Heart failure caused by systolic dysfunction affects more than 5 million adults in the United States and is a common source of outpatient visits to primary care physicians. Mortality rates are high, yet a number of pharmacologic interventions may improve outcomes. Other interventions, including patient education, counseling, and regular self-monitoring, are critical, but are beyond the scope of this article. Angiotensin-converting enzyme inhibitors and beta blockers reduce mortality and should be administered to all patients unless contraindicated. Diuretics are indicated for symptomatic patients as needed for volume overload. Aldosterone antagonists and direct-acting vasodilators, such as isosorbide dinitrate and hydralazine, may improve mortality in selected patients. Angiotensin receptor blockers can be used as an alternative therapy for patients intolerant of angiotensin-converting enzyme inhibitors and in some patients who are persistently symptomatic. Digoxin may improve symptoms and is helpful for persons with concomitant atrial fibrillation, but it does not reduce cardiovascular or all-cause mortality. Serum digoxin levels should not exceed 1.0 ng per mL (1.3 nmol per L), especially in women.
Heart failure is a disease with considerable public health impact. Approximately 5.2 million Americans are affected,1 and the condition accounts for more than 3 million outpatient visits to primary care physicians each year.2 Incidence increases with age and, because the American population is aging, the incidence of heart failure and its associated morbidity and mortality are expected to increase. After a heart failure diagnosis, the one-year mortality rate is 20 percent.1
Unlike some diseases for which treatment options are limited, several interventions have been proven to reduce mortality in patients with heart failure. As a consequence, there is confusion regarding the best way to initiate and titrate therapy. This article presents a clinically useful guide (based on evidence from large clinical trials) for the appropriate use of pharmacologic therapy. Appropriate management of heart failure also includes other interventions (e.g., patient education, counseling, self-monitoring) that are beyond the scope of this article.
Although patients with symptomatic heart failure may have systolic or diastolic dysfunction, valvular heart disease, or isolated right-sided heart failure, the preponderance of evidence comes from trials of those with left ventricular systolic dysfunction; therefore, left ventricular systolic dysfunction will be the focus of this article. Clinical trials have used different ejection fraction cutoffs; however, systolic dysfunction is most often defined as an ejection fraction below 35 to 40 percent.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Unless contraindicated, an ACE inhibitor should be given to all patients with heart failure; angiotensin receptor blockers are an alternative if ACE inhibitors are not tolerated. | A | 4 |
| Beta blockers are recommended to reduce mortality in symptomatic patients with heart failure. | A | 5–8 |
| Aldosterone antagonists are recommended to reduce mortality in patients with heart failure who have current or recent rest dyspnea and in patients with recent myocardial infarction who develop systolic dysfunction with either clinically significant signs of heart failure or concomitant diabetes mellitus. | B | 11–12 |
| Direct-acting vasodilators, in addition to background therapy with ACE inhibitors, beta blockers, and diuretics (if needed), improve overall mortality for persistently symptomatic black patients with heart failure and are an alternative for patients with heart failure who cannot tolerate ACE inhibitors. | B | 17 |
| Diuretics are recommended for patients with heart failure who are volume overloaded. | B | 18 |
ACE = angiotensin-converting enzyme.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 896 or https://www.aafp.org/afpsort.xml.
Classification of Severity
The most appropriate treatment depends on the severity of heart failure. In 2001, the American College of Cardiology (ACC) and the American Heart Association (AHA) proposed the following heart failure stratification scheme: class A describes patients at risk of heart failure; class B, patients who are asymptomatic; class C, patients who are symptomatic; and class D, patients who have refractory symptoms.3 The ACC/AHA scheme has some advantages, but does not stratify symptomatic patients into subgroups to allow for easy application of clinical trial results.
The four-tier New York Heart Association (NYHA) classification of functional capacity can be used to estimate prognosis in practice and to define study populations in clinical trials. However, the NYHA system was originally designed for use in research and has limitations as a practical clinical tool because of its subjective nature.
An objective symptom classification system can be derived from inclusion criteria of clinical trials. Such a system is used to guide therapy. Relationships across these three classification schemes are shown in the top three rows of Table 1.
Table 1 Severity Classifications for Left Ventricular Systolic Dysfunction and Guidelines for Pharmacologic Treatment Based on Symptom Classification
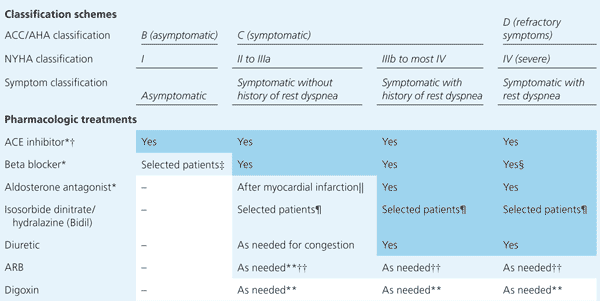
note: Intensity of shading reflects strength of recommendation.
ACC = American College of Cardiology; AHA = American Heart Association; NYHA = New York Heart Association; ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker.
*— ACE inhibitors, beta blockers, and spironolactone (Aldactone) should not be removed if symptoms improve because these medications slow disease progression and decrease mortality.
†— Although ACE inhibitors are listed first, evidence shows that an ACE inhibitor or a beta blocker may be started first and then the other added. It is reasonable to titrate the dosage of each agent in an alternating step-wise fashion to reach the target dosage. For patients intolerant of ACE inhibitors, an ARB can be substituted.
‡— No explicit evidence of benefit exists for beta blockers in asymptomatic patients; however, many of these patients will have other indications (e.g., coronary artery disease) for beta blockers.
§— Beta blockers may be safely added or continued in patients with rest dyspnea, except in those who have signs of congestion or hemodynamic instability.
‖— An aldosterone antagonist may be appropriately initiated for symptomatic patients within 14 days of a myocardial infarction.
¶— The benefit of the combination of isosorbide dinitrate and hydralazine occurred among patients self-reported as black. This combination may be added (if tolerated by the patient's blood pressure) without reducing the ACE inhibitor or beta blocker to subtarget dosages.
**— These interventions may provide symptomatic benefit. If no benefit is perceived, the medications may be withdrawn. With digoxin, however, withdrawal may lead to clinical deterioration and should be done with caution.
††— When added to ACE inhibitors, ARBs may improve symptoms. Little evidence supports the safety of using ACE inhibitors, aldosterone antagonists, and ARBs in the same patient. Because all agents can increase potassium levels, it is prudent to avoid this combination or to use it with great caution.
Pharmacologic Treatments
Table 1 summarizes recommendations for pharmacologic treatment of heart failure based on symptom severity and clinical trial results. Recommended medications and dosages are listed in Table 2. Table 3 presents practical recommendations for primary care physicians.
Table 2 Recommended Medications and Dosages to Treat Heart Failure
| Drug | Starting dosage | Target or common dosage | Monthly cost of target or common dosage* | ||
|---|---|---|---|---|---|
| Generic | Brand | ||||
| Demonstrated to decrease mortality and improve symptoms† | |||||
| Angiotensin-converting enzyme inhibitors | |||||
| Captopril (Capoten) | 6.25 mg three times daily (½ tablet‡) | 12.5 to 50 mg three times daily | $28 to 69 | $162 | |
| Lisinopril (Prinivil, Zestril) | 5 mg daily | 10 to 20 mg daily | 9 to 30 | 32, 40 | |
| Enalapril (Vasotec) | 2.5 mg twice daily | 10 mg twice daily | 64 to 75 | 94 | |
| Trandolapril (Mavik) | 1 mg daily | 4 mg daily | 36 | 40 | |
| Ramipril (Altace) | 1.25 mg twice daily | 5 mg twice daily | NA | 104 | |
| Beta blockers | |||||
| Bisoprolol (Zebeta) | 1.25 mg daily (¼ tablet‡) | 10 mg daily | 37 to 68 | 82 | |
| Metoprolol succinate (Toprol-XL) | 12.5 mg daily (½ tablet) | 200 mg daily | 65 | 69 | |
| Carvedilol (Coreg) | 3.125 mg twice daily | 25 mg twice daily | 117 to 127 | 126 | |
| Aldosterone antagonists | |||||
| Spironolactone (Aldactone) | 12.5 mg daily | 25 mg daily | 14 to 29 | 25 | |
| Eplerenone (Inspra) | 25 mg daily | 50 mg daily | NA | 119 | |
| Vasodilators | |||||
| Isosorbide dinitrate/hydralazine (Bidil) | 20/37.5 mg three times daily | 40/75 mg three times daily | NA | 405 | |
| Isosorbide dinitrate | 20 mg three times daily | 40 mg three times daily | 38 to 45 | NA | |
| Hydralazine | 37.5 mg three times daily | 75 mg three times daily | 108 to 137 | NA | |
| Angiotensin receptor blockers | |||||
| Candesartan (Atacand) | 4 mg daily | 32 mg daily | NA | 75 | |
| Valsartan (Diovan) | 40 mg twice daily | 160 mg twice daily | NA | 133 | |
| Symptomatic therapy§ | |||||
| Loop diuretics‖ | |||||
| Furosemide (Lasix) | 40 mg daily | 40 to 400 mg one to three times daily | 5 | 11 | |
| Bumetanide (Bumex) | 1 mg daily | 1 to 10 mg one to three times daily | 13 to 16 | 27 | |
| Ethacrynic acid (Edecrin) | 25 mg daily | 25 to 200 mg once or twice daily | NA | 27 | |
| Torsemide (Demadex) | 20 mg daily | 20 to 100 mg once or twice daily | 25 to 45 | 38 | |
| Thiazide diuretics‖ | |||||
| Hydrochlorothiazide | 25 mg daily | 25 to 100 mg daily | 1 to 3 | NA | |
| Metolazone (Zaroxolyn) | 2.5 mg daily | 2.5 to 10 mg daily | 39 to 79 | 47 | |
| Inotrope | |||||
| Digoxin¶ | 0.125 mg daily | 0.125 to 0.375 mg daily | 6 | 8 | |
NA = not available.
*— Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, NJ: Medical Economics Data; 2007. Cost to the patient will be higher, depending on prescription filling fee.
†— Target dosages in placebo-controlled mortality trials.
‡— Tablet is scored for ½ tablet only.
§— Common dosages.
‖— Diuretics have not been separately studied for target dosage. Titrate as needed for symptom relief.
¶— Generic is available, but brand is usually dispensed.
Table 3 Recommendations for Pharmacologic Treatment of Heart Failure
| Drug category | Recommendation |
|---|---|
| ACE inhibitors and ARBs | May cause hyperkalemia in the presence of renal failure and should be avoided or used only with great caution in patients with serum creatinine levels higher than 2.5 mg per dL (220 μmol per L), glomerular filtration rates of less than 30 mL per minute per 1.73 m2, or potassium levels higher than 5.0 mEq per L (5.0 mmol per L) Both are contraindicated in patients who are pregnant and in those with bilateral renal artery stenosis, unilateral renal artery stenosis with solitary kidney, or allergies; angioedema can occur in rare cases |
| Beta blockers | May be used in patients with heart failure caused by systolic dysfunction and who do not have contraindications (e.g., allergy, bradycardia, hypotension, severe reversible airway disease) Should be added when patients are stable to arrest the progression of the disease; they are not to be added as rescue therapy for patients who are decompensating Start at low dosage and double every two to four weeks as tolerated until target dosage reached; stop upward titration if patient is intolerant of higher dosages Absolute contraindications include heart block, bradycardia, and severe reversible airway disease Relative contraindications include rest dyspnea with signs of congestion and hemodynamic instability; once these issues have resolved, beta blockers may be added to the chronic regimen |
| Aldosterone antagonists | Risk of hyperkalemia may be significant, especially among patients not meeting clinical trial entry criteria; these risks can be minimized by ensuring appropriate patient selection before initiating treatment and by avoiding use in patients with glomerular filtration rates of less than 50 mL per minute per 1.73 m2 or serum creatinine levels higher than 2.5 mg per dL Electrolytes should be monitored closely; elevation of potassium to a level of 5.0 to 5.5 mEq per L should prompt dosage reduction or drug discontinuation |
| Isosorbide dinitrate and hydralazine | These medications are available as a fixed-dose combination in branded form (Bidil); generic constituents should be just as effective and are much less expensive Clinical trials were performed using isosorbide dinitrate; isosorbide mononitrate (Monoket) is dosed daily and is more convenient; evidence of clinical equivalence of the mononitrate form is only per expert opinion Cannot be used concomitantly with phosphodiesterase inhibitors (e.g., sildenafil [Viagra], tadalafil [Cialis], vardenafil [Levitra]) |
| Diuretics | Although not specifically tested in clinical trials, diuretics should still be used as needed for volume overload Diuretics were consistently part of background therapy in published placebo-controlled mortality trials of symptomatic patients in which ACE inhibitors, beta blockers, and aldosterone antagonists were studied ACE inhibitors and beta blockers may reduce the need for diuretic therapy |
| Combining drugs | Pharmacologic treatment described in Table 1 is the desired end point No data are available to indicate how best to introduce all of these medications; however, all major trials added beta blockers or spironolactone (Aldactone) to background therapy with ACE inhibitors, diuretics, and, sometimes, digoxin Many medications appropriate for heart failure (ACE inhibitors, ARBs, aldosterone antagonists, digoxin) can affect potassium levels or can be affected by potassium levels and renal function; vigilant monitoring is required ACE inhibitors, beta blockers, spironolactone, and ARBs should not be removed if symptoms improve because these medications slow disease progression and decrease mortality |
| Referral | Consider referral for the following clinical situations: diagnostic or revascularization procedures, ventricular arrhythmias, valvular heart disease, worsening or refractory heart failure, or consideration for transplantation |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker.
ACE INHIBITORS
Angiotensin-converting enzyme (ACE) inhibitors are indicated for the treatment of all patients with heart failure caused by systolic dysfunction. Randomized controlled trials have demonstrated the effectiveness of captopril (Capoten), lisinopril (Prinivil, Zestril), enalapril (Vasotec), trandolapril (Mavik), and ramipril (Altace) in reducing morbidity and overall mortality in asymptomatic and symptomatic patients.4 Although not all of the available ACE inhibitors have been studied for heart failure, no study has failed to show benefit with an ACE inhibitor. Their use should be considered a priority of treatment unless absolutely contraindicated. There is no evidence to suggest the superiority of one ACE inhibitor over another in treating heart failure.
ACE inhibitors are often avoided in patients with heart failure because of perceived risk and contraindications. It is important that patient factors, such as lower blood pressure, elevated serum creatinine level, and cough, not be considered absolute contraindications. However, patients with systolic blood pressure lower than 100 mm Hg or serum creatinine level higher than 2.5 mg per dL (220 μmol per L) were largely excluded from clinical trials; therefore, ACE inhibitors should be used with caution in these populations.
Some patients cannot tolerate ACE inhibitors. In these patients, an angiotensin receptor blocker (ARB) or direct-acting vasodilators, such as isosorbide dinitrate and hydralazine, may be substituted. If ACE inhibitors are contraindicated because of renal failure, then combination isosorbide dinitrate and hydralazine is preferred.
BETA BLOCKERS
Beta blockade is recommended in patients with heart failure caused by systolic dysfunction, except in those who are dyspneic at rest with signs of congestion or hemodynamic instability, or in those who cannot tolerate beta blockers. Three beta blockers (i.e., carvedilol [Coreg], metoprolol succinate [Toprol-XL], and bisoprolol [Zebeta]) at target dosages of 25 mg twice daily, 200 mg daily, and 10 mg daily, respectively, have been shown in randomized controlled trials to produce similar clinically important decreases in overall mortality (absolute risk reduction [ARR] = 5.5 percent over 0.87 year, 3.8 percent over 1.0 year, and 5.5 percent over 1.3 years, respectively).5–8 However, because at least one other beta blocker (bucindolol; not available in the United States) failed to reduce mortality in a placebo-controlled trial, beta blockers cannot be presumed to have a class effect on heart failure.9
Although the three beta blockers known to be effective differ pharmacologically, they have not been compared directly. A comparative trial demonstrated that carvedilol, 25 mg twice daily, was superior to metoprolol tartrate (Lopressor), 50 mg twice daily, in prolonging survival in patients with symptomatic heart failure.10 However, the dosage and formulation of metoprolol in this study differed from the dosage and formulation in a placebo-controlled trial in which metoprolol succinate was proved effective.7 Therefore, even though the comparative trial demonstrated the superiority of carvedilol, the critical importance of dosage and drug formulation in patients with heart failure has not been resolved.
Beta blockers should be administered with some caution to patients with heart failure, but primary care physicians can clearly manage the titration of beta blockers. The initial dosage should be started, then doubled every two to four weeks until the target dosage is reached or the patient is unable to tolerate higher levels. Symptoms of increasing dyspnea, worsening heart failure, and hypotension or symptoms of hypotension should prompt evaluation of the patient and may necessitate increasing the diuretic dosage or discontinuing or decreasing the beta-blocker dosage. Beta blockers should be added when patients are stable to diminish the progression of the disease. They are not to be added as a rescue therapy in patients who are decompensating.
ALDOSTERONE ANTAGONISTS
Aldosterone antagonism is indicated in patients with symptomatic heart failure who have rest dyspnea or a history of rest dyspnea within the past six months (ARR = 11 percent over two years; number needed to treat [NNT] = 9).11 In addition, aldosterone antagonism is indicated in patients following recent myocardial infarction who develop systolic dysfunction with either clinically significant signs of heart failure or concomitant diabetes mellitus.12
The two available agents (i.e., low-dose spironolactone [Aldactone] and eplerenone [Inspra]) differ in potency, cost, and adverse effects. Spironolactone is twice as potent as eplerenone and costs much less; however, at a dosage of 25 mg daily, it can also cause gynecomastia and/or mastodynia in men, an adverse effect not seen with eplerenone.
As aldosterone antagonists, spironolactone and eplerenone are potassium-sparing diuretics that can cause hyperkalemia, especially when administered with ACE inhibitors, ARBs, and exogenous potassium. In controlled clinical trials of aldosterone antagonists, severe hyperkalemia was rare, but patients with serum creatinine levels higher than 2.5 mg per dL were excluded, and potassium levels were closely monitored, with drug dosages adjusted according to potassium level.11,12 Even in these selected populations, patients with glomerular filtration rates of less than 50 mL per minute per 1.73 m2 developed hyperkalemia almost twice as often as patients with glomerular filtration rates greater than 50 mL per minute per 1.73 m2.11,12 Outside the carefully controlled conditions of a clinical trial, aldosterone antagonism has been associated with severe hyperkalemia and increased mortality.13 Therefore, aldosterone antagonists should not be administered to patients with glomerular filtration rates of less than 50 mL per minute per 1.73 m2 or to patients who do not meet the inclusion criteria of the clinical trials.
DIRECT-ACTING VASODILATORS
Direct-acting vasodilators were among the first medications shown to improve survival in patients with heart failure.14 Subsequently, randomized controlled trials have demonstrated that ACE inhibitors were superior, particularly in NYHA classes I and II heart failure.15 In a posthoc analysis of those trials, the combination of isosorbide dinitrate and hydralazine was particularly effective in black patients.16 Improvement in overall mortality among black patients using isosorbide dinitrate and hydralazine has since been demonstrated in a prospective trial in which these agents were added to usual background therapy (ARR = 4 percent over 10 months; NNT = 25).17 Although the patients in the trial were self-identified as black, a substudy identified a genetic polymorphism more common among black persons as the trait most likely to predict responsiveness to this drug combination. The combination of 40 mg of isosorbide dinitrate and 75 mg of hydralazine three times daily may be used (if tolerated by blood pressure) in symptomatic black patients with heart failure and may be used as a substitute agent in any patient with heart failure who is intolerant of ACE inhibitors because of cough, angioedema, or renal failure. Headache may develop, but it usually becomes less problematic with continued use.
DIURETICS
Diuretics are used, and often required, to manage acute and chronic volume overload. Because diuretics may produce potassium and magnesium wasting, monitoring of these electrolytes is important.
Although there have been no large controlled clinical studies of diuretics in the treatment of heart failure, most patients in trials of ACE inhibitors, beta blockers, spironolactone, and digoxin received diuretics as part of baseline therapy for heart failure. Also, a Cochrane meta-analysis of three small trials (n = 202) found an odds ratio for death of 0.24 (P = .02) in patients with heart failure on diuretics versus placebo.18 Loop diuretics are the most potent individual agents, but they are associated with acute and chronic distal tubular compensation (distal tubular hypertrophy). The dosage of loop diuretic will vary greatly among patients and will be determined by individual response. Combining a loop diuretic with a thiazide diuretic increases potency by minimizing distal tubular compensation.
ARBs
Evidence supports the use of ARBs as a substitute agent in patients with heart failure who cannot tolerate ACE inhibitors19; the combination of isosorbide dinitrate and hydralazine is also effective in this population.14 No trials have compared isosorbide dinitrate/hydralazine and ARBs among patients intolerant of ACE inhibitors. Although ARBs are effective alternatives, ACE inhibitors have the advantage of lower cost and more patient experience, and they are still the preferred first-line agent for suppression of the reninangiotensin system in most patients.
ARBs can also safely be added to ACE inhibitors. This combination may be appropriate for patients who remain symptomatic despite therapy with diuretics, ACE inhibitors, and beta blockers.20 Some of these patients may also be candidates for an aldosterone antagonist. Because ACE inhibitors, ARBs, and aldosterone antagonists can all increase potassium levels, they may represent a dangerous combination if used together.
DIGOXIN
The collection of drugs that have a beneficial impact on mortality in heart failure is expanding, and because polypharmacy can become a barrier to compliance, the role that digoxin will ultimately play in heart failure is unclear. Currently, digoxin is indicated for use in patients with heart failure and atrial fibrillation and may also be administered to improve symptoms and to decrease hospitalization rates in patients who remain symptomatic despite maximal individualized therapy with diuretics, ACE inhibitors, and beta blockers.21 The usual dosage range for digoxin is 0.125 to 0.250 mg daily, to be adjusted as needed based on symptoms, other drugs, or renal impairment. In general, serum digoxin levels for treatment of symptomatic heart failure should be between 0.5 and 1.0 ng per mL (0.6 to 1.3 nmol per L) when measured at least six to eight hours after dosing (not 0.8 to 1.5 ng per mL [1.0 to 1.9 nmol per L] as recommended in the past).22,23
A posthoc analysis of the Digitalis Investigation Group study revealed a trend toward increased mortality among women with heart failure who were taking digoxin; however, digoxin levels were higher among women than men.24 A prospective trial to validate these results is unlikely. Use of digoxin in women may still be safe and effective with close monitoring of digoxin levels, especially in patients with renal insufficiency. Digoxin should be discontinued with caution. Withdrawal of the drug in patients with heart failure may result in clinical deterioration; however, this theory was only tested in a small study population.25

