
Am Fam Physician. 2008;77(8):1106
I had pain for years before my condition was diagnosed. My gynecologist of 20 years kept telling me I was fine. He did not think I had a disease, but he was wrong and should have done the appropriate tests and procedures beyond an ultrasound. I was constantly shuffled between him and numerous other doctors, with no real resolution to my problem. I had what was thought to be pancreatitis, and was told I would have to live with the pain, and be on pain medication for the rest of my life. I struggled to cope with the emotional anguish associated with knowing that this was how my life was going to be, in and out of hospitals every few weeks, with no hope for relief.
When the medications no longer eased the pain, I would go to the hospital. Residents would rudely inform me I was not going to be given additional pain medication, or the emergency room physician would drug me so that I could not see to sign the discharge papers. In the six weeks before my diagnosis, I realized my suspicions were true—medical personnel in the hospitals were convinced I was looking for drugs, and probably did not believe I was in pain. If I mentioned pancreatic problems, I was a drug-seeking alcoholic, even though I have never been a drinker.
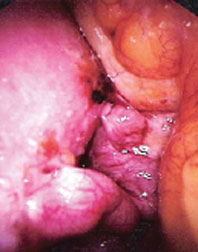
My prayers were answered when I experienced debilitating pain and was taken to the emergency room where I asked about endometriosis and was given the name of a gynecologist. After a diagnostic laparoscopy, the gynecologist said he was surprised I was even functioning. I was diagnosed with severe stage IV endometriosis—one of the two worst cases he had seen in his 12 years of practice. My ovaries could not be visualized, my tubes were destroyed, and the back of my uterus was adhered to my rectum. My pelvis was “frozen.” The cul-de-sac was obliterated by intestines. The colon was involved. My case was beyond the scope of his training, and I needed a hysterectomy performed by a gynecologic oncologist. No wonder I was beginning to pass out from the pain and needed medication. All the gynecologist could do during the diagnostic laparoscopy was take pictures of the devastation (above). —d.j.h, 48
COMMENTARY
We are reminded how important it is to listen to the patient. In this case, the patient's pain seems to have been attributed to a somatoform disorder. The differential diagnosis of chronic pain behaviors includes pseudo-addiction. In pseudo-addiction, the patient's pain is undertreated, leading to a demand for relief that is often misinterpreted as drug seeking. Although we should avoid pursuing extensive and unnecessary testing for patients with somatization, we must also give patients the benefit of the doubt, and not give up on evaluating unexplained symptoms simply because we cannot initially find an explanation. In hindsight, given the difficulty of diagnosing endometriosis clinically, it is apparent that this patient should have had laparoscopic evaluation much earlier in the course of her illness. Perhaps if a family physician or other primary care physician had been at the helm, he or she would have been more likely to pursue a diagnosis or further evaluation.