can prevent over- and undertreatment while relieving the patient's psychological distress.21
The Physician's Role at Different Stages of Disease
Illustrative case, part C: The patient's functional status has deteriorated rapidly. During chemotherapy, she developed esophagitis and recurrent neutropenic fever. Now, abdominal studies demonstrate early obstruction. Her primary care physician asks himself, “At this stage, what is my role in her care?”
The primary care physician's role changes at each stage of a patient's illness (Table 22,6,12,16,22 ). Ideally, primary care physicians form the backbone of an integrated team by providing an unbiased medical perspective, providing continuity during a stressful disease course, supporting patients and their families through emotional ups and downs, negotiating or mediating decisions, monitoring for complications, and providing perspective on the illness.6 This role is tempered by practical considerations such as the physician's practice and relationships with colleagues, available resources, and individual patient needs.
Table 2 The Primary Care Physician's Role in Patient Care During Different Stages of Cancer
| Role | Early stage | Middle stage | Late stage |
|---|---|---|---|
| Breaking bad news | Discuss diagnosis, disease course, therapeutic options, patient/family values and goals, and treatment preferences | Discuss treatment effectiveness | Assess patient/family understanding of prognosis and disease course |
| Communicating prognosis | Discuss expected prognosis | Help the patient understand changes in prognosis and refocus expectations; revisit values and preferences | Objectively discuss the advantages and disadvantages of experimental treatment, if offered by a subspecialist; discuss palliative care options such as hospice |
| Discussing disease transitions | Focus primarily on medical treatment while assessing palliative needs; the goal is extending life while improving quality of life | Focus on medical treatment and palliative needs | Focus explicitly on palliative care to relieve symptoms (e.g., pain, shortness of breath, fatigue, nausea); the goal is improving quality of life, including treatment of metastatic disease that is causing symptoms (e.g., bowel obstruction, bony metastasis) |
| Coordinating care | After referring the patient to a subspecialist, request that the patient schedule follow-up visits with you; ask the subspecialist to update you on the patient's care | Monitor the patient for symptoms and adverse effects (physical and psychological); discuss hospice as a therapeutic option; encourage the patient to begin advance care planning (e.g., advance directives, durable power of attorney for health care, living will) in case of deteriorating health | Discuss likely benefits and harms of major therapeutic options; discuss palliative care options |
| Providing support | Allow the patient to express emotion; answer questions and address concerns; provide emotional support and empathy; refer patient and family to support groups or counseling | Answer questions and address concerns; provide emotional support and empathy | Answer questions and address concerns; provide emotional support and empathy; reassure the patient that he or she will not be abandoned |
Negotiating this role to the satisfaction of everyone involved in the patient's care requires open communication. Simple questions can be asked to clarify each participants expectations: (1) to the patient: “Do you understand what is going to happen next? How are you and your family coping with this news?”; (2) to the subspecialist: “What are the expected benefits and harms from this new treatment? How much benefit accrues to the patient?”; and (3) To the health care team: “What additional resources can we mobilize for the patient?”
Primary care physicians may need to be proactive to stay involved in the patient's care.2 When referring a patient to an oncologist, primary care physicians can communicate their desire to continue caring for the patient. The physician also can ask subspecialists who are caring for the patient to provide periodic updates, and the physician can offer input or advice if the subspecialists have questions. The physician can schedule follow-up visits with the patient, even while the patient is undergoing chemotherapy or radiation.
However, primary care physicians may be uncomfortable with cancer care and may wish to transition the care of the patient to an oncologist or palliative care subspecialist. In this instance, it is important for the physician to communicate to the patient that the physician is still available, but that the subspecialists will be the main caregivers.
During the disease course, the patient's palliative and medical needs intensify. Innovative models can help physicians bridge the gap between traditional curative care and palliative care.23–25 Physicians assess palliative needs (for relief of suffering) throughout treatment. As the disease progresses, the focus shifts from curative therapy to palliative therapy. During this transition, the primary care physician should offer realistic hope and provide guidance in choosing appropriate treatment and palliative strategies.
Using simultaneous-care models, physicians can provide palliative and curative care at the same time. Newer open-access hospices provide full hospice care while allowing patients to receive disease-directed therapy. In many open-access hospices, patients may receive chemotherapy, radiation, blood transfusions, dialysis, or total parenteral nutrition.
Patients also may receive intense skilled palliative care at home (home-based hospice), often with family members as paid caregivers. A home-based hospice program is a modified version of the traditional home care model and, based on the argument that palliative care is a skilled need, is paid for by most insurance companies. Research shows that, compared with traditional home care, home-based hospice programs can improve patient satisfaction, reduce emergency department and physician office visits, and shorten nursing home and hospital stays while reducing costs by 45 percent.26
When discussing the option of hospice or other palliative care, physicians must be careful not to convey to the patient a sense of abandonment. Early in medical training, physicians may learn to use phrases that reflect a singular focus on curative therapy. If physicians see their role as only to cure disease, they may subconsciously convey their sense of failure to the patient if curative treatments are unsuccessful, and that cessation of curative options means the end of the physician's care. The shift from curative to palliative care is merely a change in the type of care that the physician is providing. Table 3 offers alternatives to commonly misconstrued physician phrases used in end-of-life discussions.12,14,27
Table 3 Commonly Misconstrued Physician Phrases Used in End-of-Life Discussions with Patients
| Physician phrase | Possible patient interpretation | Alternative phrase |
|---|---|---|
| “There's nothing we can do for you” | Abandonment: “My physician doesn't want to see me anymore” | “We can offer many options to control your symptoms and make you feel better” |
| “It's time to think about withdrawal of care” | Cessation of care: “My physician doesn't want to care for me anymore” | “Do you think that it is time to consider a different type of treatment that focuses on your symptoms? I'll be here with you no matter what you decide” |
| “Do you want us to do everything that we can to keep you alive (e.g., artificial life support)?” | Cessation of appropriate care: “If I don't have them do everything, I won't get the best medical care” | “If you become extremely ill, would you want to be put on artificial life support, or would you prefer a natural death?” |
| “You've failed the treatment (e.g., chemotherapy, radiation)” | Personal failure: “I've disappointed my physician” | “The cancer has not responded to the treatment as we had hoped. How are you doing?” |
| “I think you should consider hospice” | Despair and hopelessness: “I'm going to die soon” | “I want to provide intense, coordinated care with a team of professionals who will treat your symptoms and help you stay comfortable” |
Cultural Diversity and Individual Preferences
When a patient and physician enter into end-of-life discussions, each brings individual cultural backgrounds and values, which influence the discussions. Although understanding cultural norms is important, physicians must be careful to avoid stereotyping patients based on their culture.28
Individual culture is influenced by the culture of the family, religion and spirituality, education, occupation, social class, friends, and personal preferences. Asking open-ended questions can elicit the patient's preferences for physician frankness, decision making, and direct versus indirect communication (Table 428–34 ). Conflicts may arise when patients and families want care that physicians think is medically futile. Physicians may prevent misunderstanding and promote trust by respectfully listening to patients' beliefs and values and by negotiating mutually acceptable goals.
Table 4 Considerations for Cultural and Individual Patient Preferences in End-of-Life Discussions
| Considerations | Questions for patients | Potential consequences |
|---|---|---|
| Physician frankness (indirect or direct communication) | “How much do you want to know about your medical condition at this time?” | Physician may be regarded as rude, cruel, and uncaring if the physician is frank about the patient's condition when the patient is not ready to hear it or prefers to learn the information indirectly from a family member |
| If the patient prefers not to know everything: “Do you want to talk about this again at another time?” | The patient may experience feelings of hopelessness, depression, or anxiety if not psychologically ready to hear a bad prognosis or if he or she prefers to remain hopeful about the condition | |
| Involvement of family members or preference for autonomy | “Would you prefer that I discuss your medical condition with you directly, or would you prefer that I discuss it with a family member?” | Disagreements between the family or patient and the physician may occur when the physician does not assess whether the patient or family prefers family members to be involved |
| If the patient prefers that you discuss it with a family member: “Would you like to be present during the discussions about your medical condition?” | The patient may feel isolated if the family is not involved in discussions | |
| Decision making | “How do you want to make decisions regarding your health care?” “Do you want to make a decision yourself after I have given you all of the options?” (nondirective counseling) “Do you want me to suggest what I think is the best option?” (directive counseling) “Do you want to discuss the pros and cons of treatment and then make a decision together?” (shared decision making) | Unwelcome decisions may be made for the patient, and there can be a lack of collaboration between physician and patient (and family) if the physician uses directive counseling when the patient prefers nondirective counseling |
| The patient can lose confidence in the physician if the physician uses nondirective counseling when the patient prefers directive counseling | ||
| Advance care planning | “What are your goals for your life, right now?” “How do you feel about prolonging your life with artificial life support, even if there was no chance that you'd be able to live independent of the machines?” “If you became unable to make your own health care decisions, who would you want to make them for you?” | Overuse of potentially futile, aggressive care at the end of life and underuse of hospice services may occur if the patient does not endorse or understand available advance care planning options |
| Social, educational, and family factors | “Tell me about your family” “Have you or your family had significant experience with someone with a serious illness?” “If so, how did that experience affect you?” | The physician may offend or stereotype the patient because of incorrect assumptions if the physician does not ask about the patient's background |
| Misunderstandings between physician and patient may occur if the physician does not assess social, educational, and family preferences | ||
| Religious and spiritual factors | “Is there anything I should know about your religious or spiritual views before we discuss your medical condition?” | The physician may be regarded as disrespectful if the patient's religious and spiritual preferences are not addressed |
| The patient may reject medical advice if the physician does not understand how the patient views the physician's role and advice in the context of religion or spirituality |

